[box type=”bio”] What to Learn from this Article?[/box]
Amputation with a good prosthesis can considerably increase the quality of life in patients with advanced chondrosarcoma.
Case Report | Volume 6 | Issue 2 | JOCR April-June 2016 | Page 9-12 | O.B. Pattanashetty, Dayanand B.B, Arravind Pillai, Preetish Endigeri. DOI: 10.13107/jocr.2250-0685.406
Authors: O.B. Pattanashetty[1], Dayanand B.B[1], Arravind Pillai[1], Preetish Endigeri[1]
[1] Department of Orthopaedics, BLDEU’s, Shri B M Patil Medical College, Bijapur, Karnataka, India.
Address of Correspondence
Dr. Arravind Pillai,
Post Graduate Student, Department of Orthopaedics, Shri B M Patil Medical College, Bijapur 586103, Karnataka, India.
E-mail: arravind86@live.com
Abstract
Introduction: Dedifferentiated chondrosarcoma (DDCS) is a rare and malignant form of primary bone tumor refractive to chemotherapy and radiotherapy. It accounts for 1-2% of all primary bone tumors. Surgical resection, limb-salvage surgeries and amputation remain the mainstay of treatment. The prognosis of dedifferentiated chondrosarcoma is poor.
Case Report: We report a case of a 51-year-old male having a swelling and an ulcer distal to the left knee later diagnosed with dedifferentiated chondrosarcoma of proximal tibial and fibular metaphysis. Although DDCS is a highly malignant tumor, no metastasis was found and the patient was treated with transfemoral amputation. Post-operative histopathology showed nuclear atypia, binucleated and multinucleated chondrocytes with spindling and neoplastic cells arranged in storiform pattern and giant cells which confirmed the diagnosis of DDCS.
Conclusion: Early diagnoses and treatment are important while treating these tumors in order to prevent morbidity and mortality.
Key words: Dedifferentiated chondrosarcoma, tibia, fibula, amputation
Introduction
Chondrosarcoma (CS) is a low-grade malignant bone tumor whereas DDCS is a highly malignant, fatal tumor despite aggressive surgical resection or amputation. DDCS accounts for 10% of all chondrosarcomas. Presence of multiple types of tumor cells poses a challenge to the treatment and radical surgical resection remains the primary treatment modality [1]. Lung metastasis is found early in the disease and is often the main reason for treatment failure and death in DDCS [2]. In early stages, the tumor may be treated with radical resection or limb salvage surgery, but amputation is often necessary when there is extensive local tissue destruction or secondary infection. We report a case of dedifferentiated chondrosarcoma of proximal tibia and fibula with a discharging ulcer in a 51 year old male patient.
Case report
A 51-year-old male came to our hospital with a year old history of gradual onset pain and swelling below his left knee and repeated episodes of fever. The swelling advanced gradually over the year and ulcerated 3 months ago. Patient could walk without any assistance. On examination, there was a firm mass of 30*18*12 cm at the upper part of tibia extending to the calves and a large discharging ulcer of 12 cm diameter anteriorly with necrotic areas. The discharge was yellow, thick in consistency. Range of motion of knee was reduced. Tenderness was present over the left knee and proximal tibia. Pulsations of dorsalis pediis, posterior tibial and popliteal arteries were present. A neurological examination of the lower limbs was within normal limits. Examination of other systems was unremarkable. A clinical blood examination and a chest X-ray at the time of presentation showed no abnormality. Plain radiograph showed a large lesion with soft tissue opacity involving the metadiaphysis of left tibia, causing erosion and destruction of tibia and adjacent fibula, with linear and ring like calcifications suggesting a tumor, possibly an enchondroma, osteosarcoma or chondrosarcoma, with extensions into the soft tissue of proximal leg. Tc99m radio isotope bone scan showed increased tracer uptake in the shaft of left tibia and proximal soft tissue with no skeletal metastasis. Due to financial constraint on the side of patient, a MRI was not done. Based on the presentation and radiographic appearance, differential diagnosis included osteosarcoma and chondrosarcoma of tibia. On admission, patient was started on intravenous antibiotics and analgesics and counselled on different treatment options. Considering the preferences of the patient, including the cost factor of megaprosthesis, the size of the lesion, extend of infection and survival rate of the tumor, the patient opted for transfermoral amputation as treatment modality along with post-operative chemotherapy. Post-surgery, the cut section from the amputated leg showed a grey white tumor measuring 28*16*10 cm involving upper half of tibia and fibula with haemorrhagic, necrotic and focal myxoid characteristics, and soft tissue extension up to the knee. Microscopy revealed tumor tissues arranged in small and large irregular lobules of hyaline cartilage. The chondrocytes were both binucleated or multinucleated and showed atypia and spindling. Section from tissue surrounding the necrotic area showed spindle cells arranged in interlacing bundles, fascicles and a focal storiform pattern. These cells showed atypical mitosis and hyperchromatic nuclei. Many tumor giant cells were present. Together, these findings led to the diagnosis of DDCS. The patient underwent transfermoral amputation followed by chemotherapy. Following amputation, patient received intra-venous antibiotics and analgesics. The patient received Cisplatin and Doxorubicin as a first line chemotherapy. A soft elastic dressing was applied. Dressing was changed every two days and wound monitored for erythema, swelling and signs of infection. Patient was advised to lie prone on the bed to avoid contractures. On the 2ndpost-operative day, the drain was removed. Skin stretching exercises, basic mobilisation, upper extremity strengthening exercises and isometric muscle training of the residual limb were initiated on the 7th post-operative day. Staplers were removed on the 12thday and the patient was mobilised with assistance. In the 8th week, the patient was consulted with a prosthetist and a transfemoral prosthesis made of high-density polyethylene pipes with a single axis knee joint with a lock was prescribed, following which physical therapy was initiated. Following physical therapy, patient could walk without any assistance.
Follow-up at one year.
The incision site had healed and the patient could walk with the aid of prosthesis. Chest radiograph showed no signs of lung metastasis. Routine blood investigations and physical examination of the patient were unremarkable. A CT of the chest was advised, but the patient refused due to financial constraints. Follow up at 18 months is awaited and a CT scan of chest planned.
Discussion
DDCS, first described by Dahlin and Beabout in 1971[3], is a subtype of chondrosarcoma, affecting mostly in the 5th and 6th decade of life. It accounts for 20 to 27 % of all primary malignant osseous neoplasms. The most common sites involved are the femur (46-55%), pelvis (23-28%) and humerus. The prognosis is poor with a median survival rate of 6 months and a five year survival rate of 10-13% [4]. Chondrosarcoma may be classified as central, peripheral and periosteal based on the location of the tumor or as conventional CS, clear cell CS, mesenchymal CS and dedifferentiated CS on the basis of histological appearance [5]. On the basis of origin, chondrosarcomas maybe be divided into primary or secondary lesions. Primary chondrosarcomas are those that arise de novo, whereas secondary chondrosarcomas arise from previous cartilage lesions. 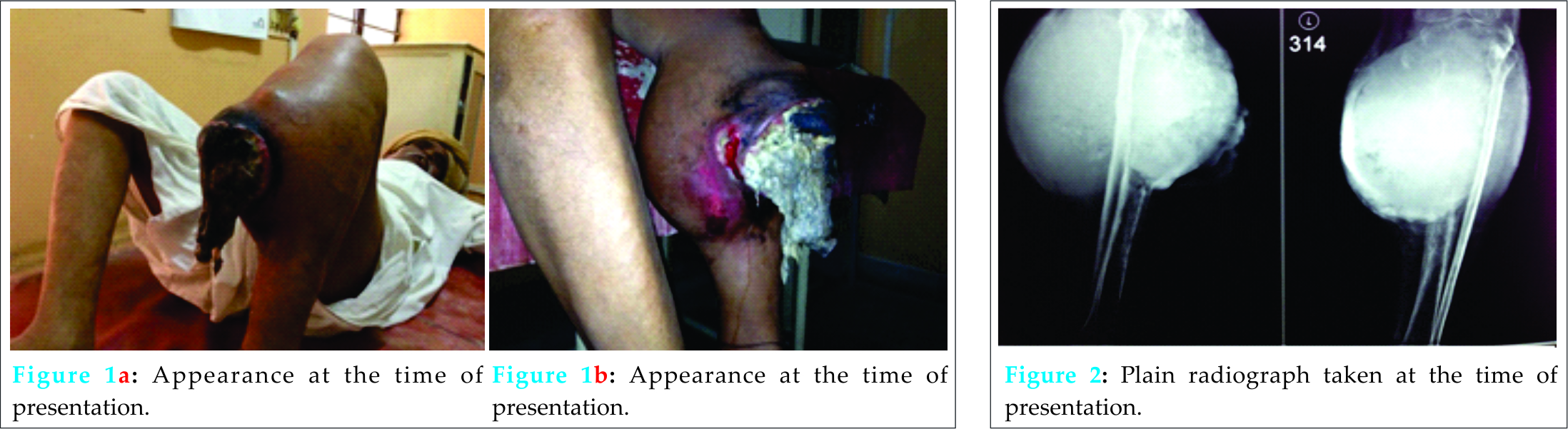
Characteristic radiographic feature is that of a bimorphic pattern with parts of the lesion being more aggressive than others. Diagnosis is confirmed histologically, and the characteristic feature is that of an abrupt interface between a benign cartilage tumor, or low to intermediate grade chondrosarcoma, and a high grade dedifferentiated non cartilaginous component [3]. The non cartilagenous component may be a osteosarcoma, fibrosarcoma, angiosarcoma, rhabdomyosarcoma, malignant histiocytoma and rarely a giant cell tumor or a clear cell chondrosarcoma [6, 7]. The characteristic histological feature is of chondrocytes of various sizes, with polymorphic nuclei and a highly sarcomatous connective tissue with small dense polymorphic hyperchromatic nuclei [8]. In this case, microscopy of the cut section revealed binucleated and multinucleated chondrocytes with nuclear atypia along with giant cells which led us to the diagnosis of DDCS. Pathogenesis of DDCS remains controversial. Multiple theories exist on the pathogeneis of DDCS. Dahlin and Beabout proposed that dedifferentiation is the result of direct transformation of a well differentiated cartilage lesion [3]. Several genetic theories have been implicated in the pathogenesis and progression of chondrosarcoma which include a higher rate of proliferation rate on Ki-67 immunochemistry with loss of heterozygosity at many loci ,amplification of the c-myc proto oncogene and fos/jun, PTHR1 mutation, and also the involvement of the hedgehog signalling pathway, p53and insulin like growth factor [9,10]. Sanerkin and Woods thought DDCS to be a type of collision tumor, whose differentiated components originated from reactive fibrous tissue in the necrotic region around cartilage [11]. Another theory states an independent origin of the different tumor cell types, some of which differentiate into poorly differentiated chondrosarcoma while others do not.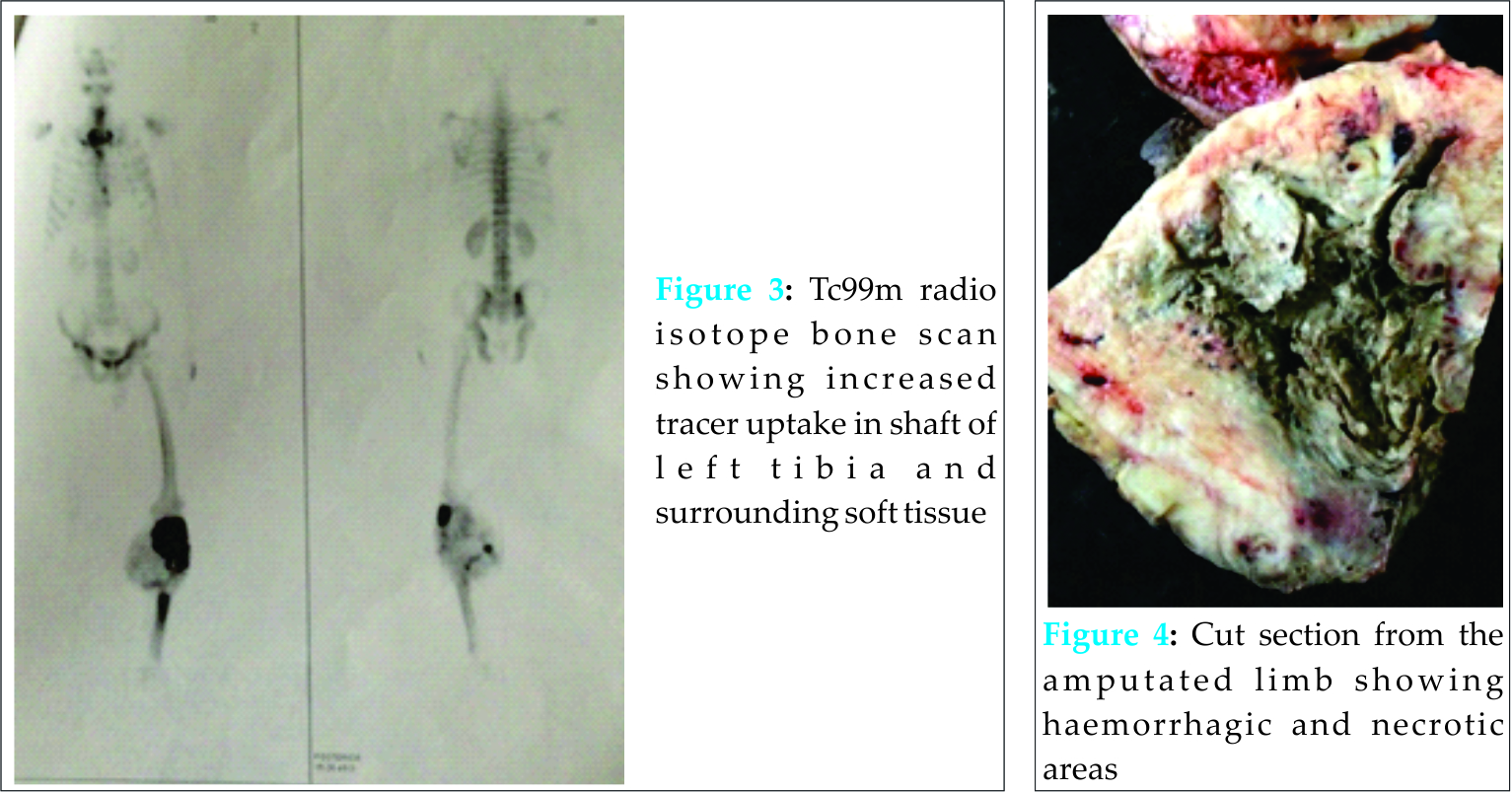
Treatment options include radical surgery, wide resection, margin resection, limb salvalge procedures with megaprosthesis and above knee amputation along with chemotherapy and tumor curettage. In a retrospective study of 22 cases of DDCS, Mitchell et al concluded that treatment with limb salvage surgery and chemotherapy does not show improvement over traditional methods of treatment [12]. Studies have shown higher rates of recurrence of tumor with limb salvaging procedures than with amputation. In a study comparing limb salvage procedures and amputations for tumors in 227 patients, Rougraff et al found better functional outcomes in patients who underwent limb salvaging surgeries, but local recurrence was higher (8 of 73) in patients treated with limb preservation than in patients treated with amputation (9 of 115)[13]. This is of significance while dealing with an aggressive tumor such as this. Also, severe infection in the surgical field and vascular invasion is a contraindication to any limb salvaging procedure [12]. Chemotherapy and radiotherapy has not shown to be effective in treatment of DDCS [1,4], but is used as an adjuvant therapy. Chemotherapy has shown to be effective in shrinking the size of the tumor pre-operatively and maybe used when excision of the tumor is opted as the management. In a study by Kazuya Yokota, out of 9 patients, 4 patients were given chemotherapy, but showed no improvement in survival rate [14]. Poor results have been shown following treatment with radiotherapy, but have been used in case of diffuse metastases. In a recent study by Folkert et al, they found significantly better local control of high grade sarcoma that had metastasized to spine in patients treated with image-guided stereotactic radiosurgery (87.9%) than in patients treated with conventional radiotherapy (50-77%) [15]. In our patient, although no evidence of metastases was found, patient was started on chemotherapy postoperatively and radiotherapy was not used. The patient presented late along with secondary infection and was beyond the scope of radical resection or limb salvage surgery. We conclude that early diagnosis and treatment are important to reduce morbidity and mortality rates in case of DDCS.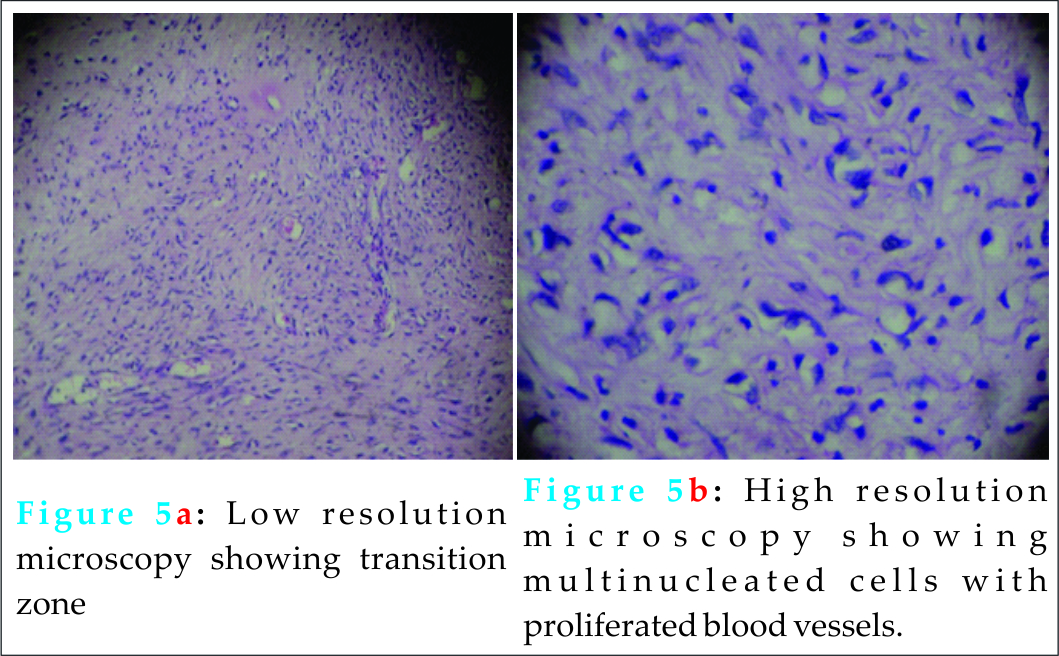
Conclusion
Dedifferentiated chondrosarcoma is a highly lethal malignancy, despite aggressive surgical resection or even amputation. Early diagnosis and treatment can improve the outcome of treatment. Amputation is an effective and often a life saving procedure in later stages of the tumor.
Clinical Message
Dedifferentiated chondrosarcoma is a very aggressive tumor and early detection and management is vital in order to save the limb and to avoid mortality. It can be diagnosed with a biopsy and treatment usually involves resection of the tumor and prevention and management of metastases which commonly involves the lungs. In cases of advanced tumors with superadded infection, amputation is almost necessary as other treatment modalities like limp salvage pose a threat of reinfection and failure. In cases where other treatment options are not available such as financial restraint on the side of the patient, amputation with a good prosthesis can improve the quality of life of the patient.
References
1. Onishi AC, Hincker AM, Lee FY. Surmounting chemotherapy and radioresistance in chondrosarcoma :Molecular mechanisms and therapeutic targets. Hindawi publishing corporation 2011.
2. Frassica FJ, Unni KK, Beabout JW, Sim FH: Dedifferentiated chondrosarcoma. A case report of the clinicopathological features and treatment of seventy-eight cases. J. Bone Joint Surg [Am] 1986;68-A:1197-1205.
3. Dahlin DC, Beaubout JW. Dedifferentiation of low-grade chondrosarcomas. Cancer 1971; 28: 461-466.
4. Staals EL, Bacchini P, Bertoni F. Dediiferentiated central chondrosarcoma. Cancer 2006;106:2882-91.
5. Matsumoto Y, Takahashi Y, Harimaya K, Nakagawa T, Kenichi K, Okada S. et al. Dedifferentiated chondrosarcoma of the cervical spine: a case report. World Journal of surgical oncology 2013;11:32.
6. Bruns J, Fieldler W, Werner M, Delling G. Dedifferentiated chondrosarcoma-a fatal disease. J Cancer Res Clin Oncol 2005;131:333-339.
7. Adler CP. Bone diseases macroscopic, Histological and radiological structural changes in the skeleton. Springer, Berlin- Heidelberg- New York, 2005:214-254.
8. Herget GW, Uhl M, Opitz OG, Adler CP, Sudkamp NP, Knoller S. The Many Faces of Chondrosarcoma of Bone. Acta Chirurgiae Orthopaedicae et Traumatologiae Cechosl 2011;78 :501-509.
9. Bovee JV, Cleton-Jansen AM, Kuipers-Dijkshoorn NJ. Loss of heterozugosity and DNA ploidy point to a diverging genetic mechanism in the origin of peripheral and central chondrosarcoma. Genes Chromosomes Cancer 1999;26(3):237-46.
10. Bovee JV, Cleton-Jansen AM, Rosenberg C, et al. Molecular genetic characterization of both components of a dedifferentiated chondrosarcoma, with implications for its histogenesis. J Pathol. 1999;189(4):454-62.
11. Sanerkin NG, Woods CG. Fibrosarcomata and malignant fibrous histiocytomata arising in relation to enchondromata [J]. Bone Joint Surg Br, 1979;61-B(3):336-372.
12. Mitchell AD, Ayoub K, Mangham DC, Grimer RJ, Carter SR, Tillman RM: Experience in treatment of dedifferentiated chondrosarcoma. J Bone Joint Surg [Br] 2000;82(B):55-61.
13. Rougraff BT, Simon MA, Kneisl JS, Greenberg DB, Mankin HJ: Limb salvage compared with amputation for osteosarcoma of the distal end of the femur. A long term oncological, functional, and quality-of-life study. J Bone Joint Surg Am 1994;76:649-656.
14. Yokota K, Sakamoto A, Matsumoto Y, Matsuda S, Harimaya K, Oda Y, Iwamoto Y: Clinical outcome for patients with dedifferentiated chondrosarcoma: a report of 9 cases at a single institute. Journal of orthopaedic surgery and research 2012;7:38.
15. Folkert MR, Bilsky MH, Tom AK, Oh JH, Alektiar KM, Laufer I, et al. Outcomes and toxicity for hypofractionated and single-fraction image-guided stereotactic radiosurgery for sarcomas metastasizing to the spine. Int J Radiat Oncol Biol Phys 2014;88(5):1085-91.
| How to Cite This Article: Pattanashetty OB, Dayanand BB, Pillai A, Endigeri P. Dedifferentiated Chondrosarcoma of Proximal Tibia and Fibula with an Infected Ulcer: A Case Report. Journal of Orthopaedic Case Reports 2016 April-June;6(2): 9-12. Available from: https://www.jocr.co.in/wp/2016/04/01/2250-0685-406-fulltext/ |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com





