[box type=”bio”] Learning Point of the Article: [/box]
TKA using constrained condylar or rotating hinge prosthesis by a combination of autologous bone graft and metal tibial block augmentation and lateral release and patellar replacement can show good outcomes in the management of patients with Charcot knee joints.
Case Report | Volume 10 | Issue 2 | JOCR March – April 2020 | Page 9-12 | Ryo Yoshikawa, Atsushi Kitagawa, Takao Inokuchi, Naoko Shima, Yasushi Hashimoto. DOI: 10.13107/jocr.2020.v10.i02.1674
Authors: Ryo Yoshikawa[1], Atsushi Kitagawa[1], Takao Inokuchi[1], Naoko Shima[1], Yasushi Hashimoto[1]
[1]Department of Orthopedic Surgery, Hyogo Prefectural Central Rehabilitation Hospital,1070 Akebono-chou, Nishi-ku, Kobe, Hyogo, 651-2181 Japan.
Address of Correspondence:
Dr. Ryo Yoshikawa,
Department of Orthopedic Surgery, Hyogo Prefectural Central Rehabilitation Hospital,1070 Akebono-chou, Nishi-ku, Kobe, Hyogo, 651-2181 Japan.
E-mail: ryskw330@gmail.com
Abstract
Introduction: Charcot arthropathy causes severe progressive and destructive joint disease. With the development of prostheses and surgical techniques, orthopedic surgeons have a greater opportunity to use total knee arthroplasty (TKA) to treat Charcot knee. However, consensus is lacking regarding prosthesis choice. Here, we present a case of staged bilateral TKA in a patient with bilateral Charcot knees in a different way.
Case Report: We report a case of a 64-year-old woman with bilateral Charcot knees. Her knee joints had become increasingly unstable with severe deformity over 1 year, and she has been unable to walk for1 month before hospitalization. We performed the first TKA of the right knee using rotating hinge prosthesis with a combination of autologous bone graft and metal tibial block augmentation; lateral release and patellar replacement were also performed. Three months after the first surgery, we performed the second TKA for her left knee using a constrained condylar prosthesis with a combination of lateral retinaculum release and patella replacement. At the 6-month follow-up, both knees were stable and in good alignment. There were no signs of loosening or fracture. The patient experienced no pain and was able to ambulate in her household using a walker.
Conclusion: TKA using constrained condylar or rotating hinge prosthesis effectively treats Charcot knee. Surgeons must acquire both appropriate alignment and ligament stability rather than the range of motion to ensure increased longevity of the prosthesis by performing various surgical techniques. Careful follow-up is needed, but Charcot knee patients can have good outcomes with TKA.
Keywords: Total knee arthroplasty, Constrained condylar prosthesis, Rotating hinge prosthesis, Charcot joint.
Introduction
Charcot arthropathy causes severe progressive and destructive joint disease caused by central or peripheral neuropathy. The degree of pain does not correspond with the severity of joint destruction. Total knee arthroplasty (TKA) for Charcot knee has classically been considered an absolute contraindication [1].With the development of prostheses and surgical techniques, orthopedic surgeons have had increasing opportunities to perform TKA for Charcot knee. However, consensus is lacking regarding prosthesis choice. Here, we describe a case of staged bilateral TKA in a patient with bilateral Charcot knees in a different way.
Case Report
Clinical history
A 64-year-old woman presented to our hospital with a 1-year history of bilateral pain and progressive deformity. She presented to a local clinic and received conservative medical treatment such as fixed knee braces and analgesics. However, her knees had become increasingly unstable with severe deformity, and she was unable to walk for 1 month before hospitalization. The patient had undergone spinal surgery due to lumbar canal stenosis with posterior instrumentation when she was 55 years old; the spinal implants were removed 3 years post-operative.
Physical examination
At the time of presentation, she was unable to walk even with a walker. Deformity, swelling, and effusion were noted in both knees. The right knee was extremely valgus and the left was contrarily varus. There was no evidence of redness or heat. The range of motion of the right knee was 15–90(recurvatum deformity), while that of the left knee was 5–100. Bilateral global laxity was noted with greater severity on the right side. Lateral patellar subluxation was observed in the right knee. The manual muscle testing (MMT) grades of the bilateral lower limbs indicated good strength (4/5). The bilateral patellar tendon reflex and Achilles reflex were depressed. There was a severe sensory loss of touch, pain, temperature, and vibration in the bilateral lower limbs, especially in the distal region.
Blood test
A blood test showed normal inflammatory parameters (white blood cell count, 4.9 × 109/L; neutrophils, 2.7 × 109/L; and C-reactive protein, 0.12 mg/dL). Her glycated hemoglobin level was normal (5.5%). Treponema pallidum hemagglutination, T-SPOT.TB, and antinuclear antibody tests were all negative.
Imaging
A plain radiograph of the right knee showed severe valgus and recurvatum deformity with a severe bone defect at the posterolateral tibial plateau (Fig. 1), while that of the left knee showed varus deformity with a large calcified loose body in the suprapatellar pouch (Fig. 2). Moreover, lateral patellar subluxation of the right knee was evident (Fig. 3). The anatomic femorotibial angle was 140at the right and 180at the left (the so-called windswept deformity) (Fig. 4). All other joints were normal.
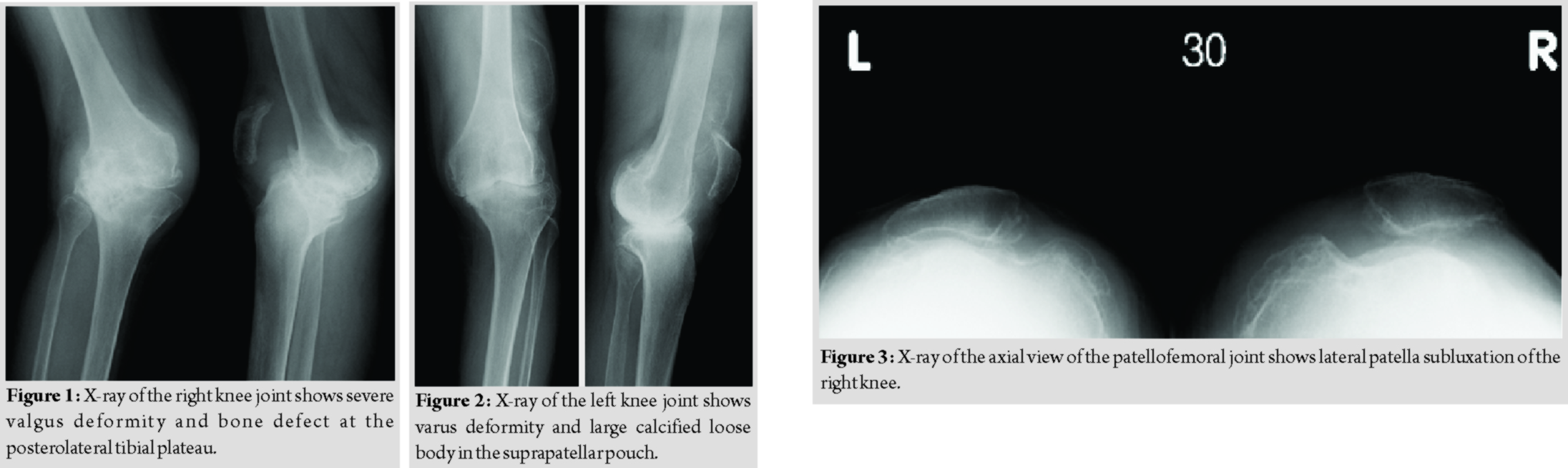
Management
After admission, bed rest and arthrocentesis relieved her knee pain. A culture of the synovial fluid was negative. An examination of the nerve conduction velocities in her legs showed us that she had severe sensory neuropathy of the bilateral lower limbs. Based on her medical history, we believed that this patient had developed bilateral neuropathic arthropathies caused by lumbar spinal canal stenosis. Because she could not walk due to instability, we decided to perform a staged bilateral TKA. We performed TKA of the right knee first because its deformity was more severe. We chose a rotating hinge prosthesis (Modular Rotating Hinge; Stryker, Mahwah, NJ, USA) and performed the procedure using a medial parapatellar approach. Modular stems were used both on the tibial and femoral implants. The procedure included autologous bone grafting and metal augmentation for tibial bone loss and patella replacement and lateral retinaculum release for patella subluxation.
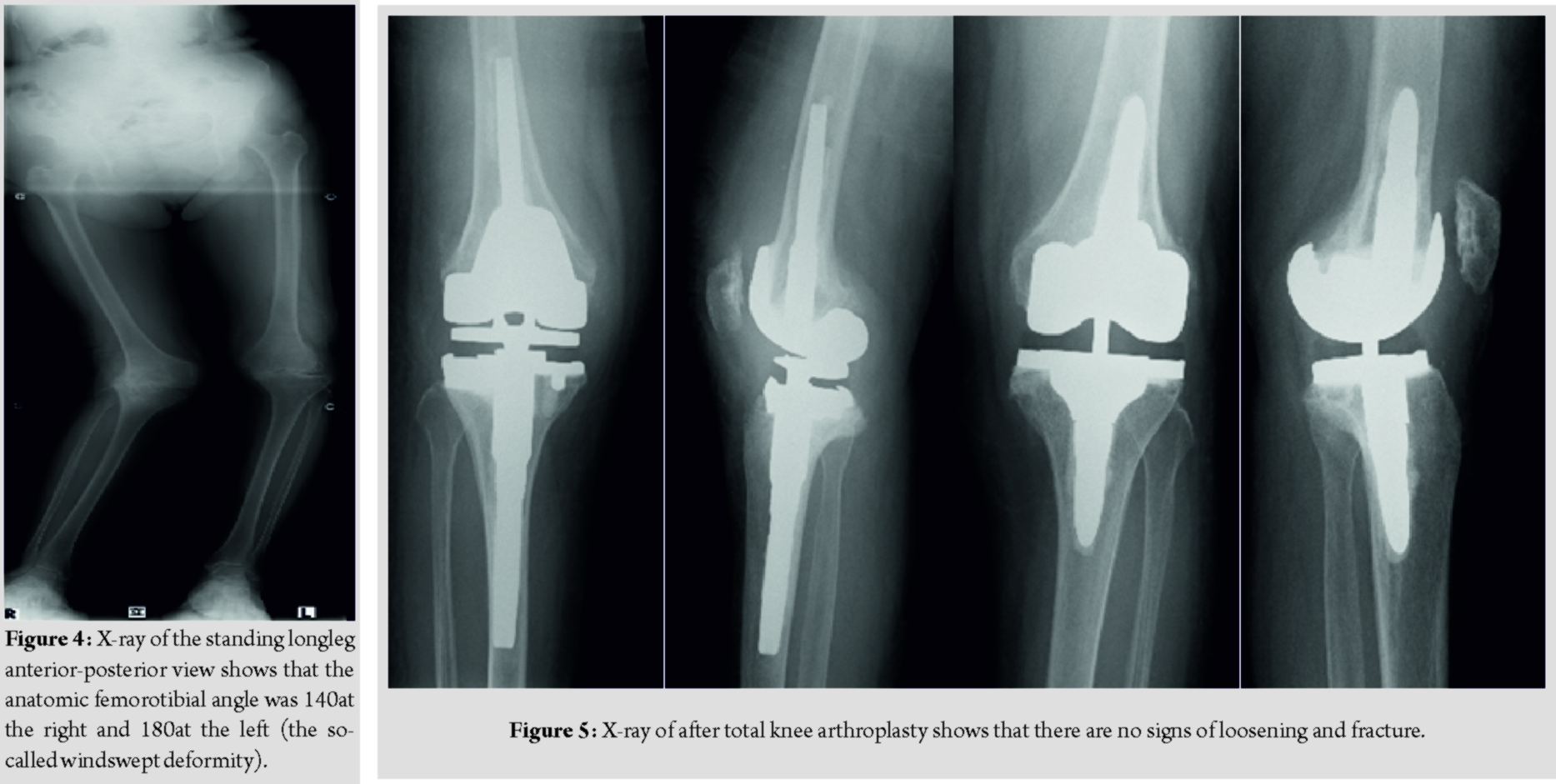
She demonstrated right drop foot immediately after the first operation. We prescribed an ankle–foot orthosis for her right ankle and started her rehabilitation therapy. The muscle power of her tibialis anterior slowly improved (MMT 3) over 3 months postoperatively. The active range of motion of the right knee was 5–95. However, the patient was unable to walk because of the left knee instability. We decided to then perform TKA for the left knee. We selected a constrained condylar prosthesis (Triathlon TS; Stryker, Mahwah, NJ, USA) using the same approach as in the first surgery. Intraoperatively, we removed a large loose body that was found in the suprapatellar pouch and performed a lateral retinaculum release and patella replacement. The active range of motion of the left knee was 0–95 and the patellar tracking was good. At the time of the 6-month follow-up, both knees were stable and in good alignment. There were no signs of loosening or fracture (Fig. 5). The patient experienced no pain and was able to ambulate throughout her house with a walker.
Discussion
The pathophysiology of Charcot arthropathy has not been well described. One theory implies that the patient’s decreased nociceptive response due to neuropathy may cause repeated undetected microtrauma, resulting in joint destruction [2]. The other theories suggest that motor neuropathy may result in ligament laxity and decreased muscle tone, and autonomic neuropathy may result in increased blood flow to joints causing bone resorption and subsequent osteopenia [3]. Baumhauer et al. reported inflammatory cytokines, such as tumor necrosis factor-α and interleukin-1, as stimulating osteoclast formation, resulting in bone resorption and weakening [4]. Syphilis used to be a major cause of Charcot joint, but its incidence is now declining with the increased use of antibiotics. Today, diabetes mellitus is its most common cause. Many other diseases including alcoholism, syringomyelia, and hereditary neuropathy (e.g., Charcot-Marie-Tooth disease) are still well-known causes of Charcot joints. Paliwal et al. reported that Charcot arthropathy could be seen even after spinal anesthesia procedures [5]. The mainstay treatments of Charcot knee are conservative management, arthrodesis, and arthroplasty. Conservative management is non-weight-bearing and elimination of joint movement through a brace. A non-weight-bearing period of 3 months has been recommended [6]. The classical surgical treatment is arthrodesis [7]. Arthroplasty has been considered an absolute contraindication [1]. With the development of prostheses and surgical techniques, orthopedic surgeons have a greater opportunity to perform TKA to treat Charcot knee. Prosthesis selection is understandably important, but there is no clear consensus about it. Long-stem components should be used on the femoral and tibial sides [8]. TKA using constrained condylar or rotating hinge prosthesis was reportedly effective for Charcot knee [9], and the latter should be selected for patients with severe deformity or instability [9, 10]. Surgeons must achieve both appropriate alignment and ligament stability to increase prosthesis longevity. Realignment of the Charcot knee joint usually requires lateral release. Tibial tubercle transfer may be needed in some cases [3]. Because bone defects are present in approximately 90% of Charcot knees, bone grafting, either autologous or synthetic, or custom augmentation may be needed [11]. The patella should also be replaced [11]. The outcome of TKA for Charcot knee is poorer than that of primary TKA for osteoarthritis (OA). Tibbo et al. reported that the 10-year rate of survivorship free of aseptic revision was 88%, while that free of any revision was 70% [12]. There is a high perioperative complication rate of TKA for Charcot knee of approximately 50%, including dislocations, periprosthetic fractures, instability, deep venous thrombosis, and infection [3]. This is remarkably higher than that of arthroplasty performed for OA. Thus, the surgical indication of TKA for Charcot knee should be carefully considered. In our case, it was difficult to probe the cause of the Charcot arthropathy. We could exclude diabetes and syphilis by blood examination and alcoholism by her medical history. Because we could not perform magnetic resonance imaging of her head and neck due to the patient claustrophobia, syringomyelia and hereditary neuropathy could not be excluded from the study. Although the patient’s movement disorder was mild, her sensory loss in the lower limbs was severe, especially in regions innervated predominantly by the L5 and S1 nerve roots. In addition, she had no symptoms in the upper limbs. Therefore, we suggested that Charcot knee might be caused by lumbar radiculopathy. Although the patient could not walk due to bilateral knee instability, we did not perform simultaneous bilateral TKA because of its high complication rate. We selected a rotating hinge prosthesis for the right TKA by a combination of autologous bone graft and metal tibial block augmentation. We also added lateral release and patellar replacement due to the severe tibial bone defect and lateral patella subluxation. The post-operative drop foot might have been caused by peroneal nerve palsy related to the modification of the severe valgus deformity. We decided to perform TKA of the opposite knee after having a careful discussion with the patient and her family. We selected a constrained condylar prosthesis for the left TKA because the bone defect and alignment were not severe. Neither an autologous bone graft nor a metal tibial block augmentation was needed.
Conclusion
Here, we reported on a case of staged bilateral TKA in a patient with bilateral Charcot knees. Careful follow-up is needed, but TKA can show good outcomes in the management of patients with Charcot knee joints.
Clinical Message
Charcot arthropathy causes severe progressive and destructive joint disease. TKA using constrained condylar or rotating hinge prosthesis by a combination of autologous bone graft and metal tibial block augmentation and lateral release and patellar replacement can show good outcomes in the management of patients with Charcot knee joints.
References
1. Marmor L. The Marmor knee replacement. Orthop Clin North Am 1982;13:55-64.
2. GuptaR. A short history of neuropathic arthropathy.Clin OrthopRelat Res1993;296:43-9.
3. BabazadehS, StoneyJD, LimK, ChoongPF. Arthroplasty of a Charcot knee.Orthop Rev (Pavia)2010;2:e17.
4. BaumhauerJF, O’KeefeRJ, SchonLC, PinzurMS. Cytokine-induced osteoclastic bone resorption in charcot arthropathy: An immunohistochemical study.Foot Ankle Int2006;27:797-800.
5. PaliwalVK, SinghP, RahiSK, AgarwalV, GuptaRK. Charcot knee secondary to lumbar spinal cord syringomyelia: Complication of spinal anesthesia.J Clin Rheumatol2012;18:207-8.
6. LeeL, BlumePA, SumpioB. Charcot joint disease in diabetes mellitus.Ann Vasc Surg2003;17:571-80.
7. DrennanDB, FaheyJJ, MaylahnDJ. Important factors in achieving arthrodesis of the Charcot knee.J Bone Joint Surg Am1971;53:1180-93.
8. YoshinoS, FujimoriJ, KajinoA, KiowaM, UchidaS. Total knee arthroplasty in Charcot’s joint.J Arthroplasty1993;8:335-40.
9. MorganH, BattistaV, LeopoldSS. Constraint in primary total knee arthroplasty.J Am AcadOrthop Surg2005;13:515-24.
10. ZengM, XieJ, HuY. Total knee arthroplasty in patients with Charcot joints.Knee Surg Sports TraumatolArthrosc2016;24:2672-7.
11. ParviziJ, MarrsJ, MorreyBF. Total knee arthroplasty for neuropathic (Charcot) joints.Clin OrthopRelat Res2003;416:145-50.
12. Tibbo ME, Chalmers BP, Berry DJ. Primary total knee arthroplasty in patients with neuropathic (Charcot) arthropathy: Contemporary results. J Arthroplasty 2018;33:2815-20.
 |
 |
 |
 |
 |
| Dr. Ryo Yoshikawa | Dr. Atsushi Kitagawa | Dr. Takao Inokuchi | Dr. Naoko Shima | Dr. Yasushi Hashimoto |
| How to Cite This Article: Yoshikawa R, Kitagawa A, Inokuchi T, Shima N, Hashimoto Y. Staged Bilateral Total Knee Arthroplasty in a Patient with Charcot Knees: A Case Report. Journal of Orthopaedic Case Reports 2020 Mar-Apr;10(2): 9-12. |
[Full
Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




