Hanky in the Pocket Dural Inlay Technique is a simple and effective tool to manage incidental dural tears in Unilateral Biportal Endoscopic Spine Surgery.
Dr. Atmaranjan Dash, Department of Neurosurgery and Spine Surgery, Care Hospitals, Bhubaneshwar, Odisha, India. E-mail: atmanranjan@gmail.com
Introduction: Unilateral biportal endoscopy (UBE) is a novel technique for spine surgeries gaining popularity in recent times. Being minimally invasive, certain complications, such as dural tears can be difficult to manage due to restricted access. Incidental dural tears are common during endoscopic spine surgery and various techniques, such as application of fibrin sealant, non-penetrating dural clips, pressure with gelfoam and conversion to minimally invasive or open surgery have been described for the management. This study aims to describe the “Hanky in the Pocket” Technique with collagen matrix inlay to manage incidental dural tears during UBE spine surgery.
Case Series: We present a prospective case series of five patients with dural tears <4 mm during UBE spine surgery for the lumbar spine managed intra operatively with the aforementioned technique. All five patients achieved the Minimal Clinically Important Difference cutoff for visual analog scale (VAS) leg pain, VAS low back ache and Oswestry Disability Index Score at the end of 3 months of surgery. No complications of cerebrospinal fluid leak or neurodeficits were encountered with this technique based on a follow-up of 1 year.
Conclusion: “Hanky in the Pocket” Technique with collagen matrix inlay is a safe and effective technique for the management of incidental small dural tears. Importantly, it is less time consuming, avoids conversion to open surgery and demonstrates a good functional outcome.
Keywords: Dural tear, dural inlay technique, hanky in the pocket technique, dural augmentation, unilateral biportal endoscopy.
Unilateral biportal endoscopy (UBE) is a minimally invasive novel surgical substitute to open spine surgery due to its explorative ability, minimal incision size, minimal muscle damage, and less blood loss, which finally contribute to faster post-operative recovery [1].
Monoportal and Biportal endoscopy are the two prevalent surgical options for endoscopic spine surgery. Advantages of Biportal surgery over Monoportal include the usage of a larger high definition camera, larger working instruments, and separate viewing and working portals. Independent portals lead to a lack of interference between the scope and instruments, which provides a wide explorative capability of this technique. Diverse spine pathologies, including intervertebral disc prolapse, moderate-to-severe spinal canal stenosis, and spondylolisthesis requiring interbody fusion, can be addressed by UBE [2].
However, as no procedure is devoid of complications, a few notable complications of UBE are dural tears, epidural hematoma, nerve root injury, and infection [3]. Incidental dural tears are a common complication in lumbar endoscopic spine surgery. The Incidence of dural tears is reported to be around ≤8.6% during endoscopic surgery [4,5]. Sequelae of dural tears include persistent cerebrospinal fluid leaks, pseudomeningoceles and cutaneous fistulas [6,7]. More severe complications, such as nerve root entrapment [8], meningitis [9] and surgical site infections have been reported.
Although there are studies mentioning about the incidence of dural tears in minimally invasive spine surgery, literature on dural tears in UBE surgery is sparse [10]. Conversion to open surgery can be an option although many surgeons avoid it due to the morbidity and increased operative time [11]. Modalities for the management of dural tear include fibrin sealant gel, pressure with gelfoam, collagen inlay substitute and non-penetrating dural clips to name a few [11,12].
In this study, we present a case series and a technical note on collagen matrix dural inlay substitute “hanky in the pocket” technique for the management of incidental dural tears during UBE spine surgery which provides excellent post-operative outcomes.
Study design and participants
This is a prospective Case Series in which a total of 336 patients were operated for degenerative moderate to severe lumbar canal stenosis through UBE. All surgeries were performed by a single surgeon at Care hospitals, Bhubaneswar, India during January 2023–January 2024 and followed up periodically 2 weeks, 4 weeks, 6 weeks and 3 months post-operatively. Follow-up for complications was done up to 1-year post-surgery. We encountered 5 cases with incidental intraoperative Dural tears. Approval was obtained by the Hospital Ethical Committee. All Dural tears were <4 mm in length and were managed by collagen matrix inlay “Hanky in the Pocket” Technique (Duragen).
Scores were generated for the pre-operative and 3 months post-operative Oswestry Disability Index (ODI) and visual analog scale (VAS) for leg and low back pain to assess patient-reported outcomes. The scores were evaluated to determine if they satisfied the minimum clinically significant difference (MCID). Depending on the calculating method, the definition of MCID changes. Leg pain improvement of at least 1.6 points, a low back pain improvement of at least 1.2 points, and an ODI improvement of at least 12.8 points were selected as the study’s MCIDs [13].
Surgical technique (Figs. 1 and 2)
Identification of the dural tear
In our study midline or paramedian dural tears were encountered most commonly due to the indentation of sharp bone edges during use of micro chisel or due to usage of Kerrisons while excising ligamentum flavum in severe canal stenosis. We classified posterior dural tears according to their anatomical location as Midline tears, Paramedian tears, Peri Shoulder tears, Peri Axillary tears, and Peri traversing root dural tears. In 3 cases, the nerve roots were contained within the Dura. In 2 cases we encountered extravasation of nerve roots. No pressure changes were made to the irrigation fluid.
Reduction of herniated nerve roots
A single attempt of reduction of nerve roots was given failing which, an onlay patch is applied to secure the roots and complete decompression of the spinal canal is completed to reduce pressure on the thecal sac. Reduction of roots was then performed after spinal decompression. We prefer to use a fine blunt ball point nerve hook to carefully reduce the nerve roots with gentle pushing movements toward the thecal sac.
Sizing the dural tear
Akin to the popular quote that objects in the mirror are closer than they appear, Dural tears in biportal endoscopy appear larger than actual due to magnification and high resolution of the endoscope. To avoid overestimation of the dural tear size, we use customized nerve hooks of different sizes which help us to approximately size the dural tear both longitudinally and horizontally under endoscopic vision.
Sizing the collagen inlay substitute
The size of the collagen inlay substitute is approximately 30% more than the size of the dural tear. A slightly larger substitute is preferred as a circumferential rim of the substitute is over the intact dura. Very large sized substitute will lead to difficulty in introduction whereas a small sized substitute will not seal the dural defect and lead to root extravasation.
Placement of collagen inlay graft
The ideal size of the collagen inlay substitute is prepared and inserted into the working portal over the dural tear. Using a blunt ball point nerve hook, the substitute is slowly and gently teased into the dural tear on all sides until it gets incorporated into the thecal sac forming a “seal” restricting root herniation. The Dural Tear is analyzed as a pocket of potential space with nerve roots and the collagen inlay dural substitute is akin to a handkerchief which is slid into pocket hence the name “hanky in the pocket” technique.
Low-energy radiofrequency ablation of the dural rent
This helps to shrink the dural defect and compact the inlay substitute.
Irrigation fluid is drained and the minivac drain is applied without suction. Closure is done in a standard manner. All patients were mobilized within 6 h post-surgery.
We have devised the Hanky in the pocket technique for the management of small dural tears in UBE Spine Surgery (Fig. 3). At present, the literature on the technical aspects of dural inlay technique especially in UBE spine surgery is sparse. We aim to provide a simplified step by step technical note on the same for meticulous and easy execution by endoscopic spine surgeons. However, certain techniques, such as patch repair, patch compression with Gelfoam and Tachosil have been described previously [14].
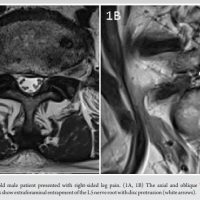
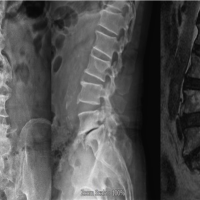
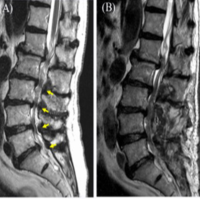
We present one of our five cases here. A 65 year old Male with presented to the Outpatient Department with severe low back pain and neurogenic claudication since 4 years. On examination, tenderness was noted over lower back with no neurological deficit. Claudication distance was 100 m. Magnetic resonance imaging (MRI) revealed L4-L5 severe lumbar canal stenosis with ligamentum flavum and bilateral facetal hypertrophy. The surgical plan was to perform a L4-L5 transforaminal lumbar interbody fusion (TLIF) and thorough decompression with UBE. However, intraoperatively there was an incidental dural tear in the midline while excising the ligmentum flavum with a Kerrison Rongeur. A few roots were found to be extruding from the dural defect which was around 3 mm in size. Intraoperative management of the dural defect was done with a collagen matrix inlay technique as described in the surgical technique. The patient was mobilized immediately after 6 h of surgery and the drain was removed after 2 days. Repeat MRI was considered only if red flag signs attributable to cerebrospinal fluid (CSF) leak were present, including persistent postural headache, nausea/vomiting, dizziness, blurring of vision, swelling over operative site, and fistulation. On sequential follow-up for 3 months, the patient demonstrated a clinically significant reduction in the VAS scores and ODI score with no complications of CSF leak and neurodeficit.
A total of five patients were included in the study, with 3 males and 2 female patients. All patients were diagnosed to have moderate to severe lumbar canal stenosis. No patients had a previous lumbar spine surgery in the past. All patients were operated in the prone position via an interlaminar approach with UBE under general anesthesia.
Operating time ranged from 93 to 162 min with an average of 151 min for a single level of UBE TLIF and 79 min per level of decompression. All Dural tears were <4 mm than size and two cases had herniation of nerve roots. No cases of dural injury with a high speed burr were noted as we use a diamond bit (Table 1 and 2).
The average duration of hospital stay post-surgery was 2.4 days. All patients were mobilized within 6 h of surgery. Criteria for drain removal was <10 mL of collection. Drain was removed by the end of post-operative day 1. No signs or symptoms of post-operative CSF leak were noted in all the patients. All five patients achieved the MCID cutoff for VAS leg pain, VAS low back ache and ODI Score at the end of 3 months of surgery (Table 3, 4, 5. At the end of 1 year of follow-up, no dural leak or neurodeficits were encountered.
Although incidental dural tears are a known complication of endoscopic spine surgery, the incidence is around 1.48% in our study, which is lesser than other reports [13].
In our experience, certain risk factors for iatrogenic dural tear include severe canal stenosis, use of Kerrisons for piecemeal removal of ligamentum flavum, bony indentation on dura while using micro chisel or osteotome, and thin Dura, which is consistent to the study done by Park et al. [12]. With reference to moderate to severe lumbar canal stenosis, the adhesions between the degenerated facet capsule and the hypertrophied ligamentum flavum to the dura mater pose a higher risk for dural tears during decompression of the spinal canal and lateral recess. In addition, Elderly patients have a combination of a fragile dura and multilevel lumbar disc degeneration, which in turn imply a greater risk for iatrogenic dural tears than usual. As UBE has a considerable learning curve, surgeon’s inexperience, blurry field due to poor hemostasis and unfamiliar endoscopic anatomy contribute to intraoperative complications [13].
In this technique, the CSF pressure seals the closure created by the dural inlay substitute, by within preventing herniation of nerve roots (Fig. 4). Multiple attempts, prolonged attempts and forceful maneuvers of reduction of extravasated roots into the thecal sac are a risk for root injury and neurological deficits [11]. Operative time after an incidental dural tear should not be prolonged as the influx of irrigation fluid into the thecal sac can lead to increased intracranial pressure [13].
Studies on the management of dural tears in biportal endoscopic spine surgery are limited. In a case series by Derman et al., three patients with incidental dural tears post-full endoscopic spine surgery treated with collagen matrix inlay substitute reported a good post-operative functional outcome and avoidance of prolonged bed rest. No complications further complications were reported on further follow-up consistent to the findings of our study [11].
Since UBE is a saline-based endoscopic procedure, the presence of fluid around the operative site in the immediate post-operative phase is expected, which makes it difficult to distinguish between a true pseudomeningocele suggestive of a CSF leak and a collection of retained saline during surgery [15]. This limitation makes the MRI findings technically inconclusive in the immediate phase and, hence, not emphasized in our study. The strength of our study lies in the fact that all dural tears encountered were well managed with collagen inlay substitute technique resulting in a good post-operative outcome and no complications.
Our study has certain limitations. All surgeries were performed at a single center and by a single surgeon with a maximum long-term follow-up of 1 year. We never encountered large dural tears beyond 4 mm and no other repair techniques were employed for comparison.
The best strategy for a dural tear is to prevent its occurrence. A pre-operative computed tomography scan enables the surgeon to visualize areas of calcification of the ligamentum flavum and make a safe operative plan as it is found that calcification correlates to increased risk for dural tears [12].
Techniques, such as dural repair and fibrin glue sealant can be cumbersome and lead to increased operative time [16]. UBE is a versatile procedure as a variety of instruments can be used, including most of them used for open spine surgery. The magnification and detailed visualization it offers leads to a clear visual monitioring of the neural structures. However, certain shortcomings include difficulty in hemostasis and longer operative time in beginner surgeons [12]. Based on our experience, we present an algorithm to manage small incidental dural tears (Table 6). The Strength of our study includes a single center and a single surgeon study, follow-up up to 1 year and a simplified, reproducible, step by step technique. Limitations include lack of control or comparison group and non-applicability of the technique for larger dural tears. However, our research on the technique and follow-up is being continued on a larger sample size for standardization.
Incidental dural tears <4 mm during UBE spine surgery are a common complication which can be effectively managed with collagen inlay substitutes as described by Hanky in the Pocket Technique. In our case series, we demonstrate a good post-operative functional outcome without the need to convert to open spine surgery intraoperative. Hanky in the pocket technique is simple and less time consuming for the management of small dural tears without complications. Continued research on a larger sample size is needed to standardize the protocol for management of incidental dural tears in UBE spine surgery.
UBE is a novel minimally invasive technique for spine surgeries, gaining popularity in recent years. However, complications, such as dural tears, can be fairly common in cases of severe stenosis, inexperienced surgeon, and improper instrumentation and so forth. Managing dural tears on table can be a challenging task due to restricted access and continuous saline flow over surgical field. Hanky in the pocket dural inlay technique is simple and fast for small dural tears, helps to seal the dural rent and prevents extravasation of roots. Importantly, it avoids the conversion to open spine surgery and offers a good functional outcome. We suggest all endoscopic spine surgeons to keep this technique in their armamentarium to manage incidental dural tears.
References
- 1. Kim SK, Kang SS, Hong YH, Park SW, Lee SC. Clinical comparison of unilateral biportal endoscopic technique versus open microdiscectomy for single-level lumbar discectomy: A multicenter, retrospective analysis. J Orthop Surg Res 2018;13:22. [Google Scholar] [PubMed]
- 2. Lin GX, Kotheeranurak V, Mahatthanatrakul A, Ruetten S, Yeung A, Lee SH, et al. Worldwide research productivity in the field of full-endoscopic spine surgery: A bibliometric study. Eur Spine J 2020;29:153-60. [Google Scholar] [PubMed]
- 3. Wang B, He P, Liu X, Wu Z, Xu B. Complications of unilateral biportal endoscopic spinal surgery for lumbar spinal stenosis: A systematic review of the literature and meta-analysis of single-arm studies. Orthop Surg 2023;15:3-15. [Google Scholar] [PubMed]
- 4. Ahn Y, Lee HY, Lee SH, Lee JH. Dural tears in percutaneous endoscopic lumbar discectomy. Eur Spine J 2011;20:58-64. [Google Scholar] [PubMed]
- 5. Tsutsumimoto T, Yui M, Uehara M, Ohta H, Kosaku H, Misawa H. A prospective study of the incidence and outcomes of incidental dural tears in microendoscopic lumbar decompressive surgery. Bone Joint J 2014;96-B:641-5. [Google Scholar] [PubMed]
- 6. Cammisa FP Jr., Girardi FP, Sangani PK, Parvataneni HK, Cadag S, Sandhu HS. Incidental durotomy in spine surgery. Spine (Phila Pa 1976) 2000;25:2663-7. [Google Scholar] [PubMed]
- 7. Guerin P, El Fegoun AB, Obeid I, Gille O, Lelong L, Luc S, et al. Incidental durotomy during spine surgery: Incidence, management and complications. A retrospective review. Injury 2012;43:397-401. [Google Scholar] [PubMed]
- 8. Nishi S, Hashimoto N, Takagi Y, Tsukahara T. Herniation and entrapment of a nerve root secondary to an unrepaired small dural laceration at lumbar hemilaminectomies. Spine (Phila Pa) 1976;20:2576-9. [Google Scholar] [PubMed]
- 9. Lin TY, Chen WJ, Hsieh MK, Lu ML, Tsai TT, Lai PL, et al. Postoperative meningitis after spinal surgery: A review of 21 cases from 20,178 patients. BMC Infect Dis 2014;14:220. [Google Scholar] [PubMed]
- 10. Park JH, Jun SG, Jung JT, Lee SJ. Posterior percutaneous endoscopic cervical foraminotomy and diskectomy with unilateral biportal endoscopy. Orthopedics 2017;40:e779-83. [Google Scholar] [PubMed]
- 11. Derman PB, Rogers-LaVanne MP, Satin AM. Collagen matrix inlay graft for management of incidental durotomy during full-endoscopic lumbar Spine surgery: Technique and case series. Int J Spine Surg 2023;17:399-406. [Google Scholar] [PubMed]
- 12. Park HJ, Kim SK, Lee SC, Kim W, Han S, Kang SS. Dural tears in percutaneous biportal endoscopic spine surgery: Anatomical location and management. World Neurosurg 2020;136:e578-85. [Google Scholar] [PubMed]
- 13. Yu H, Zhao Q, Lv J, Zhu B, Chen L, Jing J, et al. Unintended Dural tears during unilateral biportal endoscopic lumbar surgery: Incidence and risk factors. Acta Neurochir (Wien) 2024;166:95. [Google Scholar] [PubMed]
- 14. Kim JE, Choi DJ, Park EJ. Risk factors and options of management for an incidental Dural tear in biportal endoscopic spine surgery. Asian Spine J 2020;14:790-800. [Google Scholar] [PubMed]
- 15. Yang L, Yu T, Jiao J, Hou T, Wang Y, Zhao B, et al. Comprehensive analysis of UBE-related complications: Prevention and management strategies from 4685 patients. Med Sci Monit 2024;30:e944018. [Google Scholar] [PubMed]
- 16. Kothe R, Quante M, Engler N, Heider F, Kneißl J, Pirchner S, et al. The effect of incidental Dural lesions on outcome after decompression surgery for lumbar spinal stenosis: Results of a multi-center study with 800 patients. Eur Spine J 2016;26:2504-11. [Google Scholar] [PubMed]