Emerging techniques like simulation-based learning, VR/AR, flipped classrooms, and problem-based learning are revolutionizing orthopedic education, enhancing technical skills, knowledge retention, and clinical preparedness.
Dr. Madhan Jeyaraman, Department of Orthopaedics, ACS Medical College and Hospital, Dr MGR Educational and Research Institute, Chennai, Tamil Nadu, India. E-mail: madhanjeyaraman@gmail.com
Medical education has undergone a significant transformation, with orthopedic training evolving to meet the demands of modern healthcare. While traditional teaching methods, including lectures and direct patient interactions, remain fundamental, they often fall short in providing real-time feedback and sufficient hands-on practice, highlighting the need for more effective training approaches [1]. The incorporation of simulation-based learning, virtual reality (VR), augmented reality, and problem-based learning (PBL) has introduced interactive and immersive educational environments, reshaping orthopedic training [2,3,4]. Acquiring proficiency in orthopedic procedures requires extensive hands-on experience, which conventional training methods may not adequately provide. The constraints of clinical practice limit repeated procedural training, making skill acquisition challenging. Innovations such as 3D-printed anatomical models and VR-based simulations offer trainees the opportunity to refine their surgical techniques in a controlled, risk-free setting, thereby enhancing both technical skills and anatomical comprehension [5,6,7]. These advancements help bridge the gap between theoretical learning and practical application, ensuring that trainees gain exposure to the latest surgical methods and treatment strategies.
This editorial examines the emerging teaching methodologies in orthopedics, emphasizing their impact on training efficiency and clinical preparedness. By integrating modern pedagogical techniques with advanced technology, these innovations contribute to improved learning outcomes and equip future orthopedic surgeons with the necessary expertise to navigate contemporary medical challenges.
Simulation-based learning
Simulation-based learning utilizes high-fidelity simulators and VR platforms to recreate surgical environments, enabling medical trainees to practice intricate procedures in a risk-free setting [8,9,10]. These advanced tools replicate real-life scenarios, providing hands-on experience coupled with immediate feedback. In orthopedics, common applications include virtual knee replacement training, spine surgery simulations, and arthroscopy skill development. Key advantages of simulation-based learning include:
a. Realistic practice without risk – Trainees can repeatedly perform procedures without posing any risk to patients, thereby enhancing proficiency in high-risk surgeries
b. Enhanced technical skill development – Continuous exposure to simulated procedures allows for refinement of surgical techniques, particularly in joint replacements and spinal interventions c. Improved knowledge retention – Active learning, reinforced by real-time feedback, strengthens the understanding and retention of surgical concepts and procedural steps. Traditional teaching methods rely heavily on clinical exposure, which may be inconsistent, whereas simulation-based learning accelerates skill acquisition through structured and repetitive practice. By offering a controlled environment for repeated procedural training, simulation enhances surgical precision and technical competency [11]. Engaging in interactive simulations fosters better knowledge retention through active participation and systematic feedback. Unlike conventional methods that depend on patient availability, simulation ensures unlimited practice opportunities, making it a revolutionary tool in orthopedic education [12,13,14].
The flipped classroom model is a modern pedagogical approach that restructures traditional teaching by delivering instructional content outside the classroom, often through online pre-recorded lectures [15]. In orthopedics, this method has proven particularly beneficial, allowing trainees to study complex surgical techniques, anatomical structures, and disease processes at their own pace before engaging in interactive classroom discussions [16,17]. This approach fosters collaboration among students while enabling instructors to provide targeted guidance on challenging concepts and technical skills. Key advantages of the flipped classroom model include:
- Increased student engagement – By shifting the responsibility of initial learning outside the classroom, students become more actively involved with the material, leading to better focus and participation in discussions
- Deeper understanding of material – With the opportunity to review and analyze content beforehand, students enter the classroom with a solid foundational knowledge, allowing for more meaningful discussions and hands-on applications
- Better retention of complex topics – Given the intricate nature of medical and orthopedic education, repeated exposure through this model enhances long-term retention of concepts more effectively than traditional lecture-based methods.
Studies have shown that the flipped classroom significantly improves engagement levels, with students demonstrating an 85% participation rate compared to 55% in conventional lecture settings. Additionally, comprehension of orthopedic topics is higher (90%) among students in flipped classrooms versus 60% in traditional teaching environments. Retention of key orthopedic concepts also increases to 85% with active learning and repeated exposure, compared to 65% in standard lectures. This teaching strategy is revolutionizing orthopedic education by promoting active learning, deeper comprehension, and improved skill retention, making it an essential tool for training future orthopedic surgeons [18].
PBL is a student-centered educational approach that promotes active learning through the analysis and resolution of real-world clinical problems in small groups [19]. This method presents students with complex clinical scenarios, requiring them to collaboratively assess, discuss, and devise management strategies. In orthopedic education, case scenarios range from simple fractures to intricate joint reconstructions and spinal procedures. PBL encourages the integration of theoretical knowledge from anatomy, pathology, biomechanics, and surgical techniques, effectively bridging the gap between conceptual learning and clinical application [4]. Key advantages of the PBL model include:
- Development of problem-solving skills – By systematically evaluating orthopedic cases, students learn to break down complex clinical challenges and formulate logical, evidence-based treatment solutions
- Enhanced decision-making capabilities – Through PBL, students engage in structured decision-making exercises, exploring various treatment options in controlled, high-pressure surgical settings
- Improved teamwork and collaboration – PBL fosters a collaborative environment, enhancing communication, leadership, and mutual respect – skills that are essential for successful orthopedic practice.
Studies indicate that students engaged in PBL exhibit significantly higher problem-solving proficiency (85%) compared to those in traditional learning environments (60%). In addition, PBL-trained students demonstrate greater accuracy in diagnosing orthopedic conditions (90%) versus those using conventional teaching methods (65%). The team-based structure of PBL further enhances collaboration, with students reporting stronger teamwork skills (90%) compared to those in traditional settings (70%). By fostering critical thinking, improving diagnostic abilities, and encouraging teamwork, PBL is playing a pivotal role in modern orthopedic education [20].
Peer teaching and collaborative learning are interactive educational strategies that enhance orthopedic training by emphasizing active participation and teamwork [13,21]. In peer teaching, students take on the role of instructors, assisting their peers or junior learners in understanding complex topics [22]. Conversely, collaborative learning involves group-based exercises where students from various medical disciplines work together to analyze and solve clinical problems [21]. The key benefits of peer teaching and collaborative learning include:
- Reinforcement of knowledge – Teaching requires students to systematically structure and convey their understanding, thereby deepening their comprehension of intricate orthopedic concepts
- Enhanced communication skills – Both approaches necessitate clear and effective communication. Peer instructors refine their ability to explain difficult topics, while collaborative learning encourages students to articulate ideas and engage in meaningful discussions
- Leadership development – Peer teaching provides opportunities for students to take on leadership roles, guiding their peers and fostering responsibility in the learning process
- Strengthened critical thinking and problem-solving abilities – Team-based discussions and clinical scenario analyses in collaborative learning enhance critical thinking, which is crucial for orthopedic decision-making and surgical proficiency.
By promoting knowledge retention, leadership, and critical thinking, these strategies contribute to a more interactive and engaging orthopedic learning experience Table 1.
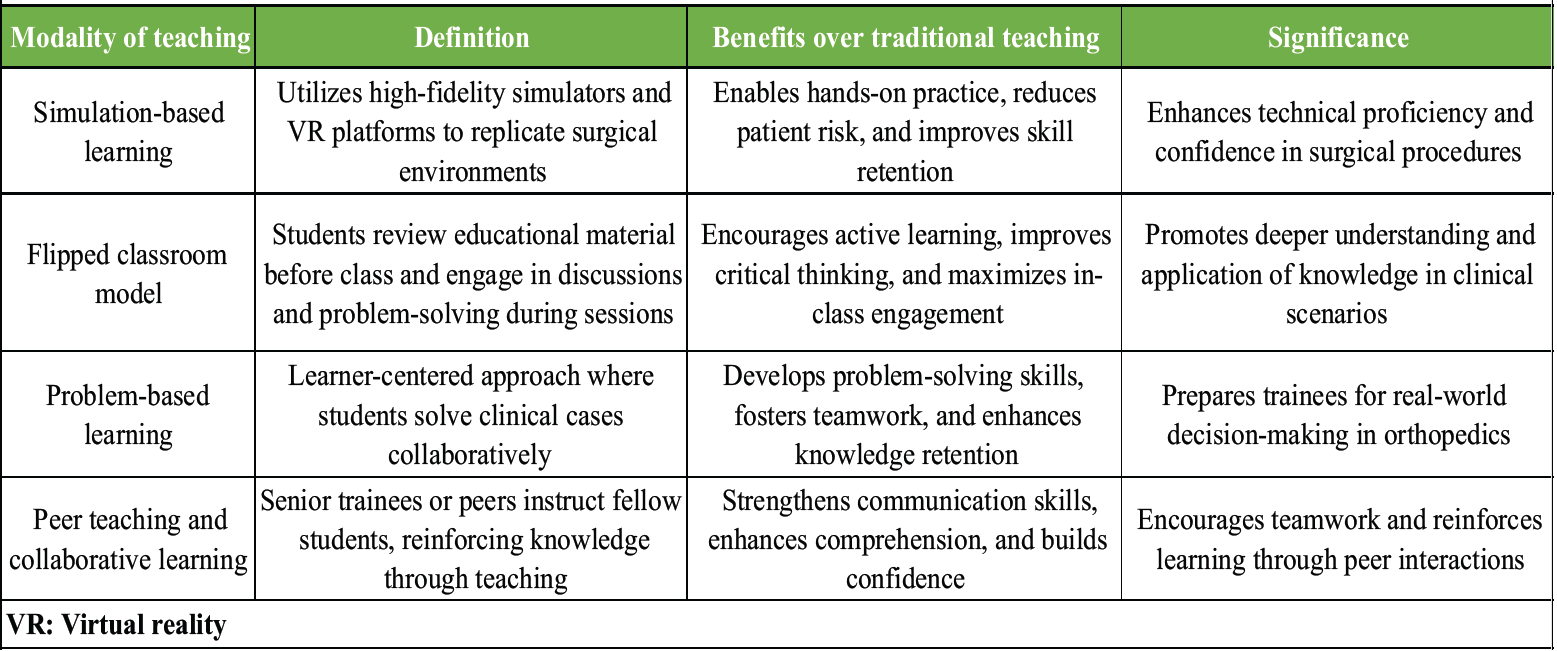
Table 1: Summary of advancements in orthopedic teaching and learning
Advancements in orthopedic education have shifted the focus from passive learning to active, student-centered methodologies that enhance skill acquisition, critical thinking, and interdisciplinary collaboration. However, challenges such as financial constraints, resistance to curricular changes, and the need for faculty training hinder widespread implementation. As medical education continues to evolve, integrating innovative teaching strategies will be instrumental in shaping the next generation of orthopedic professionals, ultimately leading to improved patient care and surgical outcomes.
• Simulation-based learning improves technical skills and knowledge retention by offering risk-free, hands-on practice with realistic scenarios, enhancing clinical preparedness
• Flipped classroom model promotes active student engagement and deepens understanding of complex orthopedic concepts by shifting instructional content outside the classroom and focusing on collaborative, in-class problem-solving
• PBL enhances problem-solving and decision-making skills, teamwork, and communication by engaging students in analyzing and solving real-world clinical cases.
References
- 1. Challa KT, Sayed A, Acharya Y. Modern techniques of teaching and learning in medical education: A descriptive literature review. MedEdPublish 2021;10:18. [Google Scholar] [PubMed]
- 2. Crogman HT, Cano VD, Pacheco E, Sonawane RB, Boroon R. Virtual reality, augmented reality, and mixed reality in experiential learning: Transforming educational paradigms. Educ Sci 2025;15:303. [Google Scholar] [PubMed]
- 3. Shah SF, Mazhar T, Shahzad T, khan MA, Ghadi YY, Hamam H. Integrating educational theories with virtual reality: Enhancing engineering education and VR laboratories. Soc Sci Humanit Open 2024;10:101207. [Google Scholar] [PubMed]
- 4. Li T, Song R, Zhong W, Liao W, Hu J, Liu X, et al. Use of problem-based learning in orthopaedics education: A systematic review and meta-analysis of randomized controlled trials. BMC Med Educ 2024;24:253. [Google Scholar] [PubMed]
- 5. Shahrezaei A, Sohani M, Taherkhani S, Zarghami SY. The impact of surgical simulation and training technologies on general surgery education. BMC Med Educ 2024;24:1297. [Google Scholar] [PubMed]
- 6. Jiang Y, Jiang H, Yang Z, Li Y. The current application of 3D printing simulator in surgical training. Front Med (Lausanne) 2024;11:1443024. [Google Scholar] [PubMed]
- 7. Riddle EW, Kewalramani D, Narayan M, Jones DB. Surgical simulation: Virtual reality to artificial intelligence. Curr Probl Surg 2024;61:101625. [Google Scholar] [PubMed]
- 8. Woodward CJ, Khan O, Aydın A, Dasgupta P, Sinha J. Simulation-based training in orthopedic surgery: A systematic review. Curr Probl Surg 2025;63:101676. [Google Scholar] [PubMed]
- 9. Khajuria A, Mathew J Jr. Simulation training and skill assessment in orthopedic surgery. In: StatPearls. StatPearls Publishing; 2025. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559080 [Google Scholar] [PubMed]
- 10. Iqbal MH, Khan O, Aydin A. Editorial commentary: Simulation-based training in orthopaedic surgery: Current evidence and limitations. Arthrosc J Arthrosc Relat Surg 2021;37:1008-10. [Google Scholar] [PubMed]
- 11. Luzzi A, Hellwinkel J, O’Connor M, Crutchfield C, Lynch TS. The efficacy of arthroscopic simulation training on clinical ability: A systematic review. Arthroscopy 2021;37:1000-7.e1. [Google Scholar] [PubMed]
- 12. Cardoso SA, Suyambu J, Iqbal J, Cortes Jaimes DC, Amin A, Sikto JT, et al. Exploring the role of simulation training in improving surgical skills among residents: A narrative review. Cureus 2023;15:e44654. [Google Scholar] [PubMed]
- 13. Koo A, Almeida BA, Kerluku J, Yang B, Fufa D. Teaching in orthopaedic surgery: Effective strategies for educating the modern learner in a modern surgical practice. JBJS Open Access 2022;7:e22.00005. [Google Scholar] [PubMed]
- 14. Kalun P, Wagner N, Yan J, Nousiainen MT, Sonnadara RR. Surgical simulation training in orthopedics: Current insights. Adv Med Educ Pract 2018;9:125-31. [Google Scholar] [PubMed]
- 15. Naing C, Whittaker MA, Aung HH, Chellappan DK, Riegelman A. The effects of flipped classrooms to improve learning outcomes in undergraduate health professional education: A systematic review. Campbell Syst Rev 2023;19:e1339. [Google Scholar] [PubMed]
- 16. Chick RC, Adams AM, Peace KM, Kemp Bohan PM, Schwantes IR, Clifton GT, et al. Using the flipped classroom model in surgical education: Efficacy and trainee perception. J Surg Educ 2021;78:1803-7. [Google Scholar] [PubMed]
- 17. Wang L, Xia Y, Qiu C, Yuan S, Liu X. Comparative studies of the differences between flipped class and traditional class in orthopedic surgery education. Front Educ 2024;9:1382948. [Google Scholar] [PubMed]
- 18. Mengesha AK, Ayele HS, Misker MF, Beyna AT. Assessing the effectiveness of flipped classroom teaching-learning method among undergraduate medical students at gondar university, college of medicine and health sciences: An interventional study. BMC Med Educ 2024;24:1108. [Google Scholar] [PubMed]
- 19. Ali SS. Problem based learning: A student-centered approach. Engl Lang Teach 2019;12:73. [Google Scholar] [PubMed]
- 20. Falahan SN, Habibi E, Kamyari N, Yousofvand V. Impact of virtual problem-based learning of cardiopulmonary resuscitation on fourth-year nursing students’ satisfaction and performance: A quasi-experimental study. BMC Med Educ 2024;24:425. [Google Scholar] [PubMed]
- 21. Fakoya AO, Ndrio M, McCarthy KJ. Facilitating active collaborative learning in medical education; a literature review of peer instruction method. Adv Med Educ Pract 2023;14:1087-99. [Google Scholar] [PubMed]
- 22. Koenemann N, Lenzer B, Zottmann JM, Fischer MR, Weidenbusch M. Clinical case discussions – a novel, supervised peer-teaching format to promote clinical reasoning in medical students. GMS J Med Educ 2020;37:Doc48. [Google Scholar] [PubMed]