Correctly diagnosing and treating hemangioblastoma originating from spinal nerves are extremely important to avoid bleeding complications and recurrence.
Dr. Søren Peter Eiskjær, Department of Orthopedic Surgery, Aalborg University Hospital, Hobrovej 18-22, 9000 Aalborg C, Denmark. E-mail: spe@rn.dk
Introduction: Previously, only 40 cases with extradural hemangioblastoma at the spinal nerve (none at the T1 nerve root) have been described in the medical literature. In toto, resection of this hypervascular tumor is essential to avoid bleeding complications. Surgery for hemangioblastoma at the cervicothoracic junction is complex and nerve resection of the T1 results in specific neurodeficits of the hand muscles which are not well known.
Case Report: A 34-year-old woman was diagnosed with a slowly growing tumor located at the left foramen T1/T2. Pressure from the tumor resulted in Horner’s syndrome and pain and paresthesia in the upper extremity. The tumor was resected in toto through a posterior midline approach and rib resection and transection of the left T1 and T2 spinal nerves. T2 hemicorporectomy and spinal stabilization were performed to gain access to and mobilize the tumor ventrally. Ptosis decreased after surgery and no neurodeficit was observed except the expected deficit (no deficit was present preoperatively) caused by the T1 resection specifically a small decrease in strength of the abductor and flexor pollicis brevis and opponens pollicis and the lateral two lumbricals. Histological examination of the tumor demonstrated a hemangioblastoma. von Hippel-Lindau disease was ruled out by genetic testing of the patient’s blood. Eight-month postoperatively, all pre-operative symptoms had decreased considerably and the radiographic examination shoved unchanged pedicle screw/rod stabilization of the cervicothoracic junction.
Conclusion: Hemangioblastoma is a rare hypervascular tumor very rarely located at the spinal nerve. The tumor should be resected in toto to avoid recurrence and bleeding. In the current case, the location was at the T1 root necessitating complex surgery with laminectomies and hemicorporectomy of T2 and a posterior rib resection/thoracotomy. Spinal stabilization is mandatory. Preferably embolization should be performed preoperatively. T1 transection results in a specific neurodeficit which should be explained to the patient preoperatively. The patients should undergo genetic testing for Hippel-Lindau disease.
Keywords: Hemangioblastoma, von Hippel-Lindau disease, in toto resection, hemicorporectomy, spinal nerve root T1 nerve lesion.
Hemangioblastoma (HB) is a benign hypervascular neoplasm often associated with von Hippel-Lindau (VHL) disease. The hypervascular tumor is commonly located in the posterior cranial fossa and the spinal cord (¾ intramedullary, ¼ extramedullary) and very rarely extradurally at the spinal nerve root. Only 40 cases with purely extradural spinal nerve root location have been described in the literature [1-4] and none involving the T1 nerve root. In almost 50% of HB with spinal nerve root location, the thoracic nerves are involved. When the HB involves the spinal nerve roots at the cervicothoracic junction a thoracic outlet syndrome (TOS) [5] can occur as well as symptoms from the involved nerve roots. The current case presentation aims to describe a specific case of a large HB with extradural involvement of the T1 root causing TOS symptoms emphasizing the surgical technique used for en bloc resection, diagnostic pitfalls, specific complications, and the association with VHL disease.
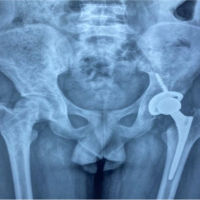
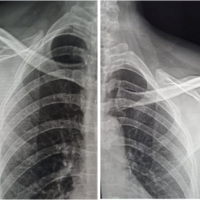
A 34-year-old woman was admitted May 2019 with sudden left shoulder pain, paresthesia’s and subjectively decreased motor function of the left upper extremity. She also suffered from visual disturbances of the left eye. On clinical examination, no objective neurodeficit was demonstrated. Initial total spine magnetic resonance imaging (MRI) showed a tumor extending from the foramen T1/T2 toward T3 and measuring 4.0 × 2.6 × 2.6 cm (Fig. 1 and 2) in a shape resembling a schwannoma. The tumor was located laterally to the foramen and did not compress the spinal cord. The tumor was hypointense to isointense on T1-weighted images, hyperintense on T2-weighted images, demonstrated intense contrast-enhancement, and possible vessel coils (Fig. 1 and 2) corresponding to the usual MRI presentation of a HB [6]. MRI of the cerebrum and computed tomography (CT) scan of the thorax and abdomen were normal. The initial symptoms decreased. The patient was followed with examinations once a year. After 3.5 years, symptoms of pain, weakness, and paresthesia in the left shoulder and upper extremity had increased to an unacceptable extent. Weakness conditional on pain and dysesthesia/paresthesia in the C8/T1 dermatome in the left upper extremity had increased to an unacceptable extent. MRI of the total spine January 2023 showed significant growth of the tumour which had increased in size to 6.4 × 3.4 × 4.2 cm (Fig. 3 and 4). The clinical examination did not demonstrate any objective decrease in muscle strength and the tendon reflexes of the upper extremity were normal. However, a moderate ptosis of the left eyelid was observed. Based on the increasing subjective symptoms, objective signs indicating Horner’s syndrome/TOS and tumor growth were decided to resect the tumor. A posterior approach was chosen. Patient consent was obtained after information about the procedure and common complications as well as specific risks including an increase in the symptoms related to Horner’s Syndrome, paresis/paralysis of the hand muscles (T1 resection) and vocal cord paresis. The surgery was undertaken May 2023 by spine surgeons from both the orthopedic surgery and the neurosurgical department supervised by a thoracic surgeon. Intraoperative monitoring with MEP and SEP was used to monitor the spinal cord function throughout the procedure. Through a posterior midline approach, pedicle screws were placed bilaterally from C7 to T4 except at the T2 level (only right side). The placement of the pedicle screws was guided by cone-beam CT navigation. Laminectomies were performed at the levels T2 and T3 and partially at T1 (left-sided). The T1 and T2 nerve roots on the left-sided were transected and ligated. A partial resection of the second and third rib was undertaken. To get access to the most anteromedial part of the tumor, a left-sided hemicorporectomy of T2 was performed. Before the hemicorporectomy the right rod was fixed in the pedicle screws. Through a retropleural approach, the tumor was resected in toto using stapler ligation of any blood vessels (Fig. 5). Before closure, the second rod was fixed to the pedicle screws and interlaminar bone transplant was applied on the right side (Fig. 6 and 7). Intraoperative blood loss was 950 mL. Postoperatively, ptosis decreased. A slight decrease in strength of the hand muscles innervated by the C8 and T1 nerve roots on the left side was observed. Otherwise, no neurological deterioration was observed postoperatively. The post-operative course was uneventful, and the patient was ready to be discharged after 7 days. Histological examination demonstrated that the tumor was a HB. Two variants of the VHL gene were present in the tumor. However, on genetic testing of the patient’s blood, the VHL gene was not found. Hence, genetic testing of the patient’s family was unnecessary. At the last control January 2024, the radiologic examination demonstrated unchanged placement of the pedicle screw/rod system, healing of the bone transplant and significantly improved subjective symptoms and no change in the findings at the objective clinical examination.





The tentative pre-operative diagnosis in the current case was a schwannoma which is the most common spinal nerve sheath tumor – to differentiate HB from a schwannoma is difficult based on MRI findings [7]. In contrast to schwannoma, an extradurally HB located at the spinal nerve root is extremely rare [1,2]. To avoid bleeding and local recurrence the tumor should be resected en bloc. In this case, a posterior approach was chosen. Posterior thoracotomies are usually preferable to preserve the stability of the thoracic cage. As can be seen on the figure, the tumor extended in front of the T2 vertebral body (Figs. 3 and 4). To be able to mobilize the tumor and visually control the mobilization, a left-sided hemicorporectomy was performed with a chisel and under radiographic control. Before this, the nerve root which adhered to the tumor had been transected and ligated. It is of obvious importance that the spinal cord is protected by applying minimal traction to the nerve root. We consider spinal stabilization with a pedicle screw/rod system, preferably with navigated insertion of the screws, to be mandatory in cases in a transition zone like the current case. HB is a hypervascular tumor and it is extremely important to avoid bleeding from the tumor during the surgical procedure. Bleeding can be profuse and is often associated with severe neurological deficits postoperatively as well as recurrence [8,9]. We were able to mobilize the tumor and resect the tumor en bloc without any bleeding from the tumor (Fig. 5). It has been recommended to do a pre-operative angiography and embolization for vascular tumor’s to guide tumor resection and reduce blood loss [10].

Transection of both the T1 and T2 nerves (as well as the rib resection) was deemed necessary to remove the relatively large tumour in toto. The C8 and T1 combine and are part of the brachial plexus. C8 and T1 supply the ulnar and medial antebrachial cutaneous nerve and send fibers to the median nerve. The abductor and flexor pollicis brevis and opponens pollicis and the lateral two lumbricals are innervated by the C8-T1. Transection of T1 can result in a variable sensory deficit and paresis of the above-mentioned hand muscles. It is imperative that the patient should be informed of the possible deficits preoperatively. Some spine surgeons are not aware of the details concerning the C8-T1 innervations [11]. It is noteworthy that preganglionic T1 sympathetic fibers passing to the sympathetic trunk participate in the sympathetic innervation of the eye and face. Lesion to these fibers may as demonstrated by the current case result in a unilateral Horner’s syndrome. VHL disease a multisystem familial neoplastic syndrome (>25 types reported) is caused by mutations of the VHL tumor suppression gene and is inherited in an autosomal dominant pattern [12]. The incidence is roughly 1/36,000 births with 20% de novo mutations [12]. The VHL tumor syndrome is characterized by central nervous system, retinal HBs, clear cell renal carcinomas, endolymphatic sac tumors, epididymis cystadenomas, pancreatic neuroendocrine tumors, and pheochromocytomas. Thus, it is mandatory that genetic testing for VHL disease should be conducted when a HB is diagnosed. If a diagnosis of VHL disease is confirmed the family should undergo testing. The patient with VHL disease should undergo MRI of the cerebrum and total spine and CT of the thorax and abdomen to rule out HB’s with other locations frequently seen with VHL disease (see above). Using the presented techniques we were able to resect the tumor en bloc with improvement in pre-operative subjective symptoms and without bleeding complications and any neurologic deficits except for an expected small decrease in hand muscle strength.
Hemangioblastoma is a rare hypervascular tumor very rarely located at the spinal nerve. The tumor should be resected en bloc to avoid recurrence and bleeding. In the current case, the location was at the T1 root necessitating complex surgery with laminectomies and hemicorporectomy of T2 and a posterior rib resection/thoracotomy. Spinal stabilization is mandatory. Embolization should preferably be performed preoperatively. T1 transecting results in a specific neurodeficit which should be explained to the patient preoperatively. The patients should undergo genetic testing for VHL disease.
Spinal nerve tumors can be caused by a hypervascular HB and the diagnostic work up especially the imaging part should take this into consideration. Surgery is complex aiming at in toto resection and involves several surgical specialities and preferably pre-operative embolization should be carried out and after histologic verification of HB genetic testing for VHL disease should be undertaken.
References
- 1.Aytar MH, Yener U, Ekşi MŞ, Kaya B, Özgen S, Sav A, et al. Purely extradural spinal nerve root hemangioblastomas. J Craniovertebr Junction Spine 2016;7:197-200. [Google Scholar | PubMed]
- 2.Arumalla K, Deora H, Rao S, Shashidhar A, Rao MB. Spinal extradural hemangioblastoma: A systematic review of characteristics and outcomes. J Craniovertebr Junction Spine 2020;11:254-61. [Google Scholar | PubMed]
- 3.Gläsker S, Klingler JH, Müller K, Würtenberger C, Hader C, Zentner J, et al. Essentials and pitfalls in the treatment of CNS hemangioblastomas and von Hippel-Lindau disease. Cent Eur Neurosurg 2010;71:80-7. [Google Scholar | PubMed]
- 4.Gläsker S, Berlis A, Pagenstecher A, Vougioukas VI, Van Velthoven V. Characterization of hemangioblastomas of spinal nerves. Neurosurgery 2005;56:503-9. [Google Scholar | PubMed]
- 5.Teijink SB, Pesser N, Goeteyn J, Barnhoorn RJ, van Sambeek MR, van Nuenen BF, et al. General overview and diagnostic (imaging) techniques for neurogenic thoracic outlet syndrome. Diagnostics (Basel) 2023;13:1625. [Google Scholar | PubMed]
- 6.Teijink SB, Pesser N, Goeteyn J, Barnhoorn RJ, van Sambeek MR, van Nuenen BF, et al. General overview and diagnostic (imaging) techniques for neurogenic thoracic outlet syndrome. Diagnostics (Basel) 2023;13:1625. [Google Scholar | PubMed]
- 7.Sawyer B, Heng R, Ferris N. Typical magnetic resonance features of a haemangioblastoma, an uncommon nerve root lesion: Case report and literature review. Australas Radiol 2007;51:B28-30. [Google Scholar | PubMed]
- 8.Piquer-Belloch J, Rodriguez-Mena R, Llacer-Ortega JL, Riesgo-Suarez P, Rovira-Lillo V, Gamo AF, et al. A pure extradural hemangioblastoma mimicking a dumbbell nerve sheath tumor in cervical spine: Illustrative case. J Neurosurg Case Lessons 2021;2:CASE2192. [Google Scholar | PubMed]
- 9.Mitchell A, Scheithauer BW, Wharen RE, Franck J, Chan K. Hemangioblastoma of spinal nerve: A report of six cases. Clin Neuropathol 2013;32:91-9. [Google Scholar | PubMed]
- 10.Shin DA, Kim SH, Kim KN, Shin HC, Yoon DH. Surgical management of spinal cord haemangioblastoma. Acta Neurochir (Wien) 2008;150:215-20; discussion 220. [Google Scholar | PubMed]
- 11.Kim JH, Joo SM, Cho YE, Ha SW, Suh SH. Percutaneous onyx embolization of recurrent cervical nerve root hemangioblastoma: A case report and review of the literature. Clin Neuroradiol 2021;31:1209-13. [Google Scholar | PubMed]
- 12.Stoker GE, Kim HJ, Riew KD. Differentiating C8-T1 radiculopathy from ulnar neuropathy: A survey of 24 spine surgeons. Global Spine J 2014;4:1-6. [Google Scholar | PubMed]
- 13.Bisceglia M, Muscarella LA, Galliani CA, Zidar N, Ben-Dor D, Pasquinelli G, et al. Extraneuraxial hemangioblastoma: Clinicopathologic features and review of the literature. Adv Anat Pathol 2018;25:197-215. [Google Scholar | PubMed]