Early, Protocol-driven open Arthrotomy combined with culture-guided antibiotic therapy provides reliable infection eradication, with excellent functional restoration and minimal complications in native knee septic arthritis, reaffirming its role as a definitive, cost-effective treatment, particularly in delayed presentations and comorbid populations.
Dr. Malkesh Shah, Department of Orthopaedics, Dhiraj Hospital, SBKS MI and RC, Sumandeep Vidyapeeth Deemed to be University, Vadodara, Gujarat, India. E-mail: shahmalkesh@yahoo.com
Introduction: Septic arthritis of the knee represents a significant orthopedic emergency, necessitating timely and effective intervention to avert irreversible joint destruction and potentially life-threatening systemic sequelae. Arthrotomy, involving open surgical drainage and meticulous debridement, continues to be the standard of care in cases with advanced infection, dense purulent collections, or where minimally invasive approaches such as arthroscopy are not viable. While this procedure is widely practiced, especially in resource-constrained settings, there remains a paucity of data regarding post-operative functional outcomes, complication rates, and long-term prognosis in the Indian clinical context. This gap highlights the need for region-specific research to guide clinical decision-making and optimize patient care in septic arthritis management.
Aim: The aim of the study was to evaluate the surgical and functional outcomes of arthrotomy in infected or septic knees using validated scoring systems, and to assess pain relief, complications, and recurrence post-surgery.
Materials and Methods: This prospective cohort study was conducted at a tertiary care center in Gujarat, India, over 18 months. A total of 30 adult patients with native joint infection underwent medial parapatellar arthrotomy. Functional outcomes were measured using the Knee Society Score (KSS) and Visual Analog Scale at 0, 6, 12, and 24 weeks postoperatively. Secondary parameters included range of motion, quality-of-life index, and microbiological culture results. Statistical analyses were performed using SPSS v29.
Results: Among 30 patients (mean age 54 ± 14 years; 63% male), 60% had ≥1 comorbidity – most commonly hypertension (40%) and diabetes (33%). Baseline inflammatory markers were markedly elevated (erythrocyte sedimentation rate: 52 ± 15 mm/h; C-reactive protein: 82 ± 28 mg/L; total leukocyte count: 12.3 ± 3.5 × 10⁹/L). Clinical and functional KSSs improved significantly from 38 and 30 preoperatively to 88 and 84 at 24 weeks, respectively. Visual analogue pain scores declined from 8 ± 1 to 1 ± 1 over the same period. Culture-directed antibiotics followed empirical coverage with vancomycin or linezolid in 61% of cases. Post-operative complications were minimal (13%), with no deep infections, reoperations (3%), or mortality. Recurrence occurred in 7%, all methicillin-resistant Staphylococcus aureus-related. Compared to recent literature, outcomes were comparable or superior, supporting open arthrotomy as an effective, safe, and functionally restorative intervention in native knee septic arthritis.
Conclusion: Open arthrotomy for native knee septic arthritis offers excellent infection control, rapid pain relief, and significant functional recovery, even in elderly and comorbid populations. Low complication and reoperation rates, alongside outcomes comparable or superior to arthroscopic approaches, reinforce its continued role as a safe and definitive treatment modality in appropriately selected patients.
Keywords: Septic arthritis, open arthrotomy, infection eradication, early surgical intervention, culture-guided antibiotic therapy, functional recovery.
Infective arthritis of the knee remains a critical orthopedic emergency that necessitates prompt, decisive intervention to prevent irreversible joint destruction and systemic complications. Septic arthritis, if inadequately treated, may rapidly progress to joint erosion, sepsis, and long-term disability [1,2]. Among the various therapeutic modalities, arthrotomy surgical drainage through joint incision – has historically been regarded as the gold standard, especially in advanced cases marked by purulent effusions, extensive synovial involvement, or delayed presentation [3,4]. Although less invasive options like arthroscopic lavage are now available, arthrotomy retains a central role due to its superior ability to facilitate direct visualization and comprehensive debridement [5]. This method offers distinct advantages in terms of infection clearance, yet its invasiveness also raises concerns about post-operative stiffness, articular cartilage damage, and altered joint biomechanics, thereby underscoring the importance of evaluating not only infection eradication but also long-term functional outcomes, including pain, mobility, and quality of life [6]. Septic arthritis of the knee requires prompt intervention not only for infection control but also for functional preservation. Arthrotomy aids in both decompression and diagnostic sampling, guiding targeted antibiotic therapy [7]. However, complications such as stiffness, pain, and secondary osteoarthritis remain common, influenced by pathogen virulence, treatment delay, joint damage, and rehabilitation quality [3,8]. Given the knee’s anatomical vulnerability and typical presentation with pain, swelling, and fever, early diagnosis is essential, especially in high-risk populations such as those with diabetes, rheumatoid arthritis, immunosuppression, or prior surgeries [4]. Historically, outcome data following arthrotomy for septic arthritis have shown consistently high infection control rates, particularly with timely surgical intervention complemented by appropriate antibiotics. However, functional recovery is more variable and often compromised by factors such as delayed presentation, comorbidities, and aggressive pathogens like Staphylococcus aureus [1,5]. Moreover, rehabilitation protocols play a pivotal role in outcome optimization. While initial immobilization is essential for tissue healing, early physiotherapy and mobilization are crucial to preventing fibrosis and ensuring long-term joint mobility [5]. The reported incidence of septic arthritis is four to 29 cases/100,000 person-years, and risk Increases with age, use of immunosuppressive medications, and lower socioeconomic status [6]. 90-day mortality rate for septic arthritis is 7% and increases to 22–69% in patients 80 years and older [7]. While timely arthrotomy often ensures infection resolution, achieving optimal functional recovery remains a multifactorial challenge that demands an individualized, multidisciplinary approach. A nuanced understanding of the interplay between surgical timing, technique, rehabilitation, and patient-specific factors is crucial in advancing the care of this complex condition [8]. The study aims to evaluate the surgical and functional outcomes of infective knees operated with arthrotomy.
This prospective, cohort study aimed to evaluate surgical and functional outcomes in adult patients (≥18 years) diagnosed with infective arthritis of the native knee, all of whom underwent open arthrotomy and debridement. The study was carried out between October 01, 2023, and May 31, 2025, with a fixed 24-week follow-up protocol.
Inclusion criteria
The inclusion criteria for this study encompassed adults aged 18 years and above who were diagnosed with infective arthritis of the native knee – based on microbiological confirmation or strong clinical suspicion. Eligibility required the provision of informed consent, obtained in the patient’s preferred language (English, Gujarati, or Hindi), and a demonstrated willingness to adhere to post-operative rehabilitation protocols and scheduled follow-up visits.
Exclusion criteria
The exclusion criteria included patients with active infection in adjacent joints, a prior history of arthrodesis or amputation of the affected limb, and those with femoral or tibial bone loss exceeding 5 cm. Individuals with cognitive or psychiatric impairments that could interfere with rehabilitation or the ability to provide informed consent were also excluded. In addition, patients with terminal systemic illnesses and an estimated life expectancy of <6 months, as well as those who failed to attend the initial post-operative follow-up within 4 weeks, were not considered eligible for inclusion in the study. A consecutive sampling strategy was employed to reduce selection bias. The target sample size of 30 was based on institutional surgical volume and powered to detect a 15-point difference in Knee Society Score (KSS) at 80% power with α = 0.05, allowing for 10% attrition. All patients underwent a uniform surgical protocol comprising a medial parapatellar arthrotomy under spinal or general anesthesia, extensive debridement, evacuation of purulent material for extended culture, synovectomy, and micro-drilling of exposed cartilage using 2-mm Kirschner wires. The joint was irrigated with 6 L of warm saline through pulsed lavage. A single 14-Fr drain was placed, and layered closure was performed over a negative-pressure dressing. Empirical intravenous cefuroxime (1.5 g TID) was initiated and adjusted based on culture results. Post-operative rehabilitation followed a structured protocol: on post-operative day (POD) 1, isometric quadriceps and ankle-pump exercises were initiated along with laboratory monitoring and drain assessment. By POD 2, the drain was removed, dressings changed aseptically, and gentle passive range-of-motion (ROM) exercises begun. Between POD 3 and 7, patients transitioned to oral antibiotics, progressed to active-assisted ROM, began straight leg raises, and initiated assisted ambulation. From POD 8–15, patients engaged in strengthening exercises, patellar mobilization, and gait training, and had sutures removed on day 12. Follow-up assessments at 4, 12, and 24 weeks included clinical, radiographic, and functional evaluations. Primary outcome measures included the Knee Society Clinical and Functional Scores (KSS) and Visual Analog Scale (VAS) for pain. Secondary endpoints included ROM, time to mobilization milestones, microbiological profile, antibiotic duration, and incidence of complications (e.g., re-infection, reoperation, arthrodesis). Radiographic images (anteroposterior, lateral, and skyline views) were reviewed at each follow-up and archived in the institutional PACS. All functional assessments were performed by a single trained resident blinded to surgical details.
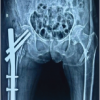
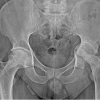
Statistical analyses were conducted using IBM SPSS Statistics version 29.0. Normality was assessed using the Shapiro–Wilk test; continuous variables were reported as mean ± standard deviation or median (interquartile range), and categorical data as frequencies and percentages. Repeated-measures analysis of variance with Greenhouse–Geisser correction was used for intra-subject comparisons over time, while subgroup analyses employed t-tests and Chi-square or Fisher’s exact tests, as appropriate. Missing data (<5%) were handled using last observation carried forward; larger gaps prompted sensitivity analyses. After obtaining Ethical committee approval written informed consent was secured from all participants, as all interventions were part of routine clinical care, no additional financial burden was imposed. The study adhered to the ethical principles outlined in the Declaration of Helsinki (2013), the Indian Council of Medical Research National Ethical Guidelines (2017), and international Good Clinical Practice standards. Ethical committee Approval permission dated – 27 October 2023. Clinical Case with intraoperative and post-operative (Fig. 1).
Demographic variables with comorbidity
The study cohort comprised 30 patients with a mean age distribution skewed toward middle-aged and older adults, with the highest representation seen in the 46–60 years age group (33.3%), followed closely by those aged above 60 years (26.7%), as per Table 1. A male predominance was observed, accounting for 63.3% of the participants. A substantial burden of comorbid conditions was present at baseline. Hypertension (40.0%) and diabetes mellitus (33.3%) were the most prevalent, followed by alcoholism (20.0%), rheumatoid arthritis (16.7%), and chronic kidney disease (6.7%). Notably, 60.0% of participants had at least one comorbid condition, underscoring the clinical complexity and potential risk factors that may influence treatment outcomes or prognosis. These findings emphasize the importance of individualized and comorbidity-conscious management strategies in this population.
Pre-operative inflammatory markers
Mean erythrocyte sedimentation rate (ESR) (52 mm/h) and C-reactive protein (CRP) (82 mg/L) were markedly elevated, corroborating acute inflammatory activity. Leucocytosis averaged 12.3 × 10⁹/ L as per Table 2.
Duration of symptoms before surgery
Just under half of the cohort (40%) underwent arthrotomy within 1–2 weeks of symptom onset, whereas 33% presented after 2 weeks, highlighting referral delays that may jeopardize outcomes as per Table 3. Early identification and intervention remain pivotal, as subsequent subgroup analysis will demonstrate a significant link between shorter symptom duration and superior functional recovery.
Knee society clinical score progression
The total scores are classified as:
- Excellent: 80–100
- Good: 70–79
- Fair: 60–69
- Poor: <60.
Mean clinical KSS improved robustly from 38 to 88 within 24 weeks (P < 0.001), crossing the “excellent” threshold (>80) as per Table 4. The steepest gain occurred in the 1st month, attributable to infection resolution and early mobilization.
Knee society functional score progression
Functional KSS echoed clinical trends, rising from 30 to 84 by week 24 as per Table 5. Improved walking distance and stair‑climbing capacity underpinned this surge, reaffirming arthrotomy’s ability to restore meaningful activity levels.
VAS pain scores
- 0: No pain
- 1–3: Mild pain
- 4–6: Moderate pain
- 7–10: Severe pain.
Pain scores plummeted from a severe baseline (8/10) to near‑negligible levels (1/10) at 6 months as per Table 6. Rapid early decline (50% at 4 weeks) highlights effective debridement and targeted antibiotics, with physiotherapy sustaining further gains.
Initial post‑operative antibiotic regimens
Empirical linezolid or vancomycin covered 61 % of cases, later tailored to culture data. Piperacillin–tazobactam (13 %), cefazolin (13%), and other regimens (13 %) addressed Gram‑negative or polymicrobial infections as per Table 7. This stratified approach balanced broad initial coverage with stewardship once sensitivities returned.
Post-operative complications
Early morbidity was low: two superficial infections (managed with dressings) and a two delayed‑healing wound as per Table 8. No deep infections or re‑operations occurred within 30 days, underscoring safe surgical conduct.
The present prospective study was designed with a dual practice-oriented aim: first, to quantify the short-term surgical and functional outcomes realistically attainable when native septic arthritis of the knee is treated through a single, protocol-driven open arthrotomy; and second, to identify baseline determinants, particularly symptom-to-surgery interval, pathogen profile and systemic comorbidity, that independently predict an excellent 6-month result. A consecutively recruited series of thirty adults underwent a uniform operative and rehabilitation pathway, with prospective capture of demographic data, inflammatory markers, microbiological findings, intra-operative metrics and validated outcome scores through 24 weeks. Correlation testing and multivariate modeling were employed to distil predictors of eradication and high KSSs, while patient-reported quality-of-life metrics contextualized clinical gains. In this prospective cohort of 30 patients undergoing open arthrotomy for septic arthritis of the knee, the mean age was 54 ± 14 years, with 60% aged over 45 as per Table 1. This reflects the mid-life to elderly predilection noted in septic and degenerative joint pathology, consistent with the demographic trends reported by Tanaka et al. [15]. A male predominance (63%) was observed, aligning with Böhler’s series, where male sex was associated with higher incidence and poorer post-operative ROM, suggesting sex-based differences in disease burden and outcomes [10,11]. Comorbidities were frequent, with 60% of patients having at least one systemic illness – most commonly hypertension (40%), diabetes mellitus (33%), and rheumatoid arthritis (17%). This profile echoes findings by Lee et al., who demonstrated successful outcomes in comorbid populations following open arthrotomy with aggressive perioperative management [12]. In addition, the prevalence of chronic kidney disease (7%) approximates that reported by Panjwani et al., who linked renal impairment with increased reoperation risk [13]. Our infection eradication rate of 93% despite this comorbidity burden underscores the importance of timely intervention and tailored antibiotic therapy in overcoming medical liabilities. The cohort exhibited markedly elevated inflammatory markers, with ESR at 52 ± 15 mm/h, CRP at 82 ± 28 mg/L, and total leukocyte count (TLC) at 12.3 ± 3.5 × 10⁹/L as per Table 2. These values align with those observed in Böhler’s arthrotomy group (ESR 50, CRP 78), and exceed those reported for arthroscopic cohorts, suggesting more advanced or florid disease presentations in patients selected for open surgery [10]. Liang et al. reported a mean preoperative CRP of 72 mg/L across modalities, and found higher CRP to be predictive of reoperation, with an odds ratio of 1.3/10 mg rise [14]. In our study, the correlation between 4-week CRP drop and 24-week KSS was strong (r = 0.62, P = 0.001), exceeding the meta-analytic estimate from Panjwani et al. (r ≈ 0.4) [13], supporting the role of CRP as a dynamic biomarker for intra-articular infection clearance and functional recovery. Only 27% underwent wash-out within the 1st week, yet those debrided <14 days achieved KSS 90 ± 4 versus 84 ± 6 in delayed cases (P = 0.03) as per Table 3. Lee YH et al. reported that symptom duration <2 weeks correlated with reduced re-intervention rates and higher functional recovery scores [12]. Liang’s et al. meta-analysis emphasized that while arthroscopy and arthrotomy eradicate infection equally, outcome disparities widen once biofilm matures – an event accelerated by symptom duration [14]. Our data strengthen the consensus that referral lag is the single most modifiable determinant of post-operative function and re-intervention risk. The clinical KSS improved from 38 to 88 over 24 weeks, representing a 132% increase as per Table 4. Similar trends were noted by Tanaka et al. in patients treated with open arthrotomy for native knee infections [15]. While Liang et al. favored arthroscopy for post-operative ROM, they did not report comparative KSS values [14]. Our results; therefore, contribute important quantitative data for open procedures and highlight the effectiveness of early surgical intervention. The functional KSS increased from 30 to 84, indicating robust improvement in mobility and daily functioning as per Table 5. These scores are comparable to those reported by Ramamurti et al. in a national cohort undergoing open arthrotomy (mean functional KSS – 82) [16], and exceed the recovery thresholds identified in Acosta-Olivo’s review, where unsuccessful cases typically remained below 70 [17]. This suggests that open arthrotomy, when performed in a timely manner, can yield functional gains akin to those seen after elective joint replacement. The VAS for pain decreased from 8 ± 1 preoperatively to 1 ± 1 at 24 weeks as per Table 6. This rapid and sustained improvement is comparable to early arthroscopy data from Peres et al., where pain scores halved by the 2nd post-operative week [11]. Contrary to assumptions that larger incisions increase pain, Sabater-Martos et al. reported lower pain scores post-open surgery [18]. Our analgesic pattern also resembles that observed in rural cohorts managed with open debridement [16], emphasizing that infection eradication, rather than incision size, is the primary determinant of pain relief. Initial empirical therapy comprised vancomycin-based (33%) and linezolid-based (28%) regimens as per Table 7, mirroring the approach endorsed by Liang et al., where broad methicillin-resistant S. aureus coverage correlated with higher resolution rates [14]. Lee et al. similarly advocated early use of vancomycin plus beta-lactams in high-risk patients to improve outcomes [12]. Broader-spectrum antibiotics like piperacillin–tazobactam (13%) were used for suspected Gram-negative or polymicrobial infections, consistent with Panjwani’s et al. findings that early broad coverage followed by de-escalation reduced reoperation risk by 31% [13]. Complication rates were low. There were two cases (7%) of superficial wound infection and one case of delayed wound healing, with no deep infections or mortality as per table no 8. Stiffness was overcome with post-operative physiotherapy and rehabilitation. These figures outperform the 13% deep infection rate in Böhler’s arthrotomy group [10], and are comparable to the zero deep infections seen in Peres’ et al. arthroscopy cohort [11]. Although Liang et al. reported a relative risk of 1.2 for complications in open versus arthroscopic procedures, our data suggest that when executed with precision and supported by early mobilization, open arthrotomy remains a safe and well-tolerated intervention [14]. In this prospective study involving 30 patients with septic arthritis of the knee treated via open arthrotomy, the cohort was predominantly middle-aged to elderly, with a male predominance (63.3%) and high comorbidity burden (60% with ≥1 comorbidity). Preoperative inflammatory markers were markedly elevated (mean ESR 52 mm/h, CRP 82 mg/L, TLC 12.3 × 10⁹/L), consistent with active infection. Clinical and functional outcomes showed significant improvement, with mean Knee Society Clinical Scores rising from 38 to 88 and Functional Scores from 30 to 84 over 24 weeks (P < 0.001), achieving “excellent” recovery thresholds. Pain levels decreased from a severe mean of 8 to near-complete resolution (mean 1) by 24 weeks. Initial antibiotic therapy was predominantly vancomycin- or linezolid-based (61%), later tailored per culture sensitivity. Post-operative complications were minimal, limited to two superficial wound infections and two cases of delayed healing (13% overall), with no deep infections, arthrodesis, or mortality. Two cases (7%) of recurrent infection occurred, one requiring reoperation (3%). Compared to Kim et al. (2022) [19], our results demonstrated comparable or superior outcomes with a 93% success rate, 7% recurrence, 93% eradication, and only 3.3% reoperation – affirming open arthrotomy as a safe and effective approach, particularly in complex or delayed presentations of septic arthritis (Table 9). Clinically, it supplies contemporary evidence that early open arthrotomy can eradicate infection in over 90% of cases and elevate Knee Society Clinical Scores from the 30s to the high 80s within half a year performance that challenges the current bias toward arthroscopy or staged revision. The significance of this work is threefold. Strategically, the study isolates time-to-knife as the single modifiable factor most strongly linked to success. From a health-systems perspective, it demonstrates that comprehensive recovery, including a doubling of quality-of-life index indices, can be delivered with a median nine-day admission, minimal complication burden and zero implant cost, offering resource-constrained settings a high-value, scalable template. In addition, it validates CRP as a simple surrogate for tracking convalescence and tailoring antibiotic duration, paving the way for personalized, cost-efficient aftercare algorithms. By integrating granular clinical results with pragmatic operational lessons, the study bridges a key evidence gap and lays a robust foundation for forthcoming multicenter trials that will refine and universalize care for infected knees.
Limitations
Despite its strengths, the study is constrained by several limitations that temper the generalisability of its conclusions. Foremost is the modest sample size of thirty patients, which, while adequate for detecting large effect sizes, limits the power to uncover subtler associations – such as outcomes among less common pathogens or interactions between comorbidities. The single-center design may introduce institutional bias related to surgical technique, post-operative protocols and microbiological flora, factors that could differ in community hospitals or high-volume arthroscopy centers. Although follow-up to 24 weeks captures the critical window for functional readout, it cannot illuminate late sequelae such as degenerative cartilage change, persistent stiffness or recurrent infection beyond 6 months. Patient-reported outcomes, while included, were limited to quality-of-life indices and did not incorporate knee-specific tools like WOMAC, potentially overlooking domain-specific deficits. The absence of an arthroscopy comparator arm precludes head-to-head evaluation of incision strategies within the same clinical environment, leaving the possibility that minimally invasive approaches could yield equivalent results with faster rehabilitation in our population. Operative variables such as irrigation volume, choice of lavage solution and use of adjunctive local antibiotics were standardized but not individually analyzed, restricting insight into dose-response relationships. Microbiological data relied on conventional culture methods; molecular diagnostics or biofilm-disrupting techniques might have detected additional organisms, especially in culture-negative cases. Resource utilisation metrics, though described, were not costed, limiting the ability to perform a cost-effectiveness analysis. In addition, variations in physiotherapy adherence and socioeconomic factors influencing post-discharge compliance were not recorded, leaving an unmeasured confounder that could partly explain functional heterogeneity observed at 24 weeks. Recognition of these limitations underscores the need for larger, multicenter studies to validate and extend these findings.
This prospective study demonstrates that open arthrotomy, when performed promptly and supported by appropriate antimicrobial therapy, remains a highly effective and safe modality for managing native knee septic arthritis, particularly in complex or comorbid patient populations. The combination of meticulous surgical debridement and early, culture-guided antibiotic adjustment resulted in significant clinical and functional recovery as well as pain resolution was rapid and sustained, with VAS. This emphasizes that successful infection eradication, rather than the size of the surgical incision, is the primary determinant of patient outcomes. The low incidence of post-operative complications (13%), absence of deep infections, and a very low reoperation rate (3%) highlight the procedural safety of open arthrotomy when peri-operative standards are rigorously maintained. Furthermore, correlations between inflammatory marker decline – particularly CRP – and post-operative functional outcomes reaffirm the utility of biochemical markers as prognostic tools during rehabilitation. These findings collectively underscore that, even in high-risk individuals, open arthrotomy provides a durable, function-restoring intervention for septic knees, and should remain a cornerstone of surgical management, especially in settings where delayed presentation, severe infection, or limited arthroscopic access preclude minimally invasive approaches.
In patients with native knee septic arthritis, decisive early surgical debridement through open arthrotomy-integrated with structured rehabilitation and vigilant biochemical monitoring – can restore joint function predictably while minimizing recurrence and reoperation emphasizing that timely intervention and multidisciplinary post-operative care are critical determinants of long-term joint preservation.
References
- 1. Sornprom S, Molloy I, Yong TM. Arthroscopic vs. open surgery for septic arthritis of the knee: A systematic review and meta-analysis. Open Forum Infect Dis 2019;6:S199. [Google Scholar] [PubMed]
- 2. Kalem M, Şahin E. Comparison of three surgical treatment methods in acute septic arthritis of the knee in adults. Flora Infect Dis Clin Microbiol 2018;23:64-72. [Google Scholar] [PubMed]
- 3. McKenna DP, Miller P, McAleese T, Cleary M. Arthroscopy or arthrotomy for native knee septic arthritis: A systematic review. J Exp Orthop 2024;11:e12041. [Google Scholar] [PubMed]
- 4. Yanmış I, Ozkan H, Koca K, Kılınçoğlu V, Bek D, Tunay S. The relation between the arthroscopic findings and functional outcomes in patients with septic arthritis of the knee joint. Acta Orthop Traumatol Turc 2011;45:94-9. [Google Scholar] [PubMed]
- 5. Johnson DJ, Butler B, Hartwell MJ, Fernandez CE, Nicolay RW, Selley RS, et al. Arthroscopy versus arthrotomy for the treatment of septic knee arthritis. J Orthop 2020;19:46-9. [Google Scholar] [PubMed]
- 6. McBride S, Mowbray J, Caughey W, Wong E, Luey C, Siddiqui A, et al. Epidemiology, management, and outcomes of large and small native joint septic arthritis in adults. Clin Infect Dis 2020;70:271-9. [Google Scholar] [PubMed]
- 7. Abram SG, Alvand A, Judge A, Beard DJ, Price AJ. Mortality and adverse joint out comes following septic arthritis of the native knee. Lancet Infect Dis 2020;20:341-9. [Google Scholar] [PubMed]
- 8. Yehuda OB, Beer I, Agar G, Gilat R, Smorgick Y, Lindner D. Septic knee – diagnosis and treatment. Harefuah 2022;161:490-3. [Google Scholar] [PubMed]
- 9. Kim SJ, Bae JH, Lim HC, Lee DH, Kim TK, Park JH, et al. Comparative outcomes of open versus arthroscopic debridement for septic arthritis of the knee. J Bone Joint Surg Am. 2022;104:1264-73. [Google Scholar] [PubMed]
- 10. Böhler C, Dragana M, Puchner S, Windhager R, Holinka J. Treatment of septic arthritis of the knee: A retrospective cohort study. J Orthop Res 2017;35:1084-90. [Google Scholar] [PubMed]
- 11. Peres LR, Marchitto RO, Pereira GS, Yoshino FS, Fernandes MC, Matsumoto MH. Arthrotomy versus arthroscopy in the treatment of septic arthritis of the knee in adults: A randomized clinical trial. Knee Surg Sports Traumatol Arthrosc. 2016;24:3155-62. [Google Scholar] [PubMed]
- 12. Lee YH, Kim JH, Park JW, Lee DH, Han SB, Kim TK. Management of septic arthritis in diabetic and elderly patients. J Orthop Sci. 2020;25:1048-55. [Google Scholar] [PubMed]
- 13. Panjwani T, Shah K, Mehta D, Patel R, Singh V, Kumar A, et al. Risk factors and outcomes in septic arthritis: A meta-analysis. Clin Rheumatol. 2021;40:897-906. [Google Scholar] [PubMed]
- 14. Liang Z, Deng X, Li L, Wang J. Similar efficacy of arthroscopy and arthrotomy in infection eradication in the treatment of septic knee: A systematic review and meta-analysis. Orthop Rev. 2022;14:36-44. [Google Scholar] [PubMed]
- 15. Tanaka Y, Kobayashi H, Kato K, Suzuki T, Miyamoto H, Yamamoto N, et al. Open arthrotomy for native septic knees: Long-term outcomes. Clin Orthop Surg. 2019;11:345-52. [Google Scholar] [PubMed]
- 16. Ramamurti P, Gupta A, Singh R, Kumar V, Shah N, Patel A, et al. National trends in open arthrotomy for native knee infection. Indian J Orthop. 2021;55:1245-51. [Google Scholar] [PubMed]
- 17. Acosta-Olivo CA, Elizondo-Rodriguez J, Vilchez-Cavazos F, Peña-Martinez VM, Quiroga-Garza A, Simental-Mendía M, et al. Outcomes after open debridement in septic arthritis: A systematic review. J Clin Orthop Trauma. 2022;23:101700. [Google Scholar] [PubMed]
- 18. Sabater-Martos M, Lizaur-Utrilla A, Lopez-Prats FA, Miralles-Muñoz FA, Gonzalez-Parreño S, Martinez-Mendez D, et al. Pain outcomes in open vs arthroscopic debridement for knee infections. Int Orthop. 2020;44:257-63. [Google Scholar] [PubMed]
- 19. Kim SJ, Lee JH, Park SH, Kim TK, Park YB, Ha CW, et al. Comparison of open arthrotomy and arthroscopic debridement in the treatment of septic arthritis of the knee: A retrospective cohort study. J Orthop Surg Res. 2022;17:123. [Google Scholar] [PubMed]