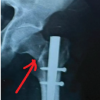
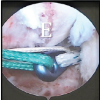
There is ease of maintaining reduction and positioning of the patient intraoperatively while doing the tibial nailing through the suprapatellar approach.
Dr. Shubham Sakarkar, Department of Orthopaedics, All India Institute of Medical Sciences, Raipur, Chhattisgarh, India. E-mail: shubham24apr96@gmail.com
Introduction: Tibial fractures are among the most frequently encountered long-bone injuries requiring surgical management. The conventional infrapatellar (IP) approach for intramedullary nailing (IMN) is associated with challenges, such as difficulty in position holding the reduction and post-operative knee pain. The suprapatellar (SP) approach has emerged as an alternative, potentially offering ease in the intraoperative position of the limb, holding the reduction and better functional outcomes with less knee pain. This study aims to compare the functional and radiological outcomes, as well as complication rates, between SP and IP approaches for tibial shaft IMN.
Materials and Methods: This randomized controlled trial included 85 patients with tibial shaft fractures, allocated to either SP (n = 40) or IP (n = 45) groups. All underwent closed reduction and internal fixation using IMN. Functional outcomes were assessed using the Visual Analog Scale (VAS) and Lysholm scores, while radiological outcomes were measured using the Radiographic Union Scale for Tibia (RUST) and alignment parameters. Evaluations were performed at post-operative day 2, 2 weeks, 6 weeks, 12 weeks, and 6 months.
Results: There was no statistically significant difference in age, gender, fracture type, or AO classification between the groups. RUST scores and fracture alignment were comparable across all time points. The SP group demonstrated significantly lower VAS scores at 6 weeks, 12 weeks, and 6 months (P < 0.001) and higher Lysholm scores at corresponding intervals (P < 0.001). The mean time to union was marginally shorter in the SP group (19.27 weeks) than the IP group (20.13 weeks), though not statistically significant (P = 0.342). Post-operative complications, including anterior knee pain, were lower in the SP group (5%) compared to the IP group (26.7%).
Conclusion: The SP approach for tibial IMN yields superior early functional outcomes and reduced anterior knee pain without compromising radiological healing or alignment. These findings support its broader use, especially where early mobilization and patient comfort are priorities. Long-term studies are warranted for further validation.
Keywords: Tibial shaft fracture, suprapatellar approach, infrapatellar approach, intramedullary nailing, Visual Analog Scale score, Lysholm score, radiographic union scale for tibia score, knee pain, fracture alignment.
Tibia fracture is the most common type of long bone fracture and the most common cause is high-energy trauma [1]. Tibial fractures occur 16.9 times for every 100,000 individuals in the global population each year [2]. There is a significantly higher incidence of the injury in men (21.5/100,000 people/year) compared to females (12.3/100,000) [3]. Between the ages of 10 and 20, the incidence rate of tibial fractures is 43.5/100,000/year, which is higher among males [4]. This triangular bone is responsible for supporting over 80% of the body weight in the lower limb. Deforming stresses contribute to malalignment in cases with proximal tibial shaft fractures. The patellar tendon or extensor retinaculum causes deformation of the proximal tibia fragment into extension. The gastrocnemius muscle and hamstrings pull the lower part of the tibia towards flexion. The pes anserinus pulls the upper part of the tibia toward the varus [5]. A thorough history is required to determine the cause of the injury at the time of presentation. Both low and high-impact injuries may cause fractures in the tibia. AP and lateral radiographs of the tibia, as well as the joints above and below, that is, knee and ankle, are recommended for imaging. Computed tomography imaging is needed whenever fractures extend within the joint, either tibial plateau or plafond. As per the AO/OTA (Arbeitsgemeinschaft für Osteosynthesefragen/Orthopaedic Trauma Association) classification, bone segment 42 is represented by the tibial shaft, and its fracture is classified as (A) simple, (B) wedge, and (C) complex. The AO/OTA classification system includes additional subclassifications that are determined by the presence and location of a concomitant fibula fracture [6]. Intramedullary interlock nailing for tibial fractures had given a promising result in terms of functional and radiological outcomes [7,8]. After intramedullary nailing (IMN), functional scores had shown that 73% of patients experience knee discomfort, and 33% report subjective leg swelling [9]. The traditional infrapatellar (IP) approach for tibia IMN is a commonly used surgical technique for treating tibial fractures. Nevertheless, the insertion of an IMN via the IP method continues to be difficult due to the stress exerted by the quadriceps muscle, which may cause displacement of the fracture fragments towards the proximal end when the knee is flexed. There is also a higher risk of getting valgus and procurvatum defects post-nail insertion [10]. To overcome these challenges, Tornetta et al initially proposed a semi-extended technique for tibial IMN insertion [11]. A suprapatellar (SP) method using an insertion site through the quadriceps tendon was later developed by Cole et al. [12]. According to this novel method, lateral and anteroposterior imaging of the tibia can be more easily achieved if the patient maintains a fully or near fully extended knee position, thus avoiding valgus and procurvatum malalignment [13]. However, the main issue with this approach is the risk of patellofemoral articulation damage, which may worsen both anterior knee pain after IMN fixation and patellofemoral arthritis [14]. A recent RCT study demonstrated that the SP approach was more effective than the IP approach in treating tibial shaft fractures in terms of functional knee outcomes [15]. Nevertheless, multiple studies reported no statistically significant difference between the SP and IP methods in terms of pain, range of motion, knee functional score, or time to union [16]. There has been no clear verdict on whether the SP or IP method is better so far. This study will compare the functional and radiological outcomes of the SP and IP approaches for intramedullary interlock nailing for tibial fractures in this specific geographic region of Chhattisgarh, India, due to the scarcity of studies done here. This study will help us find whether the SP approach is better, worse, or the same as the IP approach in terms of functional and radiological outcomes.
This randomized controlled trial, single blind study was conducted in the Department of Orthopaedics at a tertiary care hospital and involved patients presenting with tibial fractures. The study was approved by the Institutional Ethics Committee and was carried out over a period of 18 months, which included 12 months for patient enrolment and surgical intervention, followed by a 6-month post-operative follow-up. Patients were recruited from both the emergency department and the orthopedic outpatient clinic. All participants were evaluated against pre-defined inclusion and exclusion criteria to determine eligibility. Sample size estimation was based on a prior study by Dic et al., which reported a mean Lysholm score of 90 in patients treated with SP nailing and 75 in those treated with IP nailing. Using this difference as a reference, the minimum required sample size was calculated to be 78. To compensate for potential dropouts and ensure adequate statistical power, a total of 85 patients were ultimately enrolled. Randomization was performed using the Sequentially Numbered Opaque Sealed Envelope (SNOSE) technique to maintain allocation concealment. The patients were divided into two groups. Group 1 included 40 patients who underwent closed reduction and internal fixation (CRIF) with intramedullary interlock nailing via the SP approach. Group 2 included 45 patients who underwent CRIF using the IP approach. Fractures were classified according to the AO classification system to ensure uniformity across both groups.
Flow Diagram Showing the Methodology
Patient selection criteria
Inclusion criteria
- Radiological findings confirming the shaft of tibia fracture according to AO classification (Type 42A, B, C, and 43A)
- The patient was willing to have surgery
- Patients more than 18 years of age
- Patients with compound fracture, including Gustilo Anderson type I and
Exclusion criteria
- Patients with compound fractures, excluding Gustilo Anderson type I and II, and including severe soft tissue injury
- Patients with polytrauma
- History of old surgery in the same limb
- History of fracture in other than the tibia or fibula in the ipsilateral or contralateral limb at the same time
- Patients who are medically unfit for
Statistical analysis
- Statistical analysis was carried out using statistical packages for the IBM Statistical Package for the Social Sciences version 22 for Windows. Continuous and categorical variables were expressed as mean ± standard deviation and percentages, respectively
- Descriptive statistics were done for the distribution of surgeries done, the approach used for nailing
- Chi-square test was used to see the difference in distribution of age group, gender, type of surgery, fracture site, side of fracture, and AO Classification, between the two groups
- An independent t-test was done to compare the Radiographic Union Scale for Tibia (RUST) score, Visual Analog Scale (VAS) score, and Lysholm’s score between the two groups on day 2, 2 weeks, 6 weeks, 12 weeks, and 6 months
- Two-sided P-values were considered statistically significant at P < 05.
- (Fig. 1 & 2.)
• Among 85 study participants, 40 (47.1%) underwent thSP and 45 (52.9%) underwent the IP approach of nailing
• In the present study, almost 30 % of participants belonged to the age group 21-30 years and 20 % belonged to the age group 31- 40 years. There is no significant difference (P = 0.329) in the distribution of age groups between the two groups. The Mean Age of the SP group was 41.67 ± 16.17; the IP group was 36.80 ± 16.19, and for the overall study participants was 39.09 ± 16.27 years
• Almost 80 % of participants were male and 20 % were female. There is no significant difference (P = 0.802) in the distribution of gender between both the groups
• Nearly ¾ of participants had closed fractures and ¼ had open fractures. There is no significant difference (P = 0.763) in the distribution of the type of Fracture between the groups
• There was no significant difference in the distribution of fracture sites between the two groups, although there was more of middle site fracture (51.1%) in IP compared to SP (37.5%) and more of distal (52.5%) and proximal (10%) site fracture in SP than distal (42.2%) and proximal (6.7%) site fracture in SP
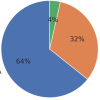
• Most of the participants belonged to the 42A3 classification, followed by 42A2 in both groups, and also 42B2 in the IP group. The difference in distribution was not significant (P = 0.205) (Fig. 3).
• There was no significant difference (P > 0.05) in RUST score between the two groups at Day 2, 2 weeks, 6 weeks, 12 weeks, and 6 months. (Fig. 4).
There was no significant difference (P > 0.05) in VAS score between the two groups at Day 2 and 2 weeks. A statistically significant difference (P < 0.05) was found at 6 weeks, at 12 weeks, and 6 months. (Fig. 5).
• There was no significant difference (P > 0.05) in Lysholm score between the two groups at 2 weeks. A statistically significant difference (P < 0.05) was found at 6 weeks, 12 weeks, and 6 months, although the difference was not much clinically significant
• Both groups had 100% Acceptable alignment at each time interval
• There is no significant difference (P = 0.342) in time required for union between the two groups, although SP takes less time (19.27 ± 3.69 weeks) compared to IP (20.13 ± 4.60) weeks
• There was no intraoperative complication in 90% of patients in the SP group and 100% in the IP group. In 4 patients with the SP approach, there was difficulty in passing the patella protection sleeve, so a 10 ml syringe was cut and used as a sleeve
• Post-operative Complication was not found in 92.5% of the SP group and 73.3% of the IP group. 26.7% of them had knee pain in the IP group, and 2.5% had knee stiffness in the SP group.
In this study, we had compared functional and radiological outcomes between the SP and IP approaches for IMN in tibial fractures. Out of 105 patients assessed during the study period, 85 met the inclusion criteria and were randomized using the SNOSE method. Forty patients were allocated to the SP group and 45 to the IP group. The demographic profile showed that the majority of patients were male (80%), with the largest age group being 21–30 years (approximately 30%). The mean age in the SP group was 41.67 ± 16.17 years, and in the IP group, 36.80 ± 16.19 years. Most fractures were closed (75%), primarily classified as AO 42A3, followed by 42A2 and 42B2. Fracture distribution by site and side (midshaft/distal shaft and left/right) was similar across groups. Post-operative assessments included the RUST, VAS for pain, Lysholm’s functional score, and radiographic alignment. Evaluations were conducted on post-operative day 2, and subsequently at 2 weeks, 6 weeks, 12 weeks, and 6 months. Lysholm’s scores were not assessed on day 2. RUST scores demonstrated no statistically significant differences at any follow-up interval (P > 0.05), which is consistent with the findings of Umur et al., who reported no significant difference in radiological union scores between the two approaches [17]. Similarly, radiographic alignment was 100% acceptable in both groups, suggesting this outcome is largely surgeon-dependent. VAS score analysis revealed no significant difference at day 2 and 2 weeks; however, from 6 weeks onwards, the SP group exhibited significantly lower pain scores. This aligns with findings by MacDonald et al., who reported reduced post-operative anterior knee pain in patients undergoing the SP approach [18]. Lysholm’s scores were comparable at 2 weeks but were significantly higher in the SP group at 6 weeks, 12 weeks, and 6 months. While statistically significant, the clinical impact may be limited. These findings are similar to the meta-analysis by Wang et al., which concluded that the SP approach yields superior functional outcomes [19]. Time to union was marginally shorter in the SP group (19.27 weeks) compared to the IP group (20.13 weeks), although the difference was not statistically significant, supporting the results of Chen et al. [19]. Functionally, our study demonstrated superior Lysholm scores in the SP group at 6 weeks, 12 weeks, and 6 months, indicative of faster and more comfortable recovery. This is consistent with the outcomes reported by Panda et al., where SP patients had better early KOOS, KOOS-PF, and EQ-5D-5L scores at 6 months. Although long-term (12-months) Lysholm scores were not significantly different in their study, the early post-operative functional advantage with SP nailing is notable [20]. Intraoperative complications occurred in 10% of SP cases, primarily due to difficulty in inserting the patella protection sleeve. In some cases, a modified 10 ml syringe was used as a substitute, suggesting a need for narrower sleeves tailored to patients with smaller anatomical dimensions. Two cases were converted to the IP approach due to failed sleeve insertion. Post-operative complications were fewer in the SP group (8%) compared to the IP group (27%), with anterior knee pain being more prevalent in the latter (26% vs. 5%). One case of post-operative knee stiffness was noted in the SP group. After compiling and analyzing the information at hand, it becomes clear that both approaches were comparable in terms of Radiological outcomes, which partly supports our hypothesis. The SP approach has better functional outcomes than the IP approach, which is statistically significant but may not be clinically significant. This is partly against our hypothesis.
Tibia shaft fractures are one of the prevalent injuries that can result from high or low-velocity trauma and involve more commonly males as compared to females. Surgical fixation gives faster rehabilitation and quicker recovery. Among surgical fixation, IMN is the most preferable method as compared to other approaches, such as plating or external fixator application. Intramedullary interlock nailing can be done via various approaches and older and conventional approaches have been IP with other approaches also described as SP, parapatellar etc. In this study, we compared the functional outcomes (VAS score, Lysholm’s score), and radiological outcomes (RUST score, Acceptable alignment, radiological time to union) of the SP approach with the conventional (IP) approach. In this trial, the participants (patients) were divided into two groups, one is SP and the other one IP approach, and assessed at 2nd day, 2 weeks, 6 weeks, 12 weeks, and 6 months after surgery for functional and radiological outcomes. The findings of our study suggest that there is no significant difference in the radiological outcomes of these surgical approaches while the SP approach has better functional outcomes than the IP approach, mainly at and after 6 weeks of surgery, which are statistically significant but may not be clinically significant. The advantages of the SP approach include ease in positioning of the limb and maintaining the reduction during insertion of the nail, less post-operative anterior knee pain and non-significant but less time to union. Patellar tendon splitting leading to the involvement of the IP nerve and the intra-articular damage were all causes of post-operative knee pain, which the SP approach attempts to prevent. Whenever there is difficulty in passing the patellar protection sleeve, joint can be dilated by intraarticular injection of normal saline or 10 ml syringe can be used instead of a patellar protection sleeve. Although there is 1 case reported of knee stiffness with the SP approach, its root cause has to be investigated. It is essential to conduct more comparative research and assessment of other parameters of radiological and functional outcomes.
Limitations
This study has several limitations that should be considered while interpreting the findings. First, it was conducted at a single tertiary care centre, which may limit the external validity and generalizability of the results to other healthcare settings. Second, although the sample size was adequately powered for primary outcomes, the total cohort of 85 patients may be insufficient to detect smaller but clinically meaningful differences, particularly for less common complications. The duration of follow-up was limited to 6 months, which precludes assessment of long-term outcomes, such as persistent anterior knee pain, implant-related complications, or late functional decline. A longer follow-up period would provide a more comprehensive evaluation of the durability of outcomes. The study employed a single-blind design in which only patients were blinded to the surgical approach. Surgeons and outcome assessors were not blinded, introducing the possibility of performance and observer bias. In addition, surgeon-dependent factors, such as familiarity with each approach and operative experience may have influenced intraoperative ease, reduction quality, and complication rates, although the majority of cases have been operated by the team of surgeons, including the author. Objective assessment of patellofemoral cartilage status was not performed using post-operative MRI or arthroscopy; therefore, potential subclinical cartilage injury associated with the SP approach could not be evaluated. Functional outcomes were assessed using VAS and Lysholm scores, which are patient-reported measures and may be influenced by subjective perception. Broader health-related outcome measures, such as KOOS, SF-36, or EQ-5D were not included. The study included a heterogeneous group of fracture patterns (AO 42A, B, C, and 43A), which may influence healing and functional recovery. Subgroup analysis based on fracture location (proximal, midshaft, distal) was not performed. Only Gustilo-Anderson type I and II open fractures were included, limiting applicability to more severe open injuries. A potential learning-curve effect associated with the SP approach may have influenced operative parameters and intraoperative challenges. Economic considerations, such as cost of instrumentation and operative time were not analysed. Furthermore, post-operative rehabilitation compliance was not objectively measured, which may have influenced functional outcomes. Finally, although several functional differences reached statistical significance, their clinical relevance – particularly with respect to Lysholm score differences – may be modest. Larger multicentre trials with longer follow-up are required to validate these findings.
Suprapatellar nailing for tibial fracture gives a promising functional and radiological outcome and at the same time it’s easy to maintain reduction and positioning of patient intraoperatively.
References
- 1. Court-Brown CM, Caesar B. Epidemiology of adult fractures: A review. Injury 2006;37:691-7. [Google Scholar] [PubMed]
- 2. Kazley J, Jahangir A. Tibia Diaphyseal Fracture. Treasure Island, FL: StatPearls; 2019. [Google Scholar] [PubMed]
- 3. Larsen P, Elsoe R, Hansen SH, Graven-Nielsen T, Laessoe U, Rasmussen S. Incidence and epidemiology of tibial shaft fractures. Injury 2015;46:746-50. [Google Scholar] [PubMed]
- 4. Zhang J, Stevenson A, Zhou A, Lu V, Josipović M, Bradshaw F, et al. 1118 epidemiology of tibial fractures, a UK major trauma centre perspective. Br J Surg 2023;110:znad258.696. [Google Scholar] [PubMed]
- 5. Gosman JH, Hubbell ZR, Shaw CN, Ryan TM. Development of cortical bone geometry in the human femoral and tibial diaphysis. Anat Rec (Hoboken) 2013;296:774-87. [Google Scholar] [PubMed]
- 6. Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, DeCoster TA, et al. Fracture and dislocation classification compendium – 2007: Orthopaedic trauma association classification, database and outcomes committee. J Orthop Trauma 2007;21:S1-133. [Google Scholar] [PubMed]
- 7. Kwasnicki RM, Hettiaratchy S, Okogbaa J, Lo B, Yang GZ, Darzi A. Return of functional mobility after an open tibial fracture: A sensor-based longitudinal cohort study using the hamlyn mobility score. Bone Jt J 2015;97-B:1118-25. [Google Scholar] [PubMed]
- 8. Larsen P, Lund H, Laessoe U, Graven-Nielsen T, Rasmussen S. Restrictions in quality of life after intramedullary nailing of tibial shaft fracture: A retrospective follow-up study of 223 cases. J Orthop Trauma 2014;28:507-12. [Google Scholar] [PubMed]
- 9. Lefaivre KA, Guy P, Chan H, Blachut PA. Long-term follow-up of tibial shaft fractures treated with intramedullary nailing. J Orthop Trauma 2008;22:525-9. [Google Scholar] [PubMed]
- 10. Hiesterman TG, Shafiq BX, Cole PA. Intramedullary nailing of extra-articular proximal tibia fractures. J Am Acad Orthop Surg 2011;19:690-700. [Google Scholar] [PubMed]
- 11. Tornetta P 3rd, Collins E. Semiextended position of intramedullary nailing of the proximal tibia. Clin Orthop Relat Res 1996;328:185-9. [Google Scholar] [PubMed]
- 12. Cole JD. Distal tibia fracture: OPINION: Intramedullary nailing. J Orthop Trauma 2006;20:73-4. [Google Scholar] [PubMed]
- 13. Franke J, Hohendorff B, Alt V, Thormann U, Schnettler R. Suprapatellar nailing of tibial fractures-Indications and technique. Injury 2016;47:495-501. [Google Scholar] [PubMed]
- 14. Hernigou P, Cohen D. Proximal entry for intramedullary nailing of the tibia. The risk of unrecognised articular damage. J Bone Joint Surg Br 2000;82:33-41. [Google Scholar] [PubMed]
- 15. Sun Q, Nie XY, Gong JP, Wu JZ, Li RL, Ge W, et al. The outcome comparison of the suprapatellar approach and infrapatellar approach for tibia intramedullary nailing. Int Orthop 2016;40:2611-7. [Google Scholar] [PubMed]
- 16. Jones M, Parry M, Whitehouse M, Mitchell S. Radiologic outcome and patient-reported function after intramedullary nailing: A comparison of the retropatellar and infrapatellar approach. J Orthop Trauma 2014;28:256-62. [Google Scholar] [PubMed]
- 17. Umur L, Sari E, Orhan S, Sürücü S, Yildirim C. Dilemma of supra- or infrapatellar tibial nailing: Anterior knee pain vs. Intra-articular damage. Int J Clin Pract 2022;2022:8220030. [Google Scholar] [PubMed]
- 18. MacDonald DR, Caba-Doussoux P, Carnegie CA, Escriba I, Forward DP, Graf M, et al. Tibial nailing using a suprapatellar rather than an infrapatellar approach significantly reduces anterior knee pain postoperatively: A multicentre clinical trial. Bone Joint J 2019;101-B:1138-43. [Google Scholar] [PubMed]
- 19. Wang C, Chen E, Ye C, Pan Z. Suprapatellar versus infrapatellar approach for tibia intramedullary nailing: A meta-analysis. Int J Surg 2018;51:133-9. [Google Scholar] [PubMed]
- 20. Panda SS, Jain M, Patro BP, Patra SK, Pradhan S. Assessment of functional and radiological outcomes of suprapatellar and infrapatellar approaches of tibial nailing in patients with tibial shaft fracture: A randomized control study. J Clin Orthop Trauma 2024;55:102515. [Google Scholar] [PubMed]