This study demonstrates the feasibility of day-care total hip arthroplasty (THA) using the direct anterior approach (DAA) within the urban Indian population when integrated with enhanced recovery after surgery (ERAS) protocols. It highlights that high early functional outcomes can be achieved through minimally invasive techniques, multimodal analgesia, and early mobilization. Importantly, it identifies that sociocultural apprehensions, rather than clinical limitations, are the primary barriers to same-day discharge. The findings underscore the need for structured patient education, caregiver involvement, and post-operative support to improve acceptance of outpatient THA in resource-constrained and culturally diverse settings like India.
Dr. Kunal Aneja, Max Super Speciality Hospital, Shalimar Bagh, New Delhi, India/Naveda Healthcare Centers, New Delhi, India. E-mail: drkunalaneja@gmail.com
Introduction: While total hip arthroplasty (THA) has evolved toward outpatient care in many regions, its adoption in the Indian subcontinent remains limited due to cultural apprehensions, logistical barriers, and concerns regarding early discharge safety. This study evaluates the feasibility, safety, and functional outcomes of day-care direct anterior approach (DAA) THA in the urban Indian population using enhanced recovery after surgery (ERAS) protocols.
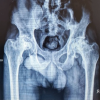
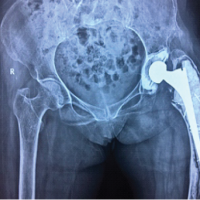
Materials and Methods: Data of 76 American society of anesthesiologist I/II patients, aged 22–50 years, with avascular necrosis of the femoral head who underwent DAA THA under a standardized ERAS protocol were retrospectively assessed. Pre-operative education, multimodal analgesia, and early mobilization were incorporated. Data on demographics, surgical metrics, length of stay (LOS), complications, and functional outcomes using Harris Hip score (HHS) and Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) scores were also analyzed postoperatively at 2- and 6-weeks, 6 months and 1 year.
Result: The mean age was 35.1±8.4 years (54 males, 22 females). The mean surgical time was 213.45±22.13 min, with an average blood loss of 201.7±20.72 mL. No intraoperative complications or transfusions were required. A total of 31 patients (40.8%) were discharged within 24 h, while 45 patients (59.2%) remained hospitalized beyond 24 h due to concerns about complications and post-operative symptoms. The longest stay was 3 days, due to post-operative nausea and vomiting. The average LOS was 1.8 days. At 1 year, the mean HHS increased from 44.6 (pre-operative) to 97.1, and the WOMAC score improved from 74.6 (pre-operative) to 10.2. No readmissions or major post-operative complications were observed.
Conclusion: Day-care THA using DAA achieved high early functional outcomes through minimally invasive techniques, multimodal analgesia, and enhanced recovery protocols. Pre-operative counseling and structured discharge planning enabled a significant proportion of patients to opt for same-day discharge, though sociocultural apprehensions remained a barrier. Strengthening patient education, caregiver involvement, and post-operative support is essential to further improve acceptance of outpatient THA in the Indian population.
Keywords: Direct anterior approach, day care surgery, total hip arthroplasty, avascular necrosis, patient education, enhanced recovery after surgery protocols, urban Indian population.
With the increasing demand for joint replacement surgeries, optimizing surgical efficiency while maintaining patient safety has become a critical focus in orthopedic care. Total hip arthroplasty (THA) is a well-established procedure that restores mobility and alleviates pain in patients with advanced hip pathology [1]. However, the strain on healthcare resources, coupled with concerns over hospital capacity and rising costs, has driven the need for streamlined perioperative pathways that facilitate early discharge without compromising outcomes [2]. In this context, outpatient THA has emerged as a viable strategy, particularly in urban settings where healthcare systems are under strain to enhance surgical throughput and reduce hospitalization. The concept of enhanced recovery after surgery (ERAS), originally developed for colorectal procedures, has gained traction in orthopedic surgery [3,4]. ERAS protocols employ a multimodal approach that includes pre-operative education, optimized analgesia, minimally invasive surgical techniques, and early mobilization, with the overarching goal of reducing surgical stress and facilitating faster recovery [5]. In recent years, ERAS pathways have demonstrated significant success in shortening hospital length of stay (LOS) without compromising patient safety or satisfaction [4]. These outcomes have been further supported by innovations in surgical approaches such as the direct anterior approach (DAA), which minimizes soft-tissue damage, facilitates earlier post-operative mobilization, and lowers the risk of dislocation and post-operative narcotic requirements [6]. Studies have shown that early organ dysfunction, pain, nausea, fatigue, dizziness and orthostatic hypotension is the primary barrier to same-day discharge following THA [7]. These symptoms are often the result of neuroendocrine and inflammatory responses triggered by surgical trauma [8]. Addressing these physiological stressors through targeted interventions, including advanced anesthesia techniques and rigorous post-operative protocols, has proven critical in enabling outpatient arthroplasty [9]. In addition, fast-track programs that incorporate enhanced rehabilitation strategies and streamlined organizational processes have been shown to lower morbidity, mortality, and overall costs while improving patient outcomes and reducing LOS [8]. Despite the promising outcomes associated with outpatient THA, its adoption in the urban Indian diaspora remains limited. Cultural perceptions, logistical challenges, and the lack of standardized care pathways contribute to the slower implementation of day-care models in this population [10]. However, with the rising demand for THA in India and the increasing emphasis on cost-effectiveness, there is an urgent need to optimize outpatient surgical pathways tailored to the unique demographic and healthcare infrastructure of the region. Notably, many of these pathways emphasize the importance of patient education and managing patient expectations as critical components of successful implementation [11]. This study aims to assess the feasibility and clinical outcomes of day-care DAA THA within the urban Indian population. Utilizing evidence-based ERAS protocols and addressing population-specific challenges, the research aims to propose practical strategies to optimize healthcare delivery, minimize LOS, and improve patient satisfaction in resource-limited settings. The study also evaluates discharge patterns, patient-reported reasons for prolonged hospital stays, and functional outcomes. The findings highlight the complex interplay of patient apprehensions regarding day-care surgery in India and emphasize the pivotal role of structured patient education in overcoming these barriers.
Study design and patient selection
This retrospective cohort study analyzed data from an institutional database to identify all primary THAs performed in a routine clinical setting by a single experienced surgeon between January 2023 and December 2023. Day-care/outpatient THA was defined as hospital admission and discharge occurring within the same calendar day. All consecutive patients meeting the inclusion criteria during the study period were included to reflect real-world clinical practice. The study included consecutive self-funded patients who underwent primary THA for avascular necrosis (AVN) of the femoral head at a single institution. The most common etiologies of AVN in this cohort were previous COVID-19 infection (leading to suspected vascular compromise or inflammatory sequelae), idiopathic causes, chronic steroid usage and alcohol consumption. Inclusion criteria comprised primary THA, American Society of Anesthesiologists (ASA) physical status of 1 or 2, ensuring medical fitness for minimally invasive surgery under the ERAS pathway, availability of a dedicated support person throughout the recovery period, and willingness to provide informed consent, while exclusion criteria included patients with higher ASA scores (≥3), complex medical comorbidities to minimize perioperative risks, and lack of a reliable social support system or home assistance, rendering them ineligible for outpatient surgery. Given the retrospective observational design of the study, no formal sample size calculation was performed.
Data collection
Patient demographics, including age, body mass index (BMI), and ASA classification, were retrieved from the institutional database. Perioperative data, including operative duration, estimated blood loss, adverse events, transfusion requirements, hospital LOS, and discharge disposition, were retrospectively reviewed. Perioperative complications, defined as any wound or systemic issues occurring within 6 weeks post-surgery, were identified through documented emergency room visits, readmissions, or self-reports recorded at 6-week follow-up visits. Functional assessments and patient-reported outcome measures, including Harris Hip Score (HHS) and Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), were extracted from medical records and evaluated preoperatively and at post-operative intervals of 2-, and 6 weeks, 6 months and 1 year.
Pre-operative care and education
As part of pre-operative preparation, patients and their families participated in multidisciplinary counseling sessions led by orthopedic surgeons, anesthesiologists, and physiotherapists. These sessions comprehensively addressed:
- The surgical steps of the DAA THA procedure
- Expected recovery milestones and timelines
- Potential complications and their management
- The feasibility and benefits of discharge within 24 h under the ERAS
To facilitate patient comprehension, a multimodal educational approach incorporating visual aids, instructional videos, and interactive anatomical models was implemented. Printed educational materials, available in multiple languages, provided supplementary reinforcement of key perioperative concepts. All patients were required to have access to a 24-h caregiver at home to ensure adequate post-operative support upon discharge.
ERAS protocol
All patients were managed using a standardized ERAS pathway detailed in Table 1 (Appendix with full protocol details). Key components of appendix include:
- Pre-operative optimization: Smoking cessation counseling, medical optimization of any mild comorbidities, and carbohydrate-loading drinks up to 2 h preoperatively.
- Anesthesia and analgesia: A multimodal analgesia approach with limited opioids, incorporating peripheral nerve blocks or local infiltration analgesia, and prophylactic
- Intraoperative care: All procedures were performed by a single experienced surgeon using a minimally invasive DAA. Cementless THA was performed in all cases under a standardized ERAS pathway. The mean incision-to-closure time was 55.2 ± 7.8 min per hip. With meticulous soft-tissue handling and hemostasis, resulting in an average blood loss of ~200 mL.
- Post-operative recovery: Early mobilization, typically starting 4–6 h post-surgery, combined with proactive physiotherapy and pain control.
- Discharge criteria: Stable vital signs, ability to ambulate with assistance, tolerable pain levels, and no concerning laboratory abnormalities.
Patient demographics and surgical details
This study analyzed data from 76 patients (54 males, 22 females; Fig. 1) (Table 2) with a mean age of 35.06 ± 8.39 years (range: 22–50 years) diagnosed with AVN of the femoral head. The primary etiologies were categorized as COVID-19-related vascular compromise or inflammatory sequelae (44.73%), idiopathic causes (27.63%), and chronic alcohol consumption or steroid use (27.63%) (Fig. 2). All patients were classified as ASA 1 (n = 35) or 2 (n = 39) (Fig. 3), with a mean BMI of 25.34 ± 2.73 kg/m2 (Table 1). The DAA THA was performed with a mean surgical time of 54.40 ± 5.25 min per hip resulting in a total bilateral operative duration of 213.45 ± 22.13 min and an average intraoperative blood loss of 201.7 ± 20.72 mL (Table 3). Notably, no patients required intraoperative or post-operative blood transfusion.
LOS and discharge patterns
All patients were offered discharge within 24 h under the ERAS protocol. Among 76 patients, 40.8% (n = 31) chose to be discharged at or before the 24-h mark. The majority, 59.2% (n = 45), elected to stay longer, citing concerns such as apprehension about immediate access to surgeons or hospital facilities in case of complications, generalized anxiety regarding potential unforeseen issues at home, and lack of familiarity with day care surgical pathways (Table 4). The overall average LOS for all patients was 1.8 days, reflecting the successful integration of the ERAS protocol while accommodating patient preferences and concerns. The single longest stay was 3 days, attributed to a patient experiencing post-operative nausea and vomiting (PONV) (Table 4).
Clinical and functional outcomes
All patients successfully achieved early mobilization within 4–6 h post-surgery, a critical milestone in ERAS protocol. Patients reported high satisfaction with both pain management and overall recovery, highlighting the effectiveness of the multimodal analgesia strategy and patient-centred perioperative care.
Functional outcomes demonstrated significant improvement, with the mean HHS increasing from a pre-operative baseline of 44.64–67.73 at 2 weeks and further to 97.08 at 1-year post-operative follow-up period (Fig. 4). Similarly, WOMAC scores decreased from a pre-operative mean of 74.63–44.23 at 2 weeks postoperatively and further to 10.21 at 1 year (Fig. 5), reflecting substantial functional recovery and improved patient-reported outcomes.
Complications and readmissions
The study reported no major complications, such as infections, prosthetic failures, or dislocations, and no blood transfusions were required. One patient experienced persistent PONV, extending their hospital stay to 3 days (Table 4). During the 6-week follow-up, there were no readmissions or delayed complications.
The implementation of day care THA represents a significant advancement in orthopedic surgery, offering patients the benefit of reduced hospital stays, faster recovery, and lower healthcare costs [12]. However, the success of this approach in the Indian diaspora is contingent on addressing patient apprehension and fear, which can significantly impact pre-operative anxiety, post-operative recovery, and overall satisfaction. This retrospective assessment of day care DAA THA analyses the safety and feasibility of the procedure with ERAS protocols, the challenges posed by patient apprehension, strategies to mitigate these fears, and the implications for optimizing day care DAA THA in this demographic.
Safety and feasibility of DAA THA with ERAS
Outpatient THA is a safe and feasible option, specifically for patients classified as ASA 1 and 2 [13]. A large retrospective study on same-day THA discharge reported a major complication rate of 0.3% within 48 h postoperatively, reinforcing the safety of early discharge in appropriately selected patients [14]. According to the literature, these patients are typically medically informed, have no significant comorbidities, possess adequate home support, and demonstrate the ability to adhere to post-operative care protocols [14]. These findings are consistent with our retrospective analysis, which revealed no hospital readmissions due to complications or revision surgeries and an absence of significant major post-operative complications in the study cohort. PONV remains a common complication in fast-track surgery, typically occurring within 6 h postoperatively due to surgical stress or anesthesia-related factors. The use of opioids in analgesia has been identified as a contributing factor to PONV [15]. ERAS protocols, which emphasize multimodal pain management and reduced opioid use, can significantly decrease the incidence of PONV and facilitate outpatient surgery [13]. In a multicenter prospective study (n = 220), the authors found that 24% (n = 27/112) of planned outpatient procedures were converted to overnight stays due to nausea and dizziness-associated hypotension [16]. Our study observed PONV in 1 patient (1.3%), requiring an extended hospital stay beyond 24 h. However, no other major complications, such as infection, dislocation, or implant failure, were noted.
Clinical and functional outcomes
The implementation of a multimodal enhanced recovery approach in THA has been shown to significantly improve early clinical and functional outcomes in THA. In our study, patients undergoing THA through DAA exhibited a substantial improvement in functional scores, with the HHS increasing from a pre-operative mean of 44.64 to 82.65 at 6 weeks and 97.08 at 1-year postoperatively, while the WOMAC score decreased from 74.63 to 27.43 at 6 weeks and further decreased to 10.21 during the same period. These results are consistent with those reported by Kutzner et al. [17], who observed an HHS of 93.8 (± 8.0) 6 weeks after surgery following ERAS approach, and Leiss et al. [18], who reported an improvement in HHS from 52.95 preoperatively to 91.99 at 12 months postoperatively with a similar approach. These findings underscore the efficacy of enhanced recovery protocols in achieving excellent functional outcomes in outpatient THA. Comparative studies have also shown that patients undergoing DAA THA achieve better early functional scores than those receiving a direct lateral approach, with higher HHS and Lower Extremity Activity scores at 6 weeks [19]. In addition, the DAA has been linked to shorter hospital stays, making it a strong candidate for inclusion in enhanced recovery protocols without increasing complication rates during the transition to this technique [20]. Studies further suggest that the functional benefits of the DAA are sustained for at least 4–12 weeks postoperatively, reinforcing its role in accelerating recovery [21]. Our results align with these studies, demonstrating that the multimodal enhanced recovery protocol, combined with the DAA, facilitates significant improvements in early post-operative functional outcomes for patients undergoing THA. Larsen et al. demonstrated the feasibility and safety of day-case THA using a structured clinical pathway, reporting no major complications or readmissions at 6 weeks [22]. While their study focused on conventional THA, our findings highlight that day-case THA using DAA can also achieve excellent early functional outcomes when combined with ERAS protocol. The minimally invasive nature of the DAA, with reduced soft-tissue disruption and faster post-operative mobilization, likely contributed to improved functional outcomes and successful early discharge in 40.8% of patients.
Patient apprehension and fear: A multifaceted challenge
Patient apprehension remains a significant barrier to the adoption of outpatient THA. Fear of pain, surgical complications, and uncertainty about outcomes contribute to pre-operative anxiety [23]. In the urban Indian setting, additional sociocultural factors, such as familial expectations and traditional beliefs, further exacerbate these concerns. The concept of day-care surgery, where patients are discharged within 24 h, may be perceived as rushed or inadequate, leading to heightened anxiety. Many patients and their families believe that extended hospital stays are necessary for optimal recovery, a cultural mindset that can hinder the acceptance of early discharge protocols [24]. In addition, patients frequently express concerns about insufficient post-operative care at home and their ability to cope with the physical and emotional demands of major surgical procedures [25]. Despite the high success and low complication rates of DAA THA, our study found that only 40.8% of patients opted for discharge within 24 h, while 59.2% chose to stay beyond this period. These findings highlight the unique sociocultural and logistical barriers to early discharge in this population. Concerns regarding immediate access to hospital care, apprehensions about post-operative complications, and a lack of understanding and confidence in outpatient surgical protocols – despite pre-operative counseling – due to overall lower awareness contribute to patient hesitation. This trend aligns with findings from a systematic review, which identified advanced age, female sex, and comorbidities such as hypertension and diabetes as significant predictors of extended hospital stays post-THA [26]. These factors may further contribute to patient reluctance toward same-day discharge. In addition, previous studies indicate that surgical duration and anesthesia time influence hospital stay length, with prolonged operative times leading to increased post-operative monitoring and extended hospitalization [27].
Strategies to mitigate patient apprehension
To optimize day care DAA THA, it is essential to implement strategies that address patient apprehension and fear. Pre-operative education plays a pivotal role in reducing anxiety and improving patient satisfaction. Studies have shown that patients who receive comprehensive information about the procedure, expected outcomes, and post-operative care report lower anxiety levels and higher satisfaction [28]. Mitigating patient apprehension regarding outpatient THA in the urban Indian population requires a structured, patient-centered approach that addresses both cultural and logistical concerns [29]. A key strategy involves comprehensive pre-operative counseling tailored to Indian patients, focusing on the safety, efficacy, and recovery expectations of same-day discharge. Many patients and their families perceive prolonged hospital stays as essential for optimal recovery, making it crucial to integrate culturally sensitive educational interventions that reinforce the benefits of early mobilization and home-based recovery. Involving family members in the pre-operative and post-operative process, providing them with structured guidance on wound care, mobility, and medication adherence, can enhance patient confidence in home-based recovery and may help further alleviate patient fears and anxieties. In the Indian diaspora, family plays a central role in healthcare decision-making, and their reassurance can significantly reduce patient apprehension [24,29]. Equipping families with comprehensive and clear information regarding the surgical procedure and recovery process can cultivate a supportive environment, thereby bolstering patient confidence [24,29]. In addition, the integration of peer support groups and patient testimonials may further reinforce trust in early discharge protocols, promoting greater acceptance and adherence. Strengthening post-operative support systems is equally critical, particularly in India, where home healthcare infrastructure remains underdeveloped. Establishing 24/7 helplines, dedicated emergency contact teams, and structured telemedicine follow-ups within 24–48 h postoperatively can alleviate fears of limited hospital access.
Limitations
This study has several limitations. As a single-center study, its findings may not be generalized to other healthcare settings with different infrastructures or patient demographics. The small sample size limits broader applicability, and the inclusion of only ASA 1 or 2 patients introduces selection bias, restricting relevance to healthier individuals. The urban Indian population focus adds cultural specificity, affecting result transferability. However, one of the primary strengths of this study is its real-world applicability, as it evaluates outpatient THA using DAA within the urban Indian population, a demographic where data on same-day discharge protocols remains scarce. By analyzing a retrospective cohort, this study provides valuable insights into patient apprehensions, sociocultural influences, and logistical barriers to early discharge, contributing to a better understanding of the challenges and feasibility of outpatient THA in resource-limited settings. In addition, the inclusion of functional outcome measures, such as HHS and WOMAC, allows for an objective assessment of early recovery patterns, reinforcing the effectiveness of enhanced recovery protocols.
This study demonstrates that outpatient THA using DAA can achieve excellent early functional outcomes when combined with a structured ERAS protocol. The use of minimally invasive techniques, multimodal analgesia, and early mobilization strategies may have contributed to significant improvements in post-operative function. In addition, targeted pre-operative counseling and patient education helped motivate a substantial proportion of patients to opt for same-day discharge, reinforcing the importance of clear communication and structured discharge planning. However, persistent sociocultural apprehensions, anxiety, and concerns about post-operative care highlight the need for stronger patient engagement, caregiver involvement, and post-operative support systems to further improve acceptance of early discharge. Future research should focus on optimizing discharge protocols and addressing patient concerns, along with long-term functional assessment to expand the feasibility of outpatient THA in India.
Day-care THA using the DAA is clinically safe and effective in appropriately selected patients. However, overcoming sociocultural apprehensions through targeted education and structured post-operative support is essential to broaden its acceptance in the Indian healthcare context.
References
- 1. Shapira J, Chen SL, Rosinsky PJ, Maldonado DR, Lall AC, Domb BG. Outcomes of outpatient total hip arthroplasty: A systematic review. Hip Int 2021;31:4-11. [Google Scholar] [PubMed]
- 2. Pollock M, Somerville L, Firth A, Lanting B. Outpatient total hip arthroplasty, total knee arthroplasty, and unicompartmental knee arthroplasty: A systematic review of the literature. JBJS Rev 2016;4:e4. [Google Scholar] [PubMed]
- 3. Li J, Zhu H, Liao R. Enhanced recovery after surgery (ERAS) pathway for primary hip and knee arthroplasty: Study protocol for a randomized controlled trial. Trials 2019;20:599. [Google Scholar] [PubMed]
- 4. Malek IA, Royce G, Bhatti SU, Whittaker JP, Phillips SP, Wilson IR, et al. A comparison between the direct anterior and posterior approaches for total hip arthroplasty: The role of an ‘Enhanced Recovery’ pathway. Bone Joint J 2016;98-B:754-60. [Google Scholar] [PubMed]
- 5. Zhu S, Qian W, Jiang C, Ye C, Chen X. Enhanced recovery after surgery for hip and knee arthroplasty: A systematic review and meta-analysis. Postgrad Med J 2017;93:736-42. [Google Scholar] [PubMed]
- 6. Galakatos GR. Direct anterior total hip arthroplasty. Mo Med 2018;115:537-41. [Google Scholar] [PubMed]
- 7. Lamo-Espinosa JM, Mariscal G, Gómez-Álvarez J, Benlloch M, San-Julián M. Causes and risk factors for same-day discharge failure after total hip and knee arthroplasty: A meta-analysis. Sci Rep 2024;14:12627. [Google Scholar] [PubMed]
- 8. Vehmeijer SB, Husted H, Kehlet H. Outpatient total hip and knee arthroplasty. Acta Orthop 2018;89:141-4. [Google Scholar] [PubMed]
- 9. Okamoto T, Ridley RJ, Edmondston SJ, Visser M, Headford J, Yates PJ. Day-of-surgery mobilization reduces the length of stay after elective hip arthroplasty. J Arthroplasty 2016;31:2227-30. [Google Scholar] [PubMed]
- 10. Dash A, Senapati JN, Sahu MC. Evolvement of day care orthopaedic surgery in a tertiary care teaching institute. Int J Pharm Sci Rev Res 2016;37:15-8. [Google Scholar] [PubMed]
- 11. Padilla JA, Feng JE, Anoushiravani AA, Hozack WJ, Schwarzkopf R, Macaulay WB. Modifying patient expectations can enhance total hip arthroplasty postoperative satisfaction. J Arthroplasty 2019;34:S209-14. [Google Scholar] [PubMed]
- 12. Thompson JW, Wignadasan W, Ibrahim M, Beasley L, Konan S, Plastow R, et al. Day-case total hip arthroplasty: A literature review and development of a hospital pathway. Bone Jt Open 2021;2:93-102. [Google Scholar] [PubMed]
- 13. Sang W, Liu Y, Jiang Y, Xue S, Zhu L, Ma J. Direct anterior approach with enhanced recovery protocols in outpatient total hip replacement. Int J Clin Exp Med 2020;13:3608-15. [Google Scholar] [PubMed]
- 14. Berend KR, Lombardi AV Jr., Berend ME, Adams JB, Morris MJ. The outpatient total hip arthroplasty: A paradigm change. Bone Joint J 2018;100-B:31-5. [Google Scholar] [PubMed]
- 15. Wang Y, Yang Q, Lin J, Qian W, Jin J, Gao P, et al. Risk factors of postoperative nausea and vomiting after total hip arthroplasty or total knee arthroplasty: A retrospective study. Ann Transl Med 2020;8:1088. [Google Scholar] [PubMed]
- 16. Goyal N, Chen AF, Padgett SE, Tan TL, Kheir MM, Hopper RH Jr., et al. Otto aufranc award: A multicenter, randomized study of outpatient versus inpatient total hip arthroplasty. Clin Orthop Relat Res 2017;475:364-72. [Google Scholar] [PubMed]
- 17. Kutzner KP, Meyer A, Bausch M, Schneider M, Rehbein P, Drees P, et al. Outcome of an “Enhanced Recovery” program in contemporary total hip arthroplasty in Germany. Z Orthop Unfall 2020;158:214-20. [Google Scholar] [PubMed]
- 18. Leiss F, Götz JS, Maderbacher G, Meyer M, Reinhard J, Zeman F, et al. Excellent functional outcome and quality of life after primary cementless total hip arthroplasty (THA) using an enhanced recovery setup. J Clin Med 2021;10:621. [Google Scholar] [PubMed]
- 19. Connolly KP, Kamath AF. Direct anterior total hip arthroplasty: Comparative outcomes and contemporary results. World J Orthop 2016;7:94-101. [Google Scholar] [PubMed]
- 20. Free MD, Owen DH, Agius PA, Pascoe EM, Harvie P. Direct anterior approach total hip arthroplasty: An adjunct to an enhanced recovery pathway: Outcomes and learning curve effects in surgeons transitioning from other surgical approaches. J Arthroplasty 2018;33:3490-5. [Google Scholar] [PubMed]
- 21. Di Martino A, Keating C, Butsick MJ, Platano D, Berti L, Hunter LN, et al. Enhancing recovery: Surgical techniques and rehabilitation strategies after direct anterior hip arthroplasty. J Orthop Traumatol 2024;25:45. [Google Scholar] [PubMed]
- 22. Larsen JR, Skovgaard B, Prynø T, Bendikas L, Mikkelsen LR, Laursen M, et al. Feasibility of day-case total hip arthroplasty: A single-centre observational study. Hip Int 2017;27:60-5. [Google Scholar] [PubMed]
- 23. Akutay S, Ceyhan Ö. The relationship between fear of surgery and affecting factors in surgical patients. Perioper Med (Lond) 2023;12:22. [Google Scholar] [PubMed]
- 24. Raj V, Agarwal S, Kumar A, Bandil S. An analysis of socio-cultural barriers limiting timely discharge of patients after day care surgery: A prospective observational study. Int J Acad Med Pharm 2024;6:156-60. [Google Scholar] [PubMed]
- 25. Londhe SB, Shah RV, Patwardhan M, Doshi AP, Londhe SS, Subhedar K. Understanding the apprehension and concern haunting patients before a total knee arthroplasty. Arthroplasty 2021;3:14. [Google Scholar] [PubMed]
- 26. Baker P, Andrews SN, Mathews K, Nishioka S, Nakasone CK. Stepping toward outpatient total hip arthroplasty with a rapid discharge protocol. J Orthop 2021;27:153-7. [Google Scholar] [PubMed]
- 27. Fraser JF, Danoff JR, Manrique J, Reynolds MJ, Hozack WJ. Identifying reasons for failed same-day discharge following primary total hip arthroplasty. J Arthroplasty 2018;33:3624-8. [Google Scholar] [PubMed]
- 28. Moulton LS, Evans PA, Starks I, Smith T. Pre-operative education prior to elective hip arthroplasty surgery improves postoperative outcome. Int Orthop 2015;39:1483-6. [Google Scholar] [PubMed]
- 29. Muthu S, Jeyaraman M, Jeyaraman N, Ramasubramanian S. Optimizing outcomes: Implementing enhanced recovery after surgery in orthopedic surgery. World J Methodol 2024;14:95558. [Google Scholar] [PubMed]