Understanding the spinopelvic relationship is essential for optimizing acetabular component positioning in Total Hip Arthroplasty, as individualized assessment of pelvic tilt and functional anteversion helps minimize dislocation risk, enhance implant stability, and improve femoral head coverage for better long-term outcomes.
Dr. Sajal Maingi, Department of Orthopedics, Dayanand Medical College and Hospital, Rajpura DMC Rd, Block-B, Udham Singh Nagar, Tagore Nagar, Ludhiana - 141001, Punjab, India. E-mail: ssmaingi@gmail.com
Introduction: Dislocation remains one of the most common complications following total hip arthroplasty (THA). Although the classical “Lewinnek’s safe zone” for acetabular cup positioning has long guided surgeons, a considerable number of dislocations still occur even within this zone. Recent evidence emphasizes the importance of the dynamic spinopelvic relationship, specifically variations in pelvic tilt and functional anteversion, which directly influence acetabular orientation and joint stability. This study aims to analyze the spinopelvic relationship and its effect on acetabular cup anteversion and femoral head coverage in THA.
Materials and Methods: A total of 30 patients aged between 20 and 70 years undergoing primary THA were included in the study. Pre-operative assessment involved X-rays of the lumbar spine and pelvis in both supine and standing positions to determine changes in pelvic tilt. Acetabular anteversion was modified accordingly. Postoperatively, acetabular cup positioning and femoral head coverage were evaluated radiographically using the Woo and Morrey method for anteversion and the lateral center edge angle (LCEA) of Wiberg. Statistical analysis was performed using the Statistical Package for the Social Sciences version 23.
Results: The mean pelvic tilt in supine and standing positions was −3.30° and −5.77°, respectively, with a mean change of −2.44°. The mean target anteversion was 13.32°, and the mean achieved anteversion was 14.65°. The mean LCEA was 50.51°. A weak negative correlation was found between anteversion achieved and LCEA (ρ = −0.27, P = 0.141). The LCEA was highest when acetabular anteversion was within 5°–25°, suggesting optimal femoral head coverage within this range.
Conclusion: The study highlights that a fixed “safe zone” for acetabular cup placement is insufficient. Individualized cup orientation based on spinopelvic parameters enhances joint stability and femoral head coverage. Functional assessment of pelvic tilt and anteversion should be integrated into pre-operative planning to reduce the risk of impingement and dislocation in THA.
Keywords: Spinopelvic relationship, total hip arthroplasty, pelvic tilt, acetabular anteversion, femoral head coverage, lateral center edge angle.
Aim and background
Dislocation is among the most common complications after total hip arthroplasty (THA), with an estimated range between 0% and 5% [1,2,3]. The etiology of hip dislocation is multifactorial, including patient-specific factors such as females, developmental dysplasia of the hip (DDH), post-traumatic disorders, alcoholism, neurological impairment, and surgery- related factors such as component malposition, femoral head size, surgical approach, impingement, abductor muscle dysfunction, and revision surgery. Due to advances in modern implants, most atraumatic dislocations occur from altered spinopelvic kinematics that lead to a functionally unsafe acetabular position [4,5]. Lewinnek et al. defined a “safe zone” for acetabular component position 40 years ago [6]. However, despite the implementation of a “safe zone,” the incidence of impingement and subsequent dislocation remains unacceptably high. Some reports demonstrated up to 70% of dislocated hips had cups placed within Lewinnek’s safe zone of anteversion. Defining an updated acetabular orientation requires an understanding of the dynamic relationship between the hip joint, the spine, and the pelvis, as well as the alterations in posture and the effect of that relationship upon THA stability. Acetabular orientation is a dynamic parameter that can be impacted by forces acting on the pelvis by changes in pelvic tilt, obliquity, and rotation [7,8]. The surgeon can modify and alter these parameters, which in turn can also alter the orientation of the acetabular socket secondary to pelvic motion. The estimation of the safe zone remains largely dependent on static measurements that do not address the pelvis dynamic changes, even in navigation systems [9,10]. Changes in the spinal balance can alter pelvic rotation through changes in pelvic tilt and obliquity. Any preexisting condition that alters the pelvic tilt can affect the functional position of the acetabular cup [11,12]. Hence, in a patient with spinal deformity whose pelvis tilts posteriorly from the supine to the standing position, less anteversion is suggested to prevent anterior dislocation when standing. This is because posterior pelvic tilt creates an increase in functional anteversion. For every 1° change in posterior pelvic tilt, the anteversion increases by 0.8° [13]. The angle that should cause concern is not a specific number for pelvic tilt, but rather, the change from one position to another. Such patients need to be identified preoperatively to minimize the risk of posterior impingement and anterior edge-loading/dislocation. In cases of fixed flexion deformity, the pelvis tilts anteriorly, and the correction of acetabular implant anteversion is not required. In a flexion contracture, this may resolve to some degree after THA, and therefore, anatomical positioning is acceptable. In spinal deformity, increased anteversion is suggested. Patients with stiff spines will have less posterior pelvic tilt when moving from standing to the relaxed seated position. These patients need to be identified preoperatively as they will require increased anteversion to accommodate femoral flexion when sitting. The awareness for need of individualized cup orientation to avoid prosthetic articular impingement and edge loading has been growing recently. Sagittal pelvic kinematics vary amongst individuals and affects the risks of impingement and dislocation [14,15,16]. The present study aims to evaluate spinopelvic parameters preoperatively in patients undergoing primary THA and determine their influence on acetabular cup anteversion and femoral head coverage as measured by the lateral center edge angle (LCEA).
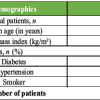
A total of 30 patients in the age group of 20–70 years underwent primary THA. Of the total participants, 46.7% had a diagnosis of avascular necrosis, 33.3% had a diagnosis of osteoarthritis, and 20.0% had a diagnosis of fracture neck femur (Table 1).

Table 1: Summary of basic details
Patients with concomitant spinal deformity secondary to spine fractures and those undergoing revision THA were excluded from the study. The institutional review board approved the study on October 30, 2019 (S.No: IEC/VMMC/SJH/Thesis/2019-10/197). Consenting patients were included in this study after being counseled about the surgical procedure and its outcomes.
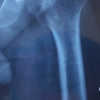
Any change in the pelvic tilt in supine and standing positions was measured, and the angle of anteversion of acetabular cup during total hip replacement (THR) was changed accordingly, excluding any change to anterior pelvic tilt from supine to standing position originating due to fixed flexion deformity at hip. Posterior pelvic tilt was represented as a negative angle, and anterior pelvic tilt was represented as a positive angle. The value of change in pelvic tilt was obtained by subtracting pelvic tilt supine from pelvic tilt standing. Standardized imaging protocol was used to improve accuracy on radiographic studies [17]. The anteroposterior pelvic radiographs (Fig. 1) were made with the patient supine on the X-ray table.

Figure 1: Anteroposterior radiograph of the pelvis with both hips in supine position used for pre-operative templating and assessment of acetabular orientation.
The X-ray tube-to-film distance was 120 cm with the tube oriented perpendicular to the table. To maximize the length of the femoral neck, both lower extremities were oriented in 15° of internal rotation. The crosshair of the beam was centered on the point midway between the superior border of the pubic symphysis and a line drawn connecting the anterior superior iliac spines. The lateral pelvic radiographs were made with the patient in supine (Fig. 2) and standing positions (Fig. 3).

Figure 2: Pre-operative lateral radiograph of the lumbosacral spine and pelvis in supine position showing change in pelvic tilt measurement.

Figure 3: Pre-operative lateral radiograph of the lumbosacral spine and pelvis in standing position showing baseline pelvic tilt measurement.
The X-ray tube-to-film distance was 120 cm with the tube-oriented perpendicular to the table in supine position and parallel to the floor in standing position. The crosshair of the beam was centered on the cranial tip of greater trochanter. Pelvic tilt was measured as an angle between the vertical and a line connecting the midpoint of the two anterior superior iliac spines with the pubic symphysis. Templating was done before each procedure.
Surgical procedure
Standard operative procedure was followed for anterolateral approach to the hip. Patients were placed in a lateral position, and the surgical incision was given beginning 2–4 cm lateral to the anterior superior iliac spine of the pelvis. It was then carried distally and posteriorly over the lateral aspect of the greater trochanter and shaft of femur. Surgical plane was made between gluteus medius and tensor fascia lata. The joint capsule was incised along the anterosuperior surface of the femoral neck. Gentle traction was then applied to the operative limb. Mueller and Hohmann retractors were placed intracapsularly around the femoral neck. A reciprocating saw was used to make a femoral neck osteotomy as per templating. Once the femoral head was removed, traction was released, and the leg was externally rotated to improve exposure for acetabular preparation. Care was taken right from the start of reaming to maintain the desired acetabular anteversion and inclination values. This was facilitated by the available anteversion jig in the instrumentation. The jig had an inbuilt angle of anteversion of 20° and inclination of 45°. The final acetabular components were then implanted in the well-prepared acetabular cavity. Femoral preparation was done. Once the final implants were in situ, the hip was reduced. Then, after thorough wash with saline, the closing of the surgical site was done by giving subcutaneous suturing followed by stapler application over skin. Then sterile dressing was done.
Post-operative assessment
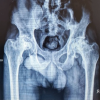
Postoperatively, X-rays of the pelvis with hip anteroposterior (Fig. 4) and cross-table lateral (Fig. 5) were done to assess the accuracy of acetabular cup positioning in terms of its anteversion and femoral head coverage achieved by the acetabular cup on the basis of measurement of LCEA of Weiberg.

Figure 4: Post-operative anteroposterior radiograph of the pelvis showing acetabular component placement and overall alignment following total hip arthroplasty.

Figure 5: Post-operative cross-table lateral radiograph demonstrating acetabular cup anteversion as measured by the Woo and Morrey method.
Acetabular anteversion was measured using the method of Woo and Morrey [18]. It was measured as the angle between a line touching the opening surface of the acetabular component and a line drawn perpendicular to the table. Computed tomography (CT) scan was not used to measure the anteversion angle due to factors like enhanced radiation exposure and investigation cost. LCEA of Weiberg was measured as an angle between measured between two lines originating at the center of the femoral head. One line extends superiorly perpendicular to the transverse axis of the pelvis. The second line passes through the lateral edge of the acetabular component. Same standardized imaging protocol was used to improve accuracy on radiographic studies [17]. The anteroposterior pelvic radiograph was made with the patient supine on the X-ray table. The cross-table lateral radiograph was made with the patient supine on the X-ray table with the contralateral hip and knee flexed beyond 80° and the symptomatic limb internally rotated 15° to expose the anterolateral surface of the femoral head-neck junction. The X-ray beam was kept parallel to the table and oriented at a 45° angle to the symptomatic limb, with the crosshairs directed at the center of the femoral head.
Statistical analysis
Data were coded and entered in MS Excel spreadsheet program. The Statistical Package for the Social Sciences version 23 was used for data analysis. Descriptive statistics were elaborated in the form of means/standard deviations (SD) and medians/interquartile range (IQRs) for continuous variables, and frequencies and percentages for categorical variables. Data were presented in a graphical manner wherever appropriate for data visualization using histograms/box-and-whisker plots/column charts for continuous data and bar charts/pie charts for categorical data. Group comparisons for continuously distributed data were made using the independent sample “t” test when comparing two groups. If data were found to be non-normally distributed, appropriate non-parametric tests in the form of the Wilcoxon Test were used. Chi-squared test was used for group comparisons for categorical data. In case the expected frequency in the contingency tables was found to be <5 for >25% of the cells, Fisher’s Exact test was used instead. Linear correlation between two continuous variables was explored using Pearson’s correlation (if the data were normally distributed) and Spearman’s correlation (for non-normally distributed data). Statistical significance was kept at P < 0.05.
The mean pelvic tilt supine was −3.30° (SD 6.39°). The mean pelvic tilt standing was −5.77° (SD 6.23°). The mean change in pelvic tilt was −2.44° (SD 9.38°). The mean change in functional anteversion was 1.69° (SD 6.53°). The mean Target Anteversion was 13.32° (SD 6.54°). The mean anteversion achieved was 14.65° (SD 6.65°). The mean LCEA was 50.51° (SD 4.84°) (Table 2).

Table 2: Summary of spino-pelvic parameters

Figure 6: Scatter plot showing correlation between acetabular anteversion achieved and lateral center edge angle depicting the relationship between anteversion and femoral head coverage.
Fig. 6 represents a scatterplot that depicts the correlation between anteversion achieved and LCEA. Individual points represent individual cases. The solid black trendline represents the general trend of correlation between the two variables. The shaded grey area represents the 95% confidence interval of this trendline. Non-parametric tests (Spearman Correlation) were used to explore the correlation between the two variables, as at least one of the variables was not normally distributed. There was a weak negative correlation between anteversion achieved and LCEA, and this correlation was not statistically significant (rho = −0.27, P = 0.141).

Table 3: Comparison of the 3 subgroups of the variable anteversion achieved category in terms of LCEA (n=30)
Table 3 represents a comparison of the 3 subgroups of the variable anteversion achieved category in terms of LCEA (n = 30). The variable LCEA was not normally distributed in the 3 subgroups of the variable anteversion achieved category. Thus, non-parametric tests (Kruskal–Wallis test) were used to make group comparisons. The mean (SD) of LCEA in the anteversion achieved categories <5, 5–25, and >25 were 49.30 (NA), 51.23 (4.59), 44.70 (4.19), respectively. The median (IQR) of LCEA in the anteversion achieved categories <5, 5–25, and >25 were 49.3 (49.3–49.3), 50.75 (48.18–54.17), and 45.7 (42.9–47), respectively. The LCEA in the anteversion achieved categories <5, 5–25, and >25 ranged from 49.3 to 49.3, 42.1 to 58.7, and 40.1–48.3, respectively.
There was no significant difference between the groups in terms of LCEA (χ2 = 4.740, P = 0.093).
Strength of association (Kendall’s Tau) = 0.24 (small effect size).
On changing position from supine to standing, the number of acetabular components in the safe zone decreased from 82% to 64% in a study conducted by Eilander et al. [19] on 56 patients. Abdel et al. [20] retrospectively identified from a cohort of 9784 THAs conducted at an institution, the 206 THAs that had dislocated and noted that 58% of the THAs which dislocated had a cup placed within Lewinnek’s safe zone. The mean cup inclination was 44°, with 84% of the THAs within the safe zone, and the mean cup anteversion was 15°, with 69% of the THAs in the safe zone. Spine-hip relationship has been progressively gaining importance among hip surgeons, and its understanding has now been deemed important to identify patients at high risk for dislocation and prevent it by individualizing the acetabular component orientation in each patient. Inaba et al. [21] studied 75 patients who underwent THA, and patients were divided into three groups on basis of standing pelvic tilt. Intermediate group (60%) had tilt between −10° and +10°, anterior tilt group (12%) had tilt of more than +10°, and posterior tilt group (28%) had tilt of more than −10°. In the supine position, mean inclination, mean anteversion, and mean combined anteversion were 39.3° ± 4.1°, 16.9° ± 6.0°, and 35.0° ± 5.8°, respectively. In the standing position, mean inclination, mean anteversion, and mean combined anteversion were 40.5° ± 4.2°, 20.8° ± 6.3°, and 38.9° ± 5.7°, respectively. The combined anteversion did not differ significantly in the three groups in either supine or standing position, as pre-operative planning for implant placement was done taking into consideration the pelvic tilt and executed with the help of a CT-based navigation system. In our study, we have tried to measure the spine-hip relationship preoperatively and place the acetabular component at anteversion angles specific to each patient based on their spine-hip relationship. Post-operative estimation of acetabular coverage of the femoral head has been done by measuring the LCEA of Weiberg. It measures the superolateral acetabular coverage of the femoral head more specifically. In a study by Tiberi et al. [22], axial component position was assessed for 52 hips, with at least three radiographic series, using einzel-bild-roentgen-analyze (EBRA), and on true lateral radiographs using the Woo and Morrey method and the ischiolateral method. The mean SDs of the ischiolateral (2.15°) and EBRA (2.06°) methods were lower than that of the Woo and Morrey method (3.65°) but were not different from one another. We conducted all measurements on X-rays, considering the cost and radiation exposure associated with CT scans. LCEA was not normally distributed in the three subgroups of the anteversion achieved category in our study. The mean LCEA was highest in the anteversion achieved category 5°–25° (51.23°), followed by category <5° (49.3°), followed by category >25° (44.7°). It can be inferred that the value of LCEA is maximum in the Lewinneck’s safe zone of anteversion of the acetabular cup, that is, between 5° and 25°, and it decreases with any acetabular cup orientation lying outside these values. LCEA has been used as an important parameter to assess femoral head coverage in DDH. To the best of our knowledge, no prior studies have been done to use LCEA as a measure of femoral head coverage in THA patients. Further studies are needed to assess the significance of LCEA in measuring the degree of femoral head coverage in THR patients.
Limitations of study
The present study has certain limitations. The sample size was relatively small, which may limit the generalizability of the findings. The duration of the study was shorter compared to previous research, and postoperative assessments were based on plain radiographs rather than CT scans, which could have provided more precise measurements of acetabular anteversion. In addition, the absence of a control group restricted comparative evaluation with standard acetabular positioning methods.
The Lewinneck’s safe zone for component positioning in THA has now been refuted by several studies, and the recommendations for component placement are now switching to a more patient-specific approach. The concept of functional cup orientation and KA-THR has come up in recent years and is still being explored. Spinal deformity and abnormal spinopelvic mobility lead to a change in functional anteversion which unless addressed intraoperatively, can cause malpositioning of acetabular components and subsequent dislocation. We conclude that the femoral head coverage as measured by LCEA is maximum when the acetabular cup is positioned in 5°–25° of anteversion. Since no prior studies have been done using LCEA as a measure of femoral head coverage in THR, further studies are needed to investigate the use of LCEA as a measure of the degree of femoral head coverage.
Pre-operative assessment of the spinopelvic relationship is crucial for optimizing acetabular component positioning in THA. Individualized adjustment of cup anteversion based on pelvic tilt can significantly enhance femoral head coverage, minimize the risk of impingement and dislocation, and improve overall implant stability and functional outcomes.
References
- 1. Delaunay C, Hamadouche M, Girard J, Duhamel A, SoFCOT Group. What are the causes for failures of primary hip arthroplasties in France? Clin Orthop Relat Res 2013;471:3863-9. [Google Scholar] [PubMed]
- 2. Hailer NP, Weiss RJ, Stark A, Kärrholm J. The risk of revision due to dislocation after total hip arthroplasty depends on surgical approach, femoral head size, sex, and primary diagnosis. An analysis of 78,098 operations in the Swedish Hip Arthroplasty Register. Acta Orthop 2012;83:442-8. [Google Scholar] [PubMed]
- 3. Mahoney CR, Pellicci PM. Complications in primary total hip arthroplasty: Avoidance and management of dislocations. Instr Course Lect 2003;52:247-55. [Google Scholar] [PubMed]
- 4. Sariali E, Lazennec JY, Khiami F, Catonné Y. Mathematical evaluation of jumping distance in total hip arthroplasty: Influence of abduction angle, femoral head offset, and head diameter. Acta Orthop 2009;80:277-82. [Google Scholar] [PubMed]
- 5. Miki H, Kyo T, Kuroda Y, Nakahara I, Sugano N. Risk of edge-loading and prosthesis impingement due to posterior pelvic tilting after total hip arthroplasty. Clin Biomech (Bristol) 2014;29:607-13. [Google Scholar] [PubMed]
- 6. Lewinnek GE, Lewis JL, Tarr R, Compere CL, Zimmerman JR. Dislocations after total hip-replacement arthroplasties. J Bone Joint Surg Am 1978;60:217-20. [Google Scholar] [PubMed]
- 7. Lazennec JY, Boyer P, Gorin M, Catonné Y, Rousseau MA. Acetabular anteversion with CT in supine, simulated standing, and sitting positions in a THA patient population. Clin Orthop Relat Res 2011;469:1103-9. [Google Scholar] [PubMed]
- 8. Kanawade V, Dorr LD, Wan Z. Predictability of acetabular component angular change with postural shift from standing to sitting position. J Bone Joint Surg Am 2014;96:978-86. [Google Scholar] [PubMed]
- 9. Barrack RL. Dislocation after total hip arthroplasty: Implant design and orientation. J Am Acad Orthop Surg 2003;11:89-99. [Google Scholar] [PubMed]
- 10. Wixson RL. Computer-assisted total hip navigation. Instr Course Lect 2008;57:707-20. [Google Scholar] [PubMed]
- 11. Esposito CI, Gladnick BP, Lee YY, Lyman S, Wright TM, Mayman DJ, et al. Cup position alone does not predict risk of dislocation after hip arthroplasty. J Arthroplasty 2015;30:109-13. [Google Scholar] [PubMed]
- 12. Lafage V, Schwab F, Patel A, Hawkinson N, Farcy JP. Pelvic tilt and truncal inclination: Two key radiographic parameters in the setting of adults with spinal deformity. Spine (Phila Pa 1976) 2009;34:E599-606. [Google Scholar] [PubMed]
- 13. Lembeck B, Mueller O, Reize P, Wuelker N. Pelvic tilt makes acetabular cup navigation inaccurate. Acta Orthop 2005;76:517-23. [Google Scholar] [PubMed]
- 14. Mellon SJ, Grammatopoulos G, Andersen MS, Pandit HG, Gill HS, Murray DW. Optimal acetabular component orientation estimated using edge-loading and impingement risk in patients with metal-on-metal hip resurfacing arthroplasty. J Biomech 2015;48:318-23. [Google Scholar] [PubMed]
- 15. McCarthy TF, Alipit V, Nevelos J, Elmallah RK, Mont MA. Acetabular cup anteversion and inclination in hip range of motion to impingement. J Arthroplasty 2016;31:264-8. [Google Scholar] [PubMed]
- 16. Laffargue P, Pinoit Y, Tabutin J, Giraud F, Puget J, Migaud H. Computer-assisted positioning of the acetabular cup for total hip arthroplasty based on joint kinematics without prior imaging: Preliminary results with computed tomographic assessment. Rev Chir Orthop Reparatrice Appar Mot 2006;92:316-25. [Google Scholar] [PubMed]
- 17. Clohisy JC, Carlisle JC, Beaulé PE, Kim YJ, Trousdale RT, Sierra RJ, et al. A systematic approach to the plain radiographic evaluation of the young adult hip. J Bone Joint Surg Am 2008;90 Suppl 4:47-66. [Google Scholar] [PubMed]
- 18. Woo RY, Morrey BF. Dislocations after total hip arthroplasty. J Bone Joint Surg Am 1982;64:1295-306. [Google Scholar] [PubMed]
- 19. Eilander W, Harris SJ, Henkus HE, Cobb JP, Hogervorst T. Functional acetabular component position with supine total hip replacement. Bone Joint J 2013;95-B:1326-31. [Google Scholar] [PubMed]
- 20. Abdel MP, von Roth P, Jennings MT, Hanssen AD, Pagnano MW. What safe zone? The vast majority of dislocated THAs are within the lewinnek safe zone for acetabular component position. Clin Orthop Relat Res 2016;474:386-91. [Google Scholar] [PubMed]
- 21. Inaba Y, Kobayashi N, Suzuki H, Ike H, Kubota S, Saito T. Preoperative planning for implant placement with consideration of pelvic tilt in total hip arthroplasty: Postoperative efficacy evaluation. BMC Musculoskelet Disord 2016;17:280. [Google Scholar] [PubMed]
- 22. Tiberi JV, Pulos N, Kertzner M, Schmalzried TP. A more reliable method to assess acetabular component position. Clin Orthop Relat Res 2012;470:471-6. [Google Scholar] [PubMed]