Extracorporeal shock wave therapy could be considered a promising non-invasive alternative for the management of ulnar shaft fracture delayed healing following surgical fixation, demonstrating consistently successful outcomes.
Dr. Grigorios Kastanis, Orthopaedic Consultant & Hand Surgeon. Department of Orthopaedics, General Hospital of Heraklion-Venizeleio, Heraklion, Crete, Greece. E-mail: kastanisg@gmail.com
Introduction: Isolated ulnar shaft fractures are uncommon injuries but are prone to developing delayed union. Delayed union of such fractures is a well-recognized complication, regardless of the type of treatment. The standard treatment for this complication initially involves observation, and if non-union develops, it is followed by internal fixation with a compression plate, combined with biological stimulation using an autologous iliac crest bone graft. Recently, extracorporeal shock wave therapy (ESWT) has been proposed as a non-operative alternative for the treatment of delayed union. The aim of the present study is to report the outcomes of ESWT in the treatment of ulnar shaft delayed union following initial surgical management with open reduction and internal fixation (ORIF) in a young patient. A brief review of the relevant literature is also presented on the topic.
Case Report: A 19-year-old patient with an isolated ulnar shaft fracture was surgically treated with ORIF. At 12 weeks postoperatively, the patient presented with clinical and radiographic signs of delayed union. ESWT was employed to manage the delayed bone healing. After 10 sessions, the patient was symptom-free, with radiographic evidence of fracture consolidation.
Conclusion: ESWT is considered a promising non-invasive alternative for the management of delayed fracture healing, demonstrating consistently successful outcomes. It has proven to be a safe, reliable, and highly effective modality, without the risks and complications typically associated with revision surgery.
Keywords: Ulnar shaft fracture, delayed union, extracorporeal shock wave therapy.
Isolated ulnar shaft fractures are uncommon injuries, typically resulting from a direct blow (38%), a simple fall (31%), or a pedestrian road traffic accident (14%) [1]. These fractures are considered high-energy injuries because the subcutaneous ulna absorbs the impact, and they are commonly referred to as “nightstick fractures” [2]. The incidence of these injuries demonstrates a bimodal distribution according to age and sex: in males, it is highest among younger individuals due to violent activities, whereas in females, it increases gradually in the earlier decades and more sharply in older age, reflecting underlying osteoporosis [1]. Unstable fractures are typically defined by one or more of the following criteria: angulation >10°, contact surface <50%, shortening of 3 mm or more, and/or the presence of associated instability at the proximal or distal radioulnar joint [3,4]. Open reduction and internal fixation (ORIF) using a dynamic compression plate or locking plate is generally regarded as the gold standard for treating unstable ulnar shaft fractures, particularly when the fracture cannot be adequately reduced or stabilized by closed means [4,5]. Delayed union is a recognized complication of these fractures, regardless of the treatment method used (conservative or surgical) [4,6]. In general, bone healing is considered delayed between 3 and 6 months postoperatively, depending on the specific case [7]. Various techniques (conservative or surgical) are employed in the treatment of delayed union, with approximately 80% of patients achieving good to excellent final restoration of mechanical axis alignment and proper limb length through surgical treatment if non-union ultimately develops [6]. Extracorporeal shock wave therapy (ESWT) has recently been used as a form of external bone stimulation in cases of delayed healing. This technique supports the theory that microfractures induced by shock waves can stimulate the bone repair process [7,8]. The aim of this study is to present the results of ESWT in a young patient for the treatment of delayed union following surgical fixation (ORIF) for an unstable isolated ulnar shaft fracture.
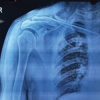
A 19-year-old right-hand dominant patient presented to the emergency department of our hospital following a road traffic accident with right forearm pain and tenderness, without skin deformities apart from swelling, and no vascular or neurological deficits. No associated injuries were identified in other organ systems. On clinical examination, the patient was unable to pronate or supinate the forearm but could fully extend and flex the elbow; hand flexion and extension were limited. Radiographic examination revealed a transverse ulnar shaft fracture (2U2A3 according to AO/OTA classification) (Fig. 1a and b). Initial closed reduction was unsuccessful, and the patient subsequently underwent surgical fixation 4 days later. Under the Wide-Awake Local Anesthesia No Tourniquet technique, the fracture was surgically fixed using ORIF with a compression plate and six cortical screws (Fig. 1c and d).

Figure 1: Anteroposterior (a) and lateral (b) pre-operative X-rays of an isolated ulnar fracture. Anteroposterior (c) and lateral (d) post-operative X-rays showing surgical stabilization with a 6-hole compression plate.
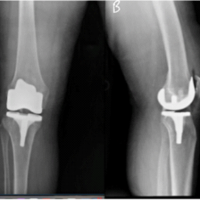
At 2 weeks postoperatively, the stitches were removed, and the wound had healed normally without any signs of infection. At the 12-week follow-up, the patient reported pain and tenderness at the surgical site during pronation, supination, and weight lifting. Radiographic examination revealed signs of delayed union, while laboratory blood tests – including C-reactive protein and erythrocyte sedimentation rate – were within normal limits (Fig. 2). ESWT sessions were recommended as a conservative alternative before considering further surgical intervention.

Figure 2: Anteroposterior (a) and lateral (b) X-rays demonstrate delayed union of the ulnar fracture at 12 weeks postoperatively.
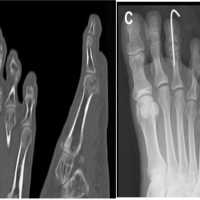
Four sessions of focused extracorporeal shock wave therapy (F-SW) were administered at 7-day intervals without the use of any form of anesthesia, using the Duolith SD1 T-TOP device. This was followed by two additional sessions at 10-day intervals. Each session consisted of 4000 impulses delivered at a frequency of 4 Hz, with an energy flux density ranging from a minimum of 0.03 mJ/mm² to a maximum of 0.55 ± 0.03 mJ/mm², applied to both the palmar and dorsal aspects of the patient’s forearm. An F-SW generator with a level 1 stand-off (10 cm penetration depth; focal zone 1.5–4.5 cm) was used. Coupling gel was applied to minimize energy loss during transmission. No complications related to the shock wave therapy were observed. Radiographic examinations were performed at 5 time points during the treatment sessions. Early signs of bone consolidation were observed, and by the end of the protocol, radiographs demonstrated clear evidence of bone healing (Fig. 3). During follow-up evaluations at 6 and 12 months, the patient exhibited full pronation and supination, was able to fully bear weight without pain, and had returned to normal daily activities and work. At the final follow-up at 12 months, the patient’s DASH score was 10/100.

Figure 3: Anteroposterior (a) and lateral (b) X-rays illustrate evidence of fracture healing following 10 sessions of extracorporeal shock wave therapy.
Delayed union of the ulna shaft is a major complication of forearm fractures, with an incidence ranging from 10% to 30% [2,4,6]. Coulibaly et al. (2015) mention that, while commonly called the stationary bone of the forearm, the ulna is the most susceptible to fracture, delayed union, or non-union [6]. Tseng et al. (2025) noted that diaphyseal delayed union or non-union of forearm bones must be differentiated from diaphyseal non-union of lower limb fractures because the primary mechanical constraints involve rotation and distraction rather than compression [5]. The main goal of treating delayed union of forearm bones is to achieve complete fracture union and restore the functional anatomy between the radius and the ulna, thereby ensuring normal hand function [1]. The treatment of forearm delayed union remains a matter of debate. Several surgical techniques, such as internal fixation with plates, intramedullary nailing, and external fixation combined with corticocancellous iliac bone grafting, have been recommended, achieving a success rate of approximately 80% and remaining the gold standard for non-union treatment [7]. Among conservative options, ESWT has emerged as a reliable and effective non-invasive modality for treating non-union; however, there is no clear evidence supporting its use in cases of delayed union [7]. Mittermayr et al. (2021) were the first to describe ESWT, supporting the theory that it causes microfractures which subsequently induce repair processes [8]. Tischer et al. verified bone formation histologically in bone samples treated with shockwaves, whereas Schaden et al. confirmed this observation clinically [9,10]. Wang et al. reported that shockwaves promote mesenchymal stem cell (MSC) growth and differentiation toward osteoprogenitors through induction of transforming growth factor-beta 1 and vascular endothelial growth factor [11]. Sun et al. noted that ESWT induces adenosine triphosphate release and promotes MSC osteogenic differentiation via P2X7 receptors [7]. Furthermore, adequate vascularity is essential for stem cell migration, and shockwaves have been shown to effectively foster neovascularization and bone repair [8]. Numerous clinical studies have demonstrated the effectiveness of ESWT in the treatment of delayed union or non-union, with success rates ranging from 41% to 91% [11,12]. Rompe et al. (2001) reported successful treatment in 72% of 43 patients with diaphyseal non-union of the tibia and femur, 9 months post-surgery [13]. Xu et al. (2009) reported a success rate of 75.4%, especially in hypertrophic non-union [14]. Similar results were reported by Cacchio et al. (2009), who compared ESWT with surgical treatment of non-union and found significantly better outcomes in the ESWT groups at both 3- and 6-month post-treatment compared to revision surgery [12]. Finally, Sansone et al., in a systematic review and meta-analysis of long bone fracture non-union treated with ESWT, concluded that the success rate depends on the anatomical location, the nature of the non-union, and the elapsed time from injury to treatment [7]. Regarding the type of non-union, hypertrophic non-union had a better chance of healing with ESWT than atrophic or oligotrophic non-union. Concerning anatomical location, the highest healing rates were observed in the metatarsals (90%), followed by the tibia (75.54%), the femur (66.91%), and, less frequently, the humerus (63.64%) [7]. A critical factor is the time from non-union diagnosis to the start of ESWT; higher success rates are seen when treatment is initiated closer to the time of injury rather than later [7]. In our case, we diagnosed delayed union 12 weeks post-surgery and initiated ESWT shortly thereafter. We believe that the timing of ESWT initiation is a key factor in achieving favorable outcomes.
ESWT for delayed fractures is a non-invasive alternative approach with successful outcomes. Overall, it has proven to be a reliable, safe, and highly effective treatment without the complications associated with revision surgery. Clinical studies with larger patient samples in the future would be highly valuable to obtain more robust results regarding the use of ESWT.
ESWT could be considered a promising non-invasive alternative for the management of ulnar shaft fracture delayed healing following surgical fixation, demonstrating consistently successful outcomes.
References
- 1. Handoll HH, Pearce P. Interventions for treating isolated diaphyseal fractures of the ulna in adults. Cochrane Database Syst Rev 2012;2012:CD000523. [Google Scholar] [PubMed]
- 2. Sauder DJ, Athwal GS. Management of isolated ulnar shaft fractures. Hand Clin 2007;23:179-84. [Google Scholar] [PubMed]
- 3. Freeland AE, Kregor PJ. Treatment of isolated fractures of the ulnar shaft. Orthopedics 1997;20:1081-2. [Google Scholar] [PubMed]
- 4. Dagtas MZ, Unal OK. Using autograft in the surgical treatment of isolated distal ulna fractures with open reduction internal fixation improves short-term clinical outcomes: 11 years of experience. Orthop Traumatol Surg Res 2021;107:103082. [Google Scholar] [PubMed]
- 5. Tseng TH, Hung CC, Yen HK, Chen HM, Wang CY, Tzeng SC, et al. Higher nonunion rates with locking plates compared to dynamic compression plates in forearm diaphyseal fractures: A multicenter study. J Orthop Traumatol 2025;26:10. [Google Scholar] [PubMed]
- 6. Coulibaly MO, Jones CB, Sietsema DL, Schildhauer TA. Results of 70 consecutive ulnar nightstick fractures. Injury 2015;46:1359-66. [Google Scholar] [PubMed]
- 7. Sansone V, Ravier D, Pascale V, Applefield R, Del Fabbro M, Martinelli N. Extracorporeal shockwave therapy in the treatment of nonunion in long bones: A systematic review and meta-analysis. J Clin Med 2022;11:1977. [Google Scholar] [PubMed]
- 8. Mittermayr R, Haffner N, Feichtinger X, Schaden W. The role of shockwaves in the enhancement of bone repair-from basic principles to the clinical application. Injury 2021;52 Suppl 2:S84-90. [Google Scholar] [PubMed]
- 9. Schaden W, Fischer A, Sailler A. Extracorporeal shock wave therapy of nonunion or delayed osseous union. Clin Orthop Relat Res. 2001 Jun;(387):90-4. doi: 10.1097/00003086-200106000-00012. [Google Scholar] [PubMed] [CrossRef]
- 10. Tischer T, Milz S, Weiler C, Pautke C, Hausdorf J, Schmitz C, Maier M. Dose-dependent new bone formation by extracorporeal shock wave application on the intact femur of rabbits. Eur Surg Res. 2008;41(1):44-53. doi: 10.1159/000128279. [Google Scholar] [PubMed] [CrossRef]
- 11. Wang FS, Yang KD, Chen RF, Wang CJ, Sheen-Chen SM. Extracorporeal shock wave promotes growth and differentiation of bone-marrow stromal cells towards osteoprogenitors associated with induction of TGF-beta1. J Bone Joint Surg Br 2002;84:457-61. [Google Scholar] [PubMed]
- 12. Cacchio A, Giordano L, Colafarina O, Rompe JD, Tavernese E, Ioppolo F, et al. Extracorporeal shock-wave therapy compared with surgery for hypertrophic long-bone nonunions. J Bone Joint Surg Am 2009;91:2589-97. [Google Scholar] [PubMed]
- 13. Rompe J.D., Rosendahl T., Schöllner C., Theis C. High-energy extracorporeal shock wave treatment of nonunions. Clin. Orthop. Relat. Res. 2001;387:102–111. doi: 10.1097/00003086-200106000-00014. [Google Scholar] [PubMed] [CrossRef]
- 14. Xu Z.H., Jiang Q., Chen D.Y., Xiong J., Shi D.Q., Yuan T., Zhu X.L. Extracorporeal shock wave treatment in non-unions of long bone fractures. Int. Orthop. 2009;33:789–793. doi: 10.1007/s00264-008-0553-8. [Google Scholar] [PubMed] [CrossRef]