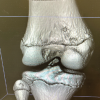
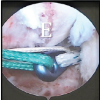
With a low risk of complications, arthroscopic treatment of carefully chosen meniscal tears results in notable short-term improvements in knee function, symptom relief, and activity levels.
Dr. Anil Vaishnav, Department of Orthopaedics, Government Medical College, Datia, Madhya Pradesh, India. E-mail: anil43854@gmail.com
Introduction: Among young, physically active people, meniscal injuries are one of the most frequent causes of knee dysfunction. Due to its minimally invasive nature and potential for early functional recovery, arthroscopic management has emerged as the preferred treatment strategy for symptomatic meniscal tears. This study used validated knee-specific scoring systems to assess short-term functional outcomes after arthroscopic treatment of meniscal tears.
Material and Methods: 123 patients between the ages of 18 and 50 who had meniscal tears that were clinically and radiologically confirmed and underwent arthroscopic treatment were included in a prospective observational study. Patients were treated with either meniscal repair or arthroscopic partial meniscectomy based on intraoperative findings. The Tegner Activity Scale, International Knee Documentation Committee (IKDC) subjective score, and Lysholm Knee Score were used to evaluate functional outcomes both before and 6 months after surgery. In addition, recorded were post-operative complications and the return to pre-injury activity levels.
Results: The study population was predominately male, with a mean age of 32.8 ± 7.6 years. Longitudinal tear patterns were most commonly seen, and medial meniscal tears were more common than lateral tears. 68.3% of patients had an arthroscopic partial meniscectomy, and 31.7% had meniscal repair. At the 6 months follow-up, all functional outcome measures showed significant improvement. The IKDC subjective score rose from 48.7 ± 10.5 to 86.2 ± 7.1, and the mean Lysholm Knee Score improved from 54.3 ± 9.8 pre-operatively to 89.6 ± 6.4 post-operatively. The score on the Tegner Activity Scale increased from 3.1 ± 1.2 to 6.2 ± 1.4 (P < 0.001). 91.1% of patients recovered without incident, and 79.7% resumed their pre-injury level of activity.
Conclusion: Arthroscopic treatment of meniscal tears promotes an early return to activity in the short term and offers notable functional improvement with low rates of complications.
Keywords: Meniscal tear, arthroscopy, partial meniscectomy, meniscal repair, functional outcome.
The knee menisci are fibrocartilaginous structures that are crucial for joint congruity, stability, load transmission, and shock absorption. Because of their role in normal biomechanics, modern management has shifted toward tissue preservation whenever possible [1,2]. The meniscus’s unique vascular pattern, which is commonly referred to as peripheral (red-red), intermediate (red-white), and central (white-white) regions, supports this biological explanation because vascularity and nutrition affect healing potential and, in turn, the appropriateness of repair versus resection [2]. Simultaneously, it is becoming more widely acknowledged that tear morphology and patient-related factors (such as age, activity demands, degenerative changes, and concurrent chondral pathology) influence recovery and prognosis [1,3]. Arthroscopic intervention for meniscal pathology is still one of the most common knee procedures performed globally, despite this emphasis on preservation [4]. Meniscal tears can occur in a wide range of conditions, from degenerative tears in middle-aged and older adults to acute traumatic lesions in younger, active people. They frequently coexist with cartilage damage, which may affect the functional trajectory and post-operative symptoms [4]. As a result, modern decision-making necessitates striking a balance between longer-term joint health concerns and immediate symptom relief and return to function [1,3]. The role of surgery has been improved by recent high-quality evidence, especially for degenerative meniscal tears. Exercise-based physical therapy showed non-inferiority to arthroscopic partial meniscectomy at 5-years follow-up for patient-reported knee function in the ESCAPE randomized clinical trial, supporting structured rehabilitation as a preferred initial strategy in many patients with degenerative tears [5]. Similarly, early arthroscopic partial meniscectomy was not better than a strategy of physical therapy with optional delayed surgery at 24 months in younger adults with magnetic resonance imaging (MRI)-confirmed isolated traumatic tears [6]. This suggests that in certain cases, non-operative pathways can lead to symptomatic improvement. The need for customized, tear-specific arthroscopic strategies rather than age-driven algorithms alone is highlighted by systematic evidence that meniscal repair can result in favorable patient-reported outcomes in appropriately selected patients, including those aged ≥40 years [3]. To describe functional recovery in practical practice, institution-level outcome data are still crucial due to the variability of tear patterns, surgical methods (repair versus partial meniscectomy), and rehabilitation pathways. Therefore, this study assesses functional recovery following arthroscopic treatment of meniscal tears by applying validated patient-reported and activity-based outcome measures across the follow-up period, while also examining factors linked to post-operative functional gains.
Study design and setting
This prospective observational study was carried out in the Department of Orthopaedics of a tertiary care teaching hospital. It was undertaken to assess functional recovery following arthroscopic treatment for meniscal injuries of the knee.
Ethical considerations
Ethical clearance was obtained from the institutional Human Ethics Committee (Ref. No. 151/IEC/GMC/2025; January 25, 2025). Written informed consent was documented from all participants, ensuring confidentiality throughout the study. All procedures were conducted in accordance with the Declaration of Helsinki.
Study population and sample size
The study included 123 consecutive patients with symptomatic meniscal tears who were planned for arthroscopic management. The sample size was based on feasibility and aligned with similar single-center clinical outcome studies in arthroscopic knee surgery. Participants were enrolled using a non-probability consecutive sampling technique.
Inclusion and exclusion criteria
Patients between 18 and 50 years of age with clinical and radiological evidence of meniscal injury were eligible for inclusion. The diagnosis was confirmed using MRI in all cases. Both isolated medial or lateral meniscal tears and tears occurring in otherwise stable knees were included. Patients were excluded if they had associated anterior or posterior cruciate ligament ruptures requiring reconstruction, advanced knee osteoarthritis (Kellgren–Lawrence grade ≥3), inflammatory joint disorders, a history of prior surgery on the affected knee, fractures around the knee joint, or systemic conditions that could adversely affect post-operative rehabilitation.
Pre-operative assessment
Baseline demographic and clinical details, including age, sex, body mass index, side involved, mechanism of injury, and duration of symptoms, were documented. A standardized clinical evaluation was performed for all patients, comprising assessment of joint line tenderness, McMurray test, and knee range of motion. Pre-operative functional status was assessed using the Lysholm Knee Scoring Scale, the International Knee Documentation Committee (IKDC) subjective knee evaluation form, and the Tegner Activity Scale.
Surgical technique
All surgeries were performed arthroscopically under spinal or general anesthesia with the patient positioned supine and a pneumatic tourniquet applied to the thigh. Standard anterolateral and anteromedial portals were utilized for diagnostic arthroscopy. Intraoperatively, the type, location, and configuration of the meniscal tear were recorded. Based on tear characteristics and tissue quality, patients underwent either arthroscopic partial meniscectomy or meniscal repair using inside-out or all-inside techniques. Maximum preservation of viable meniscal tissue was prioritized whenever feasible.
Post-operative rehabilitation protocol
All patients followed a standardized rehabilitation program. Quadriceps activation and range-of-motion exercises were initiated within the 1st post-operative week. Patients who underwent partial meniscectomy were allowed weight-bearing as tolerated, while those who had meniscal repair followed a protected weight-bearing regimen. Gradual progression to strengthening exercises and functional training was supervised by a physiotherapist. Return to sports or high-impact activities were permitted after satisfactory functional recovery, typically between 3 and 6 months, depending on the surgical procedure.
Follow-up and outcome measures
Patients were evaluated at 6 weeks, 3 months, and 6 months after surgery. At each follow-up, functional outcomes were measured using the Lysholm Knee Score, IKDC subjective score, and Tegner Activity Scale. Changes in knee function, activity level, and patient-reported symptoms were recorded and compared with baseline values. Post-operative complications, including infection, persistent pain, stiffness, or re-injury, were also noted.
Statistical analysis
Data were compiled in a spreadsheet and analyzed using standard statistical software. Continuous variables were summarized as mean and standard deviation, while categorical variables were expressed as frequencies and percentages. Pre- and post-operative functional scores were compared using paired statistical tests. A P < 0.05 was considered statistically significant.
A total of 123 patients who received arthroscopic treatment for meniscal tears were included in the final analysis. The average age of the group was 32.8 ± 7.6 years. Males made up the majority, with a male-to-female ratio of 1.7:1. There were slightly more cases of injuries to the right knee than the left. The leading cause of injury was sports-related trauma, followed by twisting incidents during everyday activities and road traffic accidents. The average duration of symptoms before surgery was 5.4 ± 2.1 months (Table 1). Intraoperative findings showed that medial meniscal tears were more common than lateral tears, making up nearly two-thirds of cases. Longitudinal tears were the most frequent type, followed by complex and horizontal tears. Most tears were found in the red–white vascular zone, while those confined to the white–white zone occurred least often (Table 2).
Arthroscopic partial meniscectomy was the most common procedure, making up more than two-thirds of the surgeries. Meniscal repair was performed in about one-third of patients, with the all-inside technique preferred over the inside-out approach for repairs (Table 3).
Evaluating functional outcomes showed significant improvements across all scoring systems at the 6 months follow-up compared to baseline values. The mean Lysholm Knee Score increased from 54.3 ± 9.8 before surgery to 89.6 ± 6.4 after surgery. Similarly, the IKDC subjective score rose significantly from 48.7 ± 10.5 before surgery to 86.2 ± 7.1 at the final follow-up. There was also a notable increase in Tegner Activity Scale scores, indicating higher activity levels after surgery. All improvements were statistically significant (P < 0.001) (Table 4).
Most patients had an uncomplicated recovery after surgery. Minor complications were reported in a few cases, with persistent knee pain and temporary stiffness being the most common. Two patients experienced superficial portal-site infections, both of which resolved with conservative treatment. No reoperations were needed during the follow-up period. By the end of 6 months, nearly eighty percent of patients had returned to their pre-injury level of activity (Table 5).
This prospective cohort study examined short-term functional recovery following arthroscopic treatment of meniscal tears and demonstrated clinically meaningful improvements in knee-specific function and activity levels by 6 months (Table 4), together with a high proportion of patients returning to their pre-injury activity status (Table 5). The observed recovery pattern aligns with pooled evidence indicating that patient-reported benefits after arthroscopic partial meniscectomy typically occur early, with most subjective improvement achieved within the first 3 months and minimal additional clinically relevant change thereafter [7]. In the present cohort, the greatest absolute improvements in Lysholm and IKDC scores were already apparent at 6 weeks and were maintained through the 6 months follow-up (Table 4), supporting the notion that early symptom relief and functional restoration are key drivers of short-term recovery after arthroscopic intervention. The rate of return to activity observed in this series (Table 5) is also consistent with contemporary rehabilitation principles that emphasize criterion-based progression rather than rigid, time-dependent milestones after meniscectomy. Readiness for activity advancement is guided by factors, such as resolution of effusion, restoration of range of motion, quadriceps strength, and neuromuscular control [8]. Although recommended timelines for return to walking, work, or sport vary across protocols, there is broad agreement that symptom resolution and objective functional criteria should dictate progression. The pattern of improvement seen in patient-reported outcome measures (PROMs) and Tegner activity levels in this study (Table 4) fits well within this framework, indicating that substantial functional recovery by 6 months is achievable in a considerable proportion of appropriately selected patients [8]. Safety outcomes in the current cohort (Table 5) compare favorably with large population-based data. A national analysis encompassing nearly 700,000 arthroscopic partial meniscectomies reported a very low absolute risk of serious complications within 90 days (0.317%), with pulmonary embolism and infections requiring surgical intervention being rare but clinically relevant events [9]. In the present study, post-operative complications were predominantly minor and self-limiting (Table 5), and no cases of deep infection, venous thromboembolism, or reoperation were observed during the 6 months follow-up. Nevertheless, the relatively small sample size and limited follow-up duration restrict conclusions regarding rare adverse outcomes. An important clinical consideration relates to the longer-term consequences of procedure selection. Meniscal preservation is increasingly advocated when repair is feasible, due to concerns regarding the risk of subsequent osteoarthritis following meniscal resection. A recent systematic review focusing on posterior medial meniscus injuries reported higher rates of osteoarthritis after meniscectomy compared with meniscal repair, supporting the biological rationale for tissue preservation [10]. Consistent with this, real-world evidence from a large claims-database study demonstrated a higher incidence of knee osteoarthritis within 5 years following isolated arthroscopic partial meniscectomy compared with isolated meniscal repair (13.5% vs. 10.7%), highlighting the potential long-term trade-offs associated with meniscal resection. Although the present study was limited to 6 months outcomes and therefore cannot address osteoarthritis progression, the distribution of surgical procedures performed (Table 3) should be interpreted in the context of evolving indications that increasingly prioritize repair in suitable tear patterns and patient profiles [11]. The findings should also be considered alongside the evidence base for degenerative meniscal tears. An economic evaluation using data from the placebo-controlled FIDELITY trial concluded that arthroscopic partial meniscectomy was not cost-effective compared with placebo surgery for degenerative medial meniscal tears, reflecting a broader body of literature questioning routine arthroscopy in degenerative disease without clear mechanical symptoms [12]. In the present cohort, patient selection and tear characteristics (Tables 1 and 2) likely contributed to the favorable short-term outcomes; however, further subgroup analyses based on traumatic versus degenerative etiology and cartilage status would be valuable to better align outcomes with current evidence-based indications. For patients undergoing meniscal repair, technique-specific considerations are important when counseling regarding recovery expectations and risk. A systematic review comparing all-inside and inside-out repair techniques for bucket-handle tears reported post-operative improvements in Lysholm and Tegner scores with both approaches, but with wide variability in failure rates and notable stiffness-related complications [13]. Another systematic review found comparable PROMs between all-inside and inside-out repairs, with all-inside techniques associated with higher re-injury rates but a greater likelihood of return to pre-injury levels of play [14]. Return-to-sport–focused analyses of all-inside repairs have reported return-to-sport rates of approximately 90%, accompanied by improvements in activity scores at follow-up [15]. Although the repair subgroup in the present study was relatively small (Table 3), the overall return-to-activity outcomes (Table 5) are consistent with these broader findings and underscore the importance of balancing early return with reinjury risk during shared decision-making. Several limitations should be acknowledged. The follow-up period was limited to 6 months and therefore does not capture long-term durability, late re-tear rates, or osteoarthritis development. The absence of a non-operative comparison group precludes definitive attribution of observed improvements to surgical intervention, particularly in subgroups with predominantly degenerative pathology. In addition, while validated PROMs were employed (Table 4), the incorporation of objective strength and functional performance testing in line with consensus recommendations could enhance future studies [8]. Despite these limitations, the prospective design, use of standardized outcome measures, and consistent improvements across multiple domains provide pragmatic short-term benchmarks for functional recovery following arthroscopic management of meniscal tears.
Arthroscopic treatment of meniscal tears led to significant functional improvement and favorable short-term clinical outcomes in most patients in this study. Consistent and substantial improvements were observed across all validated functional outcome measures, indicating meaningful recovery of knee function, reduction in symptoms, and enhancement of activity levels by 6 months after surgery. The low complication rate and the high proportion of patients returning to their pre-injury level of activity further support the safety and effectiveness of arthroscopic management when appropriate surgical techniques are combined with a structured rehabilitation program. Overall, these findings reinforce the role of arthroscopy as a dependable treatment option for symptomatic meniscal injuries, enabling early functional recovery and restoration of knee stability in an active patient population.
Management of meniscal tears should follow an individualized, evidence-informed strategy that considers tear morphology, patient activity requirements, and healing potential. When indicated, arthroscopic intervention can achieve rapid short-term functional recovery and support a timely return to pre-injury activity levels. Whenever possible, preservation of viable meniscal tissue should be emphasized to promote long-term joint health. Adherence to a structured, criterion-based rehabilitation protocol is crucial for optimizing post-operative outcomes.
References
- 1. Simonetta R, Russo A, Palco M, Costa GG, Mariani PP. Meniscus tears treatment: The good, the bad and the ugly-patterns classification and practical guide. World J Orthop 2023;14:171-85. [Google Scholar] [PubMed]
- 2. Pasiński M, Zabrzyńska M, Adamczyk M, Sokołowski M, Głos T, Ziejka M, et al. A current insight into human knee menisci. Transl Res Anat 2023;32:100259. [Google Scholar] [PubMed]
- 3. Sedgwick MJ, Saunders C, Getgood AM. Systematic review and meta-analysis of clinical outcomes following meniscus repair in patients 40 years and older. Orthop J Sports Med 2024;12:23259671241258974. [Google Scholar] [PubMed]
- 4. Valderrama J, Carredano X, León A, Vigueras C, Marín F, Acevedo M, et al. Prevalence of articular surface injuries in patients undergoing meniscal surgery: A retrospective analysis of 758 cases. Cureus 2024;16:e66789. [Google Scholar] [PubMed]
- 5. Noorduyn JC, Van De Graaf VA, Willigenburg NW, Scholten-Peeters GG, Kret EJ, Van Dijk RA, et al. Effect of physical therapy vs arthroscopic partial meniscectomy in people with degenerative meniscal tears: Five-year follow-up of the ESCAPE randomized clinical trial. JAMA Netw Open 2022;5:e2220394. [Google Scholar] [PubMed]
- 6. Van Der Graaff SJ, Eijgenraam SM, Meuffels DE, Van Es EM, Verhaar JA, Hofstee DJ, et al. Arthroscopic partial meniscectomy versus physical therapy for traumatic meniscal tears in a young study population: A randomised controlled trial. Br J Sports Med 2022;56:870-6. [Google Scholar] [PubMed]
- 7. Castle JP, Khalil LS, Abbas MJ, DeBolle S, Tandron M, Cross AG, et al. Maximum subjective outcome improvement is reported by 3 months following arthroscopic partial meniscectomy: A systematic review. J Orthop 2022;31:78-85. [Google Scholar] [PubMed]
- 8. Pujol N, Giordano AO, Wong SE, Beaufils P, Monllau JC, Arhos EK, et al. The formal EU-US meniscus rehabilitation 2024 consensus: An ESSKA-AOSSM-AASPT initiative. Part I-Rehabilitation management after meniscus surgery (meniscectomy, repair and reconstruction). Knee Surg Sports Traumatol Arthrosc 2025;33:3002-13. [Google Scholar] [PubMed]
- 9. Abram SG, Judge A, Beard DJ, Price AJ. Adverse outcomes after arthroscopic partial meniscectomy: A study of 700 000 procedures in the national hospital episode statistics database for England. Lancet 2018;392:2194-202. [Google Scholar] [PubMed]
- 10. Hurmuz M, Ionac M, Hogea B, Miu CA, Tatu F. Osteoarthritis development following meniscectomy vs. Meniscal repair for posterior medial meniscus injuries: A systematic review. Medicina (Kaunas) 2024;60:569. [Google Scholar] [PubMed]
- 11. Skinner M, Sullivan B, Conley C, Johnson D, Ireland ML, Landy D, et al. Incidence of osteoarthritis diagnosis within 5 years of surgery was greater following partial meniscectomy than meniscus repair and/or anterior cruciate ligament reconstruction. Arthrosc Sports Med Rehabil 2024;6:100903. [Google Scholar] [PubMed]
- 12. Kalske R, Kiadaliri A, Sihvonen R, Englund M, Turkiewicz A, Paavola M, et al. Arthroscopic partial meniscectomy for a degenerative meniscus tear is not cost effective compared with placebo surgery: An economic evaluation based on the FIDELITY trial data. Clin Orthop Relat Res 2024;482:1523-33. [Google Scholar] [PubMed]
- 13. Dzidzishvili L, Berreta RS, Jackson GR, Mowers CC, Cotter EJ, Allahabadi S, et al. All-inside and inside-out repair techniques for bucket-handle meniscus tears both result in improved patient outcomes and a broad range of failure rates: A systematic review. Arthroscopy 2024;40:2477-90.e1. [Google Scholar] [PubMed]
- 14. Migliorini F, Asparago G, Oliva F, Bell A, Hildebrand F, Maffulli N. Greater rate of return to play and re-injury following all-inside meniscal repair compared to the inside-out technique: A systematic review. Arch Orthop Trauma Surg 2023;143:6273-82. [Google Scholar] [PubMed]
- 15. Totlis T, Haunschild ED, Otountzidis N, Stamou K, Condron NB, Cole BJ, et al. Return-to-sport rate and activity level are high following arthroscopic all-inside meniscal repair with and without concomitant anterior cruciate ligament reconstruction: A systematic review. Arthroscopy 2021;37:2351-60. [Google Scholar] [PubMed]