Vigilance for unusual pathogens is essential, as early cytological diagnosis and tailored antifungal therapy are key to successful management of rare musculoskeletal fungal infections in immunocompromised patients.
Dr. Arjit Bansal, Department of Orthopaedics, Postgraduate Institute of Medical Education and Research, Chandigarh, Sector 12, Chandigarh - 160012, India. E-mail: arjitbansal28@gmail.com
Introduction: Fungal musculoskeletal infections are rare and often present diagnostic and therapeutic challenges, particularly in immunocompromised individuals. Phaeohyphomycosis is a dematiaceous fungal infection with a wide clinical spectrum, but isolated prepatellar bursitis due to this organism has not been previously reported. This case highlights the importance of maintaining a high index of suspicion for unusual pathogens in transplant recipients presenting with atypical joint or periarticular infections.
Case Report: We report the case of a 50-year-old female renal transplant recipient on long-term immunosuppressive therapy who presented with progressive swelling and pain over the anterior aspect of the knee. Clinical examination revealed localized swelling consistent with prepatellar bursitis, with no systemic features of infection. Initial aspiration yielded dark-colored fluid, and microscopy demonstrated pigmented fungal elements. Fungal culture confirmed the diagnosis of phaeohyphomycosis. The patient underwent surgical bursectomy followed by antifungal therapy, with gradual resolution of symptoms. At the latest follow-up, she remained asymptomatic with no evidence of recurrence.
Conclusion: This case underlines the need for early recognition of unusual infectious agents in immunosuppressed patients with persistent musculoskeletal complaints. Isolated fungal bursitis due to phaeohyphomycosis is extremely uncommon, and timely surgical intervention combined with appropriate antifungal therapy is critical for favorable outcomes. Orthopedic surgeons should be aware of this rare entity, as prompt diagnosis and multidisciplinary management can prevent morbidity and preserve function.
Keywords: Phaeohyphomycosis, prepatellar bursitis, renal transplant, fungal infection, immunosuppression.
Renal transplantation is considered the treatment of choice for end-stage renal disease. The number of renal transplants has increased rapidly over the years, with a mean incidence of approximately 14 per million population [1]. The survival of the graft has also increased with the advent of immunosuppressive therapy. However, long-term immunosuppression makes the recipient population susceptible to infections, particularly fungal infections. The incidence of invasive fungal infections in kidney transplant patients varies between 5 and 10% of all cases [2]. The most common causative agents are the Candida species and the Cryptococcus species in the yeast group, while the most common filamentous fungi are the Aspergillus species [2]. While these infections most commonly affect the lungs, bloodstream, and central nervous system, musculoskeletal system involvement is relatively uncommon in renal transplant recipients. Since the symptoms of fungal infections are non-specific and are insidious in onset, timely identification and early treatment initiation are of paramount importance in improving survival and reducing mortality. Prepatellar bursitis is usually bacterial in origin, and fungal etiology is reported rarely in immunocompromised hosts only [3]. We report a case of a 50-year-old female with progressive knee pain and swelling due to phaeohyphomycosis post-renal transplant while on immunosuppressive therapy, highlighting the unique scenario, importance of timely recognition, microbiological confirmation, initiation of early anti-fungal treatment with the involvement of a multidisciplinary team, with a favorable outcome at 6 months follow-up.
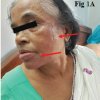
A 50-year-old female, resident of Himachal Pradesh, India, presented to the orthopedics outpatient department with complaints of persistent pain and swelling in the right knee for the past 6 months (Fig. 1).

Figure 1: Clinical photograph showing swelling over the anterior aspect of the right knee, predominantly in the prepatellar region, consistent with bursitis. The swelling was soft and mildly tender.
The swelling was insidious in onset and gradually progressive, associated with dull aching pain that worsened with movement and weight-bearing and was partially relieved with rest.
She had a past medical history of end-stage renal disease due to chronic glomerulonephritis (hepatitis C virus-related) and had undergone deceased donor renal transplantation around 10 years back. Post-transplant, she was on long-term immunosuppression with mycophenolate mofetil (MMF) and cyclosporine, along with valganciclovir prophylaxis. There was no recent history of trauma, fever, weight loss, or constitutional symptoms.
Clinical examination
On physical examination, a diffuse swelling was noted over the anterior aspect of the right knee, predominantly in the prepatellar region. The swelling was soft, mildly tender, non-fluctuant, and not adherent to the overlying skin or underlying structures. There were no signs of inflammation, ulceration, or discharge. Knee joint range of motion was slightly restricted due to discomfort and pain beyond 90° of flexion. There was no neurovascular deficit distally.
Investigations
- FNAC from prepatellar swelling: Aspirated pus with cytology showing scattered fungal hyphae with thin, septate, and branching morphology (Fig. 2), along with necrotic background. Giant cells and histiocytes were also noted. Findings were consistent with fungal inflammation, suggestive of phaeohyphomycosis.

Figure 2: Microscopic image from fine-needle aspiration cytology of the prepatellar swelling showing septate, branching fungal hyphae in a necrotic background, consistent with phaeohyphomycosis (×400 magnification).
- Magnetic resonance imaging depicted mild effusion with extension into the suprapatellar bursa. A well-defined oval-shaped hyperintense fluid collection was present, 10 mm × 18 mm over the prepatellar region, with signs of bursitis.
- Baseline liver function tests and renal profile were within acceptable limits at the start of treatment.
Treatment and course
Based on cytological findings and clinical suspicion, the patient was started on oral voriconazole therapy. Over the course of 3 months, the patient experienced a marked reduction in swelling (Fig. 3) and resolution of pain. However, she developed deranged liver function tests, associated with nausea and vomiting, necessitating discontinuation of voriconazole. No further antifungal therapy was initiated as her symptoms had resolved by the time of drug cessation.
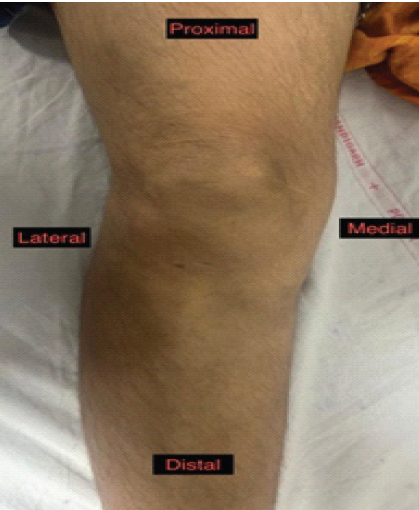
Figure 3: Follow-up clinical photograph at 1 year showing complete resolution of the prepatellar swelling with restoration of the knee contour and near-normal range of motion.
Follow-up and outcome
At her latest follow-up (approximately 1-year post-initiation of therapy), the patient remained asymptomatic, with no recurrence of knee swelling or pain. Physical examination revealed a soft, non-tender, healed prepatellar area, and she had regained a near-full range of motion. There were no clinical signs of recurrence.
Renal transplant recipients are always vulnerable to invasive fungal infections because of the long-term immunosuppressive therapy with drugs, such as calcineurin inhibitors, MMF, and steroid therapy. These drugs suppress the T-cell immune system, leading to increased susceptibility to both common and uncommon fungal pathogens [4]. The patient received a deceased donor kidney and was on cyclosporine and MMF therapy in the post-operative period. When she presented to us with prepatellar swelling without any systemic causes, initially, we thought of non-infectious bursitis. However, FNAC suggested that there were branching, septate fungal hyphae consistent with phaeohyphomycosis, which is a relatively rare cause in renal transplant recipients. The incidence of phaeohyphomycosis is extremely rare, with an incidence of 1:1,000,000/year [5]. Phaeohyphomycosis is caused due to various dematiaceous fungi with blackish pigment from the genera Wangiella, Exophiala, and Alternaria. It is widely found in the soil and is found to be an uncommon causative agent in humans, but may occur in immunocompromised or immunosuppressed patients undergoing organ transplantation [6]. A review reporting 72 cases of disseminated phaeohyphomycosis depicted 76% presenting with fever, 33% with cutaneous lesions, with skin eruptions, and ulcers. There was no case reported with any joint infection. The study reported decreased host immunity as the primary risk factor with poor outcomes reported with antifungal therapies; however, with the development of newer age antifungal agents along with combination therapy, there are promising results [7]. In the present case report, the patient presented with prepatellar bursitis with no cutaneous lesions or history of fever, depicting the rare nature of the condition, which could only be established after fungal culture. The commonest form of presentation is the development of cutaneous lesions along with subcutaneous nodules. These infections are usually superficial and preceded by a local traumatic injury after direct inoculation from contaminated earth [8]. Chahal et al. reported a rare case of joint infection with this dematiaceous fungi in a patient undergoing steroid therapy in the flexor tendon of the middle finger, leading to rupture, depicting a positive outcome after adequate antifungal therapy and debridement [9]. Thus, disease is very rarely reported with infection in the joints.
The other cases of fungal bursitis reported in the literature were caused by organisms, such as Histoplasma capsulatum [10] and Phomopsis bougainvilleicola [11]. This can spread through the hematogenous route, direct spread through minor injuries, or even local spread from the skin. In this particular patient, no history of trauma could be recalled by the patient, making hematogenous seeding a plausible route. A case report depicted a 76-year-old immunocompetent patient with suprapatellar bursitis over the knee for 2 months. The patient underwent lavage and debridement with anatomopathological analysis reporting phaeohyphomycosis. The patient was treated with itraconazole for 6 weeks with complete remission of symptoms and optimal functional outcome even after 1-year follow-up, reestablishing the need to have high suspicion of fungal infection in unusual cases [12]. Management of these kinds of cases requires early diagnosis with imaging modalities, such as ultrasound, followed by image-guided aspiration of the fluid and sending it for cytology/fluid analysis, histopathology, culture, and susceptibility testing. We have chosen voriconazole based on the susceptibility report and on the advice of the microbiologist. It also has favorable penetration into the joint tissues [13]. The patient’s symptoms resolved within 3 months of therapy, but we had to stop the drug because of its hepatotoxicity. The absence of any recurring symptoms highlights the importance of timely and targeted intervention. We report a good functional outcome after a timely intervention in collaboration with a microbiologist with no delay. It is also imperative to keep the option of debridement and lavage of the joint in such cases if no relief has occurred.
Fungal bursitis is an extremely uncommon presentation, particularly in renal transplant recipients on long-term immunosuppression. This case highlights the importance of maintaining vigilance for rare pathogens in patients with persistent bursitis unresponsive to conventional management. Early cytological confirmation, close collaboration with microbiologists, and timely initiation of antifungal therapy are critical for favorable outcomes. A multidisciplinary approach remains the cornerstone for diagnosis and management, ensuring good functional recovery and minimizing the risk of recurrence.
Chronic bursitis in immunosuppressed patients should not always be presumed bacterial; rare fungal infections, such as phaeohyphomycosis, can mimic common presentations. A high index of suspicion, early cytological diagnosis, and timely initiation of targeted antifungal therapy, supported by a multidisciplinary team, are essential to achieve favorable outcomes and prevent recurrence.
References
- 1. Mudiayi D, Shojai S, Okpechi I, Christie EA, Wen K, Kamaleldin M, et al. Global estimates of capacity for kidney transplantation in world countries and regions. Transplantation 2022;106:1113-22. [Google Scholar] [PubMed]
- 2. Mahmoud DE, Hérivaux A, Morio F, Briard B, Vigneau C, Desoubeaux G, et al. The epidemiology of invasive fungal infections in transplant recipients. Biomed J 2024;47:100719. [Google Scholar] [PubMed]
- 3. Truong J, Mabrouk A, Ashurst JV. Septic bursitis. In: StatPearls. Treasure Island, FL: StatPearls Publishing; 2025. [Google Scholar] [PubMed]
- 4. Mazzitelli M, Nalesso F, Maraolo AE, Scaglione V, Furian L, Cattelan A. Fungal infections in kidney transplant recipients: A comprehensive narrative review. Microorganisms 2025;13:207. [Google Scholar] [PubMed]
- 5. Rees JR, Pinner RW, Hajjeh RA, Brandt ME, Reingold AL. The epidemiological features of invasive mycotic infections in the San Francisco Bay area, 1992-1993: Results of population-based laboratory active surveillance. Clin Infect Dis 1998;27:1138-47. [Google Scholar] [PubMed]
- 6. Revankar SG. Phaeohyphomycosis. Infect Dis Clin North Am 2006;20:609-20. [Google Scholar] [PubMed]
- 7. Revankar SG, Patterson JE, Sutton DA, Pullen R, Rinaldi MG. Disseminated phaeohyphomycosis: Review of an emerging mycosis. Clin Infect Dis 2002;34:467-76. [Google Scholar] [PubMed]
- 8. Chowdhary A, Meis JF, Guarro J, De Hoog GS, Kathuria S, Arendrup MC, et al. ESCMID and ECMM joint clinical guidelines for the diagnosis and management of systemic phaeohyphomycosis: Diseases caused by black fungi. Clin Microbiol Infect 2014;20 Suppl 3:47-75. [Google Scholar] [PubMed]
- 9. Chahal J, Dhotar HS, Anastakis DJ. Phaeohyphomycosis infection leading to flexor tendon rupture: A case report. Hand (N Y) 2009;4:335-8. [Google Scholar] [PubMed]
- 10. Sethi J, Divyaveer SS, Gupta N, Prakash M, Kohli HS. Knee swelling in a renal transplant recipient. Indian J Transplant 2020;14:170-1. [Google Scholar] [PubMed]
- 11. Cariello PF, Wickes BL, Sutton DA, Castlebury LA, Levitz SM, Finberg RW, et al. Phomopsis bougainvilleicola prepatellar bursitis in a renal transplant recipient. J Clin Microbiol 2013;51:692-5. [Google Scholar] [PubMed]
- 12. Sadigursky D, Ferreira LN, Corrêa LM. Phaeohyphomycosis infection in the knee. Rev Bras Ortop 2016;51:231-4. [Google Scholar] [PubMed]
- 13. Saito A, Okiyama N, Hitomi S, Anzawa K, Mochizuki T, Fujimoto M. Successful treatment of cutaneous phaeohyphomycosis caused by Exophiala lecanii-corni with voriconazole. J Dermatol 2018;45:e271-2. [Google Scholar] [PubMed]