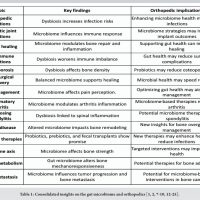
Collaborative networking in orthopedics bridges gaps in education, research, and clinical care across diverse global healthcare infrastructures, fostering inclusivity and innovation.
Dr. Madhan Jeyaraman, Department of Orthopaedics, ACS Medical College and Hospital, Dr MGR Educational and Research Institute, Chennai, Tamil Nadu, India. E-mail: madhanjeyaraman@gmail.com
Collaborations foster the exchange of knowledge, promote mentorship, and enhance research quality by uniting diverse healthcare systems and creating opportunities for young orthopedic professionals. It emphasizes the significance of partnerships bridging high-, middle-, and low-income countries to reduce disparities in training opportunities, infrastructure, and healthcare delivery. The piece highlights how international networks enable young surgeons to develop essential skills, such as leadership, management, and research methodology through professional organizations and societies. Membership in these groups provides a platform for lifelong collaborations and mentorship, shaping careers and fostering camaraderie. The integration of mentorship programs emphasizes personal and professional growth, reinforcing self-confidence and career satisfaction. Educational initiatives facilitated by networking, including continuing medical educations, virtual learning platforms, and social media, have revolutionized continuous learning. These technologies make information accessible and adaptable to individual needs, supporting clinicians in staying updated with present evidence-based practices. Virtual discussions and online forums encourage innovative research and collaborative problem-solving. Professional research organizations are showcased as enablers of high-quality research and academic growth. By supporting the dissemination of findings and fostering global collaborations, they play an instrumental role in addressing the challenges faced by low-resource settings. The article underlines the transformative impact of networking in orthopedics. While acknowledging existing challenges, it advocates for enhanced collaboration to achieve equitable and inclusive advancements in orthopedic education, research, and clinical care.
Keywords: Collaboration, networking, mentorship, research, orthopedic education.
Collaborative educational research opportunities are effective in improving and increasing scholarly assistance to orthopedic professionals. Networking in orthopedics would encompass a collaborative approach to academic and research opportunities among high-, middle-, and low-income countries. This collaboration would mean providing a larger umbrella of organized opportunities to the less privileged middle- and lower-income sectors, which are already struggling to achieve standards in the healthcare sectors. This would also mean bridging the gap and even out the disparity to academic and research opportunities across the spectrum. Orthopedic trauma has been one of the most common causes of death and disability in lower-middle and low-income country settings [1,2]. These complex orthopedic injuries result in long-term morbidity and a well-organized orthopedic network could be beneficial in a low-resource setting [1,3]. This global issue could be worsened by a lack of adequate training opportunities and substandard infrastructure, resulting in inappropriate delivery of timely orthopedic care [1]. Therefore, collaborative partnerships between countries with varied backgrounds of resources led by network building and organizational partnerships could result in bridging gaps in the healthcare sector, both in training opportunities and in delivering patient care [1,4] (Fig. 1).
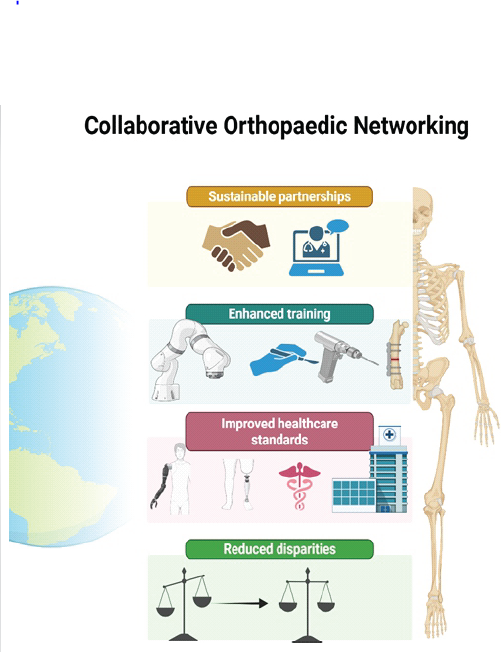
Figure 1: Various domains of collaborative orthopaedic networking.
For instance, there has been an increasing involvement of orthopedic surgeons from North American countries by volunteering in collaborative networking across borders to deliver healthcare assistance to lower-middle-income countries [1,5]. Such collaborations eventually result in the exchange of knowledge and research ideas and projects, along with clinical surgical exchange curricula, paving the way for a sustainable international surgical partnership [1,6,7,8] (Fig. 2). This review aims to analyze the importance, limitations, and recommendations for improving collaborative educational and research opportunities in Orthopedics.
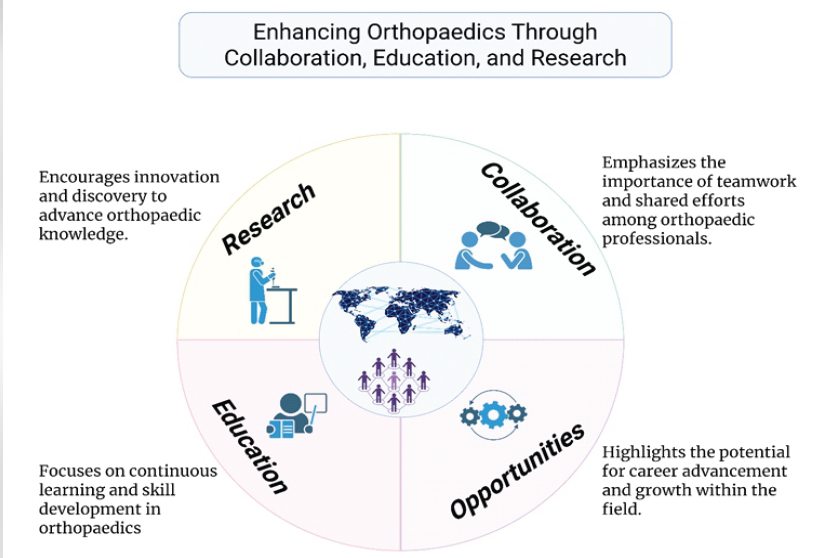
Figure 2: Various domains of networking in orthopaedics.
Collaboration in orthopedic surgery encompasses a successful partnership among academia around the world with an effort to establish a dedicated and committed relationship which benefits and promotes mutual sustainability and capability while also nurturing self-dependence and leadership [9,10,11,12]. Over the years, increasing collaboration in academia, in contrast to mere voluntary work, has improved the standard of research activities both quantitatively and qualitatively [1,9,10]. Good quality research could play a vital role in the dissemination of knowledge for the benefit of the clinician and the provider [9,11]. Although there is a significant increase in published research regarding traumatic conditions across all income group setups, the evidence in the literature cannot be considered a standard in low-income countries due to the existent inconsistency in training opportunities and infrastructure [9,13,14]. Therefore, there is a need for a better quality of research in these countries, thereby necessitating networking partnerships among the higher and lower resource setups [9,15]. This would also pave the way for better funding of resources with improved trainee guidance, thereby improving the standard of supported research opportunities as well [9,16]. Successful academic partnerships have been set up in many medical and surgical fields around the world [9,17,18,19,20,21]. Collaborative networking helps in improving building capabilities and the quicker recruitment of patients into trials while also generalizing the results, which leads to increased development of clinical and research infrastructure in low-income countries [22]. Such collaborations do help young orthopedic surgeons to develop certain skillsets, such as management skills, early on in their career [22]. Such collaborations on a global scale also result in a paradigm shift in helping tap the potential for medical research among hospitals operating form conflict zones as well [22,23]. Such research with hospitals in conflict zones not only help in increasing the influence of such centers but leads to quicker and widespread application of the result outcomes [22,23]. Such centers would also be a valuable addition in achieving equity in health around the world [22,24]. There is a necessity to develop international networks for young orthopedic surgeons who are trained in research methodology with a solid backing of trial centers and research networks [22,23]. Networking has provided surgeons from developing countries to be a part of a high-quality world call surgical research, which sometimes could be challenging to in a well-designed and developed country with high-income infrastructure as well [22].
Opportunities
Orthopedic surgery remains to be one of the most competitive branches among surgical specialties. However, it also continues to remain one of those surgical specialties where there is a lack of diversity with the underrepresentation of women according to a census report published by the American Academy of Orthopaedic Surgeons (AAOS) in 2018 [25,26,27,28,29,30,31]. Young orthopedic surgeons could find early career support opportunities through professional orthopedic organizations and societies [32]. Through these societies, orthopedic surgeons could also find an opportunity to develop camaraderie and fellowship among their cohort. This also provides them with an opportunity to hone their interpersonal skills and develop their leadership qualities while being able to provide their input for the development of guidelines for new research and management [32]. The involvement of surgeons and physicians in such leadership roles for training, research, and collaboration is beneficial to many studies [32,33,34,35]. Memberships of these societies and professional organizations could also offer many benefits to budding orthopedic surgeons during the initial stages of their careers by streamlining their interests, resulting in lifelong collaborations among surgeons of the same subspecialties [32]. Such professional collaborations could contribute to long-term beyond official activities, thereby resulting in a very casual and informal atmosphere, paving the way for better mentorships [32]. Such mentorships could also result in providing better guidance and professional fellowship opportunities in the same subspecialty. Such opportunities would contribute to shaping young orthopedic surgeons if they get introduced to professional societies early on in their careers. Leadership programs, such as AAOS Leadership Institute provide a good exposure to a leader’s perspective of mentorship and learning through personal mentoring, which is quite a unique initiative in itself in recent times [32]. Long-term collaborations and networking among professionals not only result in lifelong camaraderie but also help and inspire professional bodies to mentor, support, and create national and international fellows through collaborative initiatives [32,36].
Education
Networking and collaborations across the board are also very beneficial in creating additional learning opportunities. These opportunities are usually created through continuing medical education (CME) through courses and conferences. These CMEs provide opportunities for constant updates of additional knowledge along with some credit points, which could also help the young professionals to use for their annual appraisal and revalidation of their medical license. Continuing professional development can be achieved through conferences, courses, virtual learning platforms, and various other activities organized by professional organizations or societies. Nowadays, almost all such societies and organizations offer free virtual online learning courses, conferences, and free webinars, which are very helpful in regular professional learning.
Present advancements in social media and virtual learning platforms have resulted in a paradigm shift by revolutionizing the teaching-learning pathway by making it more interactive. Online virtual learning resources can be referred to as a portal to virtually access audiovisual access to information, as well as publications and journal databases [37]. It has many other new names, such as electronic learning (e-learning), webinars, and distributed and technology-mediated learning [37,38]. Resources, such as Web 2.0 have helped trainers or mentors with the provision of disseminating knowledge in a much more succinct manner with good content [37]. Online learning through virtual platforms or remote learning will enable trainees to tailor the CME to suit their personalized needs by signing into relevant ones and listening to them at their convenience within the target dates set by the providing society. Across these platforms, trainees and orthopedic surgeons could also involve themselves in discussions and exchange of knowledge, and also expand their social networking. This will also enable them to create a certain niche for themselves in their field of interest for research as well. The discussions held in these forums could result in better research and much better quality of research being published as well.
Mentorship
Mentorship, in simple words, would mean offering specific guidance with specific small goals to nurture a particular professional and/or personal aspect of a trainee or an orthopedic surgeon. Mentoring involves fostering a certain relationship with the juniors to nurture the all-around personal and professional development of an inexperienced individual [39,40,41]. Such a mentorship in orthopedics is extremely important in shaping a future orthopedic surgeon’s career. Mentorships are advantageous in providing self-reliance and self-confidence to have career growth with job satisfaction as well [40]. Mentors play a vital role in providing trainees with useful constructive feedback laced with expert advice and suggestions depending on the mentee’s needs. Such feedback could, in turn, shape the outcome of training if these suggestions are incorporated and thereby play a crucial role in a trainee’s career advancement and overall progress. Providing constructive feedback also helps the mentor in developing new techniques in providing useful feedback while also helping the trainee to reflect on them. This sets in tune a loop of training, feedback, learning, and incorporating, which in turn results in a better training experience. In addition to these, an ideal mentor-mentee relationship would be to build a culture of cohesiveness with importance to the exchange of thought rather than having monologues constrained and directed by hierarchy [39,42]. Therefore, mentorship is counterproductive for the progress and career advancement of both mentor and mentee, where learning becomes a shared and ongoing learning experience [39,43].
Professional research organizations have always been seen as the apex bodies of research activities in their respective subspecialties. These societies play a major role in networking and bridging gaps among orthopedic surgeons and also guide budding trainees with firsthand experience of interpersonal relationships and cultivating research methodology. These societies and professional organizations provide a platform for young orthopedic surgeons and trainees to publish or present their investigative research and to discuss their results with other colleagues. Such large congregations, although help in building collaborative networks, they also allow the young researchers to share their work and results with a larger audience and the orthopedic fraternity or subspecialty. This paves the way and helps in the dissemination of knowledge through various forms of presentations, such as posters, podium presentations, and panel discussions, and allows others to provide the researcher with constructive feedback. Such feedback is instrumental in creating collaborative networks through interpersonal relationships, which develop out of the exchange of ideas and discussions. These presentations also help the trainees update their knowledge and remain in tandem with recent evidence in the literature. Networking also helps in the creation of multicenter networks where colleagues from across a region working in different types of setups, such as Major Trauma Centers and local Trauma Units, could collaborate in churning out good quality research and publications. An example of such collaboration would be the Musculoskeletal Oncology Research Initiative, which is a multicentric collaborative initiative that helps to provide a platform for regional-level research projects while also building connections across larger regions [32]. Research helps an orthopedic surgeon or a young trainee to create a niche for themselves. Trainee orthopedic surgeons could also benefit from being exposed to the larger medical fraternity and among their subspecialty cohort. This could propel them to be recipients of coveted grants and sponsorships for major research activities [32]. Such prestigious grants and awards could further help the trainees to get noticed among their cohort and by other senior colleagues, making them accessible for future career opportunities. Apart from such large congregations, smaller local workshops could also be beneficial in building networks. Trainees could get an opportunity to express their teaching potential while also building collaborative networks through workshops. Although such workshops help the trainees hone their teaching skills, they also are of value in helping the trainee develop leadership quality and interpersonal managerial skills. These skills are integral for achieving a successful clinical and research career [32]. Surgeons are also provided opportunities through professional societies to develop specific surgical skills in the subspecialty of their interest. Such initiatives could help nurture their interests and help the young orthopedic trainees build their careers.
Collaborative networking helps in creating educational and research opportunities for orthopedic professionals and young trainees. Networking in orthopedics should involve and include a collaborative approach to bridge the gap in the academic and research sectors among countries with developed and developing infrastructure. This would in turn result in creating opportunities for the less privileged middle- and lower-income healthcare sectors. Collaborative educational research opportunities are effective in aiding young scholars and orthopedic trainees. Networking becomes necessary in creating inclusive opportunities to encourage active academic and research in developing countries to attract increased funding of resources. Professional organizations are important for playing a major role in networking and bridging gaps among orthopedic surgeons. These societies can also help offer opportunities to surgeons through workshops, conferences, and courses where the research outcomes can be shared and discussed, and be of great importance for the exchange of knowledge and career opportunities. Although there are ample opportunities that are available, the present scenario presents many challenges to budding talents from developing countries and low-resource societies. Therefore, we conclude that there is more work that needs to be done in this sector, which can be achieved by better and improved networking.
• Networking in orthopedics bridges disparities by promoting partnerships between high-, middle-, and low-income countries, improving training and patient care
• Collaborative research partnerships enhance the quality and applicability of studies, especially in resource-limited settings, by facilitating knowledge sharing and infrastructure development
• CME, virtual learning platforms, and professional societies revolutionize learning, ensuring accessibility and the dissemination of updated medical knowledge
• Structured mentorship fosters personal and professional growth, building confidence, self-reliance, and better career trajectories for young orthopedic surgeons
• Involvement in societies and mentorship programs provides early-career professionals with leadership opportunities, interpersonal skills, and lifelong collaborations.
References
- 1. Miclau T, MacKechnie MC, Shearer DW, Coact group. Consortium of orthopaedic academic traumatologists: A model for collaboration in orthopaedic surgery. J Orthop Trauma 2018;32:S3-7. [Google Scholar] [PubMed]
- 2. Haagsma JA, Graetz N, Bolliger I, Naghavi M, Higashi H, Mullany EC, et al. The global burden of injury: Incidence, mortality, disability-adjusted life years and time trends from the global burden of disease study 2013. Inj Prev 2016;22:3-18. [Google Scholar] [PubMed]
- 3. Mock C, Cherian MN. The global burden of musculoskeletal injuries: Challenges and solutions. Clin Orthop 2008;466:2306-16. [Google Scholar] [PubMed]
- 4. Riviello R, Ozgediz D, Hsia RY, Azzie G, Newton M, Tarpley J. Role of collaborative academic partnerships in surgical training, education, and provision. World J Surg 2010;34:459-65. [Google Scholar] [PubMed]
- 5. Butler MW, Krishnaswami S, Rothstein DH, Cusick RA. Interest in international surgical volunteerism: Results of a survey of members of the American pediatric surgical association. J Pediatr Surg 2011;46:2244-9. [Google Scholar] [PubMed]
- 6. Conway DJ, Coughlin R, Caldwell A, Shearer D. The institute for global orthopedics and traumatology: A model for academic collaboration in orthopedic surgery. Front Public Health 2017;5:146. [Google Scholar] [PubMed]
- 7. Ritman D. Health partnership research and the assessment of effectiveness. Glob Health 2016;12:43. [Google Scholar] [PubMed]
- 8. Spiegel DA, Abdullah F, Price RR, Gosselin RA, Bickler SW. World health organization global initiative for emergency and essential surgical care: 2011 and beyond. World J Surg 2013;37:1462-9. [Google Scholar] [PubMed]
- 9. Flores MJ, MacKechnie MC, Brown KE, O’Marr JM, Rodarte P, Socci A, et al. The current state of international academic partnerships in orthopaedic surgery between high-income and low and middle-income countries: A systematic review. JB JS Open Access 2024;9:e24.00033. [Google Scholar] [PubMed]
- 10. Shearer DW, Morshed S, Coughlin RR, Miclau T. From mission trips to partnerships: The evolution of international outreach. J Orthop Trauma 2018;32:S1-2. [Google Scholar] [PubMed]
- 11. Brown K, Flores MJ, Haonga B, Chokotho LC, Marr JM, Rodarte P, et al. Best practices for developing international academic partnerships in orthopaedics. J Bone Joint Surg Am 2024;106:924-30. [Google Scholar] [PubMed]
- 12. Beran D, Byass P, Gbakima A, Kahn K, Sankoh O, Tollman S, et al. Research capacity building-obligations for global health partners. Lancet Glob Health 2017;5:e567-8. [Google Scholar] [PubMed]
- 13. Museru LM, McharoCN. The dilemma of fracture treatment in developing countries. Int Orthop 2002;26:324-7. [Google Scholar] [PubMed]
- 14. Dormans JP, Fisher RC, Pill SG. Orthopaedics in the developing world: Present and future concerns. J Am Acad Orthop Surg 2001;9:289-96. [Google Scholar] [PubMed]
- 15. Morshed S, Shearer DW, Coughlin RR. Collaborative partnerships and the future of global orthopaedics. Clin Orthop Relat Res 2013;471:3088-92. [Google Scholar] [PubMed]
- 16. Wu HH, Liu M, Patel KR, Turner W, Baltus L, Caldwell AM, et al. Impact of academic collaboration and quality of clinical orthopaedic research conducted in low- and middle-income countries. SICOT J 2017;3:6. [Google Scholar] [PubMed]
- 17. Kohrt BA, Upadhaya N, Luitel NP, Maharjan SM, Kaiser BN, MacFarlane EK, et al. Authorship in global mental health research: Recommendations for collaborative approaches to writing and publishing. Ann Glob Health 2014;80:134-42. [Google Scholar] [PubMed]
- 18. Bloomfield GS, Xavier D, Belis D, Alam D, Davis P, Dorairaj P, et al. Training and capacity building in LMIC for research in heart and lung diseases: The NHLBI-unitedhealth global health centers of excellence program. Glob Heart 2016;11:17-25. [Google Scholar] [PubMed]
- 19. Moraes VY, Belloti JC, Faloppa F, Bhandari M. Collaborative multicenter trials in Latin America: Challenges and opportunities in orthopedic and trauma surgery. Sao Paulo Med J 2013;131:187-92. [Google Scholar] [PubMed]
- 20. Ranganathan P, Chinnaswamy G, Sengar M, Gadgil D, Thiagarajan S, Bhargava D, et al. The international collaboration for research methods development in oncology (CReDO) workshops: Shaping the future of global oncology research. Lancet Oncol 2021;22:e369-76. [Google Scholar] [PubMed]
- 21. Gibbons RV, Nisalak A, Yoon IK, Tannitisupawong D, Rungsimunpaiboon K, Vaughn DW, et al. A model international partnership for community-based research on vaccine-preventable diseases: The Kamphaeng Phet-AFRIMS virology research unit (KAVRU). Vaccine 2013;31:4487-500. [Google Scholar] [PubMed]
- 22. El-Hussuna A, Tolani MA. Current status and future perspectives of collaboration in surgical research: A scoping review of the evidence. Surgery 2021;170:748-55. [Google Scholar] [PubMed]
- 23. Søreide K, Alderson D, Bergenfelz A, Beynon J, Connor S, Deckelbaum DL, et al. Strategies to improve clinical research in surgery through international collaboration. Lancet 2013;382:1140-51. [Google Scholar] [PubMed]
- 24. Schwalbe N, Wahl B. Artificial intelligence and the future of global health. Lancet 2020;395:1579-86. [Google Scholar] [PubMed]
- 25. Nimmons D, Giny S, Rosenthal J. Medical student mentoring programs: Current insights. Adv Med Educ Pract 2019;10:113-23. [Google Scholar] [PubMed]
- 26. Day CS, Lage DE, Ahn CS. Diversity based on race, ethnicity, and sex between academic orthopaedic surgery and other specialties: A comparative study. J Bone Joint Surg Am 2010;92:2328-35. [Google Scholar] [PubMed]
- 27. Daniels EW, French K, Murphy LA, Grant RE. Has diversity increased in orthopaedic residency programs since 1995? Clin Orthop Relat Res 2012;470:2319-24. [Google Scholar] [PubMed]
- 28. Okike K, Utuk ME, White AA. Racial and ethnic diversity in orthopaedic surgery residency programs. J Bone Joint Surg Am 2011;93:e107. [Google Scholar] [PubMed]
- 29. Poon S, Kiridly D, Mutawakkil M, Wendolowski S, Gecelter R, Kline M, et al. Current trends in sex, race, and ethnic diversity in orthopaedic surgery residency. J Am Acad Orthop Surg 2019;27:e725-33. [Google Scholar] [PubMed]
- 30. Haffner MR, Van BW, Wick JB, Le HV. What is the trend in representation of women and under-represented minorities in orthopaedic surgery residency? Clin Orthop Relat Res 2021;479:2610-7. [Google Scholar] [PubMed]
- 31. Paulson AE, Gu A, Dy CJ, Fufa DT, Wessel LE. Opportunities for increasing diversity in orthopaedics through virtual mentorship programs. J Am Acad Orthop Surg 2023;32:147-55. [Google Scholar] [PubMed]
- 32. Mun F, Suresh KV, Pollak AN, Morris CD. Professional society opportunities and involvement for early-career orthopaedic surgeons. J Am Acad Orthop Surg 2023;31:167-80. [Google Scholar] [PubMed]
- 33. Stoller JK. Developing physician-leaders: Key competencies and available programs. J Health Adm Educ 2008;25:307-28. [Google Scholar] [PubMed]
- 34. Schwartz RW, Pogge C. Physician leadership: Essential skills in a changing environment. Am J Surg 2000;180:187-92. [Google Scholar] [PubMed]
- 35. Schwartz RW, Pogge CR, Gillis SA, Holsinger JW. Programs for the development of physician leaders: A curricular process in its infancy. Acad Med 2000;75:133-40. [Google Scholar] [PubMed]
- 36. Thevendran G, Glazebrook M, Eastwood D, Weber K, Kit DC, Johari A. et al. Rising within the leadership of an orthopaedic society: Learning from the presidents. Int Orthop 2022;46:443-7. [Google Scholar] [PubMed]
- 37. Anshari M, Alas Y, Guan LS. Developing online learning resources: Big data, social networks, and cloud computing to support pervasive knowledge. Educ Inf Technol 2016;21:1663-77. [Google Scholar] [PubMed]
- 38. McGill TJ, Klobas JE. A task-technology fit view of learning management system impact. Comput Educ 2009;52:496-508. [Google Scholar] [PubMed]
- 39. Bhadani JS, Mukhopadhaya J. The role of mentorship in orthopedic professional development: From training to mastery. J Orthop Case Rep 2025;15:289-300. [Google Scholar] [PubMed]
- 40. Mohamed I, MacBeth R, Stephens K, Ramaiya N, Plecha D. Women in academic radiology: Barriers and benefits of representation, mentorship, coaching, and advocacy. Curr Probl Diagn Radiol 2025;54:108-14. [Google Scholar] [PubMed]
- 41. Agarwal BB, Agarwal N, Dhamija N, Chintamani. Mentoring in surgery-mentor, parshuram, dronacharya, krishan. Indian J Surg 2018;80:81-3. [Google Scholar] [PubMed]
- 42. Hirsch B, Whittington KD, Walker J. Mentoring in radiologic science. J Med Imaging Radiat Sci 2020;51:354-7. [Google Scholar] [PubMed]
- 43. Van Patten RR, Bartone AS. The impact of mentorship, preceptors, and debriefing on the quality of program experiences. Nurse Educ Pract 2019;35:63-8. [Google Scholar] [PubMed]