To emphasize that low-velocity airgun injuries in children, though often considered harmless, can penetrate deeply into the cervical region without causing immediate neurological deficits underscoring the need for early evaluation, parental supervision, and stronger public awareness to prevent such injuries.
Dr. Chirag Sharma, Department of Orthopaedics, North Eastern Indira Gandhi Regional Institute of Health and Medical Sciences, Shillong, Meghalaya, India. E-mail: chiragammu@gmail.com
Introduction: Airgun or air-rifle injuries are often perceived as minor injuries; however, they can cause significant morbidity, particularly in children. The cervical spine, with its vital neurovascular and airway structures around, is vulnerable to any penetrating injury, even to low-velocity projectiles.
Case Report: We report the case of a 9-year-old boy who sustained an accidental posterior cervical airgun injury at home. The child was neurologically intact, and imaging revealed a retained metallic pellet deeply embedded in the posterior aspect of the neck impacted within the edge of the right lateral mass of the C7 vertebra without involvement of the spinal canal or injury to major vessels. Multiple unsuccessful retrieval attempts were performed at the district hospital before the pellet was successfully removed surgically at our tertiary care institute. The post-operative course was uneventful, and the child remained asymptomatic on follow-up.
Conclusion: Pediatric cervical airgun injuries, though often considered minor, can endanger vital cervical structures. Even in neurologically intact patients, retained projectiles may warrant surgical removal when safely accessible to prevent delayed complications such as infection or migration. This case underscores the principle of decision-making beyond deficits, where management is guided by anatomical risk, long-term safety, and the imperative to raise public awareness about the potential dangers of airguns in children.
Keywords: Airgun injuries, cervical vertebrae, penetrating wounds, decision-making.
Literature reports of air-gun pellet injuries to the brain, heart, eye, sinus, abdominal injuries, intrauterine fetal injury, skull fractures [1,2,3,4,5,6,7,8], with infrequently described for spinal [9]. Although often perceived as toys, air guns are widely available in retail outlets and sold without regulation despite their capacity to inflict serious harm. These weapons can cause significant and occasionally fatal injuries, particularly in children and adolescents. Public perception frequently underestimates the severity of air-gun trauma, yet injuries from pellets that involve the brain or spine can have devastating consequences [9]. While some foreign bodies can remain asymptomatic, we report a case of an air gun pellet removal with prior history of attempted removals where decision-making for the removal was made beyond deficits, guided by anatomical risk, long-term safety, and patient’s parent’s high desire and pursual.
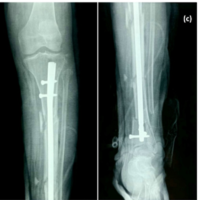
A 9-year-old male child was referred to our tertiary care center with a history of an air gunshot injury sustained 3 months back. History revealed that the injury occurred at home while playing, and the airgun accidentally discharged unintentionally. Immediate medical attention was sorted at the nearby healthcare facility, where he was found to be hemodynamically stable with intact neurology. There were two surgical failed attempts elsewhere to retrieve the bullet, and eventually the child was referred to our institute for further management. At our center, on examination, the child had a healed surgical scar present over the lower posterior aspect of the neck, with no signs of local infection, swelling, discharge, and neurological examination revealed no gross deficits. Plain radiography showed foreign body at the level of C7 Cervical spine on the right side (Fig. 1).

Figure 1: Radiograph (a and b) shows Foreign body (pallet) impacted in the right C7 lateral mas.
Computed tomography of the cervical spine showed the presence of a retained metallic foreign body in the posterior aspect of the neck embedded in the outer edge of the lateral mass of the C7 with no evidence of breaching the vertebral foramen (Fig. 2a and 2b). Computed tomography (CT) angiography (Fig. 2c) ruled out injury to the vertebral arteries or other major vessels.

Figure 2: (a) Axial computed tomography (CT) showing a metallic object impacted at the outer edge of the right lateral mass (b) Sagittal CT showing the metallic object at C7 (c) CT angiography to see for the vertebral artery integrity.
Considering the duration of the retained pellet with two previous failed attempts removal our team initially planned for a conservative management with no further surgical exploration, and the plan was shared to the parents. A repeated parental anxiety with future a concern regarding potential delayed complications led our team to the decision for surgical exploration to go ahead for the pellet retrieval after being explained all the potential risk factors pertaining to the surgical procedure. A posterior midline approach was carried out with bilateral subperiosteal dissection of posterior element of the posterior cervical spine from C5 to T1 level, a careful meticulous thinning of the right C7 lateral mass was carried out with high-speed burr more toward the edge of the lateral mass as per the CT image till the visibility of the pellet, once the pellet was exposed it was caught with the help of artery forceps and ultimately successfully removed with no surgical complications. To ensure the cervical spine remained stable because of the thinning of the lateral mass, unilaterally stabilization with a lateral mass screw was carried out. The procedure was uneventful, and the patient was discharged from the hospital on the 5th post-operative day (Fig. 3).

Figure 3: Peroperative photography (a) exposure of posterior element of cervical spine from C6 to T1 (b) after burring of the edge of the C7 lateral mass with the visible pallet (c) retrieved Pallet (d) unilateral stabilization with lateral mass screws.
Air-gun injuries have often been underestimated as toy injuries; however, multiple authors emphasize that these can lead to serious morbidity, including vascular, airway, neurologic, and infectious complications [1,2,3,4,5,6,7,8]. Retained projectiles from low-velocity weapons such as air-rifle pellets pose a challenging management dilemma, especially when lodged near critical structures such as the spine. The decision between conservative versus surgical management hinges on multiple factors, including neurologic status, risk of delayed complications (infection, fibrosis, lead toxicity), location of the foreign body, and patient parental concerns. In our case, although the initial plan was for a conservative management taking into consideration that the pellet had been lodged and retained for a period of three months with no neurological deficit or deterioration, and the previous two prior unsuccessful removal attempts. Our surgical reconsideration and decision was solely undertaken based on the ground of a doubtful concern regarding its potential delayed complications like infection, fibrosis, migration to the nearby potential vulnerable vital structures, and at the topmost a repeated parental anxiety and pursual from the parent that tilted the balance toward surgery for a reattempt pellet removal, which was carried out with successfully with no complication. Pellet and air-gun injuries involving the neck and spine are rare but well-documented. A reported case of a pellet lodged in the C1 vertebra of a child was managed conservatively, with the patient remaining asymptomatic at one-year follow-up, suggesting that non-operative management may be appropriate in carefully selected cases with stable injuries and no neurological deficit [9]. In contrast, another report described a pellet embedded in the external carotid artery following a neck injury necessitating urgent surgical repair due to vascular compromise [10]. Similarly, an air rifle pellet causing penetrating neck trauma led to vertebral artery injury and Brown-Sequard syndrome, which required decompression and stabilization surgery [11]. Conversely, a shotgun pellet retained beneath the carotid artery intima remained intact and complication-free for six months, indicating that completely embedded, infection-free missiles may often be well tolerated [12]. Given the rarity of such cases and heterogeneity of their presentations, we recommend that any retained pellet near the spine be discussed in a multidisciplinary setting and that the decision for removal be individualized taking into account the anatomical location (spinal canal or safe paraspinal region), trajectory and proximity to vessels or nerves, patient age, functional status and parental or patient expectations the number and success of prior removal attempts, duration of retention as long standing foreign bodies likely to incite fibrosis and access to surgical expertise and imaging modalities.
While a conservative management strategy may be acceptable for retained pellets in neurologically intact patients with favorable anatomy, the presence of risk factors such as failed prior removal, protracted retention, anatomical proximity to vulnerable structures, and parental anxiety should prompt careful reconsideration. Our case underscores that in such situations, surgical exploration and retrieval can be performed safely and lead to a good outcome. Future reports with longer follow-up would be valuable to better delineate guidelines for timing and indications of removal in such rare injuries.
Low-velocity airgun injuries in children may appear harmless but can lodge near vital cervical structures. Early imaging and anatomy-guided decision-making are essential even in neurologically intact patients.
References
- 1. Martínez-Lage JF, Mesones J, Gilabert A. Air-gun pellet injuries to the head and neck in children. Pediatr Surg Int 2001;17:657-60. [Google Scholar] [PubMed]
- 2. Gilmour DF, Ramaesh K, Fleck BW. Trans-orbital intra-cranial air gun injury. Eur J Ophthalmol 2003;13:320-3. [Google Scholar] [PubMed]
- 3. Alexandrakis G, Davis JL. Intracranial penetrating orbital injury. Ophthalmic Surg Lasers 2000;31:61-3. [Google Scholar] [PubMed]
- 4. Aslan S, Uzkeser M, Katirci Y, Cakir Z, Bilir O, Bilge F, et al. Air guns: Toys or weapons? Am J Forensic Med Pathol 2006;27:260-2. [Google Scholar] [PubMed]
- 5. DeCou JM, Abrams RS, Miller RS, Touloukian RJ, Gauderer MW. Life-threatening air rifle injuries to the heart in three boys. J Pediatr Surg 2000;35:785-7. [Google Scholar] [PubMed]
- 6. Chhetri DK, Shapiro NL. A case of a BB-gun pellet injury to the ethmoid sinus in a child. Ear Nose Throat J 2004;83:176-80. [Google Scholar] [PubMed]
- 7. Bhattacharyya N, Bethel CA, Caniano DA, Pillai SB, Deppe S, Cooney DR. The childhood air gun: Serious injuries and surgical interventions. Pediatr Emerg Care 1998;14:188-90. [Google Scholar] [PubMed]
- 8. Muzumdar D, Higgins MJ, Ventureyra EC. Intrauterine penetrating direct fetal head trauma following gunshot injury: A case report and review of the literature. Childs Nerv Syst 2006;22:398-402. [Google Scholar] [PubMed]
- 9. Alromaih NI, Alharbi HN, Altwaijri NA, Surur SR. Air-gun pellet at C1: A case report and literature review. J Spine Surg 2023;9:375-9. [Google Scholar] [PubMed]
- 10. Abad S, McHenry ID, Carter LM, Mitchell DA. Carotid artery injury from an airgun pellet: A case report and review of the literature. Head Face Med 2009;5:3. [Google Scholar] [PubMed]
- 11. Mahadhipta H, Shiddieqy Pohan MA, Bakri AH. Vertebral artery injury due to air rifle: A case report. Ann Med Surg (Lond) 2021;63:102149. [Google Scholar] [PubMed]
- 12. Manousi M, Sarantitis I, Papadoulas S, Diamantopoulos A, Kakkos SK, Lampropoulos G, et al. Retained subintimal pellet in a carotid artery. J Cardiovasc Ultrasound 2011;19:105-6. [Google Scholar] [PubMed]