Plate fixation over a retained broken magnetic nail can successfully restore stability and achieve union, offering a practical salvage option when nail removal is high-risk.
Dr. Mazlum Veysel Sili, Department of Orthopedics and Traumatology, Faculty of Medicine, Hacettepe University, 06000, Altindag, Ankara, Turkey. E-mail: mazlumxsili@gmail.com
Introduction: Magnetic intramedullary nails are used for deformity correction and limb lengthening because of their minimally invasive nature and reduced complication rates compared to external fixators. However, complications such as non-union and nail breakage remain rare but significant clinical challenges, particularly in cases with patient-specific risk factors. This case demonstrates a successful union after nail fracture without the removal of the intramedullary nail, using lateral plate fixation, offering a salvage option in this uncommon scenario.
Case Report: A 22-year-old female with congenital left leg shortening, previously treated with two external fixator lengthening procedures and later plate fixation after a tibia fracture, presented with progressive genu valgum and 4 cm limb-length discrepancy. Deformity correction and lengthening using a magnetic intramedullary tibial nail were performed, with an uneventful 1-week latency phase and 6-week distraction phase. Because of delayed union during consolidation, bone marrow aspirate concentrate injection was performed at post-operative 5th month, followed by iliac crest autograft placement on post-operative 7th month. At post-operative 10th month, she experienced sudden pain and a snapping sensation while descending stairs, came to the emergency room, and imaging revealed nail fracture. Revision surgery was performed, and the broken nail was intentionally left in situ and stabilized with a lateral locking plate. The patient achieved uneventful recovery with progressive weight-bearing and radiographic union, regaining full function at 9th month.
Conclusion: Magnetic intramedullary nails, while effective for limb lengthening, can fail mechanically because of delayed union and poor adherence to rehabilitation protocols. Recognizing the complications early and actively addressing risk factors are essential to improving the outcome. Most importantly, this case report shows that plate fixation over a retained broken magnetic tibial nail can restore stability and lead to union and functional recovery without the need for implant removal, offering a practical treatment option for this uncommon but challenging complication.
Keywords: Case report, magnetic intramedullary lengthening nail, distraction osteogenesis, tibia lengthening, plate fixation.
Intramedullary nails have changed the way limb length discrepancies and extremity deformities are treated by enabling controlled, minimally invasive distraction osteogenesis with fewer soft-tissue complications, better patient comfort, and improved cosmetic outcomes compared to external fixators [1,2]. Among these systems, magnetically driven nails such as the PRECICE® nail have seen widespread usage due to their precision, adjustability, and reduced need for secondary procedures. Despite these advantages, complications such as delayed union, non-union, and mechanical failure remain important clinical concerns, particularly in patients with risk factors that impair bone healing or compromise implant stability [3]. Mechanical failure, although relatively uncommon, with an overall rate reported around 9.5%, can occur when excessive mechanical loading, premature weight-bearing, or insufficient regenerative formation exceeds the implant’s structural capacity [4]. Patients with prior surgeries, altered bone biology, or smoking history are especially challenging, as the risk of delayed healing and implant failure is higher [5,6]. This case demonstrates that magnetic nail deformation and subsequent fracture can occur even during the consolidation phase, particularly in patients with risk factors that compromise bone healing. More importantly, it shows that plate fixation over a retained broken magnetic nail can be an effective salvage strategy, restoring mechanical stability and allowing successful bone union without the need for implant removal. This rarely reported approach broadens the available management options for mechanical failure of magnetic nails and highlights the importance of individualized decision-making to preserve limb function and minimize additional morbidity.
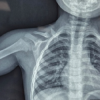
A 22-year-old female came to our clinic with a history of congenital shortening and deformity of the left lower extremity, first noticed shortly after birth and becoming more pronounced over time, leading to her first medical evaluation at another center by the age of four. In 2013 and 2017, she underwent two limb-lengthening procedures using external fixators. These operations partially corrected the limb-length difference but were later followed by a tibial fracture in 2018, which was treated with open reduction and internal fixation with a locking plate. After rehabilitation, the patient was able to walk without pain. She had no comorbidities and was not on regular medications. She had a smoking history of 4 pack-years, and she continued to smoke despite the medical advice. She worked in a sedentary occupation, was independent in daily activities, and had a body mass index of 23,03 kg/m2. There was no known family history of genetic disorders or relatives with congenital limb deformities or skeletal dysplasia. In February 2024, she was evaluated in our clinic for deformity and functional limitation of the left leg. Physical examination showed valgus alignment of the knee, approximately 4 cm of limb-length discrepancy, and a mildly asymmetric gait. Both the knee and ankle were stable with a full range of motion, and neurovascular findings were normal. There were no signs of infection or soft-tissue problems. Standard full-length lower extremity radiograph showed valgus deformity of the knee with a mechanical axis deviation of 52 mm, mechanical lateral distal femoral angle of 87°, medial proximal tibial angle of 102°, as well as the presence of a previous plate fixation (Fig. 1).

Figure 1: Standing full-length radiograph (a) taken before the intramedullary nail procedure showing mechanical axis deviation [1], mechanical lateral distal femoral angle [2], and medial proximal tibial angle [3]. Anterior-posterior (b) and lateral (c) radiographs taken after the surgery.

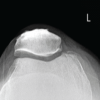
Figure 2: Anterior-posterior (a) and lateral (b) radiographs taken at 12th-week follow-up, showing insufficient callus formation.
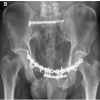
In December 2024, the patient came to our clinic with a sudden “snapping” sensation and acute pain in the left leg while descending stairs. On physical examination, there was tenderness and mild swelling on the tibia shaft, and weight-bearing was painful. The skin was intact, there were no signs of infection or neurovascular damage. The knee and ankle joints maintained a near-full range of motion, limited only by pain. A fracture of the intramedullary lengthening nail at the telescopic junction was seen on the radiographs (Fig. 3). Given the incomplete consolidation, concern for disrupting the healing process, and the procedure being technically demanding, removal of the broken nail was deemed high-risk. Instead, a salvage procedure was performed: The valgus deformity was corrected using external distractors, and internal fixation of the fracture was achieved by applying a 4.5 mm broad lateral locking plate over the retained nail, spanning the osteotomy site. Imaging confirmed satisfactory alignment and fixation (Fig. 3). The procedure was completed without complications.

Figure 3: Anterior-posterior (a) and lateral (b) radiographs taken at the emergency department and anterior-posterior (c) and lateral (d) radiographs taken after the surgery.
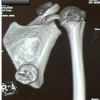
After the procedure, the patient started toe-touch mobilization at 4th week, partial weight bearing at 8th week, and full weight bearing at 12th week. At post-operative 9th month, the patient reported no resting pain and could walk for 20 min without discomfort. Clinical examination showed a full range of motion in the knee and ankle; satisfactory callus formation was seen on the radiographs (Fig. 4).

Figure 4: Anterior-posterior (a) and lateral (b) radiographs taken at 9th-month follow-up, showing callus formation.
Functional scores were also improved: Lower extremity functional scale improved from pre-op 45/80 to 76/80 at 9th month, Visual Analog Scale (VAS) pain scores decreased from seven (walking) and four (rest) to two and zero, respectively, and the SF-12 physical component summary (PCS) improved from 32 to 52. No additional complications occurred during follow-up. The timeline of management, from 2013 to the last follow-up, is summarized in Table 1.

Table 1: Timeline of the patient’s treatment
Magnetic intramedullary nails, such as the PRECICE® system, have revolutionized the management of limb length discrepancy and deformity correction due to their minimally invasive nature and precise control over the distraction process. However, despite their numerous advantages, complications such as delayed union, non-union, and nail breakage remain significant challenges in clinical practice. This case highlights several key factors contributing to these complications, as well as the surgical strategies employed to address them [4]. The patient’s history of congenital tibia shortening, coupled with multiple prior surgeries and smoking history, presented a complex clinical scenario. Initial external fixator-assisted lengthening procedures, while achieving limb equalization at earlier stages, likely predisposed the patient to further complications such as tibial fracture and deformity recurrence [7]. Subsequent interventions, including internal fixation with a plate, addressed immediate mechanical stability but failed to prevent progressive deformity. By the time, the patient presented to our clinic, significant genu valgum deformity and limb length discrepancy had developed, necessitating a comprehensive surgical approach. The use of a magnetic intramedullary nail provided a less invasive solution for deformity correction and further lengthening. However, delayed union during the consolidation phase raised concerns regarding compromised bone healing capacity, potentially related to the patient’s history of multiple prior surgeries, smoking, and altered bone biology. Smoking, a well-documented risk factor for impaired bone healing, was identified as a likely contributor [6]. In addition, smoking is associated with higher rates of nonunion and deep surgical site infections after fracture treatment [5]. This prompted additional interventions, including stem cell injection and iliac crest autograft placement, both of which are recognized as effective adjuncts in managing delayed union and non-union. Despite these measures, the osteotomy site remained vulnerable to mechanical failure. The fracture of the magnetic nail represents a rare but critical complication. The mechanical design of these nails, including their telescopic structure and motorized components, makes them susceptible to failure under excessive stress [4]. In this case, patient-related factors such as incomplete adherence to weight-bearing precautions likely contributed to the nail’s failure. Radiographic findings revealed valgus deformity at the fracture site, emphasizing the importance of early detection and intervention in similar scenarios [8].
The revision surgery involved correction of the deformity and stabilization of the tibia using a lateral plate placed over the retained broken nail. The application of a broad plate spanning the fracture site ensured immediate mechanical stability, allowing the patient to begin rehabilitation under controlled conditions. This approach is consistent with literature recommendations for managing broken intramedullary nails, which emphasize the need for rigid fixation and careful postoperative monitoring [9]. The decision to keep the fractured magnetic nail in situ rather than removing it was based on several technical and biological considerations. First, the extraction of a broken intramedullary device is often technically challenging, particularly in the presence of incomplete consolidation, as removal may compromise the fragile regenerated bone and necessitate additional osteotomies or canal reaming, further increasing morbidity. Second, implant exchange with a new lengthening nail was not a viable option at this stage due to the insufficient bone healing, which would have required renewed distraction osteogenesis and prolonged treatment duration. Lastly and importantly, the retained nail continued to provide a degree of secondary stability despite its fracture, acting as a load-sharing internal splint. Augmenting the construct with a lateral locking plate allowed us to neutralize torsional and bending forces at the fracture site. This approach aimed to minimize surgical trauma while restoring mechanical stability through plate fixation. In contrast to previously reported cases in which broken magnetic nails were removed before definitive stabilization, our patient achieved satisfactory clinical and functional outcomes despite retaining the fractured nail [10,11]. At the 9-month follow-up, the LEFS score was 76/80 (95%), VAS scores were zero at rest and two during walking, and SF-12 PCS score was 52. These results are comparable to those reported in patients treated with intact PRECICE nails, suggesting that plate augmentation over a retained broken nail may be a viable salvage strategy in selected cases [12].
This case underscores several critical lessons for clinical practice. First, patient compliance with postoperative weight-bearing protocols is paramount, particularly in cases involving advanced implants such as magnetic nails. Second, the management of delayed union and non-union requires a multidisciplinary approach, incorporating both surgical and biological strategies. Finally, the mechanical limitations of magnetic nails, while rare, highlight the need for ongoing innovation in implant design to enhance their durability and reduce the risk of failure. Future research should focus on identifying predictive factors for mechanical failure in magnetic nails and developing targeted strategies to mitigate these risks. Biomechanical and finite analyses may help clarify load-sharing mechanisms and the mechanical behavior of plate-nail constructs in similar salvage scenarios.
This case report is limited by its single-case design and lack of a comparative salvage group, and the findings should be considered hypothesis-generating rather than definitive. Follow-up was restricted to the mid-term, and long-term implant behavior and durability of union remain unknown. Patient-specific factors, including prior surgeries, smoking history, and altered bone biology, may have influenced both nail failure and healing, limiting the reproducibility of outcomes in other clinical scenarios. No biomechanical analysis or advanced imaging was performed to objectively assess construct stability or regenerate quality, and rehabilitation compliance was not objectively quantified. Finally, plate fixation over a retained broken magnetic nail is a rarely reported salvage strategy with a limited evidence base and without support from large clinical series or guideline-based recommendations. As such, this implant-specific approach reflects the experience of a specialized center and should be interpreted with caution, being reserved for carefully selected cases rather than considered a standard treatment option.
Although rare, intramedullary nail fracture is a complication orthopedic surgeons should be prepared for when using intramedullary lengthening nails. Internal fixation with a locking plate without removing the intramedullary nail is a viable treatment option with satisfactory outcomes. Patient adherence to rehabilitation protocols and modifying risk factors like smoking is also important for any procedure to succeed. To reduce mechanical failures, improvements in implant design and durability are essential.
Plate fixation over a retained broken magnetic nail can successfully restore stability and achieve union, offering a practical salvage option when nail removal is high-risk.
References
- 1. Masci G, Palmacci O, Vitiello R, Bonfiglio N, Bocchi MB, Cipolloni V, et al. Limb lengthening with PRECICE magnetic nail in pediatric patients: A systematic review. World J Orthop 2021;12:575-83. [Google Scholar] [PubMed]
- 2. Landge V, Shabtai L, Gesheff M, Specht SC, Herzenberg JE. Patient satisfaction after limb lengthening with internal and external devices. J Surg Orthop Adv 2015;24:174-9. [Google Scholar] [PubMed]
- 3. Frost MW, Rahbek O, Iobst C, Bafor A, Duncan M, Kold S. Complications and risk factors of intramedullary bone lengthening nails: A retrospective multicenter cohort study of 314 FITBONE and PRECICE nails. Acta Orthop 2023;94:51-9. [Google Scholar] [PubMed]
- 4. Hlukha LP, Alrabai HM, Sax OC, Hammouda AI, McClure PK, Herzenberg JE. Mechanical failures in magnetic intramedullary lengthening nails. J Bone Joint Surg Am 2023;105:113-27. [Google Scholar] [PubMed]
- 5. Xu B, Anderson DB, Park ES, Chen L, Lee JH. The influence of smoking and alcohol on bone healing: Systematic review and meta-analysis of non-pathological fractures. EClinicalMedicine 2021;42:101179. [Google Scholar] [PubMed]
- 6. Patel RA, Wilson RF, Patel PA, Palmer RM. The effect of smoking on bone healing: A systematic review. Bone Joint Res 2013;2:102-11. [Google Scholar] [PubMed]
- 7. Hosny GA. Limb lengthening history, evolution, complications and current concepts. J Orthop Traumatol 2020;21:3. [Google Scholar] [PubMed]
- 8. Burton MG Jr., Moon JY, Roberts DW. Distal femur valgus deformity after rigid intramedullary nailing of adolescent femoral shaft fracture. J Am Acad Orthop Surg Glob Res Rev 2023;7:e22.00220. [Google Scholar] [PubMed]
- 9. Kashyap S, Ambade R, Landge S, Salwan A. Impact of surgical timing on fracture healing in tibial shaft injuries: A comparative review of intramedullary nailing techniques. Cureus 2024;16:e70978. [Google Scholar] [PubMed]
- 10. Hidden KA, Dahl MT, Ly TV. Management of a broken PRECICE femoral nail at an ununited distraction osteogenesis site: A case report. JBJS Case Connect 2020;10:e0267. [Google Scholar] [PubMed]
- 11. Alrabai HM. Breakage of a re-activated PRECICE® nail: A case report. Int J Surg Case Rep 2023;106:108182. [Google Scholar] [PubMed]
- 12. Laubscher M, Mitchell C, Timms A, Goodier D, Calder P. Outcomes following femoral lengthening: An initial comparison of the precice intramedullary lengthening nail and the LRS external fixator monorail system. Bone Joint J 2016;98-B:1382-8. [Google Scholar] [PubMed]