In the following article, the author has described a rare occurrence of osteochondroma of the dorsal spine.
Dr. Ankit Kumar, Department of Orthopaedics, Rehabilitation and Research Centre, Dr. S.N. Medical College and Associated Group of Hospitals, Jodhpur, Rajasthan - 342001, India. E-mail: drankitkumar9472@gmail.com
Introduction: Osteochondroma is the most common benign bone tumor, typically affecting the appendicular skeleton. Its occurrence in the spine, particularly the dorsal region, is rare. Although often asymptomatic, spinal osteochondromas can present with neurological symptoms when they compress adjacent neural elements. Early diagnosis and management are critical to prevent complications, including malignant transformation.
Case Report: We present the case of a 14-year-old female who reported a progressively enlarging, painless swelling over the upper left back for 6 months. Physical examination revealed a firm, non-tender, non-mobile mass measuring approximately 5 × 5 cm, without any associated neurological deficits. Magnetic resonance imaging suggested osteochondroma. There was no family history of similar complaints, ruling out hereditary multiple exostoses. The lesion was surgically excised en bloc, and the bony base was cleared using a nibbler to minimize recurrence. Histopathological analysis confirmed the diagnosis of osteochondroma. Post-operative recovery was uneventful, and the patient remained asymptomatic during follow-up.
Conclusion: Spinal osteochondroma, particularly in the dorsal spine, is a rare presentation. Although often clinically silent, progressive growth warrants surgical intervention to avoid potential complications. Gross total resection, including removal of the cartilage cap, is recommended to prevent recurrence and reduce the risk of malignant transformation. This case highlights the importance of clinical vigilance and imaging in diagnosing and managing atypical osteochondromas.
Keywords: Osteochondroma, axial skeleton, bone tumor, exostosis, dorsal spine.
Osteochondroma, also known as osteocartilaginous exostosis, is the most common benign bone tumor, primarily affecting the appendicular skeleton [1]. Osteochondromas arising from the spine are rare, accounting for a small subset of cases, and may present as solitary lesions or in association with hereditary multiple exostoses (HME) [2]. These tumors typically originate from the posterior column of the spine [3]. When these benign masses cause spinal cord compression, they can lead to neurological symptoms, such as weakness, paresthesia, myelopathy, radiculopathy, headache, and dizziness [4]. The cervical spine, particularly the C1-C2 region, is the most common site of spinal osteochondroma, followed by the thoracic and lumbar spine, likely due to the greater mobility of the cervical spine, which subjects the epiphyseal cartilage to increased stress and microtrauma [5]. Osteochondroma is a disease of growing bone, typically presenting in the second to third decade of life with a male predominance [6]. These tumors arise from endochondral ossification of remnants of the epiphyseal plate trapped beneath the periosteum [7]. Malignant transformation, usually into chondrosarcoma, occurs in approximately 1% of solitary osteochondromas and up to 10% of cases associated with HME [8].
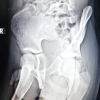
This is a case report of a young school-going 14-year-old female child who presented to the outpatient department with complaints of swelling over the upper back on the left side. The swelling was noticed first by her mother 6 months ago about 1 × 0.5 cm in size, when no treatment was taken. A plain radiograph in anteroposterior and lateral view was done to look for the swelling (Fig. 1).

Figure 1: Plain radiographs (Anteroposterior and lateral views) showing a mass protruding from the D8 vertebra (marked with arrows).
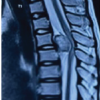
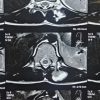
In the past 3 months, the swelling has increased to its current size 5 × 5 cm. The swelling is firm, non-mobile, globular in shape, smooth margins with normal overlying skin without any sinuses or scars. On physical examination patient had no local pain or neurological symptoms. Surgical excision of the mass was planned based on the magnetic resonance imaging (MRI) film and report (Figs. 2 and 3), which suspected it to be an osteochondroma. Patient does not have similar swellings at any other site or similar complaints in any family member.

Figure 2: Magnetic resonance imaging film (T2- weighted sagittal image) shows a well-defined, lobulated mass which is hypointense at the periphery with central hyperintensity arising from the posterior element of D8 vertebra. (marked with arrow).

Figure 3: Magnetic resonance imaging film (T2-weighted axial image) shows a well-defined lesion with heterogeneous intensity arising from the transverse process of D8 vertebra, causing compression of the spinal cord on the left side.
Surgical approach
After painting and draping, a skin incision was given directly over the swelling, after dissection (Fig. 4) mass was excised en bloc (Fig. 5) and sent for biopsy. The base was cleared thoroughly with a nibbler to prevent any remnant leading to increased risk of recurrence. No intraoperative neuro-monitoring was done as imaging revealed no canal compression, and the lesion was confined to the posterior elements without neurological deficits. The histopathologic examination was conclusive of bening osteochondroma showing features, such as cartilaginous cap and bony trabeculae with empty marrow spaces (Fig. 6).

Figure 4: Intra-operative image showing a well-defined, encapsulated shiny mass.

Figure 5: Gross specimen showing the en bloc resected mass.

Figure 6: Histopathological examination of the resected mass showing features of osteochondroma. (Marked arrow shows cartilaginous cap and star depicts the bony trabeculae with empty marrow space).
Follow-up
The patient was followed up for 2 years after the surgical procedure and showed complete post-operative recovery without any residual neurological symptoms and deficit. Patient also reported complete pain relief and a significant reduction on the Visual Analog Scale, where the pre-operative score being 5/10 and the post-operative score being 0/10. The resected specimen was sent for histopathology, which confirmed its benign nature, and subsequent post-operative radiographs were obtained at intervals till past follow-up showed no signs of regrowth of the mass or any similar mass elsewhere, thus ruling out malignancy.
Osteochondromas are the most common benign primary cartilaginous tumors in the appendicular skeleton [1]. They are considered hamartomas rather than true neoplasms due to their developmental origin [6]. These lesions develop through progressive endochondral bone formation within the periosteum, resulting from an epiphyseal growth disorder of the perichondral ring, with lateral displacement of a portion of the physis through the perichondral fibrous ring [7]. Osteochondromas can be solitary or multiple, the latter associated with HME, which has a strong positive family history and is inherited in an autosomal dominant pattern [2]. Osteochondroma of the spine is a rare phenomenon, and when present, it generally arises from the posterior column [3]. Plain radiographs can help establish the diagnosis, but computed tomography provides better delineation of the bony mass, while MRI aids in assessing the extent of soft tissue involvement [4,9]. Osteochondromas are typically treated with surgical excision and curettage, as performed by the author in this case report [5,10]. Gross total resection is generally curative and prevents recurrence, although malignant transformation should always be kept in mind in recurrent or rapidly enlarging lesions [8,11].
Osteochondroma of the dorsal spine is a rare occurrence, especially with neurological compromise, and is difficult to diagnose by clinical and radiologic examination. Gross total resection is advised of all diagnosed OC that involve the mobile spine because of the risk of local recurrence or malignant transformation. Osteochondroma causing neurological symptoms can be surgically addressed in most patients with a good expectation of functional recovery.
Although rare, osteochondromas can occur in the spine and may remain asymptomatic for long periods. A progressively enlarging spinal mass, even without neurological symptoms, warrants early imaging and intervention. Complete surgical excision is crucial to prevent recurrence and potential malignant transformation.
References
- 1. Dahlin DC, Unni KK. Bone Tumors: General Aspects and Data on 11,087 Cases. 5th ed. Springfield: Charles C Thomas; 1996. [Google Scholar] [PubMed]
- 2. Schmale GA, Conrad EU 3rd, Raskind WH. The natural history of hereditary multiple exostoses. J Bone Joint Surg Am 1994;76:986-92. [Google Scholar] [PubMed]
- 3. Lotfinia I, Vahedi P, Tubbs RS, Ghavame M, Meshkini A. Spinal osteochondroma: A review of 68 cases. J Neurosurg Spine 2010;12:581-90. [Google Scholar] [PubMed]
- 4. Khosla A, Martin DS, Awwad EE. The solitary intraspinal vertebral osteochondroma: Report of 10 cases. J Neurosurg 1999;90 1 Suppl:73-8. [Google Scholar] [PubMed]
- 5. Charest-Morin R, Boily M, Doyon D, Labelle H, Mac-Thiong JM. Spinal cord compression secondary to a solitary osteochondroma of the cervical spine. Spine J 2015;15:e9-15. [Google Scholar] [PubMed]
- 6. Bernard SA, Murphey MD, Flemming DJ, Kransdorf MJ. Improved differentiation of benign osteochondromas from secondary chondrosarcomas with imaging. Radiographics 2010;30:721-40. [Google Scholar] [PubMed]
- 7. Unni KK, Inwards CY. Dahlin’s Bone Tumors: General Aspects and Data on 10,165 Cases. 6th ed. Philadelphia, PA: Lippincott Williams and Wilkins; 2010. [Google Scholar] [PubMed]
- 8. Ahmed AR, Tan TS, Unni KK, Collins MS, Wenger DE, Sim FH. Secondary chondrosarcoma in osteochondroma: Report of 107 patients. Clin Orthop Relat Res 2003;411:193-206. [Google Scholar] [PubMed]
- 9. Kim NH, Park JY, Kim HJ. Solitary osteochondroma of the thoracic spine causing spinal cord compression. Yonsei Med J 2000;41:259-62. [Google Scholar] [PubMed]
- 10. Gille O, Pointillart V, Vital JM. Course of spinal solitary osteochondromas. Spine (Phila Pa 1976) 2005;30:E13-9. [Google Scholar] [PubMed]
- 11. Murphey MD, Choi JJ, Kransdorf MJ, Flemming DJ, Gannon FH. Imaging of osteochondroma: Variants and complications with radiologic-pathologic correlation. Radiographics 2000;20:1407-34. [Google Scholar] [PubMed]