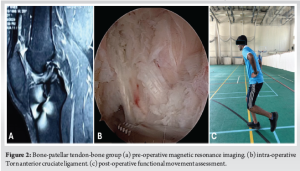
Peroneus longus graft provides an alternative to BPTB in revision case scenarios, especially in the developing world where the availability of allograft and cost are issues. This allows surgeons to have many graft options in revision anterior cruciate ligament reconstruction when already there is a limitation of graft options.
Dr. Vivek Kumar Gupta, Centre for Sports Science, Sri Ramachandra Institute of Higher Education and Research, Chennai, Tamil Nadu, India. E-mail: drvivekkumargupta1@gmail.com
Introduction: Due to the yearly rise in primary anterior cruciate ligament (ACL) reconstructions, revision ACL reconstruction is becoming more and more common in knee surgery. Choosing the appropriate graft and determining the surgical treatment staging by assessing the likelihood of doing the most anatomical revision canals and placing them with the primary canals before surgery are crucial factors affecting treatment outcomes.
Aim of the Study: The purpose of this study was to evaluate the differences in the patient-reported functional outcomes in revision ACL reconstruction using peroneus longus and bone-patellar tendon-bone (BTB) autografts in a single-stage revision ACL reconstruction.
Materials and Methods: Twenty-three patients who were eligible for follow-up among 25 surgeries performed between 2015 and 2023 were included in this retrospective analysis and met the inclusion criteria. The patient reported functional outcome, Lysholm knee score, Tegner activity level, and Visual Analog Scale (VAS) for pain before the injury and during the most recent follow-up. The peroneus longus (PL) and bone-patellar tendon-bone (BPTB) groups’ patient-reported results were assessed.
Results: There were no significant differences between the two revision groups with PL and BPTB autograft in terms of age, sex, duration between injury and surgery, concurrent injuries, and isolated or complex surgeries. There was not a significant difference between the groups’ pre-injury patient-reported outcomes, including the Lysholm knee score, Tegner activity, and VAS for pain (n.s.). There was not a significant difference in the two groups’ functional results at follow-up, although both groups’ functional outcomes improved and all patients recovered to their pre-injury activity level.
Conclusion: Overall, the findings suggest that graft options (peroneus longus and BTB) and surgical complexities (isolated and complex revision) yield comparable functional outcomes for most measures. However, notable differences in post-operative pain levels warrant further exploration. These results underscore the effectiveness of both graft types and surgical techniques in achieving satisfactory recovery while acknowledging the necessity of customized approaches to pain management based on individual patient circumstances.
Keywords: Autograft, anterior cruciate ligament, peroneus longus, revision, bone-patellar tendon-bone.
Retear rates following anterior cruciate ligament (ACL) surgery are correlated with several patient-related factors, including age, sex, and tibial slope; surgeon-related factors, including graft size, type, and tunnel placement; and additional factors, including activity level, concurrent injuries, and timing of return to sport [1, 2]. When planning a revision ACL reconstruction, the choice of graft is one of the most crucial factors. Although revision ACL reconstruction is common, there is not one universally accepted graft option. The chosen graft should ideally have structural and biomechanical properties that are comparable to those of the natural ligament and enable early, active rehabilitation. It should have reduced donor site morbidity, enabled quick biological integration, and enabled secure fixation [3, 4]. One of the most frequent reasons for revision ACL surgery is graft failure [5]. The choice of graft has an impact on functional results and graft failure [6]. As a result, choosing the right graft is an essential part of revising ACL reconstruction. Graft selection in the primary reconstruction of the ACL usually comes down to the surgeon’s preference, but in revision surgery, it depends on a number of variables, including the selected surgical approach, tunnel enlargement, and the type of graft utilized in primary surgery. Autograft harvest sites for primary and revision ACL reconstructions are currently available in a number of choices. For primary ACL reconstruction, the bone-patellar tendon-bone (BTB) and hamstring tendons (HT) are the most often used grafts. Nonetheless, the bone-patellar tendon graft and peroneus longus (PL) can be an extra beneficial option for revision surgery in the event of tunnel expansion or previously harvested grafts. Depending on the patient’s preference and the tissue utilized for the initial reconstruction, autologous grafts can be taken from the ipsilateral or contralateral limb. BTB and quadriceps tendon (QT) may not be suitable harvesting alternatives if there is substantial patellofemoral degeneration. The application of these grafts may worsen patellofemoral syndrome symptoms and cause weakening in the extensor mechanism after surgery. This could hinder the rehabilitation process and slow the patient’s recovery. Due to the increased trend of using HT graft in primary ACL reconstruction, the choice of graft for the revision ACL reconstruction is mostly limited to either bone-patellar tendon-bone (BPTB), PL, or QT. As mentioned above, the use of BPTB and QT grafts is limited in patients with patellofemoral degeneration. Hence, PL graft provides a good option for revising ACL reconstruction. The graft from the peroneus longus muscle’s half tendon, which was made using the GraftLink technique, ruptured at a force which is 1.8 times more than the graft from the semitendinosus muscle [7]. The tensile strength of the tendons of the hamstrings and peroneus longus is the same. However, the tensile strength of the peroneus longus tendon (PLT) is substantially higher than that of the patellar and QTs [8]. The PLT may be used as an autograft in ligament reconstruction surgeries because studies have demonstrated that it has no influence on walking disorders or ankle stability [9]. Shi et al., based on their experience, observed that the PLT is clinically effective in both width and length, with a diameter of 8–9 mm and a length of around 30 cm from the myotendinous junction to its insertion [10]. The authors are aware of no study yet that analyses the functional outcomes with PL and BPTB autograft in revision ACL reconstruction. Thus, the purpose of this study was to evaluate the variation in functional results as reported by patients following revision ACL surgery using PL and BPTB autografts.
This study was done at Sri Ramachandra Centre for Sports Sciences Chennai, AFC Centre for Excellence. Retrospectively, the collection of data was done from the center’s patient database. Patients were included in the study only if they fulfilled the required inclusion criteria which were age between 18 and 50 years, revision of ACL reconstruction with PL, and BPTB graft, with a minimum of 1-year follow-up. The exclusion criteria were multiligament reconstruction, use of other grafts than PL and BPTB, <1 year of follow-up, patients with concomitant bony injuries of the knee, and any other condition that will affect the normal follow-up for revision ACL. Similar protocols of pre-operative investigations were followed for all the patients. X-ray, computed tomography (CT) scan with 3D reconstruction, magnetic resonance imaging (MRI), and scanogram were done. 3D CT was specifically used to measure both tibial and femoral tunnel diameter and determine the femoral and tibial tunnel position, tunnel widening, and tunnel convergence. All the patients were operated on in a single-stage revision surgery. In cases in which the tunnel was in an anatomical location with not much widening, the same tunnels were used, and in cases with anatomical tunnels with dilation <12 mm, larger screws and thick grafts were used for a single-stage reconstruction. In cases with complete non-anatomical tunnels, new tunnels were created for revision. Cases with partial anatomical tunnels with or without enlargement were also considered for single-stage revision surgery. The most challenging examples were tunnel positions that were not entirely correct. Initially, a small tunnel was created and subsequently dilated using a dilator to prevent a significant bone defect and to retain the original graft that remained after this process. The same surgical procedures were used for all the cases irrespective of the grafts used. Meniscal damage and articular cartilage lesions were assessed, and if required, meniscal repair or meniscectomy, as well as cartilage lesion treatment (chondroplasty or microfracture) were carried out. We made every effort to protect the meniscus and maintain the stability of the knee joint. Two-strand PL tendon grafts were prepared and performed in conventional transportal femoral tunnel technique with no augmentation needed. For BPTB, a modified transtibial technique was used in which a tibial tunnel was used to make a femoral tunnel and graft passage. We used interference screws in the case of a BPTB on both the femoral and tibial side, whereas for PL, suspensory fixation was used on the femoral side, and interference screws on the tibial were used. Twenty-three patients (12 who received a PL and 11 who received a BPTB graft) who had revision ACL reconstruction between 2015 and 2023 matched the inclusion requirements. Each surgery was performed by senior arthroscopic surgeons. Patients were asked to complete the questionnaire based on their pre-injury status (shortly before the primary reconstructed ACL failed). Patients were also assessed for Lysholm knee score, Tegner activity level, and Visual Analog Scale (VAS) for discomfort during the follow-up period. Patient-reported outcomes were compared between the PL and BPTB groups. Patients who experienced graft failure were excluded from the follow-up outcome analysis. Similar post-operative protocols were followed in both groups’ early range of motion, preserving quadriceps function and increasing functional activities, whereas staying within the limits of the involved tissue-healing qualities are the main goals of rehabilitation. Limiting weight-bearing-to-toe contact and gradually increasing it as tolerated once quadriceps strength and function have returned is the best course of action [11]. When locked in extension, knee braces can enable early weight-bearing by stabilizing the knee until adequate quadriceps strength has returned [12].
Statistical analysis
Data analysis was performed using the software JAMOVI version 2.6.13. Descriptive statistics were calculated for continuous variables, including mean, median, and interquartile range (IQR). The Chi-square test was used for categorical variables. The Shapiro–Wilk test assessed normality, with the Mann–Whitney U test applied for non-normally distributed variables and the independent samples t-test for normally distributed data. For comparisons involving multiple groups, the Kruskal–Wallis H test was used. A P < 0.05 indicates statistical significance, ensuring valid and reliable conclusions.
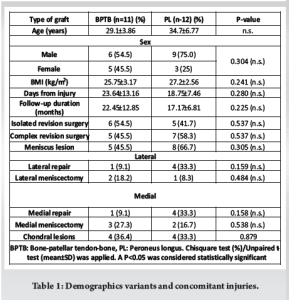
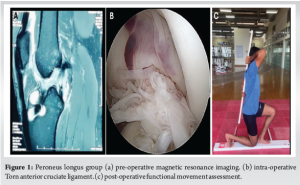
In terms of age distribution, the mean age for the PL group was 34.7 ± 6.77 years, whereas the BPTB group had a mean age of 29.1 ± 3.86 years. The age distribution did not reveal a statistically significant difference between the two groups, and the variation in sex distribution between the groups was not significant. Concerning body mass index (BMI), the mean BMI was slightly elevated in the PL group (27.2 ± 2.56 kg/m2) relative to the BPTB group (25.75 ± 3.17 kg/m2). These findings indicate that although some baseline characteristics differ, none of the comparisons achieved statistical significance, suggesting that the groups are well-matched regarding age, sex, and BMI. The time from injury to surgery was marginally shorter in the PL group (18.75 ± 7.46 days) compared to the BPTB group (23.64 ± 13.16 days). However, this difference did not reach statistical significance (P = 0.280). Similarly, the follow-up duration was shorter in the PL group (17.17 ± 6.81 months) than in the BPTB group (22.45 ± 12.85 months). However, this difference was also not statistically significant (P = 0.225). Overall, the results indicate that the follow-up characteristics between the two groups were largely comparable. In terms of isolated revision surgery, 5 patients (41.7%) in the PL group and 6 patients (54.5%) in the BPTB group underwent this procedure, with no statistically significant difference noted between the two groups (P = 0.537). Similarly, for complex revision surgery, 7 patients (58.3%) in the PL group and 5 patients (45.5%) in the BPTB group received this treatment, again revealing no statistically significant difference (P = 0.537). These findings indicate that the proportion of patients undergoing isolated or complex revision surgeries did not vary significantly between the PL and BPTB groups. With respect to medial meniscus lesions, 8 patients (66.7%) in the PL group and 5 patients (45.5%) in the BPTB group were found to have lesions. However, no statistically significant difference was noted (P = 0.305). In terms of medial meniscus meniscectomy, 2 patients (16.7%) in the PL group and 3 patients (27.3%) in the BPTB group underwent the procedure, with no significant difference detected (P = 0.538). Regarding medial meniscus repair, 4 patients (33.3%) in the PL group received the repair compared to just 1 patient (9.1%) in the BPTB group. However, this difference was not statistically significant (P = 0.158). Lateral meniscus meniscectomy was performed on 1 patient (8.3%) in the PL group and 2 patients (18.2%) in the BPTB group, again revealing no significant difference (P = 0.484). For lateral meniscus repair, 4 patients (33.3%) in the PL group underwent the procedure. In contrast, only 1 patient (9.1%) in the BPTB group did, with a P-value of 0.159 indicating no significant difference. Finally, chondral lesions were present in 4 patients (33.3%) in the PL group and 4 patients (36.4%) in the BPTB group, showing no significant difference (P = 0.879) (Table 1). Figs. 1 and 2 show pre-operative MRI, intra-operative torn ACL, and functional movement assessment post-operative for both groups, respectively.
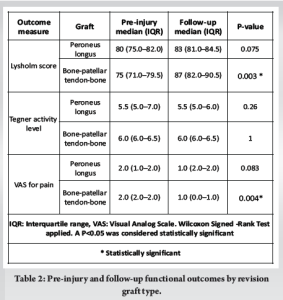
For the Lysholm score, the PL group improved from a pre-injury median of 80 (IQR: 75.0–82.0) to a follow-up median of 83 (IQR: 81.0–84.5). However, this improvement was not statistically significant (P = 0.075). In contrast, the BPTB group showed a significant increase from a pre-injury median of 75 (IQR: 71.0–79.5) to a follow-up median of 87 (IQR: 82.0–90.5), with a P = 0.003, indicating a notable enhancement in functional recovery for this group.
For the Tegner activity level, the PL group maintained a median of 5.5, with no significant difference between pre-injury (IQR: 5.0–7.0) and follow-up (IQR: 5.0–6.0) scores (P = 0.260). Similarly, the BPTB group retained a stable median of 6.0 (IQR: 6.0–6.5) across both time points, with a P = 1.000, reflecting no significant change in activity levels postoperatively. In terms of VAS for pain, the PL group demonstrated a reduction in median scores from 2.0 (IQR: 1.0–2.0) pre-injury to 1.0 (IQR: 2.0–2.0) postoperatively; however, this change did not reach statistical significance (P = 0.083). The BPTB group, on the other hand, experienced a significant decrease in pain levels, with median scores dropping from 2.0 (IQR: 2.0–2.0) pre-injury to 1.0 (IQR: 0.0–1.0) postoperatively (P = 0.004). In summary, both graft types improved functional outcomes and pain levels after revision ACL reconstruction. However, the BPTB graft group exhibited statistically significant improvements in Lysholm scores and pain reduction, suggesting it may offer superior post-operative recovery compared to the PL graft. Despite these differences, Tegner activity levels remained unchanged in both groups (Table 2).
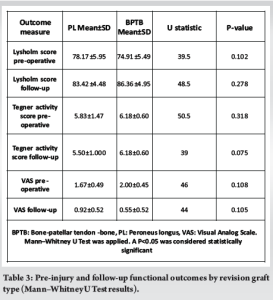
For the Lysholm score, the pre-injury scores were slightly higher in the PL group (78.17 ± 5.95) compared to the BPTB group (74.91 ± 5.49). However, this difference was not statistically significant (U = 39.50, P = 0.102). In follow-up, the BPTB group exhibited higher mean scores (86.36 ± 4.95) than the PL group (83.42 ± 4.48). However, this difference failed to reach statistical significance (U = 48.50, P = 0.278). For the Tegner activity score, pre-injury activity levels were comparable between the PL group (5.83 ± 1.47) and the BPTB group (6.18 ± 0.60), with no significant difference (U = 50.50, P = 0.318). Similarly, follow-up scores were higher in the BPTB group (6.18 ± 0.60) compared to the PL group (5.50 ± 1.00). However, the difference did not achieve statistical significance (U = 39.00, P = 0.075). Regarding VAS for pain, pre-injury pain scores were slightly lower in the PL group (1.67 ± 0.49) compared to the BPTB group (2.00 ± 0.45). However, this difference was not statistically significant (U = 46.00, P = 0.108). Follow-up pain levels also showed no significant difference, with mean scores of 0.92 ± 0.52 in the PL group and 0.55 ± 0.52 in the BPTB group (U = 44.00, P = 0.105) (Table 3).
The American Orthopedic Foot and Ankle Society (AOFAS) scale was used to evaluate the functional condition of the foot and ankle joints in the PL group. Pre-injury outcomes for all 12 patients were similar, at 99.00 ± 0.94 (97–100), and follow-up, at 99.21 ± 0.71 (98–100) (P = 0.919).
Overall, while both graft types resulted in improved functional outcomes and pain reduction postoperatively, the differences between the PL and BPTB groups were not statistically significant for any of the measures analyzed. These findings suggest that both grafts are comparably effective for revision ACL reconstruction.
This study’s key findings indicate that following ACL reconstruction revision, there was a notable improvement in patient-reported functional outcomes, as evidenced by the Lysholm knee score, Tegner activity level, and VAS for pain score across all groups. At the final follow-up, there was no difference in the functional outcomes between the two groups. The pre-injury activity level was regained by every patient. Revision ACL reconstruction is expected to become more prevalent as the annual rate of primary reconstructions rises, driven by the growing participation in athletic activities among individuals of all ages [13]. Outstanding outcomes following primary ACL reconstruction enable patients to engage in strenuous activities such as jumping, cutting, deceleration, and pivoting sports [14]. However, these activities significantly elevate the risk of re-injury, leading to a rise in the necessity for revision surgeries over the years [1]. Due to the patient’s lifestyle, level of education, and limited availability of synthetic or allograft, graft selections pose a challenge for both surgeons and patients, particularly in developing nations [15]. The anterior half, or the entire tendon of a PLT graft, has recently become a viable substitute for donor grafts. Although some surgeons are worried that PLT grafts impair ankle flexion and eversion, Kerimoğlu et al. observed that PLT grafting had little to no impact on foot and ankle function [16]. . also found no appreciable differences in ankle joint strength or range of motion between before and after the graft. Likewise, BPTB graft also has some stated complications such as anterior knee pain, but in a study done in our same institute with over 1250 patients undergoing BPTB graft, Janani et al. stated a similar incidence of anterior knee pain as in hamstring graft [17]. Every graft has its own benefits and limitations. Hence, this study was performed to compare both the graft options for revision ACL reconstruction. Alardi and Alsalman stated that PL auto graft represents a good graft option in revision ACL surgeries with no or little donor site morbidity [15]. Selcuk et al. concluded in their study that given its comparable clinical results, low donor site morbidity, and lower cost in ACLR revisions, particularly if the first ACLR was carried out utilizing grafts obtained around the knee, PL autograft may be a viable substitute for allografts [18]. Gofer et al., in their study, found that the results of an objective assessment between the revision ACL reconstruction with PL and primary ACL reconstruction with HT are comparable [19]. et al., in their other study with 36 RACL reconstruction cases with PL graft with one-stage, is a safe and successful surgical procedure that yields good objective and subjective clinical outcomes. When compared to HT autograft, the PLT autograft yields superior results [5]. Interestingly, the BPTB group showed a significant improvement from pre-injury to final follow-up. The BPTB group’s significantly higher Lysholm and VAS scores from pre-injury to final follow-up may have been caused, in part, by the patients’ somewhat younger ages (29.1 ± 3.86) as opposed to PL’s (34.7 ± 6.77). et al. [20] observed in their most recent study that the BPTB group had a significantly higher Lysholm score for revision ACL reconstruction than the HT group. Age, intensity of athletic activity, prior tunnel position, tunnel enlargement, graft used in initial ACL surgery, and surgeon preference are some of the variables that may limit the selection of graft for revision ACL reconstruction based on previously used grafts [21, 22]. Given that a single-stage revision operation is feasible with a bigger graft diameter, graft selection is particularly important in cases with a tunnel slightly off the anatomical position with or without enlargement. Because BPTB and PL autografts have a bigger diameter, they are better suited for this case. Graft failure is influenced by the choice of graft [6]. According to the multicenter ACL revision study, autografts are 2.78 times less likely than allografts to cause ACL reconstructive re-rupture [23]. In the same way, other meta-analyses found that autografts had a lower rate of graft failure than allografts [24, 25]. Autografts are, therefore, particularly advised for young, extremely demanding patients. Considering these findings, the current study solely employed autografts for ACL reconstructive revision. The data from recent studies indicate that the function of the foot and ankle joints is not significantly harmed by the use of PLT as an autograft for ACL reconstruction. Specifically, He et al.’s meta-analysis found statistically significant but non-meaningful differences between pre-operative and post-operative scores on the AOFAS scale (mean score decreased by 0.31; P = 0.01), and the results were comparable when measured by the foot and ankle disability index scale (mean difference of 0.02 points) [25]. Our study’s findings further demonstrate that there is no noticeable effect on ankle and foot function. In particular, the AOFAS score analysis revealed that the pre-operative and post-operative values were quite comparable (P = 0.919). In our present study, we did not find any significant differences in functional outcomes between the graft materials.
Limitation
The current study has many drawbacks. The initial and most significant issue is the limited sample size, which makes it underpowered to detect any differences in functional results. Revision ACL reconstruction compared to primary reconstruction, ACL reconstruction is less commonly done. Second, although all data were gathered prospectively, this research was retrospective in nature and used patient-reported subjective outcome measures. A prospective study that considers both subjective and objective scores should have to be carried out. Given the rising prevalence of revision ACL reconstruction and the need for surgeons to be knowledgeable about all available graft alternatives, the current study has clinical significance. In comparison to other grafts, PL autograft is the least researched and utilized graft, particularly for revision ACL reconstruction. When discussing the PL with patients, many surgeons do not even take it into consideration as a potential graft choice. There are still encouraging clinical findings on the feasibility of PL autograft in revision ACL surgery.
Patient-reported outcomes for revision ACL reconstruction were satisfactory for both autografts (peroneus longus and BTB). Because revision ACL surgery is becoming more common, surgeons should be knowledgeable about all the graft alternatives. When choosing grafts for revision ACL restoration, the results of this study will help the surgeons. Both grafts provided satisfactory outcomes.
Overall, this study highlights that both PL and BPTB grafts are viable options for revision ACL reconstruction, with the BPTB graft showing some advantages in terms of pain reduction and functional recovery. However, the choice of graft should be tailored to the individual patient’s needs and circumstances.
References
- 1.Erickson BJ, Cvetanovich GL, Frank RM, Rif AJ, Bach BR Jr. Revision ACL reconstruction: A critical analysis review. JBJS Rev 2017;5:e1. [Google Scholar]
- 2.Barié A, Ehmann Y, Jaber A, Huber J, Streich NA. Revision ACL reconstruction using quadriceps or hamstring autografts leads to similar results after 4 years: Good objective stability but low rate of return to pre-injury sport level. Knee Surg Sports Traumatol Arthrosc 2019;27:3527-35. [Google Scholar]
- 3.Miller SL, Gladstone JN. Graft selection in anterior cruciate ligament reconstruction. Orthop Clin North Am 2002;33:675-83. [Google Scholar]
- 4.West RV, Harner CD. Graft selection in anterior cruciate ligament reconstruction. J Am Acad Orthop Surg 2005;13:197-207. [Google Scholar]
- 5.Yumashev AV, Baltina TV, Babaskin DV. Outcomes after arthroscopic revision surgery for anterior cruciate ligament injuries. Acta Orthop 2021;92:443-7. [Google Scholar]
- 6.Grassi A, Nitri M, Moulton SG, Marcheggiani Muccioli GM, Bondi A, Romagnoli M, et al. Does the type of graft affect the outcome of revision anterior cruciate ligament reconstruction? A meta-analysis of 32 studies. Bone Joint J 2017;99:714-23. [Google Scholar]
- 7.Mikhaylov I, Puseva M, Balzhinimaev D, Semenov A, Verkhoturov V, Verkhoturova E. Comparative determination of the mechanical strength of the grafts models of the half of the peroneus longus tendon and the semitendinosus tendon (experimental study). Genij Ortopedii 2021;27:789-94. [Google Scholar]
- 8.Phatama KY, Hidayat M, Mustamsir E, Pradana AS, Dhananjaya B, Muhammad SI. Tensile strength comparison between hamstring tendon, patellar tendon, quadriceps tendon and peroneus longus tendon: A cadaver research. J Arthrosc Joint Surg 2019;6:114-6. [Google Scholar]
- 9.Buchanan CI, Marsh RL. Effects of exercise on the biomechanical, biochemical and structural properties of tendons. Comp Biochem Physiol A Mol Integr Physiol 2002;133:1101-7. [Google Scholar]
- 10.Shi FD, Hess DE, Zuo JZ, Liu SJ, Wang XC, Zhang Y, et al. Peroneus longus tendon autograft is a safe and effective alternative for anterior cruciate ligament reconstruction. J Knee Surg 2018;32:804-11. [Google Scholar]
- 11.Bedi A, Allen AA. Procedure 30: Revision anterior cruciate ligament reconstruction. In: Reider B, Terry MA, Provencher MT, editors. Operative Techniques: Sports Medicine Surgery. Philadelphia, PA: Saunders Elsevier; 2010. p. 487-514. [Google Scholar]
- 12.Anbari A, Bach BR. Revision anterior cruciate ligament reconstruction. In: Cole BJ, Sekiya JK, editors. Surgical Techniques of the Shoulder, Elbow, and Knee in Sports Medicine. Philadelphia, PA: Elsevier Saunders; 2008. p. 647-59. [Google Scholar]
- 13.Azar FM. Revision anterior cruciate ligament reconstruction. Instr Course Lect 2002;51:335-42. [Google Scholar]
- 14.D’Ambrosi R, Meena A, Raj A, Giorgino R, Ursino N, Mangiavini L, et al. Good results after treatment of RAMP lesions in association with ACL reconstruction: A systematic review. Knee Surg Sports Traumatol Arthrosc 2022;31:358-71. [Google Scholar]
- 15.Alardi IM, Alsalman IA. Peroneus tendon autograft in a revision anterior cruciate ligament reconstruction. Mod Med 2024;31:123-7. [Google Scholar]
- 16.Kerimoğlu S, Koşucu P, Livaoğlu M, Yükünç I, Turhan AU. Magnetic resonance imagination of the peroneus longus tendon after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 2009;17:35-9. [Google Scholar]
- 17.Janani G, Suresh P, Prakash A, Parthiban J, Anand K, Arumugam S. Anterior knee pain in ACL reconstruction with BPTB graft - is it a myth? Comparative outcome analysis with hamstring graft in 1,250 patients. J Orthop 2020;22:408-13. [Google Scholar]
- 18.Selcuk H, Baz AB, Egerci OF, Kose O. Peroneus longus tendon autograft versus allograft in revision ACLR: A retrospective comparison. Orthop Traumatol Surg Res 2024;110:103775. [Google Scholar]
- 19.Gofer AS, Alekperov AA, Gurazhev MB, Avdeev AK, Lukinov VL, Rubtsov DV, et al. Mid-term results of a single-stage revision anterior cruciate ligament reconstruction: A retrospective analysis of 36 cases. Traumatol Orthop Russia 2024;30:76-88. [Google Scholar]
- 20.Musahl V, Karlsson J. Anterior cruciate ligament tear. N Engl J Med 2019;380:2341-8. [Google Scholar]
- 21.Buerba RA, Boden SA, Lesniak B. Graft selection in contemporary anterior cruciate ligament reconstruction. J Am Acad Orthop Surg Glob Res Rev 2021;5:e21.00230. [Google Scholar]
- 22.MARS Group, Wright RW, Huston LJ, Haas AK, Allen CR, Anderson AF, et al. Predictors of clinical outcome following revision anterior cruciate ligament reconstruction. J Orthop Res 2020;38:1191-203. [Google Scholar]
- 23.Rahardja R, Zhu M, Love H, Clatworthy MG, Monk AP, Young SW. Factors associated with revision following anterior cruciate ligament reconstruction: A systematic review of registry data. Knee 2020;27:287-99. [Google Scholar]
- 24.Fan D, Ma J, Zhang L. Patellar tendon versus artificial grafts in anterior cruciate ligament reconstruction: A systematic review and meta-analysis. J Orthop Surg 2021;16:478. [Google Scholar]
- 25.He J, Tang Q, Ernst S, Linde MA, Smolinski P, Wu S, et al. Peroneus longus tendon autograft has functional outcomes comparable to hamstring tendon autograft for anterior cruciate ligament reconstruction: A systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc 2021;29:2869-79. [Google Scholar]