Minimally invasive posterior plating can be a safe and effective alternative for treating complex middle to distal 1/3rd highly comminuted humeral shaft fractures, prioritizing soft tissue and vascularity preservation with optimal functional recovery.
Dr. Shlok Patel, Department of Orthopedic Surgery, B.J Medical College, Ahmedabad - 380016, Gujarat, India. E-mail: pshlok27@gmail.com
Introduction: Humeral shaft fractures constitute 1–1.5% of all fractures, with most occurring in the middle and distal segments. While conservative treatment is common, surgical fixation is often preferred for displaced or comminuted fractures, particularly in young, active individuals. Minimally invasive plate osteosynthesis (MIPO) techniques have been developed to minimize soft-tissue damage and reduce the risks of complications such as non-union and radial nerve palsy. Although anterior approaches are well-studied, the posterior approach remains less explored. This case report highlights the use of a minimally invasive posterior approach similar to MIPO for treating a highly comminuted middle to distal 1/3rd humeral shaft fracture.
Case Report: A 25-year-old woman presented with a comminuted middle to distal one-third humeral shaft fracture after a fall. Due to the small size of the distal fragment, anterior plating was unfeasible. A conventional posterior incision from deltoid to lateral supracondylar ridge was made. A minimally invasive triceps split was done with minimal soft-tissue disruption. Radial neurovascular bundle was isolated and protected. An anatomical extra-articular plate was inserted via a submuscular tunnel, and four distal screws were fixed. The patient began early mobilization postoperatively, and at 5 months, X-rays confirmed fracture union, with full functional recovery of the left upper extremity.
Conclusion: This case demonstrates the successful use of a minimally invasive posterior approach albeit with a conventional posterior incision for distal comminuted humeral fractures. Comparable to the MIPO technique, this technique prioritizes the preservation of soft-tissue envelope around the fracture fragments, blood supply, and muscle integrity, resulting in favorable outcomes and minimal complications. It supports minimally invasive posterior techniques as a safe and effective alternative for complex distal humeral fractures, warranting further research into its long-term outcomes.
Keywords: Minimally invasive plating osteosynthesis, minimally invasive, humeral shaft fractures, comminuted, middle to distal one-third, posterior approach.
Of all the fractures, humeral fractures constitute 3–5% with shaft fractures accounting for 1–1.5% [1-3]. Majority of the shaft fractures are located in the middle and lower segments [3]. Although humeral shaft fractures are primarily managed conservatively, operative treatment is generally preferred in most displaced or comminuted fractures, especially in young, active patients. Operative management is associated with a lower risk of non-union and early functional gains [4]. Commonly used techniques include conventional open plate fixation and intramedullary nailing (IMN) [1,2]. Conventional open reduction and fixation involves soft-tissue stripping and disruption of periosteal circulation, caused by extensive surgical exposure, resulting in a wide array of complications. Most commonly non-union and infrequently secondary radial nerve palsy or infection may occur [5]. Despite the emphasis on the protection of the radial nerve during conventional surgery, the incidence of post-operative lesion is 5.1–17% [1]. Minimally invasive plate osteosynthesis (MIPO) offers a viable alternative with a lesser risk of non-union and secondary radial nerve palsy by mitigating the need for extensive soft-tissue stripping [3,5]. Minimally invasive procedures utilizing anterior and lateral approaches for the treatment of humeral shaft fractures have been widely described [6-10]. These approaches offer excellent access to the fracture site due to the relatively flat surface of anterior humerus and the radial nerve’s course along the posterior, medial, and lateral aspects of the bone. There is a paucity of literature on minimally invasive posterior approach, which has proven to be useful for distal two-thirds comminuted shaft fractures [11]. The purpose of this case report is to validate the efficacy of a minimally invasive technique similar to MIPO, utilizing an anatomic extra-articular plate via the posterior approach for treating a highly comminuted humeral shaft fracture from the mid-shaft to the distal one-fourth. Secondary objective of this report is to analyze the functional and radiological outcomes of this procedure.
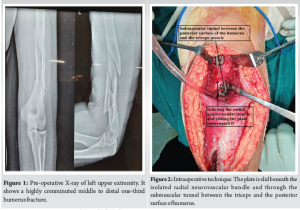
A 25-year-old woman presented to our hospital with a left humeral mid to distal 1/3rd long segmental comminuted shaft fracture 4 days following a fall from a two-wheeler vehicle. Patient had her left upper extremity casted elsewhere before the visit. On local examination, there was swelling distally, tenderness at the fracture site, and pain around the lower arm. Examination did not reveal any radial nerve palsy. Her X-ray (Fig. 1) showed severely comminuted segmental fracture of the middle to distal one-third left humerus with relatively preserved alignment and no gross displacement. The distal fragment measured approximately 5 cm, which won’t allow two screws of 4.5 locking compression plate, making anterior bridge plating unfeasible. Due to the patient’s preference for definitive surgical fixation, she was admitted, and her pre-operative workup was performed. On the 5th day following injury, she was scheduled for a procedure.
Operative note
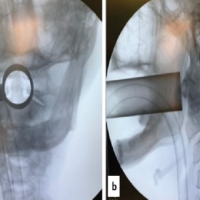
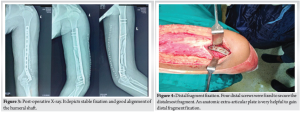
Patient was operated under brachial block and sedation. She was placed in the right lateral decubitus position with elbow support such that the forearm was dangling free, and the elbow was in 90° flexion. Overall reduction with mild traction was checked by the C-arm in anteroposterior and lateral views. A posterior midline incision proximally from the level of deltoid insertion to distally along the lateral supracondylar ridge (approx 18–20 cm long) was made. Skin, subcutaneous tissue, and deep fascia were cut to expose the triceps muscle, and hemostasis was achieved. Proximally, the interval between lateral and long head of triceps was identified and dissected to find the radial nerve with its vena comitans and profunda brachii artery (Fig. 2). The entire neurovascular bundle with its sheath was elevated from the posterior surface of the humerus using a blunt and curved periosteal elevator. Distally, the triceps were split along the lateral pillar of distal humerus. Olecranon fossa was identified. With a blunt and narrow periosteal elevator, a submuscular tunnel between the posterior surface of the humerus and the triceps muscle was created very carefully so as not to displace any of the comminuted fragments. Extra-articular anatomical titanium 3.5 mm, 10-hole plate specific for the left side was slid in the tunnel underneath the radial neurovascular bundle under fluoroscopic guidance. With mild traction, acceptable reduction was achieved and confirmed under image-intensifying television with both views. Preliminary K-wires through the plate and a 3.5 mm cortex screw proximally and distally were fixed. Reduction was again confirmed and further locking screws were fixed. A total of 7 screws (3 proximal and 4 distal) were fixed and stability in flexion, extension as well as varus, and valgus was confirmed. Normal saline wash, meticulous hemostasis, and muscle closure with 1–0 vicryl was done (Fig. 3). This was followed by subcutaneous and skin closure in layers. Sterile well-padded dressing was applied, and the arm was immobilized in a pouch arm sling. Post-operative X-ray is shown in Fig. 4.
Discharge and follow-up
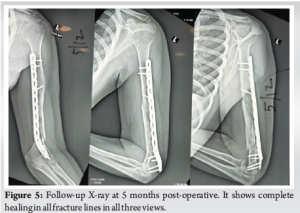
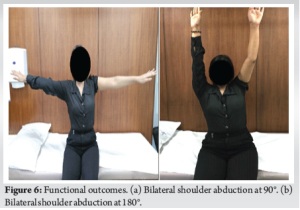
Gentle elbow range of motion exercises was initiated the next day, and the patient was encouraged to move with the sling. After 48 h post-operative, dressings were changed, and the patient was discharged. Patient was advised stitch removal on the 20th day and follow-up at 6 weeks. Patient did not follow-up until 5 months later as she lived in a small village and travel was difficult for her. She reported starting normal use of the left upper extremity by 6 weeks and full resumption of all activities by 3 months. She never underwent physiotherapy, and no follow-up X-rays were performed up to 5 months. She visited us at 5 months post-operative due to concern for hypertrophic scar. Her follow-up X-ray (Fig. 5) showed complete healing in all fracture lines in three views and clinical examination revealed full function of shoulder, elbow, wrist, and hand (Fig. 6a and b). There was only mild scar tenderness for which she was referred to plastic surgery.
Posterior approach, which is the workhorse for plating in the middle and lower third humerus, is also an extensile approach which involves significant damage to the triceps. When such an approach is used for comminuted fractures and multiple interfragmentary screws are planned, it involves extensive soft-tissue stripping which interferes with the vascularity of bone fragments and ultimately fracture healing. By avoiding this dissection and splitting the triceps along the full length, the vascularity is preserved, bone healing is enhanced, and principles of biological plate fixation are followed. In our procedure, the skin incision is like conventional plate fixation, but the muscle dissection and soft-tissue stripping are minimized. Depending on the degree of comminution and feasibility of interfragmentary screw fixation, a varying degree of muscle split and soft-tissue dissection can be utilized. This approach can also be useful for a combined supra + intercondylar fracture with shaft humerus fracture, albeit with different implant combinations. Our method is primarily based on the MIPO technique, although the incision is longer and similar to the conventional fixation. It is to keep the option of conventional plate fixation open in case deemed necessary. However, we also recommend two small incisions as employed by Krupko et al. and Gallucci et al., who utilized a similar minimally invasive technique with a posterior approach to fix distal humeral fractures. The incision can be lengthened in case further dissection is required. At present, open reduction and plate fixation are the gold standard management for unstable and displaced humeral shaft fractures. Recently, MIPO techniques have also yielded encouraging results. Primary goal of MIPO, a surgical technique involving small incision, closed reduction, or mini-open reduction, that minimizes soft-tissue dissection and helps preserve the periosteal blood supply, is to achieve bony union with minimal damage to vascularity and the best possible functional outcomes. A study on humeral shaft fractures by Esmailiejah et al., concluded a shorter union time, lesser complication rate, and comparable functional and clinical outcomes with MIPO compared to open reduction and internal fixation [12]. A meta-analysis of eight articles (391 patients) was unable to find any significant difference between MIPO and conventional fixation (IMN and open reduction and plate osteosynthesis [ORPO]) in terms of operative time, fracture union rate, and fracture union time. However, it concluded that MIPO has a lesser rate of complications and iatrogenic radial nerve palsy than ORPO, and higher adjacent joint function scores than IMN [5]. Majority of the research on the outcomes of MIPO focuses on the anterior approach. However, if the fracture is within 6 cm of the olecranon fossa, the anterior approach is impractical as there is not enough space for the minimum two screw hold in the distal fragment [9]. In such cases, the posterior approach MIPO may be effective by reducing blood loss and preserving the triceps. It allows the fixation of very small distal fragments with anatomically curved humerus extra-articular plates which allow distal most screws just above the elbow joint (Fig. 5). Unlike the anterior approach, it requires radial nerve dissection, increasing the risk of radial nerve palsy. A few studies [1,2,11,13] have discovered evidence in favor of the posterior approach MIPO over conventional plate fixation. In 2014, Balam and Zahrany reported 37 patients who underwent posterior MIPO for type B and C humeral diaphyseal fractures [13]. Radiological union was achieved in 35 patients by 16–21 weeks, while 2 required one session of extracorporeal shock-wave therapy for healing of delayed union. Four patients had residual varus deformity, and two patients developed post-operative radial nerve palsy which resolved in 8 weeks [13]. In 2015, Gallucci et al. reported a retrospective study of 21 patients with distal third of humerus fractures that were treated with MIPO through the posterior approach. All patients achieved fracture union, although varus deformity was noted in 16 of them [2]. Only one patient developed radial nerve palsy, which resolved 6 weeks after surgery [2]. Krupko et al. demonstrated a surgical technique utilizing MIPO with posterior approach for an 18-year-old patient with meta-diaphyseal comminuted fracture, although follow-up data was not reported [11]. In this case, a fracture with multiple fragments, which otherwise would take much longer to heal, showed radiological union, X-ray with perfect alignment, and full functional outcomes at 5 months post-operative. Subsequently, we emphasize on the efficacy of posterior plating with a minimally invasive technique and advocate the utility of the same for the treatment of distal comminuted fractures of the humeral shaft. We further contribute to the limited evidence supporting the safe use of the minimally invasive posterior approach for distal comminuted humeral shaft fractures and highlight the need for more large-scale randomized controlled trials and observational studies to better evaluate its outcomes and associated complications.
Distal highly comminuted humeral shaft fractures near the olecranon fossa cannot be treated by anterior MIPO. This study demonstrates the successful use of a minimally invasive posterior approach for such fractures. The technique preserves soft-tissue, vascularity, and musculature, thereby promoting fracture healing, improving functional outcomes, and minimizing complications. Although we used a conventional incision for the procedure, we also approve the utility of two small incisions and then lengthening it if minimally invasive is not possible. This report adds to the limited literature on minimally invasive posterior approaches, advocating for its safe use in managing complex distal humeral fractures and emphasizing the need for further studies to evaluate its long-term outcomes and safety.
A minimally invasive posterior approach for treating complex middle to distal one-third humeral shaft fractures is a viable and effective alternative to conventional methods. It allows for the preservation of soft-tissue, vascularity, and muscle integrity, which promotes fracture healing and minimizes complications such as non-union and radial nerve palsy. This technique can achieve favorable functional outcomes, especially in challenging fracture patterns where anterior approaches may be unsuitable.
References
- 1.Gallucci G, Boretto J, Vujovich A, Alfie V, Donndorff A, De Carli P. Posterior minimally invasive plate osteosynthesis for humeral shaft fractures. Tech Hand Up Extrem Surg 2014;18:25-30. [Google Scholar]
- 2.Gallucci GL, Boretto JG, Alfie VA, Donndorff A, De Carli P. Posterior minimally invasive plate osteosynthesis (MIPO) of distal third humeral shaft fractures with segmental isolation of the radial nerve. Chir Main 2015;34:221-6. [Google Scholar]
- 3.Cen C, Cao Y, Zhang Y, Hu C, Luo C. Preoperative position and protection of radial nerve by B-ultrasound combined with MIPPO for treatment of middle-inferior humerus fractures. J Orthop Surg Res 2022;17:260. [Google Scholar]
- 4.Stevens NM, Sgaglione MW, Ayres EW, Konda SR, Egol KA. A retrospective analysis of functional and radiographic outcomes of humeral shaft fractures treated operatively versus nonoperatively. JSES Int 2024;8:926-31. [Google Scholar]
- 5.Beeres FJ, Diwersi N, Houwert MR, Link BC, Heng M, Knobe M, et al. ORIF versus MIPO for humeral shaft fractures: A meta-analysis and systematic review of randomized clinical trials and observational studies. Injury 2021;52:653-63. [Google Scholar]
- 6.Shetty MS, Kumar MA, Sujay KT, Kini AR, Kanthi GK. Minimally invasive plate osteosynthesis for humerus diaphyseal fractures. Indian J Orthop 2011;45:520-6. [Google Scholar]
- 7.Concha JM, Sandoval A, Streubel PN. Minimally invasive plate osteosynthesis for humeral shaft fractures: Are results reproducible? Int Orthop 2010;34:1297-305. [Google Scholar]
- 8.López-Arévalo R, De Llano-Temboury AQ, Serrano-Montilla J, De Llano-Giménez EQ, Fernández-Medina JM. Treatment of diaphyseal humeral fractures with the minimally invasive percutaneous plate (MIPPO) technique: A cadaveric study and clinical results. J Orthop Trauma 2011;25:294-9. [Google Scholar]
- 9.Kobayashi M, Watanabe Y, Matsushita T. Early full range of shoulder and elbow motion is possible after minimally invasive plate osteosynthesis for humeral shaft fractures. J Orthop Trauma 2010;24:212-6. [Google Scholar]
- 10.Zhiquan A, Bingfang Z, Yeming W, Chi Z, Peiyan H. Minimally invasive plating osteosynthesis (MIPO) of middle and distal third humeral shaft fractures. J Orthop Trauma 2007;21:628-33. [Google Scholar]
- 11.Krupko T, Mayer R, Scott A, Aneja A, Moghadamian E. Minimally invasive plate osteosynthesis posterior approach to distal humeral shaft fractures-a surgical technique. J Orthop Trauma 2020;34:S5-6. [Google Scholar]
- 12.Esmailiejah AA, Abbasian MR, Safdari F, Ashoori K. Treatment of humeral shaft fractures: Minimally invasive plate osteosynthesis versus open reduction and internal fixation. Trauma Mon 2015;20:e26271. [Google Scholar]
- 13.Balam KM, Zahrany AS. Posterior percutaneous plating of the humerus. Eur J Orthop Surg Traumatol 2014;24:763-8. [Google Scholar]