Intra-articular corticosteroid injection of the small upper extremity joints can precipitate Central Serous Chorioretinopathy (CSC) and should be avoided in patients with known risk factors.
Dr. Monica Pecache Bagatsing, Christine M. Kleinert Institute for Hand and Microsurgery, Louisville, Kentucky. E-mail: monica.pecache@uoflhealth.org
Introduction: Central serous chorioretinopathy (CSC) is a chorioretinal disorder characterized by the accumulation of subretinal fluid and is often associated with corticosteroid exposure. While well-recognized in ophthalmology, awareness of CSC remains limited among musculoskeletal specialists, especially following intra-articular injection of the small joints of the upper extremity.
Case Report: We report the case of a 58-year-old female treated for left thumb carpometacarpal joint osteoarthritis. Following a second intra-articular injection of triamcinolone acetonide, she developed acute unilateral visual impairment. Ophthalmologic examination confirmed serous detachment of the neurosensory retina, leading to a diagnosis of CSC. The patient later revealed a history of a transient visual episode during a previous stressful period, suggesting a predisposition to the condition. The subretinal fluid resolved over 6 weeks with conservative management.
Conclusion: This case highlights the systemic risks of local corticosteroid injections. Even small doses used in small joint osteoarthritis can precipitate CSC, particularly in susceptible individuals. Clinicians should recognize this potential complication to ensure prompt diagnosis and appropriate counseling.
Keywords: Central serous chorioretinopathy, corticosteroid, thumb carpometacarpal joint, carpometacarpal joint, thumb carpometacarpal joint, osteoarthritis, corticosteroid injection.
Central serous chorioretinopathy (CSC) is an ocular condition characterized by the serous detachment of the neurosensory retina and has been associated with psychological stress, behavioral attributes, and corticosteroid administration [1]. The underlying pathophysiology involves choroidal thickening and congestion with altered blood flow and hyperpermeability leading to retinal degeneration with subretinal fluid accumulation and neurosensory detachment [1,2]. Clinically, patients present with blurred vision (typically unilaterally), metamorphopsia, micropsia, mild dyschromatopsia, and reduced contrast sensitivity, although some patients may be asymptomatic [3,4]. The association between CSC and endogenous hypercortisolism or exogenous corticosteroid administration is well-established in ophthalmologic literature and results from mineralocorticoid receptor-mediated effects on choroidal vasculature [1,5,6]. The development or recurrence of CSC can occur regardless of the route of corticosteroid uptake and has been reported with topical, intra-nasal, intra-articular, or systemic steroid use [5,7,8,9,10]. Unfortunately, awareness of this association remains sub-optimal among non-ophthalmologists and should be improved, especially among orthopedists, where corticosteroid injections are a cornerstone of non-operative management of osteoarthritis and other musculoskeletal conditions. Despite the widespread use of intra-articular corticosteroids, reports of CSC following musculoskeletal intra-articular or peri-articular injections remain sparse in orthopedic hand literature, with only a few cases described after large-joint injections in the knee and shoulder [8,9,10]. To our knowledge, CSC following intra-articular corticosteroid injection for thumb carpometacarpal joint (CMCJ) osteoarthritis has not previously been reported in the orthopedic case-report literature. In this report, we present a case of CSC after the administration of a corticosteroid injection for thumb CMCJ osteoarthritis and discuss its implications for clinicians who routinely use local corticosteroid therapy in the hand and upper extremity.
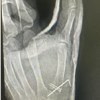
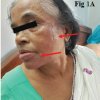
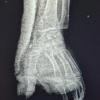
A 58-year-old right-hand-dominant female with a medical history of hypertension and hyperlipidemia presents with a 1-year history of progressive left thumb pain. The pain was aggravated by pinching and gripping, especially after a workday, and significantly limited her functionality. Clinical examination and radiographic imaging confirmed CMCJ osteoarthritis, and she was treated with an intra-articular corticosteroid injection consisting of 0.5 mg triamcinolone acetonide mixed with 0.5 mL lidocaine. She reported significant and sustained pain relief following this first injection. Unfortunately, the patient developed similar symptoms in her right thumb 6 months later, for which a second similarly dosed corticosteroid injection was administered. Two days after the second injection, she experienced sudden-onset unilateral visual disturbance in the left eye, described as a central gray spot obscuring her vision. She denied associated pain, flashes, or floaters. Ophthalmologic evaluation revealed serous detachment of the neurosensory retina in the macular region, and she was subsequently diagnosed with CSC secondary to corticosteroid injection. With conservative management and close monitoring, the subretinal fluid gradually resolved over six weeks, resulting in full visual recovery. Of note, following this episode, the patient recalled a prior episode of transient visual loss during a period of severe psychological stress; however, she had not previously considered it relevant to her osteoarthritis or corticosteroid treatment and thus did not disclose it to her orthopedic team.
CSC results from the accumulation of serous fluid under the neurosensory retina following choroidal hyperpermeability and dysfunction of the retinal pigment epithelium (RPE) and recent studies implicate CSC as part of the pachychoroid spectrum [1,11]. Multiple risk factors have been associated with the onset of CSC, including male sex (6:1 male-to-female ratio), middle-age, Type A personality trait, psychological stress, hypertension, and corticosteroid use [12,13,14]. Although our patient was female and slightly older than the typical demographic, she had hypertension and a history of significant psychological stress, both recognized contributors. The association between corticosteroid administration and CSC is well established and occurs likely from the induction of choroidal vasodilation and increased permeability while also impairing the RPE barrier function [5,6,7,12,14]. While systemic oral/intravenous corticosteroids are most commonly implicated, CSC has also been reported with inhaled, topical, peri-ocular, intra-vitreal, epidural, and intra-articular corticosteroid administration [5,7,8,9,10,14,15,16,17,18]. The risk of corticosteroid-associated CSC appears to be independent of the dose and duration of corticosteroid use, likely reflecting individual susceptibility related to choroidal and RPE biology rather than isolated pharmacokinetics [14]. Consequentially, even “local” corticosteroid formulations carry a rare but real risk of CSC due to systemic absorption [5]. Despite the commonplace use of intra-articular corticosteroids in musculoskeletal practice, CSC is rarely reported in orthopedic journals. Balakrishnan et al. described a 59-year-old female with bilateral CSC with blurring of her central vision 36 h following intra-articular corticosteroid injection into her knee [8]. Additional reports describe CSC after glenohumeral and other intra-articular corticosteroid injections [9,10]. Our case adds to this body of evidence by demonstrating that even small-joint steroid injections in the hand can be sufficient to trigger CSC in susceptible individuals. Thumb CMC osteoarthritis is a common source of hand disability. Intra-articular corticosteroids are often utilized following failure of relief with activity modification, splinting, occupational therapy, and oral analgesics. Injections are widely regarded as safe, with reported complications typically limited to local pain, infection, skin or fat atrophy, depigmentation, and very rarely tendon rupture or osteonecrosis [19,20]. Systemic adverse events are considered uncommon at the doses used for small joints. This case challenges the assumption that small-joint injections are free of systemic consequences. In a patient with hypertension, psychosocial stress, and a probable history of prior CSC, systemic absorption of triamcinolone from a thumb CMC injection appears to have been sufficient to precipitate acute CSC. Importantly, the temporal relationship (onset of visual symptoms within two days of injection) and the absence of alternative triggers support a possible causal link. Furthermore, the absence of ocular complications following the patient’s first injection demonstrates that prior tolerance to corticosteroids does not guarantee safety in subsequent administrations; the risk remains unpredictable and potentially cumulative. Given the recurrent nature of CSC and the risk of possible permanent damage, this has direct implications for treatment choices in patients with known CSC or strong risk factors. For these patients, clinicians should emphasize non-steroidal modalities or even earlier surgical consideration to avoid further steroid exposure unless the potential benefits clearly outweigh the ocular risks and the decision is made in close collaboration with the patient and the ophthalmology team.
This case highlights the importance of increased awareness among clinicians regarding the ocular complications of corticosteroid therapy. Patients with a history of CSC or identifiable risk factors should be counseled about these risks, and alternative treatment options should be considered whenever feasible. Given the potential for recurrence and long-term visual impairment, musculoskeletal specialists should recognize CSC as a possible adverse effect of intra-articular corticosteroid injections, even when administered into the small joints of the upper extremity.
Intra-articular corticosteroid injections, even in small joints of the upper extremity, can induce central serous chorioretinopathy (CSC), and musculoskeletal clinicians should counsel at-risk patients and avoid repeat steroid exposure after any visual disturbance.
References
- 1. Jain M, Mohan S, Van Dijk EH. Central serous chorioretinopathy: Pathophysiology, systemic associations, and a novel etiological classification. Taiwan J Ophthalmol 2022;12:381-93. [Google Scholar] [PubMed]
- 2. Bousquet E, Provost J, Torres-Villaros H, Behar-Cohen F. Central serous chorioretinopathy: A review. J Fr Ophtalmol 2023;46:791-802. [Google Scholar] [PubMed]
- 3. Semeraro F, Morescalchi F, Russo A, Gambicorti E, Pilotto A, Parmeggiani F, et al. Central Serous Chorioretinopathy: Pathogenesis and Management. Clin Ophthalmol 2019;13:2341-52. [Google Scholar] [PubMed]
- 4. Wang M, Munch IC, Hasler PW, Prünte C, Larsen M. Central serous chorioretinopathy. Acta Ophthalmol 2008;86:126-45. [Google Scholar] [PubMed]
- 5. Carvalho-Recchia CA, Yannuzzi LA, Negrão S, Spaide RF, Freund KB, Rodriguez-Coleman H, et al. Corticosteroids and central serous chorioretinopathy. Ophthalmology 2002;109:1834-7. [Google Scholar] [PubMed]
- 6. Zhao M, Célérier I, Bousquet E, Jeanny JC, Jonet L, Savoldelli M, et al. Mineralocorticoid receptor is involved in rat and human ocular chorioretinopathy. J Clin Invest 2012;122:2672-9. [Google Scholar] [PubMed]
- 7. Bouzas EA, Karadimas P, Pournaras CJ. Central serous chorioretinopathy and glucocorticoids. Surv Ophthalmol 2002;47:431-48. [Google Scholar] [PubMed]
- 8. Balakrishnan S, Apsingi S, Manjure SB. Sudden loss of visual acuity following intra-articular steroid injection in to the knee joint: A case report. Cases Rep 2008;1:428. [Google Scholar] [PubMed]
- 9. Mondal LK, Sarkar K, Datta H, Chatterjee PR. Acute bilateral central serous chorioretinopathy following intra-articular injection of corticosteroid. Indian J Ophthalmol 2005;53:132-4. [Google Scholar] [PubMed]
- 10. Hurvitz AP, Hodapp KL, Jadgchew J, Solomon DJ, Provencher MT, Stolldorf HS. Central serous chorioretinopathy resulting in altered vision and color perception after glenohumeral corticosteroid injection. Orthopedics 2009;32:600-2. [Google Scholar] [PubMed]
- 11. Nogueira HS, Arruda MP, Braga JP, Cardillo JA, Lima LH. Updated review of the pachychoroid spectrum and central serous chorioretinopathy. Rev Bras Oftalmol 2025;84 Suppl 3:ex0004. [Google Scholar] [PubMed]
- 12. Kaye R, Chandra S, Sheth J, Boon CJ, Sivaprasad S, Lotery A. Central serous chorioretinopathy: An update on risk factors, pathophysiology and imaging modalities. Prog Retin Eye Res 2020;79:100865. [Google Scholar] [PubMed]
- 13. Liu B, Deng T, Zhang J. Risk factors for central serous chorioretinopathy. Retina 2016;36:9-19. [Google Scholar] [PubMed]
- 14. Tsai DC, Chen SJ, Huang CC, Chou P, Chung CM, Chan WL, et al. Risk of central serous chorioretinopathy in adults prescribed oral corticosteroids: A population-based study in Taiwan. Retina 2014;34:1867-74. [Google Scholar] [PubMed]
- 15. Tliba A, Boussetta N, Metoui L, Gharsallah I, Ajili F, Louzir B, et al. Central serous chorioretinopathy secondary to epidural corticosteroid infiltration. Tunis Med 2016;94:166. [Google Scholar] [PubMed]
- 16. Kleinberger AJ, Patel C, Lieberman RM, Malkin BD. Bilateral central serous chorioretinopathy caused by intranasal corticosteroids: A case report and review of the literature. Laryngoscope 2011;121:2034-7. [Google Scholar] [PubMed]
- 17. Ricketti PA, Unkle DW, Cleri DJ, Prenner JL, Coluccielo M, Ricketti AJ. Central serous chorioretinopathy secondary to corticosteroids in patients with atopic disease. Allergy Asthma Proc 2015;36:123-9. [Google Scholar] [PubMed]
- 18. Chan LY, Adam RS, Adam DN. Localized topical steroid use and central serous retinopathy. J Dermatol Treat 2016;27:425-6. [Google Scholar] [PubMed]
- 19. Kamel SI, Rosas HG, Gorbachova T. Local and systemic side effects of corticosteroid injections for musculoskeletal indications. Am J Roentgenol 2024;222:e2330458. [Google Scholar] [PubMed]
- 20. Honcharuk E, Monica J. Complications associated with intra-articular and extra-articular corticosteroid injections. JBJS Rev 2016;4:e2. [Google Scholar] [PubMed]