A neglected locked patellar dislocation is a very rare injury which can be managed successfully by open reduction with careful release of all adhesions, derotation of patella and meticulous retinacular repair.
Dr. Sumedh D. Chaudhary,
Department of Orthopaedics, Indira Gandhi Government Medical College, Nagpur, Maharashtra, India.
E-mail: sumedhchaudhary@yahoo.com
Introduction: Dislocation of patella is a very common injury which usually reduces spontaneously or can be reduced easily using gentle manipulation. Irreducible patellar dislocations are rare and usually result due to either rotation of patella along the horizontal or vertical axis or due to bony impaction. Neglected locked patellar dislocations are extremely rare injuries presenting additional challenges.
Case Report: We are reporting a case of a 24-year female who presented to us 4 months after suffering a knee injury for which she received native treatment initially. On presentation, patient was able to walk with a limp and some discomfort but was unable to squat or sit cross-legged. Clinical examination revealed a patellar dislocation which was irreducible. On open reduction, the patella was found to be locked in the lateral gutter with rotation along its vertical axis and with an osteochondral fracture of its medial margin. There were a lot of fibrotic adhesions which required extensive release, following which the patella could be derotated and reduced into the trochlear groove. The medial retinaculum was repaired using transosseous sutures. Postoperatively, the patient developed wound edge necrosis which was managed with debridement and secondary suturing. At 1-year follow-up patient had almost full knee range of motion without any signs of patellar pain or instability and was able to squat and sit cross-legged.
Conclusion: Unlike acute irreducible patellar dislocations which can be managed easily with open reduction, a neglected dislocation necessitates wider surgical exposure and a lot of soft tissue releases, which may jeopardize vascularity of the soft tissues leading to wound healing problems. Release of all adhesions while taking care to prevent further chondral injury, adequate lateral retinacular release, derotation of patella to relocate it into trochlear groove, and meticulous medial retinacular repair is essential for a successful outcome.
Keywords: Irreducible, locked, neglected, patellar dislocation, proximal realignment.
Patellar dislocations are quite common and usually reduce spontaneously or can be reduced easily with simple manipulation maneuvers. Irreducible patellar dislocations are rare and mostly result due to either rotation of patella or due to impaction of bone [1]. Neglected trauma presents its own share of additional challenges. We report a rare case of a neglected locked patellar dislocation in a 24-year female.
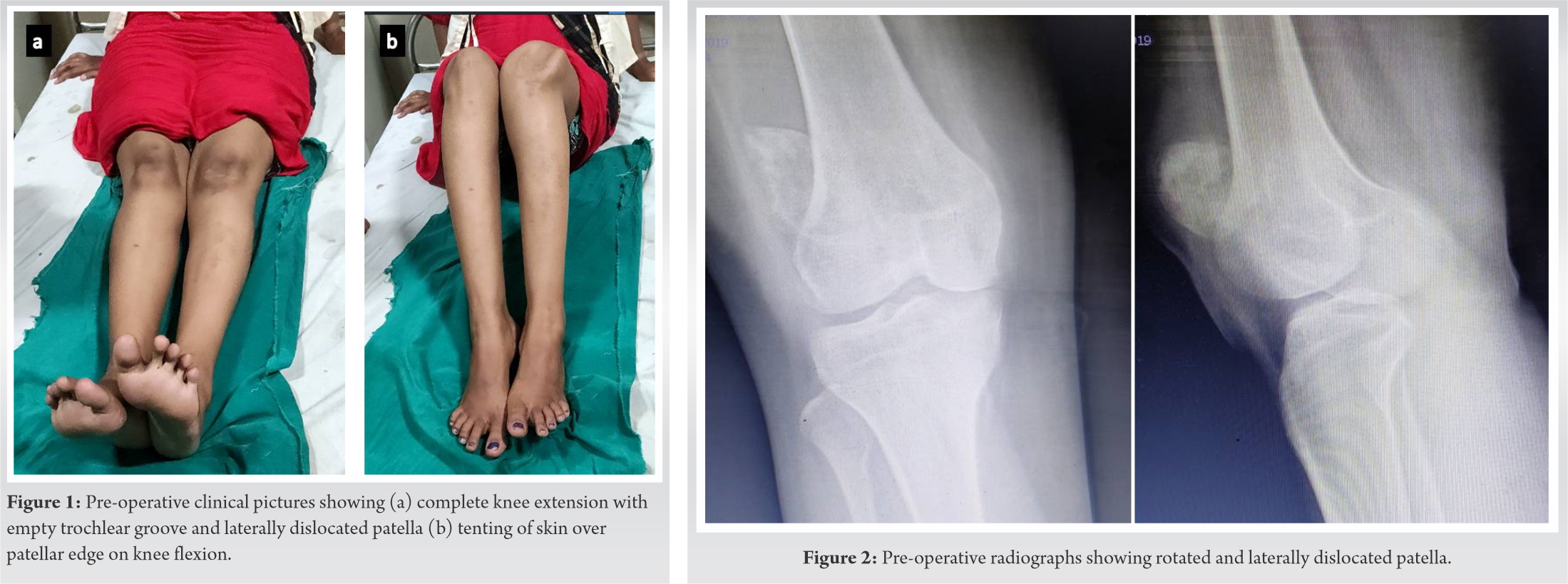
A 24-year female suffered a twisting injury to the left knee while walking on an uneven surface, following which she fell down and was unable to walk. She received some native treatment for 3 weeks, following which she was able to walk with a limp and some discomfort. However, she was not able to squat or sit cross-legged for which she presented to us 4 months later. Clinical examination revealed that the trochlear groove was empty and the patella was dislocated laterally with the anterior skin tenting over the patellar edge on knee flexion (Fig. 1). The patella was irreducible even on complete knee extension. The patient had an extensor lag of 20° with knee flexion up to 100°. She did not have any signs of generalized ligamentous laxity.
Radiographs revealed a laterally dislocated patella (Fig. 2).
Pre-operative magnetic resonance imaging revealed “focal disruption of the medial patellar retinaculum with lateral patellar dislocation and rotation of the patellar axis. Tibial tubercle-trochlear groove (TT-TG) distance was ~20 mm. Sulcus angle measured ~139°.” Since this was a neglected, locked patellar dislocation, open reduction was planned. The joint was exposed through a longitudinal, anterior midline skin incision. The patella could be felt in the lateral gutter. The soft tissue overlying the patella was incised, revealing that the patella had rotated by about 90° around its vertical axis with its articular surface facing laterally (Fig. 3a). There were a lot of adhesions which were carefully released before the patella could be derotated and reduced into place (Fig. 3b, c). The lateral femoral condyle showed a small indentation where the patella had keyed in (Fig. 3c). There was a small loose osteochondral fragment from the medial patellar border which was excised. The medial soft tissues were repaired to the medial border of patella through trans-osseous sutures. (Fig. 3d).
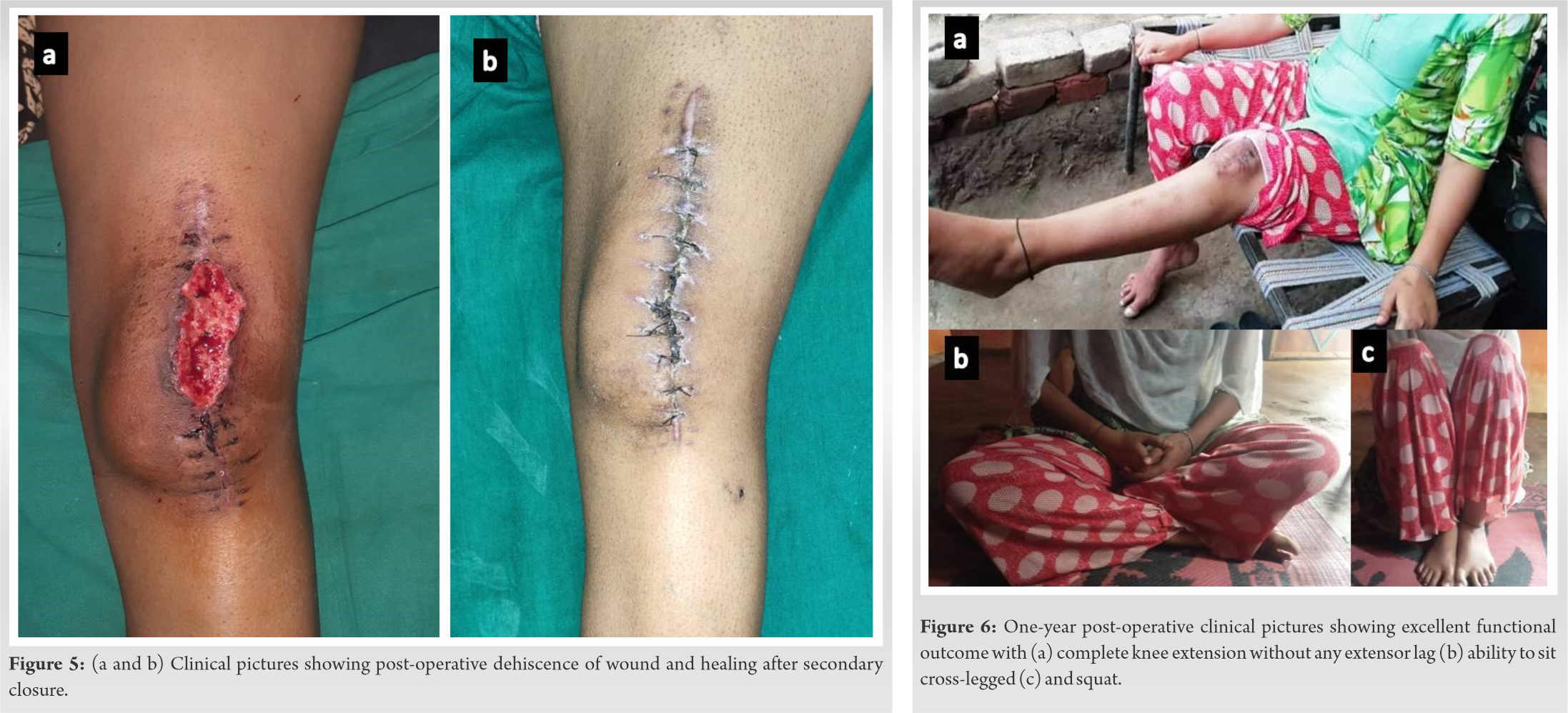
Lateral retinaculum which had been incised during the initial surgical exposure was repaired while taking care to avoid over-tightening of the lateral structures. Patella was tracking normally at the end of the procedure. Post-operative radiographs showed a well-relocated patella (Fig. 4). The patient was given a hinged knee brace with flexion allowed up to 70° for the first 3 weeks and mobilized full weight-bearing from the 2nd post-operative day. She was discharged on the 5th post-operative day with a healthy-looking wound. On her follow-up visit at post-operative 3 weeks, wound inspection revealed skin edge necrosis and dehiscence of the central part of the surgical wound (Fig. 5a). The patient was readmitted and underwent debridement of the wound followed by application of negative pressure wound therapy dressings to approximate the wound edges followed by secondary wound closure 5 days later. The wound healed well eventually (Fig. 5b).
The patient was followed up at regular intervals and regained complete knee flexion by 3 months. At her latest follow-up at 1-year post-operative, she is able to walk comfortably without any discomfort, is able to squat and sit cross-legged, and has complete knee extension without any extensor lag (Fig. 6).
Patellar dislocations are common and may result due to direct trauma to the medial side of the knee or due to indirect injury with forced internal rotation of the femur on externally rotated planted tibia while the knee is flexed [1, 2]. Adolescent patients, females, and athletes are more susceptible to this injury. Incompetent medial patellofemoral ligament, trochlear dysplasia, patella alta, lateralized tibial tubercle, or femorotibial malrotation may predispose to patellar instability [3]. Patellar dislocations may be intraarticular or extra-articular. Most patellar dislocations reduce spontaneously or can be reduced by manipulation with the knee in extension. Irreducible patellar dislocations are rare injuries and causes of irreducibility include rotation along the horizontal or vertical axes or impaction of patellar border into lateral femoral condyle [1]. The malrotated patella results in increased tension within the extensor mechanism, which in turn locks the patella in the lateral gutter and leads to irreducibility [2, 4]. Although closed manipulation can be attempted in acute cases, open reduction is recommended to reduce the risk of chondral damage by repeated attempts at manipulation and to repair or remove any osteochondral fractures [1]. Our patient suffered a non-traumatic patellar dislocation associated with an osteochondral fracture of the medial patellar border. With the knee in flexion, the raw fracture surface of the medial patellar border probably struck against the lateral femoral condyle causing the patella to rotate along its vertical axis by around 90°. Thus, both bony impaction as well as vertical rotation led to irreducibilty in our patient. As the patient belonged to a rural background, initially, she received native treatment and reported to us 4 months later with a neglected, locked patellar dislocation. Although missed patellar dislocations have been reported in patients having other skeletal injuries [5], isolated neglected locked patellar dislocations are extremely rare and to the best of author’s knowledge, only a few cases have been reported in literature till date. Gupta et al. reported a case of a 6-year-old boy who presented to them 2 months post-injury with the inability to flex the knee. During open reduction, the patella was seen to be rotated along the vertical axis and wedged lateral to the lateral femoral condyle. The patella was derotated, medial retinaculum was repaired, and lateral retinaculum was plicated, with full functional recovery [2]. Mittal et al. reported a 28-year male who presented to them 4 months post-injury with an intra-articular patellar dislocation with 180° rotation of the patella around its vertical axis within the intercondylar notch. Interestingly, this patient had full knee range of motion with only complaints of knee pain while climbing stairs. The authors found that there was a lot of fibrosis around the patella and trochlea which was carefully dissected and removed during open reduction [6]. Singhi et al. reported a 22 year male with a 4-year-old neglected patellar dislocation with a range of motion of 20–120° and complaints of painful knee range of motion affecting his activities of daily living. The patient had a Dejour grade D trochlear dysplasia and patella alta. The patient underwent diagnostic knee arthroscopy followed by open reduction of patella combined with proximal and distal realignment procedure. The authors mention that arthrolysis and adhesiolysis were required to mobilize the patella before reduction. Postoperatively patient developed a thyroid storm which settled with medical management. The patient also had delayed wound healing [7]. Irreducible patellar dislocations managed in the acute setting can be easily tackled with open reduction. Even arthroscopic reduction technique has been reported [8]. A neglected dislocation, however, presents additional problems as there is a lot of fibrosis which needs to be carefully removed, avoiding injury to the chondral surface. As has been observed by other authors [2, 6, 7] and also seen in our case, a lot of releases are required before the patella can be mobilized and relocated back into the trochlear groove. This may lead to soft tissue healing problems, as was seen in our case and also the case reported by Singhi et al. [7]. Our patient had an osteochondral fracture of the medial patellar margin which has also been reported by ElMaraghy et al and Hackl et al. [4, 9] Once the patella is relocated, medial retinacular structures need to be repaired meticulously to prevent re-dislocation. This can be achieved with bone anchors [9], sutures [10], or through trans osseous tunnels, as was done in our case. In non-traumatic dislocations, predisposing factors if any need to be evaluated and tackled. TT-TG distance more than 20 mm or patella alta (Caton-Deschamps index more than 1.2) are indications for a tibial tubercle osteotomy. Sulcus angle more than 145° indicates trochlear dysplasia and a deepening trochleoplasty is indicated in patients with severe trochlear dysplasia [3]. Our patient did not have any evidence of patella alta or severe trochlear dysplasia and hence did not require any additional procedures.
In summary, irreducible patellar dislocations are usually associated with malrotation or bony impingement and mostly need open reduction. Neglected dislocations pose more challenges and the increased soft tissue dissection necessitated may increase chances of soft tissue complications, as was seen in our patient. Careful dissection avoiding injury to the articular surface during relocation and proximal realignment to prevent patellar instability is the key to success in this rare injury.
Irreducibility of acute patellar dislocations should arouse the suspicion of rotation of patella along vertical or horizontal axis. Although closed reduction may be attempted, open reduction is preferable to avoid further injury to articular surface and to address associated injuries. Neglected dislocations require extensive soft tissue releases with an increased risk of soft tissue healing complications.
References
- 1.Grewal B, Elliott D, Daniele L, Reidy J. Irreducible lateral patellar dislocation: A case report and literature review. Ochsner J 2016;16:180-4. [Google Scholar]
- 2.Gupta RK, Gupta V, Sangwan SS, Kamboj P. Neglected locked vertical patellar dislocation. Indian J Orthop 2012;46:581-4. [Google Scholar]
- 3.Diduch DR, Kandil A, Burrus MT. Lateral patellar instability in the skeletally mature patient: Evaluation and surgical management. J Am Acad Orthop Surg 2018;26:429-39. [Google Scholar]
- 4.ElMaraghy AW, Berry GK, Kreder HJ. Irreducible Lateral patellar dislocation with vertical axis rotation: Case report and review of the literature. J Trauma 2002;53:131-2. [Google Scholar]
- 5.Elmadag M, Ceylan HH, Bilsel K, Acar MA. A case of neglected patella dislocation related to tibial plateau fracture. Bezmialem Sci 2014;1:39-42. [Google Scholar]
- 6.Mittal S, Arkesh M, Shankar V, Singh S, Sharma P, Mittal R. Patellar inversion: 180 degree rotation of the patella around its vertical axis within the intercondylar notch. Knee 2017;24:158-62. [Google Scholar]
- 7.Singhi PK, Raju S, Raghavakumar VP, Somashekar V. A case report of neglected patellar dislocation with postoperative complication of thyroid storm mimicking infection – A double whammy. J Arthrosc Joint Surg 2020;7:235-8. [Google Scholar]
- 8.Teixeira J, Gamba C, Ophuis J, Buijze GA, Kerkhoffs GM. Arthroscopic reduction of a locked patellar dislocation: A new less invasive technique. Knee Surg Sport Traumatol Arthrosc 2018;26:3706-10. [Google Scholar]
- 9.Hackl W, Benedetto KP, Fink C, Sailer R, Rieger M. Locked lateral patellar dislocation: A rare case of irreducible patellar dislocation requiring open reduction. Knee Surg Sports Traumatol Arthrosc 1999;7:352-5. [Google Scholar]
- 10.Devgan A, Rohilla R, Jain A, Mehta H, Singh S. Recurrent patellar instabilty culminating in a vertically rotated and a locked patellar dislocation – A rare entity. J Orthop Case Rep 2016;6:95-7. [Google Scholar]