Urgent/emergent surgeries in patients with active lice infestation may benefit from delaying lice treatment until after conclusion of operation, as pre-operative permethrin treatment may paradoxically and transiently augment locomotor activity and jeopardize sterility of surgical field.
Dr. Richard Casey Rice, 401 Glenwood Dr., Redlands, California, 92373, USA. E-mail: richardcrice@llu.edu
Introduction: Little is known about the perioperative management of Pediculus capitis (lice) infestations, including risk of contamination to the sterile field, whether to delay surgery, and optimal time to treat and/or operate.
Case Report: Two identical twin patients presented for elective in situ percutaneous pinning of chronic slipped capital femoral epiphyses. Active pediculosis capitis was noted intraoperatively by the anesthesia team during the first patient’s surgery. Meticulous examination of the sterile field at that time demonstrated no organisms or other sources of contamination. The second patient’s surgery was delayed to discuss her case with the infectious disease team. Scant literature exists to guide recommendations. Ultimately, a single permethrin treatment immediately before surgery was recommended and followed by our team. After careful prepping and draping, a louse was observed on the sterile field near the planned pin insertion site. The case was immediately canceled and delayed indefinitely. After two additional treatments over the next 4 days, only eggs (but no active insects) were observed in the patient’s hair. We elected to proceed to surgery at that time, which concluded without issue.
Conclusion: The surgical implications of an active lice infestation are numerous. Administration of antiparasitic medication in the immediate pre-operative period causes increased movement in pediculosis capitis, which may increase risk of sterile field contamination. Elective procedures should be postponed to complete multiple rounds of permethrin. In cases of urgent/emergent surgery, or in which treatment delay is unfeasible, foregoing delousing treatment in the immediate pre-operative period may be recommended.
Keywords: Lice, surgery, permethrin, pediculosis, orthopedics
Pediculosis, colloquially called “lice,” is an infestation of lice from the suborder Anoplura [1]. Many forms of pediculosis are described, however, the most commonly observed infestation is Pediculus humanus capitis, or head lice. Within the United States, pediculosis capitis is most prevalent among 3–12-year-old females, with an estimated incidence of 3% of infestation rate among school-aged children. The parasites are highly contagious and spread from direct head-to-head contact, where they are inadvertently transferred to a newly contacted host [2]. Adult lice lay eggs, which hatch lymphs (immature lice), and subsequently develop into adult lice. Lice obtain nutrients by piercing infected skin with their mouth apparatuses and secreting saliva that allows feeding on the hosts’ blood [1, 2]. Diagnosis is usually clinical with the identification of eggs and/or active parasites on the patient’s hair, follicles, or scalp. While no single treatment is shown to completely eradicate active pediculosis capitis, the most commonly employed treatment consists of permethrin lotion or shampoo, which is efficacious, cost-efficient, and readily available [3]. Permethrin is a pyrethroid insecticide used medically to treat scabies and lice infestations [4]. For pediculosis capitis, a single treatment of permethrin shampoo for 10 min is typically sufficient for eradication of the infestation. Despite the prevalence of pediculosis capitis within the United States, scant literature examines the surgical implications of operating on patients with active infestations. Intuitively, the notion that an infestation may increase the risk of disrupting the sterile surgical field is logical, however, there is no evidence to support this hypothesis. The only publication on perioperative lice management anecdotally suggests that surgery may be safe during an active infestation, and postulates that cases should not be delayed [5]. However, since little research exists, we hope to provide our perspective on the differential management of pediculosis capitis in identical twins undergoing elective hip pinning surgery, and, ultimately, offer therapeutic recommendations.
Two 11-year-old Caucasian twin sisters presented to the pediatric orthopedic surgery clinic for evaluation and management of chronic bilateral hip pain and antalgic gait. The limping in both patients was first noticed by their parents approximately 2 years before. At that time, patients sought medical attention from their pediatrician; however, the presentation of symptoms coincided with the peak of the COVID pandemic. Due to the inherent limitations of performing a comprehensive physical exam during a video appointment, the true etiology of the hip pain was not promptly identified. Interestingly, multiple studies have previously characterized this pandemic-related phenomenon and implicated it as a causal mediator of delayed care, diagnosis, and management in multiple fields of healthcare [6, 7, 8, 9, 10, 11]. Patient A was noted to have chronic, unilateral left slipped capital femoral epiphysis (SCFE), and Patient B was noted to have severe, chronic bilateral SCFE. The pathogenesis and treatment options for SCFE were discussed with the patients’ mother, who elected to proceed with percutaneous in situ fixation of the bilateral hips for both twin sisters. Patients A and B were admitted preoperatively the morning of the scheduled surgeries, and Patient A was taken to odds ratio (OR) as first case. Approximately 30 min into the surgery, an active Pediculus capitis infestation was noted by a member of the anesthesia team. Meticulous examination of the surgical field and incision site was performed in a comprehensive manner by all surgical providers, which demonstrated no insects on the sterile surgical field. The surgery was finished without complications, at which time, the sterile field was again carefully examined and noted to be without evidence of insect contamination. Although Patient B’s surgery was scheduled to follow Patient A’s, the decision to delay the case was unanimously agreed on after thorough discussion with patients’ mother, anesthesia, and surgical staff. Literature review performed jointly by both the pediatric infectious disease and orthopedics teams revealed a paucity of literature and recommendations regarding perioperative lice management.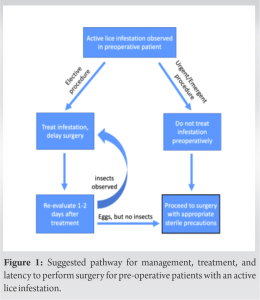
The importance of characterizing the perioperative risks and complications of lice infestations are vast and include both financial and professional implications. For example, lice are estimated to account for a potential 4–8 billion dollar annual loss to the US economy secondary to lost wages, daycare expenses, and healthcare-related costs, among many others [12, 13]. In addition, same day cancellations of pediatric outpatient surgeries impart a quantifiable emotional and economic burden on both patients and their parents [14]. Despite this financial burden, in addition to the seemingly common rates of infestation within the United States, scant literature examines the implications of performing surgery in a patient with active pediculosis capitis. This paradox might exist for several reasons; however, it is likely related to the difficulty in identifying and diagnosing pediculosis capitis, as 44.5% of patients are asymptomatic [15] and latency to diagnosis appears to correlate with infestation burden [16]. This notion is corroborated by the retrospective paper on lice, in which, active pediculosis capitis was first identified intraoperatively by the anesthesia staff in 4/9 cases, by the EMG technician in 4/9 cases, and preoperatively in only 1/9 cases [5], highlighting the challenging nature of (1) accurately diagnosing lice preoperatively and (2) studying the perioperative implications. Few studies have investigated the relationship between lice and perioperative complications. Sharma et al. reported an increased risk for peri-incisional wound infections secondary to pruritus in neurosurgical procedures on the scalp/head, which is unsurprising as these surgeries were performed on sites of active infestation [17]. In regards to surgeries performed on areas caudal to the head/neck, it is intuitive that an active infestation may increase the risk of disrupting the sterile surgical field; however, there is no prior evidence to support this notion. The only prior article examining the feasibility and safety of operating on patients with lice suggests that an active infestation may be a “lousy” reason to delay and/or cancel surgery for procedures, especially those involving the abdomen or lower back [5]. In this retrospective review, the authors highlighted the importance of weighing the pros and cons associated with canceling surgery, as there were no documented complications or morbidity from the cases diagnosed intraoperatively. In our two patients undergoing elective in situ hip pinning for SCFE, we observed a louse on the sterile field in the sister who was treated with permethrin shampoo an hour before surgery, but not in the untreated sister who was diagnosed intraoperatively. The authors of this paper hypothesize that the pre-operative administration of permethrin may have paradoxically mediated a transient increase in locomotor behavior of the insects. This effect was also likely magnified by the high infestation burden accumulated over the extended time period, the pediculosis had been left untreated. It also must be acknowledged that the difference in sterile field contamination between Patients A and B is observational in nature and may be coincidental. Unlike fleas or flies, lice are unable to jump or fly, and instead rely on crawling as their lone means of movement. They can be very active and are estimated to be able to crawl 23 cm/min [18]. Pyrethroids, such a permethrin, act as axonic excitotoxins by binding the hydrophilic interior of axonal sodium channels with high specificity, mediating irreversible channel opening [4]. Initially, this causes an immense sodium ion influx, causing depolarization, and the firing of an action potential. However, when the sodium channels remain open, the axon is unable to re-polarize ions across the axonal membrane, culminating in neuronal dysfunction and paralysis at the cellular and biomechanical levels, respectively. If administered in the immediate pre-operative period, the initial neuroexcitation of Pediculus humanus caused by permethrin may augment motor activity and drive behavioral patterns that increase risk of surgical field contamination. For this reason, and given lack of treatment precedent, we propose that: (1) Elective procedures be delayed until the patient has received at least one permethrin treatment, sufficient disinfestation has occurred, and careful scalp examination reveals no active parasites and (2) urgent/emergent cases, especially cases performed caudal to the head/neck that cannot be delayed without significant patient morbidity may proceed with the consideration of withholding permethrin treatment until after the conclusion of the surgery, to prevent permethrin-induced transient increase in parasite locomotion.
Despite the prevalence of pediculosis capitis among the pediatric population in the United States, only a small amount of literature has evaluated the surgical implications associated with operating during an active infestation. Only one study offers surgical recommendations concerning perioperative treatment, management, and latency from treatment to surgery. In this case report, Patient A was observed to have active pediculosis capitis ~ 45 min into the surgery; however, no insects were observed on the sterile field. Conversely, Patient B was diagnosed with, and consequently treated for, pediculosis capitis ~ 1 h before surgery, but insects were observed to contaminate the sterile field intraoperatively. Based on the differing pre-operative treatments and subsequent different outcomes in sterility, this paper provides recommendations regarding perioperative management of lice infestation and timing to surgery.
Little prior research has studied, characterized, or offered management strategies for latency to operate in surgical patients with active lice infestation. This is the first report that provides first-hand experience into the differential treatment of two twin sisters undergoing identical surgeries, and the implications those treatments ultimately mediated on maintaining surgical field sterility. Moreover, we offer the first management pathway that may help guide perioperative decision-making and treatment based on the urgency of the surgery.
References
- 1.Centers for Disease Control and Prevention. Parasites: Line-head Lice. Available from: https://www.cdc.gov/parasites/lice/head/epi.html [Last accessed on 2023 Apr 23]. [Google Scholar]
- 2.Bonilla DL, Kabeya H, Henn J, Kramer VL, Kosoy MY. Bartonella quintana in body lice and head lice from homeless persons, San Francisco, California, USA. Emerg Infect Dis 2009;15:912-5. [Google Scholar]
- 3.Frankowski BL, Bocchini JA Jr., Council on School Health and Committee on Infectious Diseases. Head lice. Pediatrics 2010;126:392-403. [Google Scholar]
- 4.Nanda J, Juergens AL. Permethrin. In: StatPearls. Treasure Island: StatPearls Publishing; 2023. p. 1-8. [Google Scholar]
- 5.Walker C, Sebastian R, Krishna S, Tobias JD. A lousy reason for surgery cancellations. Clin Pediatr (Phila) 2016;55:707-11. [Google Scholar]
- 6.Van Vliet ED, Eijkelboom AH, van Giessen A, Siesling S, de Wit GA. Physical and mental health outcomes of COVID-19 induced delay in oncological care: A systematic review. Front Oncol 2023;13:998940. [Google Scholar]
- 7.Jabbal IS, Sabbagh S, Dominguez B, Jtani M, Mohanna M, Samuel T, et al. Impact of COVID-19 on cancer-related care in the United States: An overview. Curr Oncol 2023;30:681-7. [Google Scholar]
- 8.Angelini M, Teglia F, Astolfi L, Casolari G, Boffetta P. Decrease of cancer diagnosis during COVID-19 pandemic: A systematic review and meta-analysis. Eur J Epidemiol 2023;38:31-8. [Google Scholar]
- 9.Khunti K, Aroda VR, Aschner P, Chan JC, Del Prato S, Hambling CE, et al. The impact of the COVID-19 pandemic on diabetes services: Planning for a global recovery. Lancet Diabetes Endocrinol 2022;10:890-900. [Google Scholar]
- 10.Amsah N, Md Isa Z, Ahmad N, Manaf MR. Impact of COVID-19 pandemic on healthcare utilization among patients with Type 2 diabetes mellitus: A systematic review. Int J Environ Res Public Health 2023;20:4577. [Google Scholar]
- 11.Ye Z, Chen H, Liu X, Wei G. Delayed care seeking and outcomes of testicular torsion among children during the COVID-19 pandemic: A systematic review and meta-analysis. Eur J Pediatr Surg 2022;e-pub ahead of print. [Google Scholar]
- 12.Hansen RC, O’Haver J. Economic considerations associated with Pediculus humanus capitis infestation. Clin Pediatr (Phila) 2004;43:523-7. [Google Scholar]
- 13.Mumcuoglu KY, Meinking TA, Burkhart CN, Burkhart CG. Head louse infestations: The “no nit” policy and its consequences. Int J Dermatol 2006;45:891-6. [Google Scholar]
- 14.Tait AR, Voepel-Lewis T, Munro HM, Gutstein HB, Reynolds PI. Cancellation of pediatric outpatient surgery: Economic and emotional implications for patients and their families. J Clin Anesth 1997;9:213-9. [Google Scholar]
- 15.Mumcuoglu KY, Klaus S, Kafka D, Teiler M, Miller J. Clinical observations related to head lice infestation. J Am Acad Dermatol 1991;25:248-51. [Google Scholar]
- 16.Pilger D, Khakban A, Heukelbach J, Feldmeier H. Self-diagnosis of active head lice infestation by individuals from an impoverished community: High sensitivity and specificity. Rev Inst Med Trop Sao Paulo 2008;50:121-2. [Google Scholar]
- 17.Sharma D, Kaliaperumal C, Choudhari KA. An overview of head lice infestation in neurosurgical patients. Br J Nurs 2007;16:982-6. [Google Scholar]
- 18.Burkhart CN. Fomite transmission with head lice: A continuing controversy. Lancet 2003;361:99-100. [Google Scholar]











