Recurrent soft-tissue swelling after limb surgery should arise the suspicion of arterial pseudoaneurysm.
Dr Gaurav Kumar Upadhyaya, Department of Orthopaedics, AIIMS, Raebareli, Uttar Pradesh, India. E-mail: drgkupadhyaya@yahoo.co.in
Introduction: Arterial pseudoaneurysm is a hematoma that is formed after damage to the arterial wall. We report a rare case of peroneal artery pseudoaneurysm after open reduction and internal fixation with interlocking nailing and partial fibulectomy for non-union for the right tibia in a 31-year-old male. The patient presented with a bleeding sinus over the leg swelling, and it was managed with an exploration of the pseudoaneurysm and ligation of the peroneal artery.
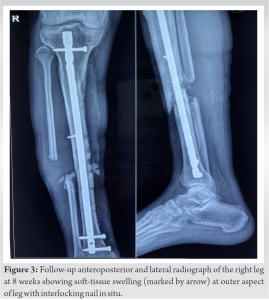
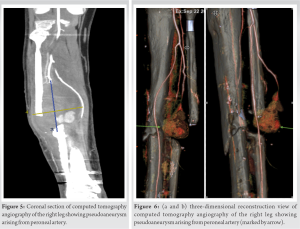
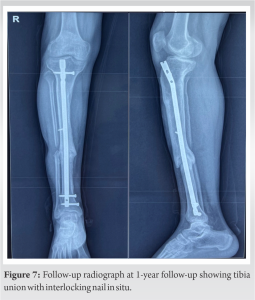
Case Report: A 30-year-old male patient presented with a non-union tibia on the right side and had undergone plating of the tibia at another institute for a fracture of both bone legs approximately 18 months ago. The revision surgery was performed in which a previously inserted implant was removed and an interlocking nail was inserted, along with a partial fibulectomy. The post-operative period was uneventful. At 8 weeks after the second surgery, the patient came with a complaint of swelling at the outer aspect of the right leg. Computed tomography and angiography confirmed a peroneal artery pseudoaneurysm of 3.2 × 2.8 × 3.8 cm. Pseudoaneurysm was explored, and the artery was overrun with a Figure-8 stitches using a monofilamentous, and non-absorbable suture.
Conclusion: This case report highlights the occurrence of pseudoaneurysm after an orthoapedic procedure such as a partial fibulectomy. A high level of clinical suspicion, proper imaging, and early endovascular or surgical intervention is recommended to prevent complications.
Keywords: Pseudoaneurysm, peroneal artery, partial fibulectomy.
Arterial pseudoaneurysm is a hematoma that is formed after damage to the arterial wall. The covering of pseudoaneurysm does not include all three layers of the arterial wall; instead, it is formed by the clotting products and surrounding tissue. Arterial pseudoaneurysm is formed either after trauma or infection. Trauma, either blunt or penetrating, may cause damage to the arterial wall and contribute to the formation of pseudoaneurysms [1,2]. Peroneal artery pseudoaneurysm is a rare entity. We report a rare case of peroneal artery pseudoaneurysm after open reduction, internal fixation with interlocking nailing, and partial fibulectomy for non-union of right, tibia in a 31-year-old male. The patient presented with a bleeding sinus over the leg swelling, and it was managed with an exploration of the pseudoaneurysm and ligation of the peroneal artery.
The patient, a healthy male in his early thirties, sustained a fracture of the right tibia and fibula, for which he underwent plating of the tibia at another institute. Following the non-union of the tibia, he sought a second opinion with us approximately 18 months after his index surgery. Radiographs confirmed the diagnosis of non-union of the right tibia with the plate in situ (Fig. 1).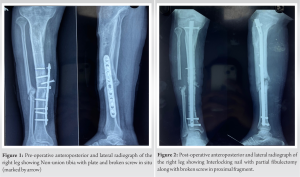

Review of Literature
On searching the English literature, 16 cases of traumatic pseudoaneurysm of the peroneal artery or perforating branches of the peroneal artery have been reported. However, only eight case reports out of those have proposed the cause of pseudoaneurysm of the peroneal artery or perforating branch of the peroneal artery as an iatrogenic injury during surgery [3-10] Table 1.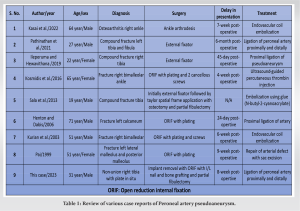
Doppler ultrasound, arteriography, CT angiography, and magnetic resonance imaging (MRI) can be used for diagnosing pseudoaneurysm. The Doppler study is the first line investigation to be performed for confirming the diagnosis. It has the advantage of being inexpensive, radiation-free, quick, portable, and non-invasive. However, the disadvantage is that it is operator-dependent and cannot provide three-dimensional images for assessment. CT angiography provides more information about the pseudoaneurysm but carries the risk of high radiation doses. Arteriography is an invasive investigation but has the advantage of being therapeutic in performing endovascular procedures. MRI is also an excellent investigation in providing the required anatomical details but is costly, time-consuming, and difficult to perform in the presence of metallic implants [4, 11, 12]. Various treatment modalities have been described in the literature, ranging from conservative ultrasound-guided thrombin injection to endovascular procedures such as coil/glue embolization or intraluminal stent placement, ligation of the artery, arterial repair, and arterial reconstruction [4, 6, 9, 11, 12, 13]. As the pseudoaneurysm is usually full of layers of clots, the size of the true cavity is often grossly underestimated on color on Doppler and angiograms. Open surgery provides the benefit of clot evacuation and the management of elements of local infection (if any) over endovascular procedures. Surgery for distal pseudoaneurysms carries low morbidity and mortality while remaining simple, expeditious, and curative. Pseudoaneurysms of vessels that may require laparotomy or thoracotomy or in moribund patients may benefit more from endovascular interventions.
This case report highlights the occurrence of a pseudoaneurysm after an orthopedic procedure such as a partial fibulectomy. Delayed presentation and non-specific complaints make it challenging to diagnose. A high level of clinical suspicion, proper imaging, and early endovascular or surgical intervention is recommended to prevent complications.
It is that high index of suspicion is required for the diagnosis of arterial pseudoaneurysm of peroneal artery after surgery involving the leg.
References
- 1.Kronzon I. Diagnosis and treatment of iatrogenic femoral artery pseudoaneurysm: A review. J Am Soc Echocardiogr 1997;10:236-45. [Google Scholar]
- 2.Sueyoshi E, Sakamoto I, Nakashima K, Minami K, Hayashi K. Visceral and peripheral arterial pseudoaneurysms. AJR Am J Roentgenol 2005;185:741-9. [Google Scholar]
- 3.Kasai T, Higashida T, Hayashi T, Yasui T. Pseudoaneurysm of the peroneal artery after ankle arthrodesis treated by endovascular coil embolization: A case report. JBJS Case Connect 2022;12(3):doi: 10.2106/JBJS.CC.22.00206. . [Google Scholar]
- 4.Pathinathan K, Sivakumaran D, Dimantha WH, Nishanthan AA, Chanaka KA, Munidasa D. Late-onset pseudoaneurysms of lower limb arteries following late complications of orthopaedic constructs-two cases and review of literature. Int J Surg Case Rep 2021;87:106457. [Google Scholar]
- 5.Ileperuma MR, Hewavithana B. Proximal peroneal artery traumatic pseudoaneurysm following a compound proximal tibial shaft fracture managed with an external fixator: A case report. J Orthop Trauma Rehabil 2020;27:89-92. [Google Scholar]
- 6.Kosmidis IA, Kourkoutas K, Stouki S, Flokatoula M. Pseudoaneurysm of the perforating peroneal artery after ankle fracture fixation: Case report and review of the literature. J Foot Ankle Surg 2016;55:1083-6. [Google Scholar]
- 7.Sala F, Salerno CF, Albisetti W. Pseudoaneurysm of the peroneal artery: An unusual complication of open docking site procedure in bone transport with taylor spatial frame. Musculoskelet Surg 2013;97:183-6. [Google Scholar]
- 8.Henton J, Dabis HS. Pseudoaneurysm of the peroneal artery following os calcis fixation. Inj Extra 2006;37:419-21. [Google Scholar]
- 9.Kurian J, Pillai SC, Chapple D, Frost RA. Pseudoaneurysm of peroneal artery following ankle fracture. Foot Ankle Surg 2003;9:233-5. [Google Scholar]
- 10.Pai VS. Traumatic aneurysm of the perforating peroneal artery following ankle fracture. J Foot Ankle Surg 1999;38:417-9. [Google Scholar]
- 11.Raherinantenaina F, Rajaonanahary TM, Ratsimba HN. Management of traumatic arterial pseudoaneurysms as a result of limb trauma. Formos J Surg 2016;49:89-100 [Google Scholar]
- 12.Luther A, Kumar A, Negi KN. Peripheral arterial pseudoaneurysms-a 10-year clinical study. Indian J Surg 2015;77 Suppl 2:603-7. [Google Scholar]
- 13.Gangadharan AN, Sekhar R, Bhanushali JP, Thusay PC. Pseudoaneurysm of posterior tibial artery management: Case report and review of literature. J Curr Surg 2015;5:209-12. [Google Scholar]











