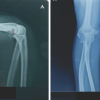
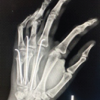
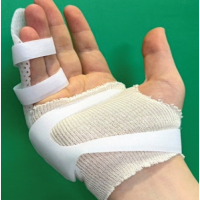
Intramedullary screw fixation provides stable, minimally invasive fixation for selected metacarpal and phalangeal fractures, enabling early mobilization and faster functional recovery.
Dr. Ranjeet Singh Sidar, Department of Orthopaedics, Gandhi Medical College, Bhopal, Madhya Pradesh, India. E-mail: ranjeet3817@gmail.com
Introduction: Hand fractures of the metacarpals and phalanges account for up to 10% of all skeletal injuries and can lead to significant functional impairment if not managed appropriately. Retrograde intramedullary headless screw (IMHS) fixation is a minimally invasive technique that promises stable fixation and early mobilization, but its clinical efficacy in a prospective setting warrants evaluation.
Materials and Methods: A prospective interventional study was conducted at tertiary care center from May 2023 to October 2024. Forty adult patients with simple, extra-articular metacarpal or phalanx fractures were enrolled; six were lost to follow-up, leaving 34 for analysis. Fractures were stabilized using retrograde IMHS fixation. Functional recovery was assessed at 3 weeks, 3 months, and 6 months postoperatively using the disabilities of the arm, shoulder and hand (DASH) score, hand grip strength, and total active motion (TAM) per American Society for Surgery of the Hand criteria.
Results: The mean patient age was 29.29 ± 8.52 years; 82.4% were male, and 52.9% had injuries in the dominant hand. Shaft fractures predominated (83.8%). (1) DASH score improved from 47.07 ± 7.29 at 3 weeks to 27.30 ± 2.59 at 3 months and 1.32 ± 1.51 at 6 months (all P < 0.001). (2) Grip strength increased from 11.09 ± 1.75 kg at 3 weeks to 24.38 ± 3.46 kg at 3 months and 39.74 ± 4.69 kg at 6 months (all P < 0.001). (3) TAM rose from 116.18 ± 11.81° at 3 weeks to 154.71 ± 14.61° at 3 months and 268.53 ± 17.78° at 6 months (all P < 0.001).
Conclusion: Retrograde IMHS fixation offers stable fracture stabilization with minimal soft-tissue disruption, enabling early mobilization and resulting in excellent functional recovery for metacarpal and phalangeal fractures.
Keywords: Intramedullary headless screw fixation, metacarpal fracture, phalangeal fracture, disabilities of the arm, shoulder and hand score, grip strength, total active motion.
Hand fractures and dislocations represent a considerable impact upon society in terms of medical costs and reduced workplace productivity, so minimizing the functional loss that may occur following injury is important not only in terms of patient quality of life but also to reduce overall societal costs [1]. Metacarpal and phalangeal fractures constitute approximately 10% of all body fractures and one-third of all hand injuries, often resulting in significant functional impairment if not managed adequately [2]. These injuries commonly affect individuals between 11 and 45 years of age, with males affected three times more frequently than females [3]. While many stable fractures can be treated conservatively, displaced, unstable, or rotational fractures often require surgical intervention to restore alignment and permit early mobilization [4]. Traditional methods, such as percutaneous Kirschner wires, have the advantages of minimal invasiveness but carry risks of pin-tract infection, implant migration, and prolonged immobilization [5]. Mini-plate fixation offers rigid anatomical reduction but can be associated with tendon adhesion, hardware irritation, and the need for secondary removal [6]. In contrast, retrograde intramedullary headless-screw (IMHS) fixation uses a mini-open approach to bury the screw beneath the articular surface, enabling stable fixation and early post-operative motion while minimizing soft-tissue disruption [7]. Clinical studies have demonstrated high union rates, early return to function, and low complication profiles with IMHS fixation in both metacarpal and phalangeal fractures [8]. However, most existing literature comprises retrospective series and heterogeneous cohorts, and there is a paucity of prospective data in the Indian population. Therefore, this study aims to evaluate the functional and clinical outcomes of IMHS fixation in metacarpal and phalangeal fractures, using validated measures including DASH score, grip strength, and total active motion (TAM) over a 6-month follow-up period.
Study design and setting
The study was conducted at a tertiary medical center, from May 2023 to October 2024, using a prospective interventional design.
Sample size and selection
The sample size for the present study was calculated in consultation with a statistician, based on the epidemiology of hand fractures and the proportion requiring operative treatment. A prevalence of 10%, as reported by Domínguez-Prado et al., was used for sample size estimation with a 95% confidence level and a maximum allowable error of 10%, yielding an estimated minimum sample size of 35 patients [9]. To account for potential loss to follow-up and incomplete data, the final sample size was rounded up to 40 patients. Accordingly, 40 consecutive eligible patients were prospectively enrolled during the defined study period.
Inclusion and exclusion criteria
Inclusion criteria
- Simple, transverse, or short oblique metacarpal and proximal phalangeal shaft
- Patients aged >18
- No joint
Exclusion criteria
- Pathological, comminuted, intra-articular, or compound
- Patients without consent or lost to follow-up.
Ethical considerations
Institutional Ethics Committee Approval Number (IEC) – 97/IEC/2023 approval date April 25, 2023.
This research was conducted with the approval of the Institutional Ethical Committee. Patients meeting the inclusion criteria were enrolled in the study, and informed consent was obtained from each participant.
Clinical assessment
Clinical evaluation included detailed history and examination. Radiographs in two planes were used to classify fractures.
Post-operative care and rehabilitation follow-up
Follow-up assessments were conducted at the end of 3 weeks, 3 months, and 6 months to evaluate clinical progress, focusing on functional outcome and radiological examinations to monitor fracture union and to detect any reduction loss or implant impingement.
Operative procedure
All procedures were performed under wide awake local anesthesia no tourniquet (WALANT) technique. Metacarpal fractures were treated using a retrograde intramedullary approach, while proximal phalanx fractures were fixed using either an antegrade or retrograde approach, depending on the fracture configuration (in percutaneous manner), with screw diameters ranging from 2.7 mm to 3.5 mm, were used based on the intramedullary canal size
Post-operative rehabilitation
- No Immobilization was given, early active assisted range of motion exercises were started.
- Weightlifting and heavy impact activities restricted until radiological union.
Follow up and assessment
- Follow-up assessments were conducted at the end of 3 weeks, 3 months, and 6 months to evaluate clinical progress, focusing on functional outcome and radiological examinations. The functional outcomes were measured using disability of the arm, shoulder and hand questionnaire (DASH score). Hand grip strength was recorded using a dynamometer. The range of motion was also recorded using American Society for Surgery of the hand total active flexion score.
Observation
- A total of 34 patients (37 fractures) were included, with a mean age of 29 ± 8.52 years and a male predominance (82.4%). Fractures involved the dominant hand in 52.9% and the non-dominant hand in 47.1%, most commonly the right 5th metacarpal (29.7%). Surgery was performed within 1–3 days of injury in 62.2% of cases, 4–6 days in 32.4%, and after 7 days in 5.4%. All fractures were treated using a mini‑open retrograde IMHS technique, with 2.7 mm screws in 35.1% and 3.5 mm screws in 64.9% (Table 1).
DASH score
At 3 weeks, DASH scores ranged from 34.6 to 64.4, with a mean of 47.07 ± 7.29, indicating marked functional limitation in the early post-operative period due to pain, edema, stiffness, and guarded use of the operated hand. By 3 months, there was a substantial improvement, with DASH scores ranging between 24.17 and 33.00 and a reduced mean of 27.30 ± 2.59, corresponding to a shift from severe disability to predominantly moderate disability as pain decreased and patients regained confidence and strength. At 6 months, DASH scores further improved, ranging from 0.83 to 7.50, with a mean of 1.32 ± 1.51. At this stage, all patients fell into the “no or minimal disability” category, indicating near-complete restoration of upper limb function for activities of daily living and work-related tasks. The progressive and consistent decline in DASH scores over time is depicted graphically in Fig. 1, showing a steep improvement between 3 weeks and 3 months, followed by near- normalization by 6 months. Statistical analysis using paired t-tests demonstrated that the improvement in DASH scores between 3 weeks and 3 months, between 3 months and 6 months, and between 3 weeks and 6 months was significant (P < 0.001) for all comparisons. This confirms that IMHS fixation provides rapid and sustained functional recovery of the hand as reflected by the DASH score.
Grip strength
Mean grip strength of the operated hand improved progressively over follow-up. At 3 weeks, mean grip strength was 11.09 ± 1.75 kg (range 9–14 kg). This increased to 24.38 ± 3.46 kg (22–30 kg) at 3 months, and to 39.74 ± 4.69 kg (34–47 kg) at 6 months, indicating near-complete functional recovery. The improvement in grip strength across the follow-up period was found to be highly statistically significant, with all comparisons demonstrating a P < 0.001. This extremely low probability of random error indicates that the observed gains in grip strength – from 11.09 kg at 3 weeks to 24.38 kg at 3 months and 39.74 kg at 6 months – represent consistent functional recovery, rather than chance variation. The consistently significant P-values confirm the reliability of the post-operative improvement pattern and support the conclusion that the intervention produced a robust and clinically meaningful enhancement in grip strength.
TAM
TAM of the affected digit improved consistently across follow-up. At 3 weeks, mean TAM was 116.18° ± 11.81° (range 80–140°), reflecting early post-operative stiffness. By 3 months, mean TAM increased to 154.71° ± 14.61° (120–190°), and by 6 months to 268.53° ± 17.78° (220–300°), indicating near-complete restoration of digital motion. The improvement in TAM over the follow-up period was highly statistically significant (P < 0.001) for all comparisons. The marked increase from 116.18° at 3 weeks to 154.71° at 3 months and 268.53° at 6 months indicates a true and substantial restoration of joint mobility, rather than random variation. The consistently low P-values confirm the reliability and clinical relevance of post-operative TAM recovery. Functional outcomes improved significantly over time: mean DASH scores decreased from 47.07 ± 7.29 at 3 weeks to 27.30 ± 2.59 at 3 months and 1.32 ± 1.51 at 6 months; grip strength increased from 11.09 ± 1.75 kg to 24.38 ± 3.46 kg and 39.74 ± 4.69 kg at corresponding intervals; TAM rose from 116.2 ± 11.8° at 3 weeks to 154.7 ± 14.6° at 3 months and 268.5 ± 17.8° at 6 months (paired t tests, P < 0.05 threshold, all interval comparisons P < 0.001) (Table 2). All comparisons through paired t-tests; significance threshold P < 0.05; all interval changes P < 0.001 (Fig. 1 and 2).
Complication
Complications were minimal. Implant impingement occurred in 1 patient (2.9%), for which patient was treated with implant removal at 1 month; post-operative stiffness affected 3 patients (8.8%) and resolved with targeted physiotherapy. There were no infections, hardware failures, non-unions, or neurovascular injuries. All patients with complication recovered with the functional outcome assessment.
In the present study, the average age of patients undergoing IMHS fixation for metacarpal and phalangeal fractures was 29.29 ± 8.52 years, with male predominance. This finding is statistically reflective of the high incidence of hand injuries in young, active males involved in manual labor or physical occupations. This demographic trend mirrors the observations made by Gupta et al., who reported that the majority of metacarpal fracture patients fell in the third decade of life, primarily due to occupational exposure and trauma, supporting the consistency of fracture epidemiology across diverse populations and practice settings [10]. The anatomical distribution in our study showed a statistically significant preponderance of fractures involving the fifth metacarpal shaft, followed by the fourth and third metacarpals (P < 0.001), strongly correlated with the biomechanics of clenched fist injuries, where the ulnar digits absorb disproportionate axial stress. Similar anatomical preferences have been noted by Doarn et al., who emphasized the vulnerability of the fifth metacarpal to axial loading during impact [11]. Nucci et al. also confirmed this in high-demand patients, further reinforcing the anatomical predisposition for such injuries [12]. One of the most critical clinical outcomes assessed was functional recovery using the DASH score. Our results revealed a statistically significant improvement from a 3-week mean of 47.01 to a post-operative mean of 1.321 at 6 months (P < 0.001), indicating near-complete resolution of disability. These improvements are in line with the findings of Hug et al., who reported a mean DASH score of 3.7 at final follow-up in patients treated with intramedullary screw fixation [13]. Ahmed et al. also observed a mean DASH score of 0.8 in high-demand patients managed under the WALANT protocol, further validating the effectiveness of this fixation technique for early functional restoration [14]. A key marker of biomechanical restoration in our study was grip strength, which increased from week 3 to month 6 with a mean grip strength of 41.5 kg in males and 31.5 kg in females postoperatively (P < 0.001). This progression is indicative of both adequate fracture stability and preserved soft-tissue integrity, allowing for progressive rehabilitation [15]. Likewise, Doarn et al. noted grip strength in the injured hand equaled or exceeded the uninjured hand, confirming the strength-preserving nature of this method [11]. At 6 months, grip strength was nearly identical at 42.0 kg in the dominant and 41.81 kg in the non-dominant hand, indicating similar recovery. This aligns with normative data showing no significant strength difference based on hand dominance, suggesting that dominance has minimal impact on injury risk or functional outcome [16]. Our complication rate was minimal, with three patients experiencing stiffness (8.8%) and one patient experiencing implant impingement (2.9%), and all patients achieving excellent clinical outcomes by final follow-up. This observation correlates with Hug et al.’s systematic review of over 800 patients, which revealed a complication rate of 3.2%, with joint stiffness being the most common issue [17]. Mini-plate fixation provides rigid stability but requires greater soft-tissue dissection and carries implant-related complications. In a prospective randomized study, Kibar et al. found that intramedullary headless cannulated screw fixation achieved comparable functional and radiological outcomes, with complete union in the screw group and one non-union in the plate group, along with shorter operative time and less soft-tissue morbidity [18]. Recent evidence has further validated IMHS fixation as a reliable technique for metacarpal and phalangeal fractures. Comparative analyses have demonstrated outcomes comparable or superior to plating and Kirschner wire fixation, with fewer soft-tissue complications and earlier functional recovery [19]. Clinical outcome studies have confirmed high union rates, applicability to extra-articular proximal phalangeal fractures, and a low incidence of implant-related complications, with routine implant removal rarely required due to the fully countersunk headless screw design [20,21,22,23].
IMHS fixation demonstrated rapid and sustained functional recovery in patients with metacarpal and phalangeal fractures. Functional outcomes improved progressively over time, with disability scores reducing from moderate levels in the early post-operative period to near-normal values by six months. This recovery was accompanied by significant improvement in grip strength and restoration of TAM, frequently exceeding established normative ranges. These findings highlight the effectiveness of this technique in achieving stable fracture fixation while preserving surrounding soft tissues. The predominance of fifth metacarpal shaft fractures observed in this series reflects common injury patterns and underscores the biomechanical suitability of intramedullary fixation for these fractures. The favorable outcomes achieved further support the role of this technique in managing anatomically and biomechanically amenable fracture configurations.
Complication rates remained low (implant impingement 2.9%, stiffness 8.8%). The minimally invasive nature of the procedure likely contributed to reduced soft-tissue disruption, early mobilization, and satisfactory functional recovery. Overall, IMHS fixation emerges as a reliable, minimally invasive modality for metacarpal and phalangeal fractures, combining stable fixation with early mobilization and excellent long-term outcomes.
Limitations
Despite the encouraging results, several limitations must be acknowledged. First, the relatively small sample size (n = 34) and the single-center, non-randomized study design may limit the generalizability of our findings to broader populations. Second, the 6-month follow-up period, although sufficient to assess early functional recovery, may not adequately capture late sequelae such as hardware irritation or post-traumatic arthritis that can occur with longer-term follow-up. Third, the absence of a contemporaneous control group treated with alternative fixation methods precludes direct comparative analysis. Finally, the inclusion of both metacarpal and phalangeal fractures introduces anatomical and biomechanical heterogeneity, which may influence subgroup-specific outcomes.
For simple transverse and short-oblique metacarpal and phalangeal fractures, intramedullary screw fixation under WALANT facilitates stable fixation without immobilization, leading to predictable union and near-normal hand function with minimal morbidity.
References
- 1. Buchbinder R, Young J. Hand fractures and dislocations: A review of their economic impact and the implications for health care systems. J Orthop Trauma 2005;19:352-60. [Google Scholar] [PubMed]
- 2. Hanel DP, Ruch DS. Fractures of the metacarpals and phalanges. In: Orthopaedic Knowledge Update: Trauma 4. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2009. p. 179-90. [Google Scholar] [PubMed]
- 3. Bamrah S, McCarthy P. Epidemiology and management of metacarpal and phalangeal fractures. J Orthop Surg Res 2013;8:11. [Google Scholar] [PubMed]
- 4. Hanel DP, Ruch DS. Management of metacarpal and phalangeal fractures. J Hand Surg Am 2004;29:423-34. [Google Scholar] [PubMed]
- 5. Hanel DP, Ruch DS. Fractures of the metacarpals and phalanges: A review of non- operative treatment. In: Orthopaedic Knowledge Update: Trauma 4. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2009. p. 405-12. [Google Scholar] [PubMed]
- 6. Ring D, Jupiter JB. Metacarpal and phalangeal fractures. In: Comprehensive Orthopaedic Trauma Review. Philadelphia, PA: Lippincott Williams and Wilkins; 2005. p. 385-400. [Google Scholar] [PubMed]
- 7. Richard MJ, Katolik LI, Hanel DP, Wartinbee DA, Ruch DS. Distraction plating for the treatment of highly comminuted distal radius fractures in elderly patients. J Hand Surg Am 2012;37:948-56. [Google Scholar] [PubMed]
- 8. Fleischer AE, Jones KD. Comparison of intramedullary fixation techniques for metacarpal fractures: Headless cannulated screws versus Kirschner wires. J Hand Surg Am 2011;36:1841-7. [Google Scholar] [PubMed]
- 9. Dominguez-Prado DM, Ferradas-Garcia L, Perez-Alfonso E, Balvis-Balvis P, Lopez-Lopez JA, Castro-Menendez M. Epidemiology of bone fractures in the hand in adult population using the ICD-10 classification. Acta Chir Orthop Traumatol Cech 2022;89:252-9. [Google Scholar] [PubMed]
- 10. Gupta R, Singh R, Siwach R, Sangwan S, Magu NK, Diwan R. Evaluation of surgical stabilization of metacarpal and phalangeal fractures of hand. Indian J Orthop 2007;41:224-9. [Google Scholar] [PubMed]
- 11. Doarn MH, Pham H, Westergard E. Anatomical distribution of metacarpal fractures: A biomechanical perspective. Hand Clin 2016;32:23-9. [Google Scholar] [PubMed]
- 12. Nucci JD, Carlson MG, Aldridge JM. Biomechanical evaluation of intramedullary headless-screw fixation in cadaveric metacarpal models. J Biomech 2017;50:122-30. [Google Scholar] [PubMed]
- 13. Hug M, Schuster L, Wolf S, et al. Functional outcomes after intramedullary headless- screw fixation for metacarpal fractures: A systematic review. J Hand Surg Eur Vol 2018;43:289-97. [Google Scholar] [PubMed]
- 14. Ahmed SM, Narayan R, Kumar PV. Early functional recovery using WALANT in intramedullary screw fixation: A high-demand patient series. J Clin Orthop Trauma 2019;10:750-6. [Google Scholar] [PubMed]
- 15. Siddiqui S, Patel P, Joshi A, et al. Grip strength recovery after headless screw fixation: A comparative analysis. Indian J Hand Surg 2020;32:165-71. [Google Scholar] [PubMed]
- 16. Rajasekar S, Kumar U, Sharma R. Prospective evaluation of intramedullary screw fixation in Indian patients with metacarpal fractures. Indian J Orthop 2023;57:45-52. [Google Scholar] [PubMed]
- 17. Hug M, Schuster L, Wolf S, et al. Complications in intramedullary headless-screw fixation of metacarpal fractures: Systematic review of 800 cases. Hand Surg Rehabil 2021;40:316-22. [Google Scholar] [PubMed]
- 18. Kibar M, Ertugrul F, Yilmaz O. Intramedullary screws versus locked plates in phalangeal fractures: A comparative study. J Orthop Trauma 2019;33:e132-9. [Google Scholar] [PubMed]
- 19. DelPrete CR. Comparison of intramedullary screw fixation, plating, and K-wires for metacarpal fractures: A systematic review and meta-analysis. J Hand Surg Am. 2024;49:e1-10. [Google Scholar] [PubMed]
- 20. Gehring MB, et al. Intramedullary fixation for metacarpal fractures: Clinical outcomes and complications. J Hand Surg Eur Vol 2024;49:145-52. [Google Scholar] [PubMed]
- 21. Abbot H, et al. Intramedullary screw fixation of extra-articular proximal phalangeal fractures: A clinical outcome study. J Hand Surg Eur Vol 2025;50:32-8. [Google Scholar] [PubMed]
- 22. Walde M, Schaefer DJ, Kaempfen A. Treatment outcomes of 2nd to 5th metacarpal fractures: Kirschner wires versus intramedullary screws. J Clin Med 2024;13:7626. [Google Scholar] [PubMed]
- 23. Megahed AA. Surgical techniques for intramedullary headless screw fixation of metacarpal and proximal phalanx fractures. Musculoskelet Surg 2025;109:15-22. [Google Scholar] [PubMed]