Near-total fibulectomy with distal fibular preservation and targeted antibiotics is a successful treatment option for extensive fibular osteomyelitis in children, maintaining ankle stability and function.
Dr. Elandevan Gunasekaran, Department of Orthopaedics, All India Institute of Medical Sciences, Guntur, Andhra Pradesh, India. E-mail: elandevangunasekaran@gmail.com
Introduction: Osteomyelitis in children typically affects the metaphysis of long bones, most commonly the femur and tibia. Fibular involvement is rare, accounting for <10% of pediatric osteomyelitis cases. Pan-diaphyseal involvement is even rarer.
Case Report: A 7-year-old girl presented with a chronic discharging sinus, pain, and swelling in the right leg for 10 months following minor trauma. Radiographs and magnetic resonance imaging revealed chronic pan-diaphyseal osteomyelitis of the fibula with a pathological fracture. After failed conservative management, she underwent sequestrectomy and near-total fibulectomy, preserving the distal 5 cm to maintain ankle stability. Intraoperative cultures confirmed methicillin-sensitive Staphylococcus aureus, and she received targeted antibiotic therapy. She achieved full recovery with a normal gait and no recurrence at 3-month follow-up.
Conclusion: This case highlights the importance of early suspicion and aggressive surgical management for chronic fibular osteomyelitis in children. Near-total fibulectomy is feasible and functionally successful when the distal fibula is preserved.
Keywords: Osteomyelitis, fibula, pediatric, fibulectomy.
Osteomyelitis is an inflammatory bone condition primarily caused by infection, typically from hematogenous spread in children. The vascular anatomy of the metaphysis makes long bones, especially the femur and tibia, common sites [1,2]. Fibular involvement is rare, accounting for <10% of cases [3]. Pan-diaphyseal involvement of the fibula is even more unusual, with limited cases documented in the literature [4]. Acute osteomyelitis often presents with fever, localized swelling, and tenderness. Chronic osteomyelitis, in contrast, develops insidiously with persistent pain, discharging sinuses, and sometimes a pathological fracture [5]. Radiological features include bone sclerosis, sequestrum formation, and sinus tracts. Magnetic resonance imaging (MRI) is the modality of choice to delineate the extent of involvement and soft-tissue changes [6]. This report describes a rare case of pediatric chronic pan-diaphyseal osteomyelitis of the fibula managed by near-total fibulectomy while preserving ankle integrity. We emphasize the diagnostic challenges and surgical decision-making in such unusual presentations.
A 7-year-old girl presented to our department with a 10-month history of right leg pain, recurrent swelling, and intermittent purulent discharge from a sinus located on the lateral leg. Her symptoms began after a slip and fall injury at school, following which she developed pain and swelling. Initial radiographs were inconclusive, and she underwent incision and drainage for a presumed abscess at another facility. However, her symptoms persisted, evolving into a chronic discharging sinus with the inability to bear weight. At presentation, she was afebrile. Examination revealed a sinus with seropurulent discharge over the mid-lateral aspect of the right leg [Fig. 1].

Fig. 1: Clinical picture of the right leg.
Diffuse tenderness was noted along the fibular shaft without surrounding cellulitis or instability at the ankle. There was mild wasting of the calf muscles. Laboratory investigations revealed an erythrocyte sedimentation rate of 82 mm/hr, C-reactive protein 7.8 mg/dL, and total leukocyte count of 9800/μL.
Plain radiographs showed patchy sclerosis, lytic changes, and a pathological fracture along the mid to distal fibular diaphysis [Fig. 2].

Fig. 2: Pre-operative X-ray of right leg.
MRI confirmed pan-diaphyseal osteomyelitis involving the entire fibular shaft with cortical destruction, sequestrum formation, and a sinus tract extending from the proximal to distal fibula.
After a trial of empirical antibiotics and immobilization failed, surgical intervention was planned. Under general anesthesia, methylene blue was injected through the sinus to delineate its extent. A longitudinal incision over the fibula allowed sinus tract excision, removal of necrotic bone, and debridement [Fig. 3]. Approximately 10 cm of diseased fibula was excised en bloc, sparing the distal 5 cm to preserve the lateral malleolus and ankle mortise [Fig. 4].

Fig. 3: (a and b) Intraoperative picture of fibula resection.
Tissue samples were sent for bacterial, fungal, and acid-fast bacilli cultures and histopathology. Methicillin-sensitive Staphylococcus aureus (MSSA) was isolated, sensitive to cloxacillin. Histopathology confirmed chronic osteomyelitis with inflammatory infiltrates and necrotic bone.

Fig. 4: Intraoperative picture of resected fibula.
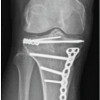
Postoperatively, the leg was immobilized in a cast, and she was initiated on intravenous cloxacillin for 2 weeks, followed by 4 weeks of oral cephalexin. She remained non-weight-bearing initially and was gradually progressed to full weight bearing at 6 weeks. At 3 months, she was ambulatory without support, and follow-up radiographs showed no recurrence or tibial involvement [Fig. 5]. There was no ankle valgus or subluxation.

Fig. 5: Post-operative X-ray of right leg.
Isolated fibular osteomyelitis is rare due to the fibula’s relatively poor blood supply and lower mechanical loading [3,4]. Pan-diaphyseal involvement is even more unusual. In our case, delayed diagnosis and prior inadequate surgical drainage may have contributed to disease chronicity. The diagnosis of chronic osteomyelitis relies on a combination of clinical suspicion, imaging, and microbiology. MRI is considered the gold standard for delineating intraosseous abscesses and sinus tracts [6]. Identification of the causative organism through biopsy and culture is crucial for targeted therapy [7]. MSSA remains the most common pathogen in pediatric osteomyelitis [8]. Surgical intervention is often required in chronic osteomyelitis to remove necrotic tissue and control infection [9]. In contrast to weight-bearing bones such as the femur or tibia, the fibula can be resected without major biomechanical consequences if the ankle mortise is preserved. As shown in our case, preservation of the distal fibula is critical to avoid valgus deformity and ankle instability [10]. A study by Vij et al. reported ankle subluxation in a 10-month-old infant after complete fibular resection for pan-diaphyseal osteomyelitis, underscoring the importance of retaining the lateral malleolus [11]. In our case, the distal 5 cm of the fibula was preserved to maintain lateral ankle support. Only a few case reports describe similar presentations [Table 1].

Table 1: Cases (especially fibular involvement and similar management) and the present case
Ostrea et al. presented a case of pediatric fibular osteomyelitis involving the entire diaphysis, treated successfully with partial fibulectomy [7]. Ulhaque et al. also described delayed diagnosis and surgical management of diaphyseal osteomyelitis in another long bone, highlighting diagnostic delays common to these presentations. Antibiotic therapy following surgical debridement is essential for the eradication of infection. Literature supports a 4–6 week course of organism-specific antibiotics for chronic osteomyelitis [12]. Our patient received a total of 6 weeks of targeted therapy and achieved full clinical and functional recovery. Our report reinforces the principles of early diagnosis, thorough imaging, appropriate surgical resection, preserving critical anatomy, and tailored antimicrobial therapy.
Pan-diaphyseal osteomyelitis of the fibula in children is a rare clinical entity. When conservative treatment fails, near-total fibulectomy with distal preservation provides effective infection control and maintains ankle stability. High clinical suspicion, timely imaging, and tailored surgical management are key to favorable outcomes.
Extensive fibular osteomyelitis in children, though rare, can be successfully managed by near-total fibulectomy with preservation of the lateral malleolus. Early diagnosis and targeted antibiotic therapy are essential to achieve complete resolution and preserve function.
References
- 1. Thakolkaran N, Shetty AK. Acute hematogenous osteomyelitis in children. Ochsner J 2019;19:116-22. [Google Scholar] [PubMed]
- 2. Waldvogel FA, Medoff G, Swartz MN. Osteomyelitis: A review of clinical features, therapeutic considerations and unusual aspects. N Engl J Med 1970;282:198-206. [Google Scholar] [PubMed]
- 3. Saadana J, Lassioued O, Abid S, Ben Mansour M, Abid A. A child with acute hematogenous osteomyelitis of the distal fibula and infective endocarditis. Cureus 15:e35429. [Google Scholar] [PubMed]
- 4. Khurana A, Chhawra S, Gupta R, Kumar S. Osteomyelitis of fibula rare case with various differential diagnosis. J Orthop Case Rep 2017;7:59-62. [Google Scholar] [PubMed]
- 5. Gupta V, Shah R, Pandey A, Khan D, Ayar S. A rare case report on chronic osteomyelitis of fibula in a child of 6 years. Indian J Orthop Surg 2020;5:287-91. [Google Scholar] [PubMed]
- 6. Lazzarini L, Mader JT, Calhoun JH. Osteomyelitis in long bones. J Bone Joint Surg Am 2004;86:2305-18. [Google Scholar] [PubMed]
- 7. Ostrea AC, Ramos MD, Frez RV. Pediatric chronic fibular pandiaphyseal osteomyelitis: Case report with literature review. Asian Journal of Orthopaedic Research (2020); 248-258 [Google Scholar] [PubMed]
- 8. Lew DP, Waldvogel FA. Osteomyelitis. Lancet 2004;364:369-79. [Google Scholar] [PubMed]
- 9. Haidar R, Der Boghossian A, Atiyeh B. Duration of post-surgical antibiotics in chronic osteomyelitis: Empiric or evidence-based? Int J Infect Dis 2010;14:e752-8. [Google Scholar] [PubMed]
- 10. González-Herranz P, Del Río A, Burgos J, López-Mondejar JA, Rapariz JM. Valgus deformity after fibular resection in children. J Pediatr Orthop 2003;23:55-9. [Google Scholar] [PubMed]
- 11. Vij N, Ranade AS, Belthur MV. Progressive ankle subluxation following panfibular osteomyelitis requiring fibular resection. Cureus 2022;14:e24112. [Google Scholar] [PubMed]
- 12. Ulhaque F, Rahman SH, Rai AK, Hadole BS, Meghashyama KS, Kumar KG. Unifocal tubercular osteomyelitis of ulna diaphysis in a child: A case report. J Orthop Case Rep 2024;14:119-23. [Google Scholar] [PubMed]
- 13. Ziani F, Martini M. Results of the surgical treatment of chronic hematogenous osteomyelitis of the fibula. Int Orthop 1990;14:167-73. [Google Scholar] [PubMed]
- 14. Varun V, Naveen S, Anuj R, Gaurav K, Shilpi S, Vikas V. Osteomyelitis of fibula in a child: A rare case report with a huge sequestrum. Scholars Acad J Biosci 2015;3:563-6 [Google Scholar] [PubMed]