[box type=”bio”] Learning Point of the Article: [/box]
Suprascapular nerve compression should be suspected in front of a painful shoulder with spinatus fossa amyotrophy, leading to magnetic resonance imaging that allows the diagnosis and to the treatment which is a surgical decompression that must be done before muscular atrophy.
Case Report | Volume 8 | Issue 5 | JOCR September – October 2018 | Page 40-42|Sabri Mahjoub, Ahmed Amine Lahmar, Mourad Zarâa, Belhadj Massoud Ahmed, Mohamed Abdelkafi, Mondher Mbarek. DOI: 10.13107/jocr.2250-0685.1202
Authors: Sabri Mahjoub[1], Ahmed Amine Lahmar[1], Mourad Zarâa[1], Belhadj Massoud Ahmed[1], Mohamed Abdelkafi[1], Mondher Mbarek[1]
[1]Department of Orthopedic Surgery, Tunis Trauma Center, Ben Arous, Tunisia.
Address of Correspondence:
Dr. Sabri Mahjoub,
Department of Orthopedic Surgery, Tunis Trauma Center, Ben Arous, Tunisia.
E-mail: sabrimahjoub@hotmail.com
Abstract
Introduction: The ductal syndromes of the shoulder combine all the compressive processes of the suprascapular nerve at the level of its passage in the spinoglenoid notch and this for several causes. The most common is a lesion of the labrum resulting in the formation of a cyst. These cysts are rare and often underestimated. Provoking a compression of the suprascapular nerve, they are likely to cause an atrophy of the external rotator muscles of the cuff.
Case Report: We present a rare case of a paraglenoid cyst resulting in a ductal syndrome by suprascapular nerve compression. A 56-year-old man consulted our department for chronic pain of the left shoulder with a decrease in muscle strength. On clinical examination, the patient had a deficit of external rotation with a clear amyotrophy of the infraspinatus fossa. We opted for arthroscopic surgical resection. At the last follow-up, the patient did not show any more pain, with a total recovery of muscle strength.
Conclusion: The clinical signs of compressive processes of the suprascapular nerve are quite misleading, so establishing a correct diagnosis and surgical management is vital before irreversible muscularatrophy takes place.
Keywords: Spinoglenoidcyst, Suprascapular nerve, Arthroscopic decompression, Labral tear, SLAP repair.
Introduction
Shoulder pain related to a ductal syndrome is infrequent (between 0.4% and 2%). The nerves involved are the suprascapular nerve, the long thoracic nerve, the axillary nerve, and the musculocutaneous nerve [1,2, 3, 4]. As it passes through the spinoglenoid indentation, the suprascapular nerve may be the seat of compression. The causes of compression or suffering can be varied; the most common is a lesion of the labrum causing the formation of these cysts. According to the literature, paraglenoid cysts are rare and often underestimated[1, 5]. They are often seen at a late stage and may have functional consequences by irreversible muscular atrophy. We report an original observation of a paraglenoid cyst resulting in ductal syndrome by nerve compression. Through this clinical case, we specify the clinical characteristics, diagnostic and surgical management of this pathology.
Case Report
A 56-year-old man, with no medical history, right-handed, consulted our department for chronic pain of the left shoulder that was not responding to medical treatment and physiotherapy. There was no history of previous trauma. Our patient also complained of a decrease in shoulder muscle strength. On clinical examination, the patient had a deficit of external rotation with a clear amyotrophy of the infraspinatus fossa (Fig. 1).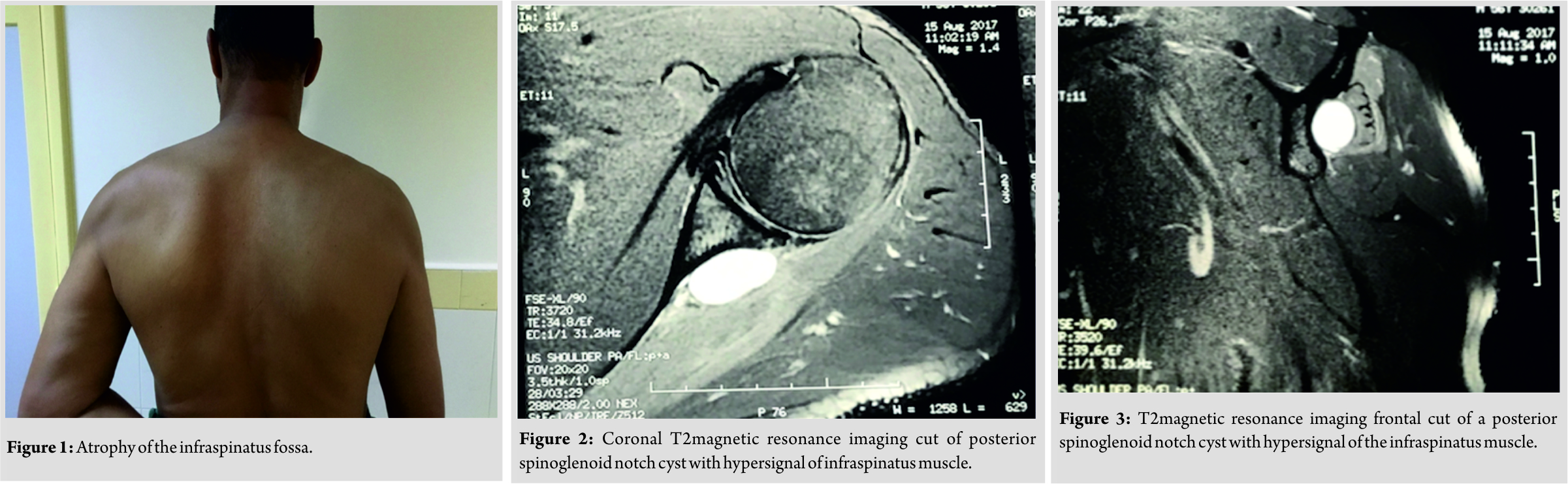
Discussion
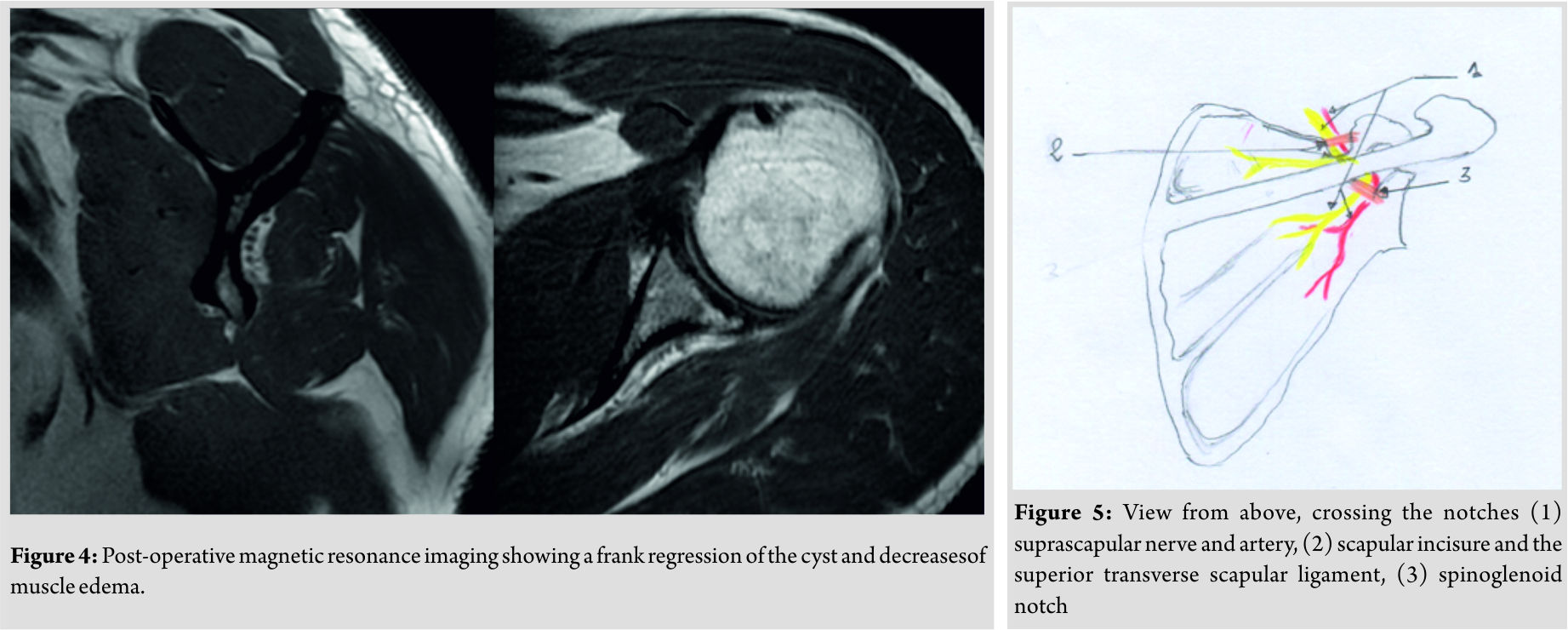
The suprascapular nerve originates from the brachial plexus (C4-C5-C6) and is essentially a motor nerve. It innervates the supra- and infra-spinatus muscles. It does not have a sensitive cutaneous territory. It is located about 2 cm from the capsule and passes through the supraspinatus fossa. Its path presents two critical points of passage(Fig. 5) [2]. A superior passage in the scapular incision which is closed at the top by the very solid superior transverse scapular ligament. An inferior and posterior passage at the spinoglenoid notch where it can be constrained by the inferior transverse scapular ligament. The muscular involvement may vary according to the seat of compression of the suprascapular nerve. The supraspinatus muscle is affected by compression at the level of its upper portion and that of the infraspinatus at its posterior portion. The causes of compression are multiple; the most common is a lesion of the labrum resulting in the formation of a cyst. The physiopathology is applicable toparameniscalcysts: The increase in intra-articular pressure drives the latter through the labral lesion, which forms a cyst. This pathology is rare with a ratio of 2–4% in the general population. However, it is often underestimated and diagnosed at a late stage [5, 6]. In our case, only the infraspinatus muscle was concerned given the location of the cyst. The upper portion of the suprascapular nerve relevant to the supraspinatus muscle did not suffer from compression by the cyst. In consequence, there was no clinical sign of supraspinatus involvement, therefore, a negativeJobb test. Ductal syndromes of the suprascapular nerve are often seen at the stage of chronic neuropathy[1, 2, 5]. The patient consults for atypical pain suggestive of cervicobrachial neuralgia or rotator cuff syndrome. The initial pain is often diurnal and nocturnal, to become secondarily mechanical. Clinical examination will essentially check for a decrease in external rotation muscle strength, as well as amyotrophy of the supraspinatus fossa by palpation and amyotrophy of the infraspinatus fossa which can be clearly visible [2, 3, 4]. MRI and arthro-MRI are currently considered as the reference examinations for the positive, topographical, and etiological diagnosis of suprascapular nerve entrapment[7]. They allow the diagnosis as well as evaluation of muscular denervation. The most common radiologic signs are edema, atrophy, and fatty degeneration. Muscular pain is initially manifested by the presence of edema, which is a sensitive and specific sign of muscular denervation. It is a T2 diffuse hypersignal, homogeneous and concerns all the muscle. The topography corresponds to the territory of the motor branch intended for supra- or infra-spinatus. TheT2 hypersignal of the infraspinatus muscle was very visible on MRI sections in our patient (Fig. 2 and 3). Muscular atrophy and fatty degeneration become visible in chronic cases with a long evolution[5, 8]. Arthro-MRI highlights its articular origin by seeking a lesion of the labrum. Computed tomography (CT) arthrography is often negative, and only the indirect sign of fat disappearing from the spinoglenoid indentation can suggest the diagnosis [7]. Nerve conductionstudies maybe helpful in confirming the diagnosis and have a greatprognostic value by giving information on the severity of the lesions. The non-operative treatment options are varied and include oral medications including nonsteroidal anti-inflammatory drugs as well as percutaneous needle aspiration associated with intralesional steroid injection. However, symptomatic paralabral cysts causing muscular atrophy that fails to respond to conservative treatment should be treated surgically. Several studies shown high prevalence of labral tears in connection with spinoglenoid cysts and have suggested a high recurrence rate if the intra-articular labral pathologic process is not addressed [1, 5, 6]. Schroder[6] objectified a recurrence rate close to 0% after labral repair. Hence, surgical treatment should not be limited to the resection of the cyst, but the labral lesion must be repaired to prevent recurrence[5, 6, 9, 10].
Conclusion
The ductal syndromes of the shoulder join all the compressive processes of the suprascapular nerve at the level of its passage in the spinoglenoid notch. The causes are numerous; the most common is a lesion of the labrum resulting in the formation of a cyst. Often considered as cervical lesions or rotator cuff lesions, their diagnoses must be discussed before the installation of a muscular atrophy.
Clinical Message
In a patient consulting for shoulder pain with spinatus fossa amyotrophy, suprascapular nerve compression should be suspected. MRI allows the diagnosis; the treatment is a surgical decompression that must be done before the muscular atrophy.
References
1. Noël E. Les syndromes canalaires de l’épaule. Rev Rhum 2007;74:339-43.
2. Bouttens D, Leonard JC. La pathologie du nerf sus-scapulaire chez le jeune sportif. Sci Sports 2006;21:166-9.
3. Vastamaki M, Goransson H. Suprascapular nerve entrapment. Clin OrthopRelat Res 1993;297:135-43.
4. Antoniadis G, Richter HP, Rath S, Braun V, Moese G. Suprascapular nerve entrapment: experience with 28 cases. J Neurosurg 1996;85:1020-5.
5. Shon MS, Jung SW, Kim JW, Yoo JC. Arthroscopic all–intra–articular decompression and labral repair of paralabral cyst in the shoulder. J Shoulder Elbow Surg 2015;24:e7-e14.
6. Schrøder CP, Lundgreen K, Kvakestad R. Paralabral cysts of the shoulder treated with isolated labral repair: Effect on pain and radiologic findings. J Shoulder Elbow Surg 2018;27:1283-9.
7. Amoretti N, Marcy PY, Hovorka E, Lesbats-Jacquot V, Fonquerne ME, Boileau P, et al. Imagerie des syndromes canalaires de l’épaule. J Traumatol Sport 2007;24:73-6.
8. Budzik JF, Wavreille G, Pansini V, Moraux A, Demondion X, Cotten A. Entrapment neuropathies of the shoulder. MagnReson Imaging Clin N Am 2012;20:373-91, xii.
9. Schroder CP, Skare O, Stiris M, Gjengedal E, Uppheim G, Brox JI. Treatment of labral tears with associated spinoglenoid cysts without cyst decompression. J Bone Joint Surg Am 2008;90:523-30.
10. Schroeder AJ, Bedeir YH, Schumaier AP, Desai VS, Grawe BM. Arthroscopic management of SLAP lesions with concomitant spinoglenoid notch ganglion cysts: A Systematic review comparing repair alone to repair with decompression. Arthroscopy 2018;34:2247-53.
 |
 |
 |
 |
 |
| Dr. Sabri Mahjoub | Dr. Ahmed Amine Lahmar | Dr. Mourad Zarâa | Dr. Belhadj Massoud Ahmed | Dr. Mondher Mbarek |
| How to Cite This Article: Mahjoub S, Lahmar A A, Zarâa M, Ahmed B M, Abdelkafi M, Mbarek M. A Rare Cause of Compression of the Suprascapular Nerve: The Paraglenoid Cyst. Journal of Orthopaedic Case Reports 2018 Sep-Oct; 8(5): 40-42. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com