In the event of a high velocity blunt trauma, one should have a high index of suspicion even in the locations where acute compartment syndrome is uncommon, such as the thigh.
Dr. Ujjal Kar, Department of Orthopaedics, Assam Medical College and Hospital, Dibrugarh - 786 002, Assam, India. E-mail: uk.ujjalkar@gmail.com
Introduction: Acute compartment syndrome of the thigh is an orthopedic emergency. Compartment syndrome of the thigh without a fracture or any other associated pre-injury pathology is scantily reported in the literature. Lack of awareness and inexperience often results in a failure to diagnose it.
Case report: In this article, we are presenting a rare case of acute compartment syndrome involving the anterior compartment of the thigh without any bony abnormality or a fracture in a 62-year-old male who sustained an injury to his lateral aspect of the right thigh by a fall from a height. We performed an emergency fasciotomy and decompression of the involved compartment. The patient needed a subsequent skin grafting for the wound closure. Finally, after 7 months of follow-up, an excellent clinical outcome of the affected limb has been achieved.
Conclusion: Thigh compartment syndrome without a fracture or other pre-injury pathological abnormalities of the thigh is relatively rare, hence there is often a fair risk that a case will go unnoticed. Therefore, a high index of clinical suspicion and prompt treatment can protect a patient with thigh compartment syndrome from long-term disability.
Keywords: Thigh compartment syndrome, blunt trauma, fasciotomy.
Acute compartment syndrome of the thigh is a known entity but without a fracture, it is rare and is associated with a significant morbidity and mortality [1]. There is also a paucity of literature regarding thigh compartment syndrome as a result of blunt trauma without a fracture or any associated major vascular injury or pre-injury pathological conditions. Compartment syndrome is defined as the increased interstitial pressure within the osseofascial compartment altering the capillary perfusion, leading to a decrease in blood supply to the soft tissues such as muscles and nerves which ultimately end up with cellular anoxia, ischemia, and necrosis [2]. The most common cause of acute compartment syndrome of the thigh is fracture or crush injury [3]. However, non-fracture conditions such as road traffic accidents, injury in a soccer player, vascular injury, lower limb revascularization syndrome, intramedullary nailing of a closed femur fracture, the use of anti-shock trousers, and contusion are the other causes [4, 5]. Atraumatic etiologies include coagulopathy due to the use of low-molecular-weight heparin, warfarin, NSAIDs, or because of medical condition like cirrhosis. Major trauma leading to coagulopathy has also been documented as a cause for thigh compartment syndrome [2]. The principle of diagnosis and management of thigh compartment syndrome remain same as the compartment syndrome of upper limb and leg [6]. This condition is often unrecognized in the absence of fracture [5]. Acute compartment syndrome is well known to every orthopedic surgeons but yet there is no clear consensus regarding its diagnostic criteria. Pain out of proportion being the most common symptom in acute compartment syndrome [3]. If the patient is alert, conscious, and well oriented, the clinical diagnosis of acute compartment syndrome of the thigh can be made on the basis of thigh pain out of proportion to the severity of injury, massive swelling, pain on passive stretch, paresthesia, poikilothermia, pulselessness, pallor, and muscle paralysis [4].
A 62-year-old man injured his right thigh by falling down from a height of around 10–12 feet on a wooden log. He developed pain and swelling over the right thigh within an hour for which he was taken to the local hospital. He was treated with injectable analgesics and discharged after few hours prescribing some oral analgesics and anti-inflammatory drugs. After reaching home, the severity of the pain gradually increased with associated numbness in the leg which was not responding to analgesic and anti-inflammatory drugs. On the next day, he visited the same hospital, the treating doctor again gave him parenteral analgesic, even then the pain did not subside and hence, they referred him to our hospital. The patient presented to us exactly 24 h after his injury. He complained of severe pain and swelling over the right thigh with loss of sensation and inability to move his affected limb which was gradually progressive and did not subside with any kind of analgesics or anti-inflammatory. In the course of the 24 h of the injury, the patient normally passed stool and urine. The patient had no significant history of illness. The patient had no history of any clotting disorder and neither of his family had suffered from any kind of bleeding diathesis. The patient neither had given any history of anti-coagulant use nor any significant drug intake. On examination, the patient was alert, conscious, and well oriented to time place and person. His blood pressure was recorded to be 148/90 mm of mercury and pulse rate of 100 per minute. On inspection, the affected thigh was grossly swollen and the overlying skin was shiny and the attitude of his hip and knee was mildly flexed. There was an ecchymosis of size around 10 × 6 cm2 over the anterolateral aspect of the thigh. On palpation, the thigh was severely tense and there was severe pain on attempted passive flexion and extension of the knee. There were no abnormal mobility and no bony crepitus in the affected limb, and the patient was able to do active straight leg raising. The affected limb was cold distal to the thigh compared to the opposite normal limb. There was lack of sensation below the knee and there was no motor activity distally. Distal pulse in the affected limb was feeble and distal SpO2 was fluctuating. Plain radiograph of the femur did not show any evidence of bony abnormality or fracture. USG color Doppler of the right lower limb showed gross collection in the anterior compartment of the thigh, subcutaneous edema, and decreased (monophasic) flow in the distal part of the femoral artery till the dorsalis pedis artery. Therefore, on the basis of the classical signs (six P’s, i.e., pain out of proportion, pain on passive stretch, pallor, paresthesia, pulselessness/ feeble distal pulse, and paralysis distal to the injury), a clinical diagnosis of compartment syndrome of the thigh involving the anterior compartment was made. Due to the late presentation, compartmental pressure measurement, further radiological investigations such as CT angiography, magnetic resonance imaging, and CT scan of the thigh were not done to avoid further delay in the definitive procedure, that is, the fasciotomy. The patient was prepared for emergency fasciotomy with emergency pre-operative work out within 3 h of presentation to the emergency department. The patient was placed in supine position on the operating table under spinal anesthesia. Under all aseptic and antiseptic measures, proper painting with 10% povidone-iodine and proper draping was done on the involved limb. Lateral incision was given over the involved thigh. The fascia lata was incised and split with scissors parallel to the skin incision along its fibers and the muscle fascia over the vastus lateralis was exposed. As the fascia was incised, the contused and swollen vastus lateralis muscle popped out. The vastus lateralis was found to be partially avulsed from the lateral intermuscular septum, while separating the vastus lateralis by blunt dissection from the fascia lata, around one and half of the kidney tray of clotted blood was evacuated which was approximately 1100 ml in amount. The vastus lateralis was retracted anteromedially and a torn thrombosed perforator was identified and ligated. After full evacuation of the clotted blood from the anterior compartment, longitudinal incision over the lateral intermuscular septum was given to relax the posterior compartment. Medial compartment was found to be soft. Multiple small horizontal incisions were given in the divided anterior edge of the tensor fascia lata to decrease the tension in the margin of the wound. Proper irrigation with normal saline was done. Few fibers of the vastus lateralis were stitched back to the lateral intermuscular septum. The wound was left open without closing the skin and a soft dressing pad was applied. Then, the patient was shifted to the ward after getting clearance from the anesthesiologist. In the course of the hospital stay, the patient regained his normal sensation and motor power (but not up to the mark). He also regained his normal distal pulse in the affected limb on the next day of fasciotomy. In the post-operative stay, he was given broad spectrum I.V. antibiotics, subcutaneous low-molecular-weight heparin (as advised by the cardiothoracic vascular surgeon), oral analgesic, oral anti-inflammatory, oral indomethacin to prevent heterotopic ossificans, and oral proton-pump inhibitor. After a few days of alternate day antiseptic dressings, vacuum-assisted closure (VAC) was applied to decrease the size of the wound. After 5 days of VAC treatment, the wound was inspected and found to be healthy and smaller than previous. As advised by the physiotherapist, the normal physiotherapy for the affected limb was started and he was given a foot drop splint for his foot drop which actually was gradually improving. The patient was shifted to the plastic surgery department in our hospital for the skin grafting on the surgical wound. Follow-up at 7 months of the injury, the patient has regained his normal muscle power and near-normal range of motion of all the joints in the affected limb.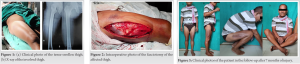
The large compartmental volume, relative elasticity of the boundaries of the thigh compartment, and no rigid interosseous membrane may be the possible explanation for the inherent capacity of the thigh to tolerate for massive swelling and significant quantity of hematoma formation. Moreover, thigh compartments anatomically blend with the hip musculature which allows free extravasation of the hematoma in the thigh compartments. Hence, the thigh compartment syndrome is rare, the complications are also less and are often delay in presentation compared to compartment syndromes of the other parts of our body [1, 4]. Hematoma collection causes continued hemorrhage in the compartment leading to late presentation as a compartment syndrome, as the hematoma has got the fibrinolytic activity and is also the reason for heterotopic ossification [4, 5].
The investigators suggest that in the absence of a reliable clinical presentation like comatose patients, compartmental pressure above 30–40 mm mercury should warrant consideration for fasciotomy. Most of the authors recommend fasciotomy in patients with impending compartment syndrome as a prophylactic measure to prevent devastating consequences of already set untreated compartment syndrome, which may include myonecrosis and muscle contractures to amputation of the involved limb [6].
We agree with the statement made by Mithoefer [4] that the assessment of compartment pressures assumes significant diagnostic relevance in unconscious patients but is of less diagnostic value when assessing alert, cooperative patients. The critical compartment pressure threshold in the thigh has yet to be defined. Fasciotomy provides effective treatment with a minimal morbidity. Suzuki [7] in their study was not able to clearly separate the contribution of arterial injuries from that of soft-tissue edema with respect to the development of the compartment syndrome. They mentioned the possibility of associated arterial injury in the development of the acute compartment syndrome of the proximal lower limb, especially in patients who sustain local blunt trauma to the thigh and show a rapid onset of the syndrome and together with hemodynamic instability. Bates [8] summarized that diagnosis of acute compartment syndrome is mainly clinical and a high index of suspicion and prompt intervention are required to diagnose and treat compartment syndrome and prevent irreversible damages. Purnell [9] revealed that the compartment syndrome of the thigh is rare and is usually associated with high-energy trauma and atraumatic causes usually involve the anterior compartment. Nwakile [10] concluded that there are limited data on thigh compartment syndrome with respect to the alternate way for fasciotomy incision, methods of wound closure, and complication rates. Fasciotomy may result in wound infection, requirement for skin grafting and post-operative adhesion may lead to restriction of range of movement in the knee joint. Many articles demonstrate certain wound closure techniques without the need for skin grafting, and good functional outcomes can be achieved with these techniques after fasciotomy [1]. In our case, since the patient was alert, conscious, and well oriented to time, place, and person, moreover, the patient already visited twice in a peripheral hospital and it was his third visit to the health-care facility for his injury, and on presentation, there was clinically full-blown compartment syndrome in his thigh. As we did not have access to the standard compartment pressure measuring devices (the Stryker system or Whitesides method) at that point of time at our institute, hence, we relied on our clinical judgment of acute compartment syndrome involving the anterior compartment of the thigh and opted for emergency fasciotomy. The probable cause of the compartment syndrome was found to be muscle contusion and the perforator injury which was diagnosed intraoperatively as a thrombosed torn vessel near the pocket of the hematoma. We did urgent USG color Doppler of the involved limb preoperatively which did not reveal any major vessel injury, aneurysm, or discontinuity. Therefore, we decided not to wait for a CT angiography, which would have been possible on the next day only, as there was already delay in presentation. Preoperatively, we took the consultation from a vascular surgeon and proceeded with the surgery with his backup.
In an inexperienced hand, there is a good chance to miss a case of thigh compartment syndrome as it is relatively uncommon without a fracture or any pre-injury pathological conditions and usually develops a few hours after the injury due to the typical anatomy of the thigh compartment. In our primary survey, we pay greater emphasis on thigh injuries that are linked to a fracture. However, in the absence of a fracture, it is frequently overlooked, and by the time, it is recognized, a full-blown compartment syndrome develops leading to the question of limb survivability. As a result, we believe that a high index of clinical suspicion combined with prompt management can spare a patient with acute thigh compartment syndrome from long-term disabilities.
Even in regions where acute compartment syndrome is rare, like the thigh, one should have a high index of suspicion in the event of a high velocity blunt trauma.
References
- 1.McCaffrey DD, Clarke J, Bunn J, McCormack MJ. Acute compartment syndrome of the anterior thigh in the absence of fracture secondary to sporting trauma. J Trauma 2009;66:1238-42. [Google Scholar]
- 2.Nooh A, Wang CK, AlAseem A, Harvey EJ, Bernstein M. Acute thigh compartment syndrome due to an occult arterial injury following a blunt trauma: A case report. JBJS Case Connect 2020;10:e0506. [Google Scholar]
- 3.Slade HJ, De Ridder K. A rare cause of acute compartment syndrome in the thigh: A case report. J Surg Case Rep 2020;2020:rjaa546. [Google Scholar]
- 4.Mithöfer K, Lhowe DW, Vrahas MS, Altman DT, Altman GT. Clinical spectrum of acute compartment syndrome of the thigh and its relation to associated injuries. Clin Orthop Relat Res 2004;425:223-9. [Google Scholar]
- 5.How MI, Lee PK, Wei TS, Chong CT. Delayed presentation of compartment syndrome of the thigh secondary to quadriceps trauma and vascular injury in a soccer athlete. Int J Surg Case Rep 2015;11:56-8. [Google Scholar]
- 6.Novak PJ, Bach BR, Schwartz JC. Diagnosing acute thigh compartment syndrome. Phys Sportsmed 1992;20:100-7. [Google Scholar]
- 7.Suzuki T, Moirmura N, Kawai K, Sugiyama M. Arterial injury associated with acute compartment syndrome of the thigh following blunt trauma. Injury 2005;36:151-9. [Google Scholar]
- 8.Bates J, Wamisho BL, Griffin M, Nyamulani N. Ward round-late presentation of acute compartment syndrome in the thigh. Malawi Med J 2009;21:85, 87. [Google Scholar]
- 9.Purnell J, Monument MJ, Johnston K, Desy NM. Proximal hamstring tendon avulsion resulting in acute posterior thigh compartment syndrome: A Case Report. JBJS Case Connect 2020;10:e0585. [Google Scholar]
- 10.Ojike NI, Roberts CS, Giannoudis PV. Compartment syndrome of the thigh: A systematic review. Injury 2010;41:133-6. [Google Scholar]








