Tibial plateau fracture can be associated with tibial avulsion injury, which can be addressed with a modified anterolateral approach. Careful evaluation is necessary to avoid missed injuries and complications related to it.
Dr. Showry Abraham Salikity, Department of Orthopaedics, All Indian Institute of Medical Sciences, Mangalagiri, Andhra Pradesh, India. E-mail: showryabraham007@gmail.com
Introduction: Avulsion fracture of the tibial tuberosity is a rare orthopedic injury, predominantly affecting adolescents but seldom seen in the adult population. Lateral tibial plateau fractures, while more common, infrequently present combined with tibial tuberosity avulsion. No established classification system currently describes or guides management for cases featuring both lateral tibial plateau split fracture and tibial tuberosity avulsion.
Case Report: This report describes a 30-year-old male presenting with acute knee pain and swelling following a road traffic accident. Radiographic evaluation revealed a unique combination of lateral tibial plateau split fracture and displaced tibial tuberosity avulsion. The patient underwent surgical fixation through an anterolateral approach, utilizing a lateral proximal tibial plate for the plateau fracture and lag screws with tension band wiring for the tuberosity avulsion. Early post-operative mobilization was implemented to mitigate the risk of stiffness.
Discussion: While tibial tuberosity fractures are historically documented in pediatric populations, their occurrence with isolated split lateral tibial plateau fractures in adults is exceptionally rare. A thorough review of the literature yielded only isolated reports of similar injury patterns, often within multi-fragmentary or bicondylar fractures. Proper radiological assessment and targeted internal fixation are crucial for optimal outcomes. Addressing the tuberosity avulsion is essential to restore extensor mechanism integrity and prevent non-union.
Conclusion: Simultaneous isolated split lateral tibial plateau fracture and tibial tuberosity avulsion highlight an uncommon injury pattern, warranting vigilance during diagnosis and treatment. Early surgical intervention and rehabilitation achieve favorable functional results.
Keywords: Lateral tibial plateau, tibial tuberosity avulsion, tension band wiring, tibial condyle.
Avulsion fracture of the tibial tubercle is a relatively uncommon injury, with a reported incidence ranging from 0.4% to 2.7%, usually seen in adolescent males approaching skeletal maturity with well-developed quadriceps musculature. Typically, these fractures present with marked displacement of the entire proximal apophysis, with or without intra-articular extension, and variable associated soft-tissue injury. The majority of these injuries are incurred during athletic activity involving jumping, most commonly basketball, and are the result of one of two possible mechanisms of injury: (1) violent knee flexion against a tightly contracting quadriceps, as in landing from a jump, or (2) violent quadriceps contraction against a fixed foot, as in jumping [1]. Tibial plateau fractures comprise 1% of all fractures. The incidence of tibial plateau fractures is 10.3/100,000 people annually. The mean age of patients incurring tibial plateau fractures is 52.6 years. The distribution of tibial plateau fractures is bimodal, with men under the age of 50 more likely to sustain this injury through high-energy mechanisms and frequently associated with soft-tissue injuries. While women over the age of 70 are more likely to have tibial plateau insufficiency fractures secondary to falls. Overall, men more commonly sustain tibial plateau fractures than women [2]. There have been many classifications for proximal tibia, including Schatzker, Hohl, and Moore, AO classification, and column concepts. None of the classifications includes tibial tuberosity avulsion as a component. Schatzker classification has different condyle, metaphyseal, and diaphyseal involvement as its components [3]. Hohl and Moore’s classification focuses on more complex patterns, including fracture dislocations and fractures causing knee instability. Recently, 4-column and 10-column concepts have been developed based on axial sections of computed tomography (CT) imaging, dividing the proximal tibial plateau into 4 or 10 columns to guide the approach and fixation [4]. AO classification describes an avulsion fracture in A type with subtype A1.2 and a lateral tibial plateau fracture split in B type with subtype B1.1. No classification system describes the combination of a lateral tibial plateau split fracture with a tibial tuberosity avulsion fracture. Here, we present a case with a combination of a lateral tibial plateau split fracture with a tibial tuberosity avulsion fracture. A thorough literature search did not show any such case in published English literature.
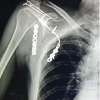
A 30-year-old male patient presented to the casualty with complaints of knee swelling, pain, and being unable to bear weight. The patient had a history of a road traffic accident. On examination, diffuse swelling was noted over the left knee with extension into the leg; the skin over the swelling was tense, with no blisters or signs of compartment syndrome. No distal neurovascular deficits were noted. AP and lateral radiographs showed a lateral tibia split fracture with tibial tuberosity avulsion (Fig. 1).

Figure 1: X-ray of the knee anteroposterior and lateral view, showing lateral condyle split fracture with tibial tuberosity avulsion with high riding of the patella.
The patient was given above knee back slab, and the limb was elevated. We monitored for signs of compartment syndrome at regular intervals. After subsidence of swelling, lateral tibial plateau fracture and tibial tuberosity fracture were addressed with an anterolateral approach with incision extended proximally for the application of tension band wiring from the patella to the distal part of tibial tuberosity (Fig. 2).

Figure 2: Demonstrating intraoperative image of the tibial tuberosity avulsion fragment.
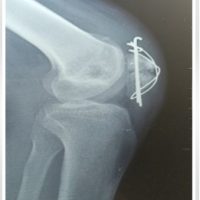
Lateral tibial plateau fracture was fixed with a T-buttress plate, and tibial tuberosity fixation was done with two cortical screws. A long knee brace was applied postoperatively to avoid knee flexion. Non-weight-bearing on the left lower limb and walker-assisted mobilization were started from day 2. (Fig. 3).

Figure 3: Post-operative X-ray of left knee anteroposterior and lateral view showing T-buttress plate for the lateral condyle and cortical screw for tibial tuberosity and tension band wiring.
Tibial tuberosity fractures are a rare injury of the proximal tibia and are usually seen in adolescent children, and are less commonly seen in the adult population. Classification of tibial tubercle fractures has gone through an evolution. The original classification system was provided by Sir Reginald Watson–Jones [5], which defined three types. Type I was an avulsion of a small part of the tibial tubercle, distal to the proximal tibial physis. Type II extended across the physis but did not enter the knee joint. Type III was an avulsion, which extended proximally to the physis into the knee. This classification was modified by Ogden et al. to more accurately define specific fracture patterns and to establish treatment for different fracture types by including displacement and comminution. Ryu and Debenham [6] then suggested the addition of a Type IV, which is a fracture of the tibial tuberosity that extends posteriorly along the proximal tibial physis, creating an avulsion of the entire proximal epiphysis. Next, the addition of a type C was proposed by Frankl et al. [7] for fractures with associated patella ligament avulsions. Finally, a Type V was suggested by McKoy and Stanitski [8], also described by Curtis, which consists of a Type IIIB fracture with an associated Type IV fracture creating a “Y” configuration. Tibial tuberosity fractures, which represent a disruption of the quadriceps mechanism, are not rare, particularly with Schatzker type V and VI fractures. Tibial tubercle fractures may easily be missed in these complex injuries. A poorly performed knee lateral radiograph can miss the fracture. Maroto et al. [9] retrospectively reviewed a prospectively compiled orthopedic trauma database and identified 392 bicondylar fractures of the tibial plateau, in which 85 tibial tubercle fractures (21.6%) were identified in 84 patients. Tan et al. [10] reported a case where Schatzker Type IV with tibial tuberosity fracture were noted. Rana et al. [11] reported a case of bicondylar proximal tibial plateau fracture with tibial tuberosity avulsion. To the best of our knowledge, this is the first case of Schatzker Type I fracture (AO type 41B1.1) with displaced tibial tuberosity avulsion. The tibia tuberosity should be fixed adequately. Fixation of the tibial tuberosity can be done with the application of cc screws, tension band wiring, or cortical screws, which can be applied as lag screws whenever there is comminution of the tibial tuberosity or posterior cortex of the tibia. In such a situation plate application should be considered. Failure to address the tibial tubercle component of a tibial plateau fracture has been shown to result in non-union of the tibial tubercle fracture [12]. In our case, we applied cortical screws as lag screws and tension band wiring done from the superior pole of the patella through a transosseous tunnel distal to the tibial tuberosity to reduce the quadriceps pull on the patellar tendon.
Tibial tuberosity fracture, along with an isolated split lateral tibial plateau fracture, is rare, especially in adults. Therefore, care should be taken to ensure it is not missed. Proper imaging, including a CT scan, should be done. Tibial plateau fracture should be fixed with appropriate internal fixation, and simultaneously, tibial tuberosity avulsion should be addressed. Early rehabilitation should be started to prevent stiffness. With proper surgical fixation and early rehabilitation, a good functional outcome can be achieved.
In patients presenting with tibial plateau fractures, particularly isolated lateral split fractures, surgeons must maintain a high index of suspicion for an associated tibial tuberosity avulsion—even in adults, where this injury pattern is rare. Careful clinical assessment and thorough radiological evaluation, including CT imaging when indicated, are essential to avoid missed diagnosis. Failure to recognize and adequately fix the tibial tuberosity component may compromise the extensor mechanism and lead to complications such as non-union, extensor lag, and poor functional outcomes. Simultaneous anatomical reduction and stable fixation of both the plateau fracture and the tuberosity avulsion, followed by early supervised rehabilitation, are critical for achieving optimal knee function
References
- 1. Frey S, Hosalkar H, Cameron DB, Heath A, David Horn B, Ganley TJ. Tibial tuberosity fractures in adolescents. J Child Orthop 2008;2:469-74. [Google Scholar] [PubMed]
- 2. Malik S, Herron T, Mabrouk A, Rosenberg N. Tibial plateau fractures. In: StatPearls. StatPearls Publishing; 2023. Available from: https://www.ncbi.nlm.nih.gov/sites/books/nbk470593 [Last accessed on 2025 Aug 27]. [Google Scholar] [PubMed]
- 3. Kfuri M, Schatzker J. Revisiting the Schatzker classification of tibial plateau fractures. Injury 2018;49:2252-63. [Google Scholar] [PubMed]
- 4. Vosoughi F, Oskouie IM, Rahimdoost N, Pesantez R. Decoding tibial plateau fracture classifications: A century of individualized insights in a systematic review. EFORT Open Rev 2025;10:316-26. [Google Scholar] [PubMed]
- 5. Watson-Jones R. The classic: “Fractures and joint injuries” by sir reginald watson-jones, taken from “fractures and joint injuries,” by R. watson-jones, vol. II, 4th ed., baltimore, williams and wilkins company, 1955. Clin Orthop Relat Res 1974;105:4-10. [Google Scholar] [PubMed]
- 6. Ryu RK, Debenham JO. An unusual avulsion fracture of the proximal tibial epiphysis. Case report and proposed addition to the Watson-Jones classification. Clin Orthop Relat Res 1985;194:181-4. [Google Scholar] [PubMed]
- 7. Frankl U, Wasilewski SA, Healy WL. Avulsion fracture of the tibial tubercle with avulsion of the patellar ligament. Report of two cases. J Bone Joint Surg Am 1990;72:1411-3. [Google Scholar] [PubMed]
- 8. McKoy BE, Stanitski CL. Acute tibial tubercle avulsion fractures. Orthop Clin North Am 2003;34:397-403. [Google Scholar] [PubMed]
- 9. Maroto MD, Scolaro JA, Henley MB, Dunbar RP. Management and incidence of tibial tubercle fractures in bicondylar fractures of the tibial plateau. Bone Joint J 2013;95-B:1697-702. [Google Scholar] [PubMed]
- 10. Tan L, Li YH, Li Y, Lin T, Zhu D, Sun DH. Tibial plateau fractures (AO type B3) combined with tibial tubercle fracture. Medicine (Baltimore) 2018;97:e12015. [Google Scholar] [PubMed]
- 11. Rana R, Ganesh A, Behera S 2nd, Behera H. Tibial plateau fracture with avulsion fracture of tibial tuberosity: A case report and review of literature. Cureus 2020;12:e7756. [Google Scholar] [PubMed]
- 12. Phisitkul P, Mckinley TO, Nepola JV, Marsh JL. Complications of locking plate fixation in complex proximal tibia injuries. J Orthop Trauma 2007;21:83-91. [Google Scholar] [PubMed]