The physical therapists and patients should be aware of this condition before administering cryotherapy. A simple and a routine test to screen cold urticaria should be included in musculoskeletal physical therapy practice.
Dr. Gopisankar Balaji, Department of Ortho Surgery, Jawaharlal Institute of Post Graduate Medical Education and Research, Puducherry, India. E-mail: drgopi9596@gmail.com
Introduction:Musculoskeletal rehabilitation is one of the frontline domains in physical therapy practice. In most countries, physical therapists prefer independent practice with referrals from general practitioners and orthopedic surgeons. Under these circumstances, the physical therapist may be the first contact professional handling these individuals who may not have adequate medical records with their personal medical history. Cryotherapy for pain relief could be the first choice of pain management opted by a musculoskeletal therapist. That is when both the therapist and the patient have to be aware of the undesirable effects of cryotherapy application and its potential local and systemic complications. The outcome of this paper could be an initiative for a standardized screening process to be incorporated into physical therapy practice.
Clinical Findings:A 30-year-old man with left knee pain who underwent exercise therapy in the physiotherapy unit of a tertiary care center developed erythematous rashes around the knee following ice application. It was noted that the patient was not aware of the same in the past. The patient was attended by a dermatologist, and a diagnosis of cold urticaria was made following confirmation with cold stimulation test.
Conclusion:From this study, it may be concluded that the awareness of cold-induced urticaria has to be emphasized on both patients and health care professionals. A simple screening protocol should be made mandatory in orthopedic physical therapy practice, which would suffice this purpose.
Keywords: Urticaria, cryotherapy, Physical therapy
Cryotherapy in rehabilitation has its therapeutic effects by reducing pain, tissue temperature, blood flow, and metabolism. Cryotherapy seems more effective in limiting pain and swelling as a short-term outcome in musculoskeletal injuries [1]. Empirical solid evidence suggesting 10min of intermittent cryotherapy has been proved effective in musculoskeletal injuries [2]. With the evident facts, contraindications for cryotherapy include allergies, Raynauds disease, cold hyper and hyposensitivity, and vascular insufficiency [3]. Cold-induced urticaria is one such condition characterized by the development of localized or diffuse urticaria, angioedema, and rarely systemic symptoms secondary to exposure to a cold stimulus which can lead to serious consequences. Patients may or may not be aware of such reactions as the cold triggers often vary. Hence in patients with no previous exposure to cryotherapy, it may be necessary to ask for a history of reactions to cold triggers. If history is suggestive, a simple diagnostic test to confirm cold urticaria can be done as a part of screening before cold administration as a therapeutic measure in musculoskeletal physical therapy practice.
A 30-year-old man with left knee pain was referred for rehabilitation. Two months before, he sustained a soft tissue injury and was treated with a Robert Jones compression bandage for 2weeks and anti-inflammatory drugs in a nearby local hospital.
On clinical evaluation, the individual had wasting of the thigh and calf muscles compared to the unaffected limb. He had an observable weakness of gluteus medius, gluteus maximus, quadriceps, and calf muscles. His ligament integrity was well preserved.
Based on the examination, he was taken up for progressive resisted exercise protocol after brief warming up session. Following safety instructions, cryotherapy gel packs (Maintained at 20°C to 25°C) were administered over the left knee and ankle to avoid muscle soreness post – exercises as a routine procedure. In a short period (2–3 min), the patient developed erythematous rashes around the knee joint not associated with itching or pain (Fig.1). However, there were no rashes or reactions observed around the ankle. No other observable reactions were noted while the individual continued to be normal. When he was questioned about a similar incident in the past, he was ignorant about the reaction and was immediately taken to the dermatologist’s opinion and care. The rashes disappeared within 30 min without any other complications.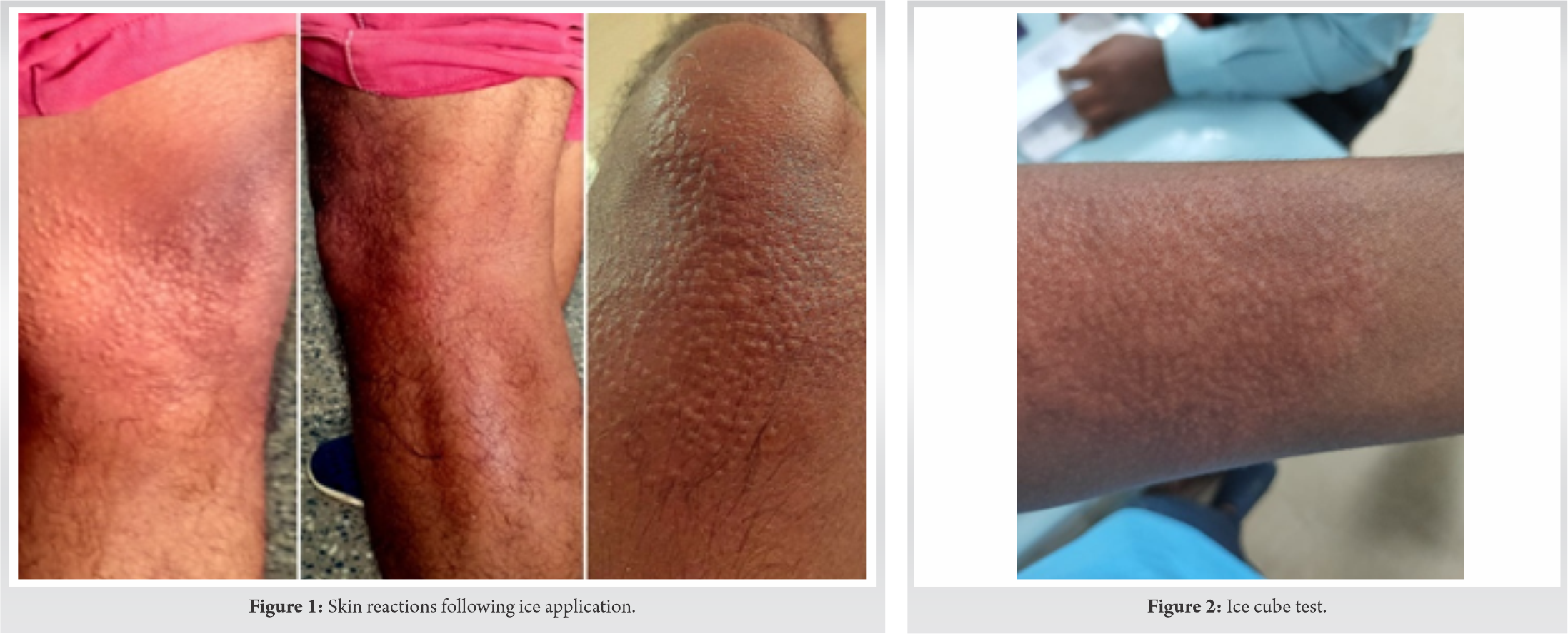
The dermatologist considered the possibility of cold contact urticaria and performed a cold provocation test using “melting ice cube” as per the standard protocol to confirm the same[4].On the ice cube test, a similar reaction with asymptomatic tiny 2–3 mm monomorphic wheals was observed at the site of contact, which disappeared within 30 min (Fig.2). He had no systemic symptoms or inducible urticarias and a family history of similar complaints. Tests for other inducible urticarias and investigations for secondary causes of acquired cold urticaria were also negative[5,6]. Hence, he was diagnosed with primary acquired cold contact urticaria with an atypical cholinergic urticaria-like presentation.
As the patient was not concerned about the reaction owing to its asymptomatic nature, lack of systemic reaction, and spontaneous resolution, he was not prescribed antihistamines. He was advised to avoid contact with cold objects.
Ever since time, cryotherapy has been used as a modality to reduce inflammatory reactions. Ignorance about the undesirable effects of ice application usually surpasses the clinical and functional outcomes of the intervention [3]. In this scientific era, the physiological mechanism behind its effect, together with clinical and empirical evidence, prove cryotherapy as effective and harmless as there is no change in heart rate, blood pressure, and cardiac changes[7] the drop in temperature in muscular tissues depends on the duration of cryotherapy application. The cooling effect on muscles is maintained several hours after removal of the cold surface application. The main effects of cryotherapy are probably induced locally, such as pain reduction, hypometabolic and vascular changes.
The vascular response to cryotherapy is complex, and the possible factors are neuronal activity, receptor mechanism, smooth muscle contractile elements, platelet activity, endothelial activity, and rheumatological factors. There have been deleterious effects of cryotherapy in various studies, such as the risk of local and systemic complications. The complications following cryotherapy can be as simple as cutaneous rash [8] to anaphylactic reactions leading to death [9]. However, cold therapy can be used as a valid therapeutic option with a precaution. Cold urticaria is one such complication, the foundation of which is awareness and avoidance of cold exposure. The potentially serious consequences of any condition in using cryotherapy can be life-threatening. The two diagnostic clinical tests used to confirm urticarial complications are cold stimulation tests and cold stimulation test time. Cold stimulation test is done by applying an ice cube on the skin and noting the subsequent skin reaction following skin rewarming. In this case, the patient did not develop similar rashes around the ankle; hence, even in a known case of cold urticaria, the response to ice may vary from one part of the body to another. Cold stimulation test time measures the maximum time to induce the reaction following ice cube application [3].
Reports in literature describe cold-induced cholinergic urticaria, which often occurs following exercise in a cooler environment in which the ice cube test is negative, or coexistence of cold and cholinergic urticaria wherein the appropriate provocation tests elicit the typical manifestations of either cold or cholinergic urticaria[4,10]. Similarly, some variants of atypical cold urticaria are extremely rare and hence are ill-characterized. These include systemic atypical cold urticaria, localized cold reflex urticaria, delayed Cold urticaria, cold-induced cholinergic urticaria, and cold-dependent dermographism. There is a need for improved classifications of cold urticaria [11].
In the present case, the patient developed monomorphic 2–3 mm wheals mimicking cholinergic urticaria but following a cold trigger. The possibility of cold-induced cholinergic urticaria can be considered in this case as cryotherapy was applied post-exercise, following which the wheals developed. Since the cold stimulation test is characteristically negative in cold-induced cholinergic urticaria [12], the diagnosis of atypical presentation of cold contact urticaria mimicking cholinergic urticaria was considered in our case as the cold stimulation test was positive. Similarly, localized cold reflex urticaria was not considered as the punctate pruritic wheals usually occur at 5–8cm adjacent to the site of cold stimulation test rather than at the site of contact with the ice as observed in our case. The atypical presentation of cold contact urticaria mimicking cholinergic urticaria has not been reported so far. However, the coexistence of multiple inducible urticarias in the same patient with the occurrence of a cholinergic type of urticaria following exercise following a cold environment has been reported [10,12].
Though our patient did not develop systemic symptoms, life-threatening complications like anaphylaxis have been reported with cold urticaria. Hence, one needs to be aware of absolute and relative contraindication for cryotherapy to avoid untoward effects. The take-home message of this report is that a screening question about the history of undesirable effects of cold exposure needs to be obtained before administering cryotherapy in physical therapy practice. A simple diagnostic test can be done to rule out cold urticaria, or other modalities of physical therapy can be considered in case of positive history.
It may be suggested that the awareness of cold-induced urticaria has to be emphasized on both patients and health care professionals. A simple screening protocol should be made mandatory in orthopedic physical therapy practice, which would suffice its purpose.
References
- 1.Hubbard TJ, Aronson SL, Denegar CR. Does cryotherapy hasten return to participation? A systematic review. J Athl Train 2004;39:88-94. [Google Scholar]
- 2.Bleakley C, McDonough S, MacAuley D. The use of ice in the treatment of acute soft-tissue injury: A systematic review of randomized controlled trials. Am J Sports Med 2004;32:251-61. [Google Scholar]
- 3.Dover G, Borsa PA, McDonald DJ. Cold urticaria following an ice application: A case study. Clin J Sport Med 2004;14:362-4. [Google Scholar]
- 4.Torabi B, Ben-Shoshan M. The association of cholinergic and cold-induced urticaria: Diagnosis and management. Case Rep 2015;2015:bcr2014205258. [Google Scholar]
- 5.Hochstadter EF, Ben-Shoshan M. Cold-induced urticaria: Challenges in diagnosis and management. Case Rep 2013;2013:bcr2013010441. [Google Scholar]
- 6.Siebenhaar F, Weller K, Mlynek A, Magerl M, Altrichter S, Vieira Dos Santos R, et al. Acquired cold urticaria: Clinical picture and update on diagnosis and treatment. Clin Exp Dermatol 2007;32:241-5. [Google Scholar]
- 7.Swenson C, Swärd L, Karlsson J. Cryotherapy in sports medicine. Scand J Med Sci Sports 1996;6:193-200. [Google Scholar]
- 8.Cook DK, Georgouras K. Complications of cutaneous cryotherapy. Med J Aust 1994;161:210-5. [Google Scholar]
- 9.Sigal C, Mitchell JC. Essential cold urticaria: A potential cause of death while swimming. Can Med Assoc J 1964;91:609-10. [Google Scholar]
- 10.Kaplan AP, Garofalo J. Identification of a new physically induced urticaria: Cold-induced cholinergic urticaria. J Allergy Clin Immunol 1981;68:438-41. [Google Scholar]
- 11.Maltseva N, Borzova E, Fomina D, Bizjak M, Terhorst-Molawi D, Košnik M, et al. Cold urticaria-what we know and what we do not know. Allergy 2021;76:1077-94. [Google Scholar]
- 12.Cheon HW, Han SJ, Yeo SJ, Lee SH, Kim MJ, Kim SH, et al. A case of combined cholinergic and cold urticaria. Korean J Intern Med 2012;27:478-9. [Google Scholar]










